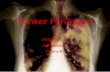
CHAPTER 1 BACKGROUND 1.1 Background Pleural effusions (liquid in the pleural space), which occur less frequently in children than in adults, can be caused by a variety of infectious and noninfectious diseases. Causes of pleural effusions in children differ significantly from those in adults. Among adults, the most frequent cause is congestive heart failure (transudate), and bacterial pneumonia and malignancy are the most frequent causes of exudate. Pleural effusions in children most commonly are infectious (50% to 70% parapneumonic effusion); congestive heart failure is a less frequent cause (5% to 15%), and malignancy is a rare cause. 1 Parapneumonic effusion and empyema have an incidence of 3.3 per 100.000 children. It has been suggested that the incidence of childhood empyema increased in the UK, although this is not a universal finding. It is not clear whether this is related to different referral patterns, changes of antibiotic usage in primary care, or whether it was a genuine increase in disease incidence. 2

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

CHAPTER 1
BACKGROUND
1.1 Background
Pleural effusions (liquid in the pleural space), which occur less frequently in children than in adults, can be caused by a variety of infectious and noninfectious diseases. Causes of pleural effusions in children differ significantly from those in adults. Among adults, the most frequent cause is congestive heart failure (transudate), and bacterial pneumonia and malignancy are the most frequent causes of exudate. Pleural effusions in children most commonly are infectious (50% to 70% parapneumonic effusion); congestive heart failure is a less frequent cause (5% to 15%), and malignancy is a rare cause.1
Parapneumonic effusion and empyema have an incidence of 3.3 per
100.000 children. It has been suggested that the incidence of childhood
empyema increased in the UK, although this is not a universal finding. It is not
clear whether this is related to different referral patterns, changes of antibiotic
usage in primary care, or whether it was a genuine increase in disease
incidence.2
Parapneumonic effusion is defined as fluid in the pleural space in the
presence of pneumonia, lung abscess, or bronchiectasis. Nontuberculous
bacterial pneumonia constitutes the most frequent origin of pleural effusion in
children. Establishing a specific causative agent depends on the patient’s age,
underlying disease, standard of laboratory culture method, and initiation of
antibiotic therapy. Staphylococcus aureus is the single most common pathogen
causing empyema (29% to 35% of cases), especially among infants younger
than 2 years of age. Streptococcus pneumoniae is the cause in up to 25% of
cases of empyema. Haemophilus influenzae is a less frequent pathogen but still

is significant in the development of parapneumonic effusion in children up to 5
years of age.1
CHAPTER 2
LITERATURE REVIEW
2.1. Pleural Effusions
2.1.1 Definition
Pleural effusions are accumulations of fluid within the pleural space. They have multiple causes and usually are classified as transudates or exudatesNormally, 10 to 20 mL of pleural fluid, similar in composition to plasma but lower in protein (< 1.5 g/dL), is spread thinly over visceral and parietal pleurae, facilitating movement between the lungs and chest wall. The fluid enters the pleural space from systemic capillaries in the parietal pleurae and exits via parietal pleural stomas and lymphatics. Pleural fluid accumulates when too much fluid enters or too little exits the pleural space.
2.1.2 Etiology
Pleural effusions are usually categorized as transudates or exudates based on laboratory characteristics of the fluid. Whether unilateral or bilateral, a transudate can usually be treated without extensive evaluation, whereas the cause of an exudate requires investigation. There are numerous causes seen in the table below.
Transudative effusions are caused by some combination of increased hydrostatic pressure and decreased plasma oncotic pressure. Heart failure is the most common cause, followed by cirrhosis with ascites and by hypoalbuminemia, usually due to the nephrotic syndrome.
Exudative effusions are caused by local processes leading to increased capillary permeability resulting in exudation of fluid, protein, cells, and other serum constituents. Causes are numerous; the most common are pneumonia, cancer, pulmonary embolism, viral infection, and TB. Yellow nail syndrome is a rare disorder causing chronic exudative pleural effusions, lymphedema, and dystrophic yellow nails—all thought to be the result of impaired lymphatic drainage.
Cause CommentsTransudateHeart failure Bilateral effusions in 81%; right-sided in 12%; left-sided

Cause Commentsin 7%
With left ventricular failure, there is increased interstitial fluid, which crosses the visceral pleura and enters the pleural space
Cirrhosis with ascites (hepatic hydrothorax)
Right-sided effusions in 70%; left-sided in 15%; bilateral in 15%
Ascitic fluid migration to the pleural space through diaphragmatic defects
Effusion present in about 5% of patients with clinically apparent ascites
Hypoalbuminemia
Uncommon
Bilateral effusions in > 90%
Decreased intravascular oncotic pressure causing transudation into the pleural space
Associated with edema or anasarca elsewhere
Nephrotic syndromeUsually bilateral effusions; commonly subpulmonic
Decreased intravascular oncotic pressure plus hypervolemia causing transudation into the pleural space
Hydronephrosis Retroperitoneal urine dissection into the pleural space, causing urinothorax
Constrictive pericarditis
Increases IV hydrostatic pressure
In some patients, accompanied by massive anasarca and ascites due to a mechanism similar to that for hepatic hydrothorax
Atelectasis Increases negative intrapleural pressure
Peritoneal dialysisMechanism similar to that for hepatic hydrothorax
Pleural fluid with characteristics similar to dialysate
Trapped lungEncasement with fibrous peel increasing negative intrapleural pressure
May be exudative or borderline effusion
Systemic capillary leak syndrome
Rare
Accompanied by anasarca and pericardial effusionMyxedema Effusion present in about 5%

Cause CommentsUsually transudate if pericardial effusion is also present; either transudate or exudate if pleural effusion is isolated
Exudate
Pneumonia (parapneumonic effusion)
May be uncomplicated or loculated and/or purulent (empyema)
Thoracentesis necessary to differentiate
Cancer
Most commonly lung cancer, breast cancer, or lymphoma but possible with any tumor metastatic to pleurae
Typically causing dull, aching chest pain
Pulmonary embolism
Effusion present in about 30%:
Almost always exudative; bloody in < 50%
Pulmonary embolism suspected when dyspnea is disproportionate to size of effusion
Viral infection
Effusion usually small with or without parenchymal infiltrate
Predominantly systemic symptoms rather than pulmonary symptoms
Coronary artery bypass surgery
Effusions left-sided or larger on the left in 73%; bilateral and equal in 20%; right-sided or larger on the right in 7%
> 25% of the hemithorax filled with fluid 30 days postoperatively in 10% of patients
Bloody effusions related to postoperative bleeding likely to resolve
Nonbloody effusions likely to recur; etiology unknown but probably with an immunologic basis
TB
Effusion usually unilateral and ipsilateral to parenchymal infiltrates if present
Effusion due to hypersensitivity reaction to TB protein
Pleural fluid TB cultures positive in < 20%Sarcoidosis Effusion in 1–2%
Extensive parenchymal sarcoid and often extrathoracic

Cause Comments
sarcoid
Pleural fluid predominantly lymphocytic
Uremia
Effusion in about 3%
In > 50%, symptoms secondary to effusion: Most commonly fever (50%), chest pain (30%), cough (35%), and dyspnea (20%)
Diagnosis of exclusion
Infradiaphragmatic abscess
Causes sympathetic subpulmonic effusion
Neutrophils predominant in pleural fluid
pH and glucose normal
HIV infection
Many possible etiologic factors: Pneumonias (parapneumonic), including Pneumocystis jirovecii pneumonia, other opportunistic infections, TB, and pulmonary Kaposi sarcoma
RAEffusion typically in elderly men with rheumatoid nodules and deforming arthritis
Must differentiate from parapneumonic effusion
SLE
Effusion possibly first manifestation of SLE
Common with drug-induced SLE
Diagnosis established by serologic tests of blood, not of pleural fluid
DrugsMany drugs, most notably bromocriptine, dantrolene, nitrofurantoin, IL-2 (for treatment of renal cell cancer and melanoma), and methysergide
Ovarian hyperstimulation syndrome
Syndrome occurring as a complication of ovulation induction with human chorionic gonadotropin (hCG) and occasionally clomiphene
Effusion developing 7–14 days after hCG injection
Effusion right-sided in 52%; bilateral in 27%Pancreatitis Acute: Effusion present in about 50%: Bilateral in 77%;
left-sided in 16%; right-sided in 8%
Effusion due to transdiaphragmatic transfer of the

Cause Comments
exudative inflammatory fluid and diaphragmatic inflammation
Chronic: Effusion due to sinus tract from pancreatic pseudocyst through diaphragm into pleural space
Predominantly chest symptoms rather than abdominal symptoms
Patients presenting with cachexia that resembles cancer
Superior vena cava syndrome
Effusion usually caused by blockage of intrathoracic venous and lymphatic flow by cancer or thrombosis in a central catheter
May be an exudate or a chylothorax
Esophageal rupture
Patients extremely sick
Medical emergency
Morbidity and mortality due to infection of the mediastinum and pleural space
Benign asbestos pleural effusion
Effusion occurring > 30 yr after initial exposure
Frequently asymptomatic
Tends to come and go
Must rule out mesothelioma
Benign ovarian tumor (Meigs syndrome)
Mechanism similar to that for hepatic hydrothorax
Surgery sometimes indicated for patients with ovarian mass, ascites, and pleural effusion
For diagnosis, disappearance of ascites and effusion postoperatively required
Yellow nail syndrome
Triad of pleural effusion, lymphedema, and yellow nails, sometimes appearing decades apart
Pleural fluid with relatively high protein but low LDH
Tendency for effusion to recur
No pleuritic chest pain

Effusions with no obvious cause are often due to occult pulmonary emboli, TB, or cancer. Etiology is unknown for about 15% of effusions even after extensive study; many of these effusions are thought to be due to viral infection.
2.1.3 Clinical manifestation
Respiratory symptoms in the presence of fluid in the pleural space are common in children. When the underlying cause is pneumonia, the predominant symptoms are cough, fever, chills, and dyspnea. If the effusion is not associated with pneumonia, the child may be asymptomatic until the effusion becomes sufficiently large to cause dyspnea or orthopnea. Children who have neurologic impairments are more likely to aspirate secretions or gastric content and develop anaerobic infections, which cause a more insidious onset of pneumonia and effusion. Older children may complain of a sharp pleuritic pain with inspiration or cough, which is due to stretching of the parietal pleura. As the effusion increases and separates the pleural membranes, pleuritic pain becomes a dull ache and disappears. Specific signs indicating pleural effusion are much more difficult to elicit in the infant or the young child. Dullness to percussion and decreased breath sounds over the affected area almost always are present, but they can be difficult to perceive if the effusion is small. In infants, breath sounds from one lung often are transmitted throughout the chest, making unilateral findings difficult to appreciate. A pleural rub, due to roughened pleural surfaces, can be present in the early phase, but it disappears as fluid accumulates. Decreased vocal fremitus and fullness of the intercostal spaces can be detected. Expectoration of purulent sputum may herald the onset of bronchopleural fistula and ensuing pyopneumothorax. Findings of chest wall abscess and costal chondritis indicate extension of the process (ie, empyema necessitatis). Decreased heart tones and pericardial rub indicate extension to the pericardium.
2.1.4 Staging
In children, parapneumonic effusion due to subpleural infectious pneumonia
is the most common cause of pleural effusion. There are three stages associated
with parapneumonic effusion that may overlap:
- Exudative stage: the inflammatory process associated with the underlying
pneumonia leads to the accumulation of clear fluid with a low white cell
count within the pleural cavity (simple parapneumonic effusion).

- Fibropurulent stage: there is deposition of fibrin in the pleural space leading
to septation and the formation of loculations. There is an increase in white
cells, with the fluid thickening (complicated parapneumonic effusion) and
eventually becoming overt pus (empyema). The presence of septations
(fibrinous strands within the pleural fluid) does not necessarily mean the fluid
does not flow freely, although separate loculations will not communicate with
each other.
- Stage of Organization: fibroblasts infiltrate the pleural cavity, and the thin
intrapleural membranes are reorganised to become thick and non-elastic (the
‘peel’). These solid fibrous pleural peels may prevent lung re-expansion
(trapped lung), impair lung function, and create a persistent pleural space with
ongoing potential for infection. At this stage spontaneous healing may occur
or a chronic empyema may develop.
2.1.5 Diagnosis
Tests may need to be ordered to rule out immune dysfunction or other underlying systemic or local pulmonary disorders that cause empyema.
Analysis of the pleural fluid is the single best method to determine the cause of a pleural effusion. Thoracentesis should be performed when sufficient fluid is present to allow a safe procedure, except when the suspected effusion is clearly secondary to a specific underlying disease (for example, congestive heart failure, nephrotic syndrome, ascites, or recent initiation of peritoneal dialysis).
Simple observation of the gross appearance of the fluid may provide a clue as to the cause of the pleural effusion, as follows:
Grossly purulent fluid indicates an empyema A putrid odor suggests an anaerobic empyema
Clear, pale yellow fluid suggests a transudate
Milky fluid is consistent with a chylothorax
Bloody pleural fluid is seen with trauma, malignancy, tuberculosis, uremia, and empyema due to group A Streptococcus
Aspergillus nigrans infection produces a black pleural fluid

In the appropriate clinical setting, measurement of pleural fluid triglyceride levels (chylous effusion), amylase (pancreatitis, esophageal rupture), and pleural fluid hematocrit (hemothorax) may be useful.
A complete blood count (CBC) with differential, blood cultures, and C-reactive protein (CRP) may help to establish the presence of infection. The white blood cell (WBC) count and CRP may be useful in monitoring treatment progress in infectious effusions. A positive blood culture finding may facilitate the selection of antibiotics in sterile empyema. (Approximately 10-22% of children with complicated parapneumonic effusions have a positive blood culture result.)
Measurement of titers may be helpful if specific organisms, such as Mycoplasma species, Legionella species, or adenovirus, are suspected. However, the use of these tests in early management of parapneumonic effusions is limited due to the need for convalescent titer.
If risk factors for tuberculosis are present, sputum (or gastric aspirates) for acid fast bacilli and a purified protein derivative (PPD) test should be performed.
Serum protein, LDH, amylase, glucose, and hydrogen ion concentration (pH) may be helpful in interpreting results of pleural fluid analysis. If chylous effusion is suspected, serum cholesterol and triglyceride levels should be obtained.
Exudate Versus Transudate
Conventionally, the initial evaluation of pleural fluid is directed at determining whether the effusion is an exudate or a transudate. The classification is based on simple biochemical criteria first proposed by Light et al. However, the Light criteria was developed and tested in adults, and its accuracy in children has been questioned.
According to the Light criteria, the pleural fluid is defined as an exudate if it fulfils at least one of 3 criteria. If none of the criteria are met, then the fluid is considered a transudate. The criteria are as follows:
Pleural fluid–to–serum lactate dehydrogenase (LDH) ratio of more than 0.6
Pleural fluid–to–serum protein ratio of more than 0.5
Pleural fluid LDH level of two thirds the upper limit of the reference range
In general, exudates have protein concentration higher than 2.9 g/dL, with the pleural fluid cholesterol level more than 45 mg/dL.
Biochemical analysis of the pleural fluid provides further information that may be useful in narrowing the differential diagnosis of exudative effusion, as follows:

Low pleural glucose level (< 60 mg/dL) or pleural fluid–to–serum glucose ratio of less than 0.5 - Seen in several conditions, such as parapneumonic effusion, tuberculosis, malignancy, esophageal rupture, and rheumatoid effusions
LDH levels of more than 1000 IU/L - Found in empyema and rheumatoid effusions
Pleural fluid–to–serum LDH ratio of 1 and pleural fluid–to–serum protein ratio less than 0.5 -Suggest effusion due to P jiroveci pneumonia
Pleural fluid pH below 7.3 (with normal arterial pH) - Seen in parapneumonic effusion, tuberculosis, malignancy, esophageal rupture, systemic acidosis, urinothorax, and rheumatoid effusions; most exudative effusions have a pH of 7.3-7.45, whereas transudates have a pleural fluid pH ranging from 7.4-7.55 (the pH of normal pleural fluid is about 7.6).

*Based on presence of fever, weight loss, history of cancer, or other suggestive symptoms.

2.1.6 Treatment
Most pediatric patients who have uncomplicated parapneumonic effusion
respond well to appropriate antibiotic therapy and do not require tube
thoracostomy. The treatment of empyema (complicated parapneumonic effusion)
in children begins with conservative therapy. The initial treatment is
administration of antibiotics directed at the underlying infection and drainage of
infected fluid by thoracentesis or by closed thoracostomy tube. Antibiotics should
be selected (Table 3) to cover the most common pathogens for pneumonia for the
child’s age group. Until the condition is diagnosed, broad-spectrum antibiotics are
warranted due to the high morbidity and mortality associated with empyema.
Intravenous antibiotics should be continued until the child is afebrile for at least 7
to 10 days, has been weaned from supplemental oxygen, and no longer appears ill.
Oral antibiotics subsequently are administered for 1 to 3 weeks.
Tabel 1 Common organism causing Parapneumonic effusion in children and
corresponding empiric antibiotic therapy
Age Predominant pathogens Therapy
0 to 6 mon Gram-negative rods*
Staphylococcus aureusStreptococcus
Nafcillin, gentamicin, and
ampicilin
7 to 12 mon Haemophilus influenzaePneumococcusStreptococcus
Nafcilin and cefuroxime
13 to 24 mon H. InfluenzaePneumococcusS. aureus
Cefuroxime, clindamycin
2 to 5 y H InfluenzaePneumococcusS. aureusStreptococcusAnaerobes
Cefuroxime and clindamycin
or imipenem
6 to 12 y PneumococcusS. aureusStreptococcusAnaerobes
Cefuroxime and clindamycin
or imipenem

13 to 18 y PneumococcusS. aureusAnaerobes
Nafcilin or cefuroxime plus
clindamycin
* Pseudomonas, Eschericia coli, Proteus, Klebsiella
Prompt drainage of the empyema prevents the development of loculation
and fibrous peel. Further, at the second stage of disease, tube drainage becomes
less effective. Whether all empyemas require drainage remains controversial; no
data in children clearly establish criteria. Generally, immediate closed-tube
thoracostomy should be considered strongly with the following:
● Pleural fluid pH is less than 7.2 or more than 0.05 units below the arterial pH
● Pleural fluid glucose is less than 40 mg/dL (2.2 mmol/L)
● Pleural fluid LDH is greater than 1,000 U/L
● Presence of frank pus
● Positive Gram stain
● Sepsis due to S aureus or H influenzae
When the chest tube drainage reaches less than 30 to 50 mL/d and the patient’s
constitutional symptoms improve, the chest tube may be removed.
Another effective therapy is introduction of streptokinase (SK) or urokinase
(UK) into the empyema cavity, which has been shown to lyse adhesions, enhance
drainage, and resolve the symptoms. SK is a bacteria-derived protein that
indirectly activates the fibrinolytic system. Problems associated with this regimen
include allergic reactions and antibody neutralization of the SK. UK is a direct
plasminogen activator. Unlike SK, there is a one to one relationship of plasmin
production for each molecule of UK, making more efficient use of pre-existing
plasminogen. UK is not antigenic. Studies have documented complete resolution
of fluid collection with persistent loculated fluid following instillation of UK into
the chest tube. No complication occurred in either series. Basic indications for UK
in pleural effusion include:
● Poor drainage despite an appropriately positioned chest tube
● Multiple loculi, as depicted by septation on ultrasonography or CT

● Presumed multi loculi, as indicated by initial drainage of a volume far less than
expected by imaging studies
2.1.7 Complication
Complications are uncommon in properly treated parapneumonic effusions. Possible complications include respiratory failure caused by massive fluid accumulation, septicemia, bronchopleural fistula, pneumothorax, and pleural thickening.
2.1.8 Prognosis
Children who have uncomplicated parapneumonic effusion respond well to conservative management with no apparent residual lung damage. Viral and mycoplasmal pleural disease generally resolve spontaneously. Patients who have empyema have more prolonged and complicated hospital courses. Virtually no deaths should occur with prompt therapy. Case fatality rates of 3% to 6% have been reported in some recent series, with the highest rate occurring among infants younger than 1 year of age. In contrast to adults, infants and children have a remarkable ability to resolve pleural thickening with no effect on subsequent lung growth and lung function.

CHAPTER III
CASE REPORT
3.1 Objective
The objective of this paper is to report a case of 1 years and 3 months old
boy with a diagnosis of pleural effusion.
3.2 Case
A, a 1 years and 3 months boy, with 9 kg of BW and 96 cm of BH, is a
new patient of infection unit in Pediatric Department in Central Public Hospital
Haji Adam Malik Medan on September 6th 2015 at 19.30. His chief complaint was
dyspnea/shortness of breath
.
History of disease:
A, a boy, 1 years and 3 months old, came to Haji Adam Malik Hospital on
September 6th 2015 with dyspnea as the chief complaint. The patient have been
experiencing this for the past 2 days. Dyspnea is not associated with weather or
activity. Patient also experienced cough (+) since 1 weeks ago with the production
of sputum (+) but hard to be expelled. Flu (+) for the past 1 week. Fever (+) since
1 weeks ago, rises and drop and hard to be reduced with fever medication. Perut
kembung (+) is noticed by the mother for the past 2 days. History of contact to
patient with prolonged cough (-). History of allergy (-). Nausea (-), Vomiting (-),
Diahreoa (-). Urine and faeces (+) normal.
History of previous illness: The patient is referred from RS Pertamina Brandon
with dd of URTI, bronchiolitis, nephrotic syndrome and GNA.
History of medication: IVFD RL, Inj. Viccilin, Inj.Novalgin, Inj.Gentamicin,
Sanmol Syrup,amborox syrup,nebule ventolin
History of family: No family history of DM and other diseases
History of parent’s medication: unclear
History of pregnancy: The gestation age was 36 weeks. No history of

complication, neonate and maternal problem.
History of birth: Birth assisted by midwife spontaneously. The baby was born
pervaginal and she cried immediately. Bluish was not found.
Body weight 3900 gram, body length 50 cm, and head
circumference was not measured.
History of feeding: Breast feeding from born till now, additional food since 2
months old.
History of immunization: BCG, Polio, Hepatitis B. Immunization is not
complete
History of growth and development: Face down: 4 months old, Sit down: 6
months old, Crawl: 8 months old, Stand
up: 10 months old, Walk: 13 months old,
Talk: 12 months old.
Physical Examination:
Present status: Level of consciousness: Consious, Body temperature:
37.8°C, BP: 100/90 mmHg, HR: 130 bpm, RR: 40 bpm, BW: 9 kg, BH: 76
cm, anemic (+), icteric (-), dyspnea (+), cyanosis (-), edema (-).
Localized status:
Head :Eyes: Light reflex +/+, isochoric pupil,
pale was found in inferior conjunctiva palpebral.
Ears: within normal range
Nose: Nostril breathing
Mouth:within normal range
Neck :Lymph node enlargement (-)
Thorax : Symmetrical fusiform, retraction (+) epigastrial, Cor
S1,S2reguler, Weak breathing sound on the left lung.
HR: 136 bpm, regular, murmur (-)
RR: 48 bpm, regular, rhonchi (+/+) wheezing (-/-), rales
(-/-)
Abdomen : Supple, normal peristaltic, liver normal

Extremities : pulse 136 bpm regular, p/v adequate, warm acral, CRT <
3”, clubbing finger(-).
Working diagnosis : Left pleural effusion + suspect of sepsis
Laboratory finding
Complete blood analysis (September 6th , 2015)
Test Result Unit Referral
Hemoglobin 8.10 g% 12.0-14.4
Erythrocyte 3.43 106/mm3 4.40-4.48
Leucocyte 39.53 103/mm3 4.5-13.5
Thrombocyte 536 103/mm3 150-450
Hematocrite 25.80 % 37-41
Eosinophil 0.30 % 1-6
Basophil 1.300 % 0-1
Neutrophil 66.20 % 37-80
Lymphocyte 23.40 % 20-40
Monocyte 9.20 % 2-8
Neutrophil absolute 11.41 103/µL 2.4-7.3
Lymphocyte absolute 4.99 103/µL 1.7-5.1
Monocyte absolute 1.39 103/µL 0.2-0.6
Eosinophyl absolute 0.18 103/µL 0.10-0.30
Basophyl absolute 0.16 103/µL 0-0.1
MCV 75.20 fL 81-95
MCH 23.60 Pg 25-29

MCHC 31.40 g% 29-31
RDW 15.70 % 11.6-14.8
Morphology: Erythrocyte: anemia hipokrom microcyte
Leukocyte: leukocytosis
Trombocyte: trombocytosis
Clinical Chemistry
Test Result Unit Referral
Carbohydrate Metabolism
Blood Glucose 87.10 mg/dL < 200
Electrolite
Natrium 132 mEq/L 135-155
Kalium 3.8 mEq/L 3.6-5.5
Chloride 101 mEq/L 96-106
Blood Arterial Gas Analyse
Ph 7.430 7.35-7.45
pCO2 30.0 mmHg 38-42
pO2 193.0 mmHg 85-100
Bicarbonate (HCO3) 19.9 mmol/L 22-26
Total CO2 20.8 mmol/L 19-25
base excess -3.9 mmol/L (-2)– (+4)

O2 Saturation 100.0 mmol/L 95-100
Therapy :
1. O2 nasal canule 1 liter/i
2. IVFD D5% Nacl 0,45% 4cc/hour
3. Inj Ceftriaxon 450 mg/12 jam /iv skin test
4. Paracetamol 3x120mg
5. Diet Peadsure 100cc/3hour/NGT
6. Correction of hipoalbuminemia
7. Consul to the respirology division

Follow Up:6th September 2015
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 38,1 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale +/+, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 136x/i, systolic murmur(-), RR: 48x/i, Ronchi -/-, Slem (+/+)Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 120x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i- IVFD D5% 4cc/
jam- Inj. Ceftriaxone 450
mg / 12 jam / IV- Paracetamol Syr. 3
x cth I (120 mg)- Diet pediasure 100
cc / 3 jam/ NGT- Hipoalbuminemia
correction- Consul respirology
divisionDipstick Urine result
7th September 2015
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 38,3 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale +/+, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 126x/i, systolic
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i- IVFD D5% 4cc/
jam- Inj. Ceftriaxone 450
mg / 12 jam / IV- Paracetamol Syr. 3
x cth I (120 mg)- Diet pediasure 100
cc / 3 jam/ NGT- Hipoalbuminemia
correction

murmur(-), RR: 44x/i, Ronchi -/-, Slem (+/+)Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 120x/i, regular, adequate pressure and volume, warm, CRT < 3’’
8th September 2015
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 39,8 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 120x/i, systolic murmur(-), RR: 42x/i, Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 120x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i
- IVFD D5% 4cc/ jam
- Inj. Ceftriaxone 450 mg / 12 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jam/ NGT

9th September 2015 – 10th September
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 37,6 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 120x/i, systolic murmur(-), RR: 40x/i, Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 120x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i
- Threeway- Inj. Ceftriaxone
450 mg / 12 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jam/ NGT
11 September 2015
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 37,8 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 110x/i, systolic
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i
- Threeway- Inj. Ceftriaxone
450 mg / 12 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jam/ NGT

murmur(-), RR: 40x/i, Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 116x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Mantoux result: Induration 0 mm
12 September 2015 – 13 September 2014
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 38,6 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (-),weaken breathing sound on left lung, HR: 110x/i, systolic murmur(-), RR: 40x/i, Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 116x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i
- Threeway- Inj. Ceftriaxone
450 mg / 12 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jam/ NGT

14 September 2015
S O A P
Dyspnea (+), cough (+), fever (+)
Sensorium: CM, T: 38,3 oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (+), epigastrial, weaken breathing sound on left lung, HR: 110x/i, systolic murmur(-), RR: 40x/i, Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 116x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Left pleural effusion + Susp. Sepsis
- O2 nasal kanul 1l/i
- Threeway- Inj. Ampicilin
450mg/6jam/IV- Inj. Ceftriaxone
450 mg / 12 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jamKeluar hasil kultur : Klebsiella pneumoniaAntibiotik Inj.Ceftiaxon changed to Inj.Meropenem 350 mg/8jam/IV
15 September 2015
S O A P
Dyspnea (+), cough (+), fever (-)
Sensorium: CM, T: 37,1oC, BW: 9 kg BH: 76cm
Head: eye reflect +/+, conj palpebral inferior pale -/-, mouth/nose/ear: normal.
Neck: JVP R+2 H2O
Thorax: symetris fusiformis, retraction (-), weaken breathing sound on left lung, HR: 110x/i, systolic murmur(-), RR: 40x/i,
Left masif pleural effusion + Sepsis ec Klebsiella pneumonia
- O2 nasal kanul 1l/i
- Inj. Meropenem 350 mg / 8 jam / IV
- Paracetamol Syr. 3 x cth I (120 mg)
- Diet pediasure 100 cc / 3 jam/ NGT

Ronchi -/-.Abdomen: Seopel, Normal peristaltic, Hepar unpalpable, Lien: unpalpable.
Extremities: Pulse: 116x/i, regular, adequate pressure and volume, warm, CRT < 3’’
Related Documents