Urinary System

Urinary System
Feb 24, 2016
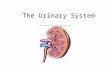
Urinary System. Consists of: . Kidney(s) Ureters Urinary Bladder Urethra. Functions:. Filter gallons of fluid from bloodstream Filter plasma 60 times/day Responsible for removing: Toxins Metabolic Wastes Excess ions. Regulates volume and chemical make up of blood - PowerPoint PPT Presentation
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Urinary System

Consists of:
• Kidney(s)• Ureters• Urinary Bladder• Urethra

Functions:
• Filter gallons of fluid from bloodstream– Filter plasma 60
times/day• Responsible for
removing:– Toxins– Metabolic Wastes– Excess ions
• Regulates volume and chemical make up of blood
• Maintains the proper pH between water, salts, acids and bases– Maintains blood pH
between 7.35 – 7.45

Functions
• Regulatory functions include:– Produce hormones Renin
and erthropoietin– Renin helps regulate BP and
kidney function– Erthropoietin stimulates
RBC production in bone marrow
– Assists in metabolizing Vitamin D to its active form.

Kidney Anatomy• Kidneys are covered by
fatty tissue; anchors kidneys to posterior wall
• Internal Anatomy – 3 distinct regions– Pelvis – where kidneys
join ureters; responsible for collecting urine
– Renal Cortex – outer region; most of nephrons are found here
– Medulla – Middle region; Renal pyramids
Medulla

• Nephron – Working Unit of Kidney; Carry out processes that form urine
C o r tex
M e d u l l a

Nephron
• Glomerulus – tuft of capillaries
• Parts of Nephron– Bowman’s capsule– Renal Tubule - 3 cm in
length• Proximal Convoluted tubule
(PCT)• Loop of Henle• Distal Convoluted tubule
(DCT)– Collecting Duct

Urine Formation Involves 3 processes
• Filtrationglomerulus and Bowman’s capsule
• Renal Reabsorption
Carried out by renal tubules
• Secretion Carried out by renal tubules

• Glomerular Filtration– Blood enters via afferent
arteriole (larger diameter) and leaves via the efferent arteriole
– Difference in vessel diameter increases BP in glomerulus and assists with filtration

• Podocytes (Bowman’s capsule) – surround capillaries
• Passive, nonselective process where fluids and solutes are passed through a membrane
• Force is cause by hydrostatic pressure– What caused pressure
increase?

• GFR (Glomerular filtration rate) is the amount of filtrate produced in the kidneys in one minute.
• Renin regulates GFR by causing an increase in blood volume and blood pressure (Constricts blood vessels)

• Filtration Pressure – Increase in BP at glomerulus forces water and solutes out of blood and into capsule.
• What passes through? What remains in the blood?
Filtrate is not Urine

• Filtrate contains both wastes and needed water and solutes
• Reabsorption begins as soon as nutrients enters the PCT
• All water can’t be excreted, so tubules claim what it needs
• Why is it called reabsorption and not absorption?

What is reabsorbed?• 100 % of organic nutrients• Most electrolytes by
facilitated diffusion• Water is passively
reabsorbed– 60 – 70 % of fluid is reaborbed
by PCT
Rate and degree of reabsorption is regulated by hormones
Problems: Hyperglycemia

Where does Reabsorption occur in the nephron? • PCT are most active
reabsorbers• The descending loop of
Henle is permeable to water but not solutes
• The ascending loop of Henle is impermeable to water and most solutes– Na and Cl are actively
reabsorbed into the blood stream
• DCT is impermeable to solutes
• Reabsorption of Na, K, and water is controlled by hormones

Figure 25.18a
Cortex
Outermedulla
Innermedulla
(a)
(b)
(c)
(e)
(d)
Na+ (65%)GlucoseAmino acids
H2O (65%) and many ions (e.g.Cl– and K+)
300
Milliosmols
600
1200
Blood pH regulation
H+,NH4
+
HCO3–Some
drugs
Active transport(primary or secondary)Passive transport
(a) Proximal convoluted tubule: • 65% of filtrate volume reabsorbed • Na+, glucose, amino acids, and other nutrients actively transported; H2O and many ions follow passively • H+ and NH4
+ secretion and HCO3– reabsorption to
maintain blood pH • Some drugs are secreted

Reabsorption
(b) The descending loop of Henle
• Freely permeable to H2O• Not permeable to NaCl or
other solutes• Filtrate becomes
increasingly concentrated as H20 leaves by ____________?
Active transport(primary or secondary)Passive transport

Figure 25.18c
Na+
Urea
Cl–
Na+
Cl–
K+
(c) Ascending limb of loop of Henle • Impermeable to H2O • Permeable to NaCl • Filtrate becomes increasingly dilute as salt is reabsorbed
(a)
(b)
(c)
(e)
(d)
Cortex
Outermedulla
Innermedulla
300
Milliosmols
600
1200
Active transport(primary or secondary)Passive transport

Figure 25.16a
Loop of Henle
Osmolalityof interstitialfluid(mOsm)
Innermedulla
Outermedulla
Cortex Active transport Passive transportWater impermeable
The ascending limb:• Impermeable to H2O• Permeable to NaClFiltrate becomes increasingly dilute as NaCl leaves, eventually becoming hypo-osmotic to blood . NaCl leaving the ascending limb increases the osmolality of blood.
Filtrate entering the loop of Henle is contains many substances that are needed in the body
The descending limb:• Permeable to H2O• Impermeable to NaClAs filtrate flows, it becomes increasingly concentrated as H2Oleaves the tubule by osmosis. The filtrate osmolality increases.
H2O
H2O
H2O
H2O
H2O
H2O
H2O
NaCI
NaCI
NaCI
NaCI
NaCI

What’s left in the nephron?
• Non-reabsorbed substances are:– Urea – 50 % is
reclaimed; the rest is waste
– Creatinine – a large lipid; insoluble molecule that is not reabsorbed at all
– Uric Acid – 50 % is reclaimed; waste product of RNA synthesis

Tubular Secretion – “Reabsorption in Reverse”
• Urine is formed from filtered and secreted substances
• Secretion occurs in the DCT tubules and collecting ducts – Hormones assist with
this process• ADH (antidiuretic
hormone)• Aldosterone• ANP

Figure 25.18d
Na+; aldosterone-regulatedCa2+; PTH-regulatedCl–; follows Na+
(d) Distal convoluted tubule • Na+ reabsorption regulated by aldosterone • Ca2+ reabsortion regulated by parathyroid hormone (PTH) • Cl– cotransported with Na+
(a)
(b)
(c)
(e)
(d)
Cortex
Outermedulla
Innermedulla
300
Milliosmols
600
1200
Active transport(primary or secondary)Passive transport

Figure 25.18e
Blood pHregulation
Urea;increasedby ADH
Na+
K+
H+
HCO3–
NH4+
H2O regulatedby ADH
Regulated byaldosterone:
(e) Collecting duct • H2O reabsorption regulated by ADH • Na+ reabsorption and K+ secretion regulated by aldosterone • H+ and HCO3
– reabsorption or secretion to maintain blood pH • Urea reabsorption increased by ADH Why?
(a)
(b)
(c)
(e)
(d)
Cortex
Outermedulla
Innermedulla
300
Milliosmols
600
1200
Active transport(primary or secondary) Passive transport

Substances that are not reabsorbed• Substances that lack
carry proteins along membrane– Urea– Uric acid
• Substances that are not lipid soluble
• Substances that are too large to pass– Creatinine

Label the parts of the nephron
Describe what is occurring at sections 1-6.1.
2.
3.
4.
5.
6.
1
2
34
5
6

Hormonal Control of Secretion• Osmolarity – number of
solute particles dissolved in one liter of waterAffects osmosis
• Kidneys are responsible for regulating solute concentrations in the body; the concentration of urine is regulated by hormones
• Four Hormones Control Kidney Function– Renin– Aldosterone– Atrial Natiuretic
Peptide (ANP)– Antidiuretic hormone
(ADH)

Renin• Released when
glomerular pressure is low
• Causes blood vessels to constrict; raising blood pressure in arteries
• The efferent arteriole constricts which increases glomerular pressure
• Stimulates secretion of ADH and aldosterone

Aldosterone
• Released by adrenal glands
• When secreted causes Na+ to be reabsorbed from DCT
• H20 follow Na+, so both Na+ and H2O are reabsorbed
• Eliminates K+ into urine
• Stimuli that cause the release of aldosterone– Decreased blood volume
– Decreased sodium in blood
– Increased potassium in blood (heart block)


If too much aldosterone is secreted:- Excessive Na+ and H20 retention (edema, hypertension- Accelerated secretion of K ions (muscle responsiveness)

Lasix – (Diuretic) inhibits Na from being reabsorbed; thus water is not reabsorbed.

Atrial Natiuretic Peptide (ANP)• Works against
aldosterone• Released by atrial
cardiac cells when blood volume and BP are too high.
• Why would the atrial cells detect a change in blood volume?
• When ANP is secreted:– Causes Na+ to be dumped into
tubules (urine)– H2O follows sodium into urine– Capillaries in glomerulus
dilate; increasing blood flow to Bowman’s capsule; increasing UO
– Inhibits the secretion of renin, aldosterone and ADH
– Urine contains more Na+ H2O; blood pressure and blood volume decrease

ADH (Antiduretic hormone)• When ADH is secreted,
water is reabsorbed from DCT and collecting tubules
• Person feels thirsty• When ADH is not
secreted, DCT and collecting tubules are impermeable to water, no reabsorption occurs here.

Concentration of Urine is controlled by ADH
• Dilute Urine– Na and other ions
are removed from filtrate
– Urine appears clear in color
• Concentrated Urine– ADH is secreted; distal
and collecting tubules reabsorb water
– When water leaves filtrate; urine concentration increases
W i t h o u t u s e o f h o r m o n e s , D C T a n d c o l l e c ti n g d u c t a re re l a ti v e l y i m p e r m e a b l e t o w a t e r a n d s o d i u m

Work of the Nephron with Hormone Secretion

Diuretics – chemicals which increase UO
• Any substance that is not reabsorbed and carrries water out of body– Alcohol – inhibits ADH– Caffeine – Increases
filtration rate (GFR)• Diuretic drugs are taken
for CHF, edema and to increase UO

Figure 25.17a
Active transport Passive transport
(a) Absence of ADH Large volumeof dilute urine
Collecting duct
Cortex
NaCI
NaCI
NaCI
Urea
Outermedulla
Innermedulla
DCT
H2O
H2O
Descending limbof loop of Henle

Maintaining a Balance
• Other Systems assist in excretion and affect kidney function– Integumentary– Respiratory– Digestive
• Fluid and Electrolyte Balance– Water into body = Water out
of the body– Neither a net gain or loss of
electrolytes should occur in body
• Acid-Base Balance– Blood pH ranges between
7.35 – 7.45– Kidneys will secrete H+ ions
when blood pH drops

• Acidosis – Blood pH drops below 7.35– Respiratory Acidosis
• Due to an increase of CO2
levels in body– Metabolic Acidosis
• Due to cell metabolism in the body
• Lactic acid in muscle metabolism
• Ketone bodies by the breakdown of fat
• Diabetics don’t use glucose due to lack of insulin; so cells will break down fat instead
Imbalances
Blood ph < 7.05 disrupts the stability of cell membrane, alters protein function (enzyme), causes heart arrhythmias and leads to coma

Kidney Stones• Hardened mineral
deposits that form in kidney
• Symptoms– Blood in urine– Increased need to go– Nausea and vomiting– Pain during urination– Tenderness in abdomen
and kidney region• Treatment
– Lithotripsy– Medication

Renal Failure – Kidney Failure• Nephrons in kidney stop
functioning– Unable to filter or
excrete waste– Can’t regulate
composition of body fluids
– Can’t control erythrocyte function or blood pressure
– Can’t control salt balance
Related Documents