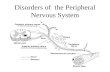
By Sean Dadswell June 2011

Peripheral nerve entrapment
Jan 21, 2015
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

By Sean DadswellJune 2011

AimsDiscuss physiology associated to PNEDiscuss general signs and symptoms of PNEIdentify:
Case StudyClinical presentation PathophysiologyDifferential diagnosisDiagnostic technique/tests Treatment of some of the more common PNE’s

Neural PhysiologyNee & Butler 2005, Prinz et al 2005
Basic structure as shownNeurons have a cell body
which contains nucleus, cytoplasm, mitochondria and other organelles.
Dendrites which collect information and transport it to the cell body
Axon which transport information away from the cell body
Synapse which transfers info to other cells
How long is a neuron?How fast do they repair?
WHY?

Axoplasmic flowProcess by which nerve
cells transport proteins, lipids and other materials essential for the maintenance and repair of the cell from the cell body along the axon.
Also means of removing molecules responsible for axon degradation
Molecules are transported down microtubules by specific proteins and enzymes
The speed of this transport is from 0.1mm-400mm day
Axons can be 10000 times longer than the cell body
Cell Transport (Prinz et al, 2005)

Nerve injuryNerve injury secondary to compression or traction depends
on intensity and duration.
Seddon has classified nerve injuries into 3 categories:First, neuropraxia, is a transient episode of motor paralysis
with little or no sensory or autonomic dysfunction. No disruption of the nerve or its sheath occurs. With removal of the compressing force, recovery should be complete.
Second, axonotmesis, is a more severe nerve injury with disruption of the axon but with maintenance of the Schwann sheath. Motor, sensory, and autonomic paralysis results. Recovery can occur if the compressing force is removed in a timely fashion and if the axon regenerates.
Third, neurotmesis is the most serious injury. The nerve and its sheath are disrupted. Although recovery may occur, it is never complete, secondary to loss of nerve continuity.

Mechanical or chemical irritation
Compromised intraneural circulation
Reduced axoplasmic flow
Hypoxia and altered microvascular permeability
Subperineurial oedema
Intraneural fibrosis
Neural Injury Cascade

How does this lead to pain?Endoneurial oedema
increases sensitivity of nocioceptors in the nervi nervorum (nerves that innervate the neural sheath of larger nerves)
Intraneural fibrosis reduces extensibility of the nerves increasing mechanical stimulation of nervi nervorum
Reduced axoplasmic flow =>Reduced myelin thickness
Formation of Abnormal Impulse Generating Sites (AIGS)As nerve injury leads
to altered gene expression and increases number of ion channels along axon (as ion channels can only form on unmyelinated parts of axon)
Ion channels increase sensitivity of neurons

AIGS sensitive to adrenaline and noradrenaline so neuropathic pain often sensitive to stress
Afferent axons (ie those travelling from spinal cord outwards) can cause the release of pro-inflammatory chemicals into their target tissue (neurogenic inflammation) so can have a detrimental impact on the tissue it supplies
Central sensitisation and altered descending pathway inhibition

Other symptomsPositive Symptoms
(abnormal level of excitability of the nervous system)Pain (often deep)ParasthesiaDysesthesia
Hyperalgesia Allodynia
Spasm
Negative symptoms (reduced impulse conduction of neural tissue)Hypoestesia/
anesthesiaweakness

Carpal Tunnel Syndrome (Shapiro & Preston 2009)
Most common entrapment neuropathy
Median nerve compression by the transverse carpal lig
More women than menOften bilat but almost
without exception more prominent in the dominant hand
Paresthesia usually in median nerve distribution
(thenar eminance spared as supplied by palmar cutaneous sensory branch which comes off proximal to the carpal tunnel
Advanced cases may have thenar muscle weakness/wasting effecting thumb opposition and ab
Median nerve sensory distribution
Median nerve
Flexor tendonsTransver
se carpal ligament

Causes of CTS
Often idiopathicRepeated stress to
connective tissueRepetitive hand useIndividuals with small
carpal tunnelSystemic disorders (RA,
hypothyroidism, DM, sarcoid, amyloidosis
Mass in wrist (ganglion cyst, neurofibroma, arteriovenous malformation)
Pregnancy
Persistent wrist flex ie during sleep
Thenar eminence wasting

CTS contPhalan’s good specific
(75-93%) and moderate sensitive (64-75%) for CTS
Tinel’s similar spec & sens (tetro et al, 1995 Bolland et al, 2008)
Carpal compression test more spec less sensitive
NCS and EMG can help confirm diagnosis and discount others (however can be normal in 25% of cases)
Differential diagnosis:C6-7 radiculopathyBracial plexopathyProximal median
neuropathyThese can be identified
by pain in the neck, reduced reflexes, weakness outside median nerve distribution, sensory loss in the thenar eminence.

Treatments for CTSRemove causative
factorsSplints (night)NSAIDsInjection (beware >3
may => tendon rupture) may be particularly helpful during pregnancy or other reversible condition i.e. Hypothyroidism
Surgical decompression (open safer than closed but longer recovery)
Wrist stretchesWrist mobsMedian nerve mobs

www.emglaboratory.com

Ulnar Neuropathy at the Elbow (Robertson & Saratsiotis 2005)Second most common
PNE in upper limbCaused by compression
of ulnar nerve in the ulnar groove or cubital tunnel
Results from repeated trauma,OA following #, ganglion/tumours/fibrous tissue
Manifests as progressive loss of grip and pinch strength and interosseus muscle function
ClumsinessWasting of thenar and
hypothenar eminence

Thenar and hypothenar eminence wasting in the left hand

Interosseous muscle wasting

Ulnar neuropathy contMay be minimal sensory
loss reported but may be evident 4th and 5th finger on Ax
Elbow pain common spreading to wrist
Ulnar nerve may be palpable and tender
Paresthesia provoked by tinel’s, ulnar nerve compression or elbow flexion
Making a fist may result in 4th and 5th finger not flexing (FDP innervated by UN)
Thumb ab and opposition are spared

Ulnar neuropathy contSeveral classic hand
postures may be presentBenediction posture Wartenberg’s signFroment’s sign

Differential diagnosisC8-T1 radiculopathyBrachial plexopathyUNE forearm or wrist
There may be weakness in muscles not innervated by the ulnar nerve or loss of sensation extending up the forearm
AxAll previously
mentioned findingsNCSEMG

Treatment for UNEConservative treatment ie
avoid aggrevating factors Jt protectionElbow splintSurgical options
Transportation Decompression cubital
tunnel Medial epicondylectomy
Many will recover spontaneously but surgery very effective (Padua et al 2002)
90% of pt’s with mild symptoms will recover with conservative Rx (Robertson & Saratsiotis 2005)
Ulnar nerve transportation

Ulnar nerve compression at the wrist
Similar manifestation with weakness of the hand intrinsics and thenar and hypothenar eminences
Exacerbated by activities such as riding bike or manual labour that repetitively compresses ulnar side of the wrist and Guyon’s canal
#, trauma, ganglion cysts, ulnar artery thombus
May require MRI or CT for diagnosis as well as EMG and NCS
Conservative treatment usually successful but may require decompression if mass present

Radial Neuropathy at the Spiral Groove (Shapiro & Preston 2009)Saturday night palsyPresents with complete wrist
and finger dropNumbness in the lat dorsum
of the handAlso weak supination and
elbow flexElbow ext normalFinger abd should be
unaffected (must be tested in neutral)
Triceps reflex normalBrachioradialis reflex
reduced or absent

Radial nerve entrapment cause.Radial nerve lies in
juxtaposed to spiral groove making it liable to compression
Prolonged compression leads to demylination
Can result from # humerus, vasculitis or stenuous muscle effort

Differential diagnosisRadial nerve compression
other sites i.e. Axilla
Posterior interosseous neuropathy (PIN)
Posterior cord radial plexus lesion
Unusual C7 radiculopathy
Central lesion
Will result in reduced elbow ext and numbness ext post forearm and upper arm
Radial dev during wrist extNo loss of reflexes
Weak lat dorsi and deltoid and weak all
Weak C7 innervated muscles including pronation and wrist flex
UMN S&S

Diagnosis and TreatmentEMG and NCS
should be done to define location of entrapment
High resolution US thought to be accurate (Lo et al, 2008; Bianchi, 2008)
Treatment usually conservative
Protection (proper crutch use)
Wrist splintRecovery depends on
demylination (several weeks) or axonal damage (several months to > 1 year)
Surgery for ongoing symptoms

Suprascapular NeuropathyAldridge et al, 2001
Presents insidious onset wasting over infra and suraspinatus
Inability to lat rot / abduct (Pt may be unaware)
Pain post sh and on palpCommon in weight liftersNerve trapped in
suprascapular notch beneath transverse scapular lig
Less common entrapment at spiroglenoid notch

Causes Suprascap nerve entrapmentCertain activities
which i.e. throwing, dancing, lifting
Ganglions, sarcoma, carcinoma
Surgical positioningDirect trauma

Differential diagnosis DiagnosisC5-6 radiculopathy
Neck painReduced biceps and
brachiorad reflexWeakness other C5-6
innervated musclesSensory changes
Brachial plexopathyAs above no neck pain
Rotator cuff tearMOIMay be difficult to
differentiate
EMG and NCSUS to differentiate rot
cuff injury
TreatmentConservative i.e stop
offending activitySurgery especially if
mass identifiedConservative and
surgical treatment equally effective usually

Peroneal Neuropathy at the Fibular HeadUsually involves both
deep and superficial peroneal nerves
Therefore weakness in ankle df and eversion
Sensory loss over dorsum of the foot and lat calf
May be pain and Tinel’s over fib neck
Ankle inversion spared as innervated by Tib nerve.

Causes
Habitual leg crossingRepetitive stretch from squattingThin pt’s Ganglions etcAssociated to ankle inversion injury including
# fibTraction to nerveProlonged immobilisation (especially sedated
pt’s)

Differential Diagnosis DiagnosisSciatic neuropathyL5 radiculopathy
Both identifiable by sensory changes lat knee and/or under/lat foot
Weak inversionReduce reflexes
CRPS
EMG and NCSMRI’s in slowly
progressing to check for masses

Treatment (Shapiro&Preston 2009; Williams&Robinson 2009)Can be injectedAFOStretches to prevent
contracturesGait rehabProprioceptive workEliminate offending
activities ie leg crossingSurgery rarely needed
except where extensive nerve damage or mass present

Meralgia Paresthetica (Williams and Trizl, 1991; Grossman et al, 2001)Classic presentation of
lateral femoral cutaneous neuropathy is burning and numbness lat thigh with no reduction in reflexes or motor power
Lat fem cutaneous nerve purely sensory
From L2-3 passes under inguinal lig
My also be hypersensitiveSymptoms may be
exacerbated by walking/standing and relieved by hip flex
Positive tenderness or Tinel’s at Inguinal lig

Causes Differential DiagnosisIdiopathicObesity Tight underwear,
wearing tool beltDMAbdominal aortic
aneurysm TumoursPregnancyPost surgeryRarely caused by
trauma
Femoral neuropathyLumbar plexopathyLumbar radiculopathy
Usually numbess less well defined
Reduce reflexWeaknessDiagnosis usually
clinical as EMG not good for these pt’s. MRI if mass suspected

TreatmentUsually time limitedReduce causitive
factor (tight clothes)Lose weightHave babyLocal steroid injNSAID’sProlonged symptoms
may require anaesthetic creams/patches
Tricyclic, anticonvulsants, anti depressants
Surgery decompression or transection
Conservative treatment successful in 91% cases
Surgical treatment successful in 95% cases

Tarsal Tunnel Syndrome and Plantar Heel/Foot pain (Alishami et al, 2008) Compression of the tibial
nerve branches under the flexor retinaculum
Pain medial ankle, burning, numbness, tingling under foot
More common women than men
Worst with weight bearingPossible wasting of intrinsics
in footTinel’s positive in tarsal
tunnelReduced light touch on soles
of foot

CausesIrritation to medial or
lateral plantar nerve or medial calcaneal nerve
IdiopathicAnkle sprain/#RA/Degenerative jt
diseaseDMHypothyroidismVV => compressionGanglionRepetitive jogging/wt
bearing

PresentationAlways pain abductor
hallucisPain after rest
particularly morningPain may radiate
distally with palp of nerve (should not in plantar fascitis)
Pain may easy with walking
Reduce d sensation over medial sole

Differential DiagnosisPlantar Fascitis
DF with eversion then SLR
Tinel’s not +ve in pfEMG/NCSHigh resolution US
Fat pad atrophyMore pain over fat
padVisible loss of fat
pad
Proximal nerve lesionCheck LspTibial nerve
entrapment in popliteal fossa

TreatmentGood evidence very
limitedRestNSAID’sSteroid InjectionsHeel padsOrthosesStretching exercises
for PF and calfAND techniques
Surgery to decompress is a last option and should only be considered if conservative treatment has failed for 6-12 months

Interdigital neuropathyMorton’s Neuroma (Cochranes review, 2011; Williams & Robinson, 2009))Compression of the
Plantar digital nerves in the space between the metatarsal heads
Usually 3rd space followed by 2nd and rarely 1st or 4th space
Can give pain which is debilitating as mobility severely limited
Pain often relieved by removing tight footwear
May be accompanied by numbness of toes adjacent to pain

Cause Differential DiagnosisMost likely etiology
is repetitive compression of common plantar digital nerve between MT heads and the transverse metatarsal lig.
TTSCan be very difficult
to differentiatePlantar fascitisTMT OA
Both of these will have no neurological S&S
Also compression of the MT heads should not be exquisitely painful

Diagnosis TreatmentEMG/NCS may help
exclude other peripheral nerve or Nerve root problems
MRI may be of more benefit but can often pick up none clinically relevant lesions
US good for predicting size of neuroma (92% Sens 100% Spec)
No good evidenceConservative
treatment helps 50%InsolesStop offending
activitiesSteroid injAlcohol inj x4Physio (not specified)
Surgery neurectomy/neurolysis (variable outcomes)

SummaryLots of nerve root entrapmentsLocation of entrapment very important in
symptomsDifferentiation relies on multiple symptomsConsider could neuropathy be adding to
symptoms/preventing/slowing recovery
Questions?
THE END
Related Documents