Interventions for Clients with Pituitary and Adrenal Gland Problems

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
- Slide 1
- Interventions for Clients with Pituitary and Adrenal Gland Problems
- Slide 2
- Hormones secreted from the anterior pituitary gland regulate growth, metabolism, and sexual development. These functions are affected when the pituitary gland secretes too much or too little of one or more hormones The posterior pituitary gland secretes vasopressin (antidiuretic hormone [ADH]). Dysfunction of the posterior pituitary gland results in fluid and electrolyte imbalance The adrenal gland produces and secretes hormones that influence homeostasis and are life sustaining
- Slide 3
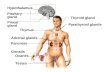
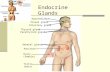
- DISORDERS OF THE PITUITARY GLAND The anterior pituitary gland (adenohypophysis) controls growth, metabolic activity, and sexual development through the actions of the following hormones: Growth hormone (GH; somatotropin) Prolactin (PRL) Thyrotropin (thyroid-stimulating hormone [TSH]) Corticotropin (adrenocorticotropic hormone [ACTH]) Follicle-stimulating hormone (FSH) Luteinizing hormone (LH) Melanocyte-stimulating hormone (MSH)
- Slide 4
- DISORDERS OF THE PITUITARY GLAND Disorders of hormones secreted by the anterior pituitary gland can result from problems arising within the anterior pituitary gland itself (primary pituitary dysfunction) or from problems in the hypothalamus that change anterior pituitary function (secondary pituitary dysfunction) In either case, one or more hormones may be undersecreted (pituitary hypofunction) or oversecreted (pituitary hyperfunction)
- Slide 5
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Pathophysiology A person with hypopituitarism has a deficiency of one or more anterior pituitary hormones, resulting in metabolic abnormalities and sexual dysfunction Decreased production of all of the anterior pituitary hormones is an extremely rare condition known as panhypopituitarism Deficiencies of adrenocorticotropic hormone (ACTH) and thyroid-stimulating hormone (TSH) are the most life threatening because they result in a corresponding decrease in the secretion of vital hormones from the adrenal and thyroid glands
- Slide 6
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Deficiency of the gonadotropins (luteinizing hormone [LH] and follicle-stimulating hormone [FSH]hormones that stimulate the ovaries and testes to produce sex hormones) changes sexual function in both men and women In males, gonadotropin deficiency results in testicular failure, with decreased testosterone production from the Leydig cells and decreased or absent spermatogenesis from the seminiferous tubules. Decreased testosterone levels in males cause delayed onset of puberty and sterility In females, gonadotropin deficiency results in ovarian failure, amenorrhea, and infertility
- Slide 7
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Growth hormone (GH) deficiency changes tissue growth patterns indirectly. GH itself has little effect on tissues and cells. Rather, the presence of GH stimulates the liver to produce substances known as somatomedins These somatomedins, especially somatomedin (insulin-like growth factor-1 [IGF-1]), then enhance growth activities in cells and tissues. Somatomedin is responsible for bone and cartilage growth and maintenance
- Slide 8
- DISORDERS OF THE ANTERIOR PITUITARY GLAND. Hypopituitarism GH deficiency may be a result of insufficient production of GH, failure of the liver to produce somatomedins, or a failure of the cells or tissues to respond to the presence of the somatomedins GH deficiency in children leads to short stature and other manifestations of growth retardation GH deficiency in adults produces no obvious anatomic changes but does increase the rate of bone destructive activity, leading to thinner, more fragile bones
- Slide 9
- DISORDERS OF THE ANTERIOR PITUITARY GLAND. Hypopituitarism Etiology The cause of hypopituitarism varies Benign or malignant pituitary tumors can compress and destroy pituitary tissue. Pituitary function can be impaired by severe malnutrition or rapid loss of body fat, such as in people with anorexia nervosa (a disorder in which people see themselves as overweight and eat so little that excessive weight loss and starvation result) Poor circulation to the pituitary gland can cause hypoxia and infarction Idiopathic hypopituitarism may result in an isolated hormone deficiency, and often the cause is unknown
- Slide 10
- DISORDERS OF THE ANTERIOR PITUITARY GLAND. Hypopituitarism Postpartum hemorrhage is the most common cause of pituitary infarction, which results in decreased hormone secretion. This clinical problem is known as Sheehan's syndrome The pituitary gland normally enlarges during pregnancy, and when hypotension results from hemorrhage, ischemia and necrosis of the gland occur Usually this condition develops immediately postpartum, although some cases have occurred several years after delivery
- Slide 11
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism
- Slide 12
- Assessment Anterior Pituitary Hormones Growth hormone (GH) Decreased bone density Pathologic fractures Decreased muscle strength Increased serum cholesterol levels Gonadotropins Women: (luteinizing Amenorrhea hormone [LH], Anovulation folliclestimulating Low circulating estrogen levels hormone [FSH]) Breast atrophy Loss of bone density Decreased axillary and pubic hair Decreased libido Fine facial wrinkles
- Slide 13
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Men: Decreased facial hair Decreased ejaculate volume Reduced muscle mass Loss of bone density Decreased body hair Decreased libido Impotence Fine facial wrinkles
- Slide 14
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Thyrotropin Decreased circulating TSH levels (Thyroid-stimulating Decreased circulating thyroid hormone [TSH]) hormone levels Weight gain Intolerance to cold Scalp alopecia Hirsuitism Menstrual abnormalities Decreased libido Slowed cognition Lethargy
- Slide 15
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Adrenocorticotropic Decreased serum cortisol levels hormone (ACTH) Pale, sallow complexion Malaise and lethargy Anorexia Postural hypotension Headache Hypoglycemia Hyponatremia Decreased axillary and pubic hair (women)
- Slide 16
- DISORDERS OF THE GLAND. Hypopituitarism Posterior Pituitary Hormones Vasopressin (antidi- Diabetes insipidus uretic hormone Greatly increased [ADH]) urine output Low urine specific gravity (< 1.005) Hypovolemia Hypotension Dehydration Increased plasma osmolarity Increased thirst Output does not decrease when fluid intake decreases
- Slide 17
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Neurologic manifestations of hypopituitarism due to tumor growth often first occur as changes in visual perception The nurse evaluates the client's visual acuity, particularly peripheral vision, for changes or loss Bilateral temporal headaches are a common finding Other manifestations may include diplopia (double vision) and ocular muscle paralysis, limiting eye movement
- Slide 18
- DISORDERS OF THE ANTERIOR PITUITARY GLAND. Hypopituitarism Stimulation tests The presence of insulin in people with normal pituitary function causes an increased release of GH and ACTH. The stimulation test for either GH or ACTH assessment involves injecting the client with regular insulin (0.05 to 1 units/kg of body weight) and checking the circulating levels of GH and ACTH The stimulation test for TSH involves injecting thyrotropin- releasing hormone (TRH) and measuring the blood levels of thyroid hormones The stimulation test for LH and FSH involves administering gonadotropin-releasing hormone (GnRH). In people with no pituitary problems, this injection results in a peak release of LH and FSH within 15 to 45 minutes after the injection The stimulation test for PRL is the same as that for TSH
- Slide 19
- DISORDERS OF THE ANTERIOR PITUITARY GLAND. Hypopituitarism Pituitary abnormalities may cause changes in the sella turcica (the bony nest where the pituitary gland rests) that can be seen with skull x-ray studies Such changes may include enlargement, erosion, and calcifications in the area of the sella turcica as a result of pituitary tumors An angiogram may be indicated to rule out the presence of an aneurysm or congenital vascular malformations, especially before any surgical intervention
- Slide 20
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Interventions Management of the adult with hypopituitarism focuses on replacement of deficient hormones Men who have gonadotropin deficiency are treated with androgens (testosterone). The most widely used and most effective route of administration is intramuscular (IM), although use of transdermal testosterone patches is increasing Therapy isusually initiated with high-dose testosterone and is continued until virilization (presence of male secondary sex characteristics) is achieved. The dose may then be decreased, but therapy continues throughout life Androgen therapy is avoided in men with prostate cancer. Side effects of testosterone therapy include gynecomastia (the development of breast tissue in men), baldness, and prostatic hypertrophy
- Slide 21
- DISORDERS OF THE PITUITARY GLAND. Hypopituitarism Women who have gonadotropin deficiency receive hormone replacement with a combination of estrogen and progesterone administered at their menstrual cycle, which causes withdrawal bleeding The risk for hypertension or thrombosis (formation of blood clots in deep veins) is increased with estrogen therapy, especially among women who smoke For women who wish to become pregnant, clomiphene citrate (Clomid) may be given to induce ovulation. Menotropins in conjunction with human chorionic gonadotropin (hCG) are used to stimulate ovulation when therapy with clomiphene citrate has failed
- Slide 22
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism Hyperpituitarism is a condition of hormone oversecretion that occurs when a client has pituitary tumors or hyperplasias PRL-secreting tumors are the most common of the pituitary adenomas. Excessive PRL secretion inhibits the secretion of gonadal steroids and gonadotropins in men and women, resulting in galactorrhea (production of breast milk), amenorrhea, and infertility
- Slide 23
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism Overproduction of GH results in gigantism or acromegaly In the client with gigantism, the onset of GH hypersecretion occurs before puberty, which causes rapid proportional growth in the length of all bones In the client with acromegaly, excessive GH secretion occurs after puberty and produces increased skeletal thickness, hypertrophy of the skin, and enlargement of many visceral organs, such as the liver and heart
- Slide 24
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism
- Slide 25
- History The nurse obtains data about the client's age, gender, and family history The client is asked about any change in hat, glove, ring, or shoe size Fatigue and lethargy are common The client with excessively high GH levels may have backache and arthralgias (joint pain) in response to bone changes He or she is asked specifically about the presence of headaches and changes in vision The client with hypersecretion of PRL (hyperprolactinemia) often reports difficulties in sexual functioning The nurse asks women about menstrual changes (e.g., amenorrhea, irregular menses, and difficulty in achieving pregnancy) and about decreased libido or dyspareunia (painful intercourse) Men may report decreased libido and impotence
- Slide 26
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism History The nurse obtains data about the client's age, gender, and family history The client is asked about any change in hat, glove, ring, or shoe size Fatigue and lethargy are common The client with excessively high GH levels may have backache and arthralgias (joint pain) in response to bone changes He or she is asked specifically about the presence of headaches and changes in vision The client with hypersecretion of PRL (hyperprolactinemia) often reports difficulties in sexual functioning The nurse asks women about menstrual changes (e.g., amenorrhea, irregular menses, and difficulty in achieving pregnancy) and about decreased libido or dyspareunia (painful intercourse) Men may report decreased libido and impotence
- Slide 27
- Slide 28
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism
- Slide 29
- Suppression tests High circulating levels of glucose have a suppressive effect on the release of GH. In a suppression test, 100 g of oral glucose or 0.5 g/kg of body weight is given intravenously. GH levels are measured serially for up to 120 minutes. GH levels that do not fall below 5 ng/mL indicate a positive (abnormal) result Administration of intravenous (IV) cortisol in the form of dexamethasone (Decadron). This agent should result in suppression of ACTH. When ACTH production continues in the presence of dexamethasone administration, the client may have pituitary Cushing's disease
- Slide 30
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism Interventions NONSURGICAL MANAGEMENT DRUG THERAPY bromocriptine mesylate (Parlodel) 7.5 mg/day - stimulates dopamine receptors in the brain and inhibits the release of many pituitary hormones, most specifically GH and PRL RADIATION THERAPY SURGICAL MANAGEMENT
- Slide 31
- DISORDERS OF THE PITUITARY GLAND. Hyperpituitarism
- Slide 32
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Disorders of the posterior pituitary (neurohypophysis) are directly related to a deficiency or excess of the hormone vasopressin (antidiuretic hormone [ADH]) Two disorders associated with ADH deficiency or excess are diabetes insipidus and the syndrome of inappropriate antidiuretic hormone (SIADH)
- Slide 33
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Diabetes Insipidus Diabetes insipidus is a disorder of water metabolism caused by a deficiency of ADHeither a decrease in ADH synthesis or an inability of the kidneys to respond appropriately to ADH ADH deficiency results in the excretion of large volumes of dilute urine. Without the presence of ADH, the distal tubules and collecting ducts of the kidney remain impermeable to water. Thus water is excreted as urine rather than being absorbed in these areas, which leads to polyuria (excessive urination with loss of free water)
- Slide 34
- DISORDERS OF THE POSTERIOR PITUITARY GLAND ADH deficiency can be classified as nephrogenic, drugrelated, primary, or secondary Nephrogenic diabetes insipidus is an inherited disorder. The renal tubules do not respond to the actions of ADH, which results in inadequate water reabsorption by the kidney. The actual amount of hormone produced is not deficient. Primary diabetes insipidus is caused by a defect in the hypothalamus or pituitary gland, resulting in a lack of ADH production or release
- Slide 35
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Secondary diabetes insipidus results from tumors within or adjacent to the hypothalamus or pituitary gland, head trauma, infectious processes, surgical procedures (hypophysectomy), or metastatic tumors, usually from the lung or the breast. Less commonly, it is caused by brain hemorrhage, brain disease, or cerebral aneurysm Drug-related diabetes insipidus is caused by the administration of lithium carbonate (Eskalith, Lithobid, Carbolith) and demeclocycline (Declomycin). These drags can interfere with the kidneys' response to ADH
- Slide 36
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Assessment Most of the clinical manifestations of diabetes insipidus are related to dehydration The nurse notes the key symptoms of an increase in the frequency of urination and excessive thirst The client is asked about a history of any known etiologic factors, such as recent surgery, head trauma, or medication use (e.g., lithium) Although increased fluid intake usually prevents serious dehydration and volume depletion, the client who is deprived of fluids or who cannot increase oral fluid intake may experience shock caused by fluid loss and plasma hyperosmolality
- Slide 37
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Signs of dehydration, such as poor skin turgor and dry or cracked mucous membranes or skin, may be present in varying degrees *Occurs when access to water is limited and rapid dehydration results
- Slide 38
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Loss of free water produces expected changes in blood and urine tests. The initial step in diagnosis is to measure a 24-hour fluid intake and output. The amount of the client's food and fluid is not restricted during this measurement. Urine output must be more than 4 L during this period for diabetes insipidus to be diagnosed. The amount of urine excreted in 24 hours may vary from 4 to 30 L/day. Urine is dilute and therefore has a low specific gravity (less than 1.005) and low osmolality (50 to 200 mOsm/kg) Fluid deprivation and hypertonic saline tests are also used for diagnosis of the disorder
- Slide 39
- DISORDERS OF THE POSTERIOR PITUITARY GLAND
- Slide 40
- Interventions Medical management is aimed at controlling the symptoms of the disease through drag therapy. If only a partial deficit of ADH is present, effective control can be achieved with oral chlorpropamide or clofibrate. These drags increase the action of existing ADH and possibly have a direct stimulating effect on the production of ADH in the hypothalamus. They have some undesirable side effects, however, and are not used as often as synthetic vasopressin When ADH deficiency is severe, ADH is replaced in amounts sufficient to maintain water balance
- Slide 41
- DISORDERS OF THE POSTERIOR PITUITARY GLAND
- Slide 42
- Syndrome of Inappropriate Antidiuretic Hormone The syndrome of inappropriate antidiuretic hormone (SIADH) occurs when vasopressin (antidiuretic hormone [ADH]) is secreted even when plasma osmolality is low or normal SIADH is also known as the Schwartz-Bartter syndrome ADH continues to be released even when plasma is hyposmolar. Water is retained, which results in dilutional hyponatremia (a decreased serum sodium level due to dilution) and expansion of the extracellular fluid volume. The increase in plasma volume causes an increase in the glomerular filtration rate and inhibits the release of renin and aldosterone. The combined effect is an increased sodium loss in urine, further contributing to hyponatremia
- Slide 43
- DISORDERS OF THE POSTERIOR PITUITARY GLAND
- Slide 44
- HISTORY The nurse pays particular attention to a history of the following: Recent trauma Cerebrovascular disease Tuberculosis or other pulmonary disease Cancer All past and current medication use
- Slide 45
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Assessment Initially, the symptoms of SIADH are related to water retention. Gastrointestinal (GI) disturbances may occur first: loss of appetite nausea and vomiting The nurse weighs the client and documents any recent weight gain The client may experience lethargy, headaches, hostility, and disorientation. A change in level of consciousness is an early sign of SIADH. Neurologic symptoms can progress from lethargy and headaches to decreased responsiveness, seizures, and coma. The nurse assesses deep tendon reflexes, which are often decreased or sluggish. Vital sign changes include tachycardia (caused by the increased fluid volume) and hypothermia (caused by central nervous system disturbance)
- Slide 46
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Diagnostic assessment Water retention changes both plasma and urine osmolality. Urine volume decreases, and urine osmolarity increases. Plasma volume increases, and plasma osmolarity decreases. Elevated urine sodium levels and elevated specific gravity reflect increased urine concentration. Serum sodium levels are decreased, often as low as 110 mEq/L, because of volume expansion and sodium excretion. Radioimmunoassay of ADH can diagnose SIADH when ADH levels are inappropriately elevated in relation to plasma osmolality. (When plasma osmolality is normal or ecreased, ADH levels should be low)
- Slide 47
- DISORDERS OF THE POSTERIOR PITUITARY GLAND Interventions Interventions to treat SIADH focus on restricting fluid intake, promoting the excretion of water, replacing lost sodium, interfering with the action of ADH, and preventing injury if the client experiences increased cranial pressure or seizures. FLUID RESTRICTION (500 to 600 mL/24 hr) DRUG THERAPY. Diuretics, Hypertonic saline (3% sodium chloride [3% NaCl])
- Slide 48
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION Insufficiency of adrenocortical steroids causes problems through the loss of mineralocorticoid (aldosterone) and glucocorticoid (cortisol) action Impaired secretion of cortisol results in decreased gluconeogenesis, leading to hypoglycemia. The glomerular filtration rate and gastric acid production decrease, leading to a reduction in urea nitrogen excretion, causing anorexia and weight loss Reduced aldosterone secretion causes potassium, sodium, and water imbalances. Potassium excretion is decreased,causing hyperkalemia; sodium and water excretion is increased, causing hyponatremia and hypovolemia. Potassium retention also promotes reabsorption of hydrogen ions, which can ultimately lead to acidosis
- Slide 49
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION Acute adrenal insufficiency, or Addisonian crisis, is a ifethreatening event in which the physiologic need for glucocorticoid and mineralocorticoid hormones is greater than the available supply In most cases, acute adrenal insufficiency occurs in response to a stressful event (e.g., surgery, trauma, or severe infection), especially when the adrenal hormone output is already compromised
- Slide 50
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION
- Slide 51
- HISTORY The client is asked about any change in activity level, because lethargy, fatigue, and muscle weakness are often present Questions about salt intake are included because salt craving is often a symptom of adrenal hypofunction Gastrointestinal (GI) problems, such as anorexia, nausea, vomiting, diarrhea, and abdominal pain, often occur. The nurse asks about weight loss during the past weeks or months Female clients report menstrual changes related to weight loss, and male clients may report impotence The nurse asks whether the client has had radiation to the abdomen or head. Significant medical problems (e.g., tuberculosis or previous intracranial surgery) and all past and current medications, especially steroids, anticoagulants, or cytotoxic drugs, are documented
- Slide 52
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION HISTORY The client is asked about any change in activity level, because lethargy, fatigue, and muscle weakness are often present Questions about salt intake are included because salt craving is often a symptom of adrenal hypofunction Gastrointestinal (GI) problems, such as anorexia, nausea, vomiting, diarrhea, and abdominal pain, often occur. The nurse asks about weight loss during the past weeks or months Female clients report menstrual changes related to weight loss, and male clients may report impotence The nurse asks whether the client has had radiation to the abdomen or head. Significant medical problems (e.g., tuberculosis or previous intracranial surgery) and all past and current medications, especially steroids, anticoagulants, or cytotoxic drugs, are documented
- Slide 53
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION PHYSICAL ASSESSMENT/CLINICAL MANIFESTATIONS The clinical manifestations of adrenal hypofunction vary, and the severity of symptoms is related to the degree of hormone deficiency In clients with primary adrenal hypofunction, plasma ACTH and melanocyte-stimulating hormone (MSH) levels are elevated because of the loss of the adrenal-hypothalamic- pituitary feedback system. Elevated MSH levels result in areas of increased pigmentation In primary autoimmune disease, areas of decreased pigmentation may occur because of destruction of pigmentproducing cells in the skin (melanocytes). Body hair may also be decreased In secondary disease, there is no increase in skin pigmentation
- Slide 54
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION
- Slide 55
- Slide 56
- The nurse assesses the client for symptoms of hypoglycemia (e.g., sweating, headaches, tachycardia, and tremors) and volume depletion (postural hypotension and dehydration) Hyperkalemia (elevated blood levels of potassium) can cause dysrhythmias with an irregular heart rate and result in cardiac arrest
- Slide 57
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION PSYCHOSOCIAL ASSESSMENT Depending on the degree of metabolic imbalance, clients may appear lethargic, apathetic, depressed, confused, and even psychotic. The nurse observes the client and checks his or her orientation to person, place, and time. Families may report that the client has a decreased energy level, experiences wide mood swings, and is forgetful
- Slide 58
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION
- Slide 59
- Plasma cortisol levels fail to rise during stimulation tests Urinary 17-hydroxycorticosteroids are the glucocorticoid metabolites, and 17-ketosteroid levels reflect the adrenal androgen metabolites. Both levels are in the low or low-normal range in adrenal hypofunction Skull x-ray films, computed tomography (CT), magnetic resonance imaging (MRI), and arteriography may aid in the search for a cause of pituitary problems leading to adrenal insufficiency Noninvasive procedures of the adrenal gland, such as CT scans without dye, may occasionally show atrophy of the gland. CT scans may help determine adrenal hypofunction
- Slide 60
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION A rapid ACTH stimulation test may be administered on an outpatient basis. Cosyntropin 0.25 to 1 mg is given intramuscularly or intravenously, and plasma cortisol levels are obtained at 30-minute and 1-hour intervals after the baseline value is established. In primary insufficiency, the cortisol response is absent or markedly decreased; in secondary insufficiency, it is decreased A longer ACTH stimulation test uses a continuous infusion of 50 units of ACTH in saline for 24 hours or an 8-hour infusion daily for 4 to 5 days, with simultaneously collected 24-hour urine samples. Levels of urinary 17- hydroxycorticosteroids and urinary free cortisol are also measured. In clients with primary adrenal insufficiency, the response is low or absent; in those with secondary insufficiency, the value for 17-hydroxycorticosteroids fails to rise above 20 mg per total volume
- Slide 61
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION Interventions Nursing interventions are aimed at promoting fluid balance and monitoring for fluid deficit The nurse or assistive nursing personnel weighs the client daily and records intake and output. Vital signs are assessed every 1 to 4 hours, depending on the client's condition and the occurrence of dysrhythmias or postural hypotension. Laboratory values are monitored to identify hemoconcentrations
- Slide 62
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPOFUNCTION Glucocorticoid and mineralocorticoid deficiencies are completely corrected by replacement therapy. Hydrocortisone corrects glucocorticoid deficiency An additional mineralocorticoid hormone, such as fludrocortisone (Florinef), may be needed to maintain correct electrolyte balance (especially sodium and potassium). Adjustments in dosage may be necessary in hot weather, when additional sodium is lost because of excessive perspiration Salt restriction or diuretic therapy should not be started without considering whether it might precipitate an adrenal crisis
- Slide 63
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Hypersecretion by the adrenal cortex may result in excessive amounts of glucocorticoids, leading to hypercortisolism (e.g., Cushing's syndrome), hyperaldosteronism (excessive mineralocorticoid production), or excessive androgen production Hypersecretion of the adrenal medulla caused by a tumor (pheochromocytoma) results in excessive secretion of catecholamines, of which 80% is epinephrine and the remainder is norepinephrine
- Slide 64
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Hypercortisolism (Cushing's Syndrome) Excessive stimulation of adrenocorticotropic hormone (ACTH) of either pituitary or ectopic origin causes adrenocortical hyperplasia, which results in loss of normal hormone secretion rhythms The client's endocrine tissues have decreased responsiveness to releasing hormones, especially prolactin (PRL), thyrotropin, and gonadotropin. Many clients also experience abnormal sleep patterns
- Slide 65
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The client with Cushing's syndrome has alterations of nitrogen, carbohydrate, and mineral metabolism. An increase in total body fat results from slow turnover of plasma fatty acids, and a redistribution of fat produces the typical body pattern of trancal obesity, "buffalo hump," and "moon face Increases in the breakdown of tissue protein and an increase in urine nitrogen excretion also occur, resulting in decreased muscle mass, atrophic (thin) skin, and bone density loss High levels of corticosteroids kill lymphocytes and shrink organs containing lymphocytes, such as the liver, the spleen, and the lymph nodes. Thus protection of the inflammatory and immune responses is reduced
- Slide 66
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION In most cases, increased androgen production causes acne, hirsutism (increased hair growth), and occasionally, clitoral hypertrophy Increased androgen production can also interrupt the normal hormone feedback mechanism for the ovary, decreasing the ovary's production of estrogens and progesterone. Oligomenorrhea (scant or infrequent menses) occurs as a result
- Slide 67
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Etiology Cushing's syndrome is a group of clinical problems caused by an excess of cortisol, secreted by the adrenal cortex (endogenous) or administered for another clinical disorder (exogenous or iatrogenic). Women are affected eight times more often than men
- Slide 68
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION
- Slide 69
- HISTORY The nurse asks about changes in activity or sleep patterns, fatigue, and muscle weakness. Osteoporosis is common in hypercortisolism, and the client is asked about bone pain or a history of fractures. The nurse also questions the client about a history of frequent infections and easy bruising, which suggest hypercortisolism. Women may report a cessation of menses Gastrointestinal (GI) complaints may indicate ulcer formation from increased hydrochloric acid secretion The nurse also refers to the client's medical history. Steroid or alcohol abuse can produce the clinical and biochemical features of Cushing's syndrome
- Slide 70
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION PHYSICAL ASSESSMENT/CLINICAL MANIFESTATIONS The client with hypercortisolism has characteristic physical changes. The general appearance of the client is observed. Changes in fat distribution may result in fat pads on the neck, back, and shoulders ("buffalo hump"); an enlarged trunk with thin arms and legs; and a round face ("moon face"). Other characteristics include generalized muscle wasting and weakness The nurse also inspects the client for skin changes resulting from increased blood vessel fragility, such as bruises, thin or translucent skin, and wounds that have not healed properly Reddish purple striae ("stretch marks") are often present on the abdomen, upper thighs, and upper arms because of the degradative effect of cortisol on collagen
- Slide 71
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION
- Slide 72
- Excessive cortisol secretion may result in a fine coating of hair over the face and body and in acne. In the female client, the nurse looks for the presence of hirsutism, clitoral hypertrophy, and male pattern balding related to androgen excess Elevations in blood glucose levels are also a frequent finding Hypertension from water and sodium retention is common
- Slide 73
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION PSYCHOSOCIAL ASSESSMENT Hypercortisolism can result in emotional lability, and the nurse asks about mood swings, irritability, confusion, or depression The client may become neurotic or psychotic as a result of changes in blood cortisol levels
- Slide 74
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION DIAGNOSTIC ASSESSMENT Plasma cortisol levels are elevated in clients with hypercortisolism. Blood for cortisol assays is obtained at the same time of day because levels vary throughout the day. Plasma ACTH levels vary, depending on the cause of hypercortisolism In ectopic (ACTHproducing) syndromes, ACTH levels are elevated. In Cushing's syndrome (primary disease of the adrenal gland), ACTH levels are low to immeasurable
- Slide 75
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Additional laboratory findings may include the following: Increased blood glucose level Elevated white blood cell count Elevated lymphocyte count Increased sodium level Decreased serum calcium level Decreased serum potassium level
- Slide 76
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Urine is tested to measure levels of free cortisol and the adrenal metabolites of cortisol and androgens (17-hydroxycorticosteroids and 17- ketosteroids) The client is instructed to save all urine for 24 hours In Cushing's disease, basal levels of urinary free cortisol, 17-ketosteroids, and 17- hydroxycorticosteroids are all elevated, as are urine levels of calcium, potassium, and glucose
- Slide 77
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Radiographic studies, computed tomography (CT) scans, magnetic resonance imaging (MRI), and arteriography may identify lesions of the adrenal or pituitary glands, lung, GI tract, or pancreas in a client with clinical manifestations of cortisol hypersecretion
- Slide 78
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The overnight dexamethasone suppression test is an initial screening test for Cushing's syndrome. The client is instructed not to take medications, especially phenytoin (Dilantin) or phenobarbital, for at least 2 days before the test. Normally, plasma cortisol levels are lower than 5 (xg/dL). Higher levels indicate that further, definitive testing is necessary
- Slide 79
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION For the 3-day, low-dose dexamethasone suppression test, the client must take no medications for at least 2 days before the test (if possible) and have no stressful procedures (e.g., barium enema, myelogram, or an intense physical therapy session) performed during the test A baseline 24-hour urine sample is collected on day 1. Dexamethasone 0.5 mg is administered every 6 hours on days 2 and 3, during which time 24-hour urine collections are taken The 24-hour urine collections are tested for 17- ketosteroids, 17-hydroxycorticosteroids, creatinine, and urinary free cortisol Normally, urinary 17-hydroxycorticosteroid excretion and free cortisol levels are suppressed by dexamethasone, and Cushing's syndrome is ruled out. If these levels are not suppressed, a higher-dose dexamethasone test is performed
- Slide 80
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The high-dose (8-mg) dexamethasone suppression test distinguishes between bilateral adrenocortical hyperplasia (e.g., Cushing's syndrome) and an adrenocortical neoplasm as the cause of hypercortisolism This test can be performed as an overnight test or a 2-day test and is similar to the tests previously discussed but uses higher doses of dexamethasone In the overnight high-dose test, the client with Cushing's disease will have a reduced plasma cortisol level that is less than 50% of baseline. This test is more reliable than the 2-day high-dose test
- Slide 81
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Interventions Goals of treatment for hypercortisolism include reduction of plasma cortisol levels, removal of tumors, prevention of complications, and restoration of normal or acceptable body appearance Preoperative and postoperative nursing care is an integral part of the management of the client with endogenous hypercortisolism because surgical intervention is usually necessary for the relief of symptoms
- Slide 82
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION NONSURGICAL MANAGEMENT. The nurse weighs the client daily and monitors intake and output to assess hydration status. Restriction of fluid intake is sometimes necessary to maintain fluid balance DRUG THERAPY. Most clients with endogenous hypercortisolism undergo surgery. Drugs that interfere with adrenocorticotropic hormone (ACTH) production or adrenal hormone synthesis, however, may be used for palliation. Mitotane (Lysodren) is an adrenal cytotoxic agent used for inoperable adrenal tumors Aminoglutethimide (Elipten, Cytadren) is an adrenal enzyme inhibitor that decreases cortisol production
- Slide 83
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Trilostane (Modrastane), also an enzyme inhibitor, has not always been effective Cyproheptadine (Periactin) is less commonly used to treat clients with adrenal hyperfunction resulting from pituitary-related Cushing's disease because it interferes with ACTH production During all drug therapy, the nurse assesses the client for therapy effectiveness and side effects or symptoms of toxicity
- Slide 84
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION RADIATION THERAPY. Radiation, applied internally or externally, may be used to treat hypercortisolism caused by pituitary adenomas. However, radiation is not always effective and also may destroy normal tissue The nurse observes for any changes in the client's neurologic status, such as headache, elevated blood pressure or pulse, disorientation, or changes in pupil size or reaction The client may experience skin dryness, redness, flushing, or alopecia at the radiation site The nurse reviews these possible side effects with the client
- Slide 85
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION SURGICAL MANAGEMENT. The surgical treatment of adrenocortical hypersecretion depends on the cause of the disease When adrenal hyperfunction is due to increased pituitary secretion of ACTH, transsphenoidal removal of an adenoma may be attempted. In many instances, small adenomas cannot be localized and hypophysectomy is needed. Hypophysectomy is performed via the transsphenoidal or transfrontal craniotomy route If hypercortisolism is caused by adrenal adenomas or carcinomas, a partial or complete adrenalectomy (removal of the adrenal gland) may be needed
- Slide 86
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION PREOPERATIVE CARE. Electrolyte imbalances are corrected before surgery, and the nurse monitors potassium, sodium, and chloride values. Dysrhythmias from potassium imbalance may occur, and cardiac monitoring may be indicated. Hyperglycemia, if present, is controlled before surgery, and the nurse monitors blood glucose levels. The nurse and assistive nursing personnel attempt to prevent infection with handwashing and aseptic technique.
- Slide 87
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The risk for falls is decreased by raising the siderails of the bed and encouraging the client to ask for assistance when getting out of bed. Glucocorticoid preparations are administered preoperatively as ordered. The client continues to receive glucocorticoids throughout the operative procedure to prevent adrenal crisis. The removal of the tumor results in a sudden drop in cortisol levels. The nurse discusses postoperative care and long-term medication therapy during preoperative teaching
- Slide 88
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION OPERATIVE PROCEDURES. A unilateral adrenalectomy is performed when one gland is involved. A bilateral adrenalectomy is necessary when ectopic ACTH-producing tumors cannot be treated by other means or when both adrenal glands are diseased Surgery can be abdominal or through the lateral flank. Abdominal surgery causes a higher degree of illness and risk. In the flank approach (the preferred approach), the abdominal cavity is not entered, and the morbidity and mortality rates are reduced. A new approach, laparoscopic adrenalectomy, may reduce the incidence of some postoperative complications
- Slide 89
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION POSTOPERATIVE CARE. After an adrenalectomy, the client is usually sent to a critical care unit. In the immediate postoperative period, the nurse assesses the client every 15 minutes to identify symptoms of cardiovascular collapse or shock (e.g., hypotension, a rapid, weak pulse, and a decreasing urine output) due to possible insufficient glucocorticoid replacement. The nurse monitors ongoing vital signs and other hemodynamic variables (central venous pressure, pulmonary wedge pressure), intake and output, daily weights, and serum electrolyte levels. After a bilateral adrenalectomy, clients require lifelong glucocorticoid and mineralocorticoid replacement. The nurse administers glucocorticoid preparations as ordered. In unilateral adrenalectomy, glucocorticoid replacement continues until the remaining gland increases hormone production. This therapy may be required for up to 2 years after surgery
- Slide 90
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION PREVENTING COMPLICATIONS. The client who has hypercortisolism is prone to injury from skin breakdown, pathologic bone fractures, and gastrointestinal (GI) bleeding. Prevention of such injuries is a major nursing care focus
- Slide 91
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Gastrointestinal Bleeding. Interventions are aimed at minimizing gastric irritation, usually through drug therapy Drug therapy involves two different types of agents: those that protect the GI mucosa (antacids) and those that decrease the secretion of hydrochloric acid (H 2 -blockers, inhibitors of gastric proton pump)
- Slide 92
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Hyperaldosteronism In clients with hyperaldosteronism, increased secretion of aldosterone results in mineralocorticoid excess. Primary hyperaldosteronism (Conn's syndrome) is due to excessive secretion of aldosterone from one or both adrenal glands, which is most commonly caused by an adenoma. In a person with secondary hyperaldosteronism, the continuous excessive secretion of aldosterone is caused by high levels of angiotensin II that are due to high plasma renin activity. Causes of this renin activation include renal hypoxemia and the use of thiazide diuretics.
- Slide 93
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Increased aldosterone levels affect the renal tubules and cause sodium retention with potassium and hydrogen ion excretion. Hypernatremia, hypokalemia, and metabolic alkalosis result. Sodium retention increases blood and interstitial fluid volume, which elevates blood pressure and suppresses renin production. The elevated blood pressure may cause strokes and renal damage. Peripheral edema rarely occurs because of the "renal escape mechanism," in which the proximal tubule decreases sodium reabsorption. However, no compensatory mechanism exists to stop or reverse the loss of potassium
- Slide 94
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Assessment Symptoms related to hypokalemia and elevated blood pressure are the most common problems of the client with hyperaldosteronism. The history may reveal nonspecific findings, such as headache, fatigue, muscle weakness, nocturia (excessive urination at night), and loss of stamina. Polydipsia (excessive fluid intake) and polyuria (excessive urine output) occur less frequently. Paresthesias (sensations of numbness and tingling) may occur if potassium depletion is severe. The client may have visual changes related to hypertension
- Slide 95
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The diagnosis of primary hyperaldosteronism is made on the basis of laboratory studies and x-ray findings. Serum potassium levels are decreased, and sodium levels are elevated. Plasma renin levels are low; aldosterone levels are elevated. Increased hydrogen ion secretion results in metabolic alkalemia (elevated blood pH). Urine studies show low specific gravity and elevated aldosterone levels. Computed tomography (CT) scans reveal the presence and location of adrenal adenomas
- Slide 96
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Interventions Surgery is the treatment of choice for hyperaldosteronism if the problem is identified in its early stages. Adrenalectomy may be unilateral or bilateral. Surgery is not performed, however, until the client's potassium levels are normal. The physician orders spironolactone (Aldactone, Novospiroton, Sincomen), a potassium-sparing diuretic and aldosterone antagonist, to promote fluid balance. Potassium supplements may be ordered to increase potassium levels before surgery.
- Slide 97
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION The client may also benefit from a low-sodium preoperative diet, but no dietary restrictions are needed after surgery because aldosterone levels should return to normal. The client who has undergone a unilateral adrenalectomy may require temporary glucocorticoid replacement, and the client who has undergone a bilateral adrenalectomy needs lifelong replacement. Glucocorticoids are administered before surgery to prevent adrenal hypofunction. The client receiving long-term replacement therapy should wear a medical alert bracelet
- Slide 98
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION When surgery is inadvisable, spironolactone therapy is continued to control the symptoms of hypokalemia and hypertension. Because spironolactone is a potassium-sparing diuretic, hyperkalemia can occur in clients who have impaired renal function or excessive potassium intake. The nurse advises the client to avoid potassium supplements and foods rich in potassium.
- Slide 99
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Because hyponatremia can occur with spironolactone therapy, the client may require increased dietary sodium. He or she is instructed to report symptoms of hyponatremia, such as dryness of the mouth, thirst, lethargy, or drowsiness. The nurse alerts clients to report any additional side effects of spironolactone therapy, including gynecomastia, diarrhea, drowsiness, headache, rash, urticaria (hives), confusion, inability to maintain an erection, hirsutism, and amenorrhea
- Slide 100
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Pheochromocytoma Pheochromocytoma is a catecholamine- producing tumor that arises in chromaffin cells Pheochromocytomas release the catecholamines epinephrine and norepinephrine (NE). Excessive epinephrine and NE stimulate alpha receptors and beta receptors and can have wide-ranging adverse effects mimicking stimulation of the sympathetic division of the autonomic nervous system
- Slide 101
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Assessment The history may include intermittent hypertensive episodes or attacks that vary in length from a few minutes to several hours. During these episodes, the client experiences severe headaches, palpitations, profuse diaphoresis, flushing, apprehension, or a feeling of impending doom. Pain in the chest or abdomen, with nausea and vomiting, can also occur. Certain stimuli, such as increased abdominal pressure, urination, and vigorous abdominal palpation, can provoke a hypertensive crisis. The client may also report heat intolerance, weight loss, and tremors.
- Slide 102
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Diagnostic tests include 24-hour urine collections for vanillylmandelic acid (VMA) (a product of catecholamine metabolism), metanephrine, and free catecholamines, all of which are elevated in the presence of a pheochromocytoma. Basal plasma catecholamine levels are elevated after the client has been at rest for at least 30 minutes. The clonidine suppression test is used in the diagnosis of a pheochromocytoma. When oral clonidine hydrochloride (Catapres, Dixarit) is given to a person who does not have a pheochromocytoma, the clonidine suppresses catecholamine release and reduces the serum catecholamine levels. The response is not seen in the client who has a pheochromocytoma.
- Slide 103
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION When the client suspected of having a pheochromocytoma has severe hypertension, testing for the disorder may include alpha-adrenergic blockade with phentolamine. Phentolamine (Regitine, Rogitine) is administered intravenously at a dose of 5 mg, and blood pressure is measured every 30 seconds for 3 minutes, then every minute for 7 minutes. When a rapid drop of at least 35 mm Hg systolic pressure and 25 mm Hg diastolic pressure results, the test is considered positive
- Slide 104
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION After diagnosis, computed tomography (CT) scans of the adrenal glands locate intra-adrenal tumors. Chest x-ray films and tomograms can locate tumors in the thoracic area; arteriograms can locate intra- abdominal tumors
- Slide 105
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Interventions Surgery is the treatment of choice for a pheochromocytoma. One or both adrenal glands are removed (depending on whether the tumor is bilateral). Preoperatively, the nurse focuses on adequate tissue perfusion, nutritional needs, and comfort measures. The nurse monitors the blood pressure regularly and places the cuff consistently on the same arm, with the client in lying and standing positions. The nurse also identifies stressors that may precede a hypertensive crisis and attempts to minimize them. The client is instructed not to smoke, drink caffeine- containing beverages, or change position suddenly. The abdomen should not be palpated. A diet rich in calories, vitamins, and minerals is provided.
- Slide 106
- DISORDERS OF THE ADRENAL GLAND ADRENAL GLAND HYPERFUNCTION Postoperative nursing care is similar to that for the client who has undergone an adrenalectomy The nurse closely monitors the client for hypotension related to the sudden decrease in catecholamine level and for hypovolemia, especially when the client was inadequately prepared for surgery. Hemorrhage and shock are possible, and the nurse administers plasma expanders and fluids as prescribed. Vital signs, as well as fluid intake and output, are monitored. If opioids are administered, the nurse observes their effect on blood pressure
Related Documents