Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
- 1. PRESENTOR-DR.JOYDEEP CHAKRABORTY MODERATOR-DR.JL BAIDYA AGMC & GBP HOSPITAL,AGARTALA
- 2. Endometriosis is defined as the presence of endometrial tissue (glands and stroma) outside the uterus. This tissue is not only morphologically similar to normal endometrium ,but is also functional. It typically a disease of reproductive years. It is estimated to occur in 7%-10% of reproductive age women Introduction
- 3. Site of endometriosis PELVIC ENDOMETRIOSIS- Tubes & ovaries Uterus-adenomyosis Peritoneum Uterovesical fold Posterior cul de sac Pelvic side wall EXTRA PELVIC ENDOMETRIOSIS Gynecologic sites-vulva, vagina, cervix. Non gynecologic sites- Bowel lungs and pleural cavity skin (episiotomy or other surgical scars, lymph glands, nerves, and brain
- 4.
- 5. Although signs and symptoms of endometriosis have been described since the 1800s, its widespread occurrence was acknowledged only during this century. Endometriosis is an estrogen-dependent disease. Three theories have been proposed to explain the histogenesis of endometriosis: 1. Ectopic transplantation of endometrial tissue 2. Coelomic metaplasia 3. The induction theory No single theory can account for the location of endometriosis in all cases. Etiology
- 6. The transplantation theory, originally proposed by Sampson in the mid-1920s, is based on the assumption that endometriosis is caused by the seeding or implantation of endometrial cells by transtubal regurgitation during menstruation Transplantation Theory
- 7. The transformation (metaplasia) of coelomic epithelium into endometrial tissue has been proposed as a mechanism for the origin of endometriosis. This theory proposed by Meyer could explain endometriosis in nearly all ectopic sites. This theory has not been supported by either strong clinical or experimental data. Coelomic Metaplasia Theory
- 8. The induction theory is, in principle, an extension of the coelomic metaplasia theory. It proposes that an endogenous (undefined) biochemical factor can induce undifferentiated peritoneal cells to develop into endometrial tissue. This theory has been supported by experiments in rabbits but has not been substantiated in women and primates. Induction Theory
- 9. Halban suggest that endometriosis could result from lymphatic & haematogenous dissemination of endometrial cells. There is extensive communication of lymphatic between the uterus ,tubes,ovaries,pelvic & vaginal lymph nodes,kidneys & umbilicus. This explain disease effecting remote sites like- lungs,muscle,skin etc. Lymphatic & vascular metastases theory
- 10. The risk or endometriosis is 7 times greater if a first- degree relative has been affected by endometriosis . Multifactorial inheritance has been postulated. Monozygotic twins are markedly concordant for endometriosis. A worldwide collaborative project (The Oxford Endometriosis Gene Study) has been organized to identify a genetic basis for endometriosis Genetic Factors
- 11. Steroid Receptor Genetics An association of estrogen receptor gene polymorphisms (two-allele and multiallele polymorphism) with endometriosis has been reported .
- 12. Aneuploidy Epithelial cells of endometriotic cysts are monoclonal , but normal endometrial glands are polyclonal. Recent studies using comparative genomic hybridization or multicolor in situ hybridization showed aneuploidy for chromosomes 11, 16, and 17 , increased.
- 13. Loss of Heterozygosity Microsatellite DNA assays reveal an allelic imbalance (loss of heterozygosity) in p16 (Ink4), GALT, p53, and APOA2 loci in patients with endometriosis.
- 14. Although retrograde menstruation appears to be a common event in women, not all women who have retrograde menstruation develop endometriosis. It has been hypothesized that the disease may develop as a result of reduced immunologic clearance of viable endometrial cells from the pelvic cavity Immunologic Factors
- 15. Decreased clearance of peritoneal fluid endometrial cells due to- Reduced natural killer (NK) cell activity, or decreased macrophage activity. Decreased cell-mediated cytotoxicity toward autologous endometrial cells. There is no clinical evidence, however, that the prevalence of endometriosis is increased in immunosuppressed patients.
- 16. Substantial evidence suggests that endometriosis is associated with a state of subclinical peritoneal inflammation, marked by peritoneal fluid volume, peritoneal fluid white blood cell concentration inflammatory cytokines, growth factors, and angiogenesis-promoting substances Macrophages or other cells may promote the growth of endometrial cells by secretion of growth and angiogenic factors such as epidermal growth factor (EGF) Inflamation
- 17. There is increasing evidence that local inflammation and secretion of prostaglandins (PG) is related to differences in endometrial aromatase activity between women with and without endometriosis
- 18. Endometriosis should be suspected in women with subfertility, dysmenorrhea, dyspareunia, or chronic pelvic pain. However, endometriosis may be asymptomatic. Clinical Presentation
- 19. In adult women, dysmenorrhea may be especially suggestive of endometriosis if it begins after years of pain-free menses. Dysmenorrhea often starts before the onset of menstrual bleeding and continues throughout the menstrual period. In adolescents, the pain may be present after menarche without an interval of pain-free menses. The distribution of pain is variable but most often is bilateral. Pain
- 20. A common observation is that some women with extensive endometriosis have little or no pain, whereas others with only minimal endometriosis complain of severe pain. Very severe pain, however, is associated with deeply infiltrating endometriosis. Local symptoms can arise from rectal, ureteral, and bladder involvement. Lower back pain can occur. Dyspareunia may be associated with deep infiltrating subperitoneal endometriosis
- 21. An association between endometriosis and subfertility is generally accepted. Although numerous mechanisms have been proposed- ovulatory dysfunction, luteal insufficiency, luteinized unruptured follicle syndrome, recurrent abortion, altered immunity, and intraperitoneal inflammation. The association between fertility and minimal or mild endometriosis remains controversial. Subfertility
- 22. Endometriosis has been associated with- Anovulation, abnormal follicular development with impaired follicle growth, reduced circulating E 2 levels during the preovulatory phase, disturbed luteinizing hormone (LH) surge patterns, premenstrual spotting, the luteinized unruptured follicle syndrome, and galactorrhea and hyperprolactinemia. Endocrinologic Abnormalities
- 23. Extrapelvic endometriosis, although often asymptomatic, should be suspected when symptoms of pain or a palpable mass occur outside the pelvis in a cyclic pattern. Intestinal Tract (especially colon and rectum) is the most common site of extrapelvic disease and may cause abdominal and back pain. abdominal distention, cyclic rectal bleeding, constipation, and obstruction. Extrapelvic Endometriosis
- 24. Ureteral -involvement can lead to obstruction and result in cyclic pain, dysuria, and hematuria. Pulmonary endometriosis can manifest as pneumothorax, hemothorax, or hemoptysis during menses. Umbilical endometriosis should be suspected when a patient has a palpable mass and cyclic pain in the umbilical area Scar Endometriosis may present with cyclical pain &swelling.
- 25. Recommended that pelvic examination be performed at the time of menses when tenderness is easier to detect. The vulva, vagina, and cervix should be inspected for any signs of endometriosis, although the occurrence of endometriosis in these areas is rare (e.g., episiotomy scar). The uterus is often in fixed retroversion, and the mobility of the ovaries and fallopian tubes is reduced. CLINICAL EXAMINATIONS
- 26. Other possible signs of endometriosis include uterosacral or cul-de-sac nodularity, cervical displacement due to uterosacral scarring , painful swelling of the rectovaginal septum, and unilateral ovarian (cystic) enlargement.
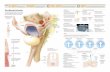
- 27. The classic chocolate cyst of the ovary is the result of a blood-filled cavity within an endometrioma. Ultrasonography and magnetic resonance imaging can be helpfulin diagnosing endometriomas. However, neither can diagnose small peritoneal implants or adhesions. Although transvaginal ultrasonography is highly accurate in diagnosing ovarian endometriomas, hemorrhagic cysts account for a significant false positive rate IMAGING STUDY
- 28. Ultrasound pictures of endometriotic cyst which shows fine stippling inside ovary (ground glass appearance)
- 29. Serum CA-125 levels are often elevated in patients with endometriosis and correlate with both the degree of disease and the response to treatment. Serum CA-125 determinations may be able to differentiate endometriotic from nonendometriotic benign adnexal cysts, especially when combined with transvaginal ultrasonography The CA-125 Assay
- 30. During diagnostic laparoscopy, the pelvic and abdominal cavity should be systematically investigated for the presence of endometriosis. This examination should include a complete inspection and palpation in a clockwise or counterclockwise fashion with a blunt probe of the bowel, bladder, uterus, tubes, ovaries, cul-de-sac, and broad ligament. Laparoscopic Findings- GOLD STANDARD
- 31. Characteristic findings include typical (powder-burn, gunshot) lesions on the serosal surfaces of the peritoneum. These are black, dark brown, or bluish nodules or small cysts containing old hemorrhage surrounded by a variable degree of fibrosis. Scarring of perotoneum causes adhesions Endometriosis can appear as subtle lesions ,including red implants (petechial, vesicular, polypoid, hemorrhagic, red flamelike), serous or clear vesicles, white plaques or scarring, yellow-brown discoloration of the peritoneum, and subovarian adhesions. Laparoscopic view of peritoneal lesion
- 32.
- 33.
- 34. 36 Upon closer view, these five small areas of endometriosis have a reddish-brown to bluish appearance.
- 35. EXTENSIVE PELVIC ENDOMETRIOSIS
- 36. DENSE ADHESIONS
- 37. The diagnosis of ovarian endometriosis is facilitated by careful inspection of all sides of both ovaries, which may be difficult when adhesions are present in more advanced stages of disease. With superficial ovarian endometriosis, lesions can be both typical and subtle. Larger ovarian endometriotic cysts (endometrioma) are usually located on the anterior surface of the ovary and are associated with retraction, pigmentation, and adhesions to the posterior peritoneum. These ovarian endometriotic cysts often contain a thick, viscous dark brown fluid (chocolate fluid) composed of hemosiderin derived from previous intraovarian hemorrhage. Ovarian endomeriosis
- 38.
- 39. 41 This is a section through an enlarnged 12 cm ovary to demonstrate a cystic cavity filled with old blood typical for endometriosis with formation of an endometriotic, or "chocolate", cyst.
- 40. Histologic confirmation is essential in the diagnosis of endometriosis. Microscopically, endometriotic implants consist of endometrial glands and stroma with or without hemosiderin-laden macrophages Histologic Confirmation
- 41.
- 42. Stage I (Minimal) 1-5 Stage II (Mild) 6-15 Stage III (Moderate) 16-40 Stage IV (Severe) >40 American society for reproductive medicine revised classification of endometriosis
- 43.
- 44.
- 45. In most cases, preservation of reproductive function is desirable. The least invasive and least expensive approach that is effective should be used. GOAL- is to excise or coagulate all visible endometriotic lesions and associated adhesions -and to restore normal anatomy. Laparoscopy can be used in most women, and this technique decreases cost, morbidity, and the possibility of recurrence of adhesions postoperatively. Laparotomy should be reserved for patients with advanced-stage disease who cannot undergo a laparoscopic procedure and for those in whom fertility conservation is not necessary. SURGICAL TREATMENT
- 46. Endometriosis lesions can be removed during laparoscopy by surgical excision with scissors, bipolar coagulation, or laser methods (CO 2 laser, potassium-titany-phosphate laser, or argon laser). Peritoneal Endometriosis
- 47.
- 48. LAPAROSCOPIC EXCISION
- 49. Superficial ovarian lesions can be vaporized. Small ovarian endometrioma (3 cm in diameter) ovarian endometrioma should be aspirated, followed by incision and removal of the cyst wall from the ovarian cortex. To prevent recurrence, the cyst wall of the endometrioma must be removed, and normal ovarian tissue must be preserved. OVARIAN ENDOMETRIOSIS
- 50. The removal of endometriosis-related adhesions (adhesiolysis) should be performed carefully . Routine use of pharmacologic or liquid agents to prevent postoperative adhesions after fertility surgery cannot be recommended based on evidence from randomized controlled trials. Adhesiolysis
- 51. Deep Rectovaginal and Rectosigmoidal Endometriosis The surgical excision of deep rectovaginal and rectosigmoidal endometriosis is difficult and can be associated with major complications. Postoperative bowel perforations with peritonitis have been reported in 2% to 3% of cases . LUNA(Laparoscopic uterosacral nerve ablation) Extrapelvic endometrios-surgical excision may be difficult. Scar endometriosis may need excision. OTHERS
- 52. In patients with severe endometriosis, it has been recommended that surgical treatment be preceded by a 3- month course of medical treatment to reduce vascularization and nodular size. However, a recent randomized study comparing 3 months of preoperative treatment with GnRH and no treatment in 75 women with moderate to severe endometriosis failed to show a significant difference in ease of surgery between the two groups . Preoperative Hormonal Treatment
- 53. Postoperative medical therapy may be required in patients with incomplete surgical resection and persistent pain. Treatment should last at least 3 to 6 months, and pain relief may be of short duration, presumably because endometriosis recurs Postoperative medical therapy
- 54. Although hormonal therapy of infertility associated with endometriosis is not of proven value, medical therapy for dysmenorrhea, dyspareunia, and pelvic pain associated with endometriosis is very successful (although relief may be short-term). Medical Treatment
- 55. Implants of endometriosis react to steroid hormones in a manner somewhat, but not exactly,similar to normally stimulated endometrium. Because estrogen is known to stimulate the growth of endometriosis, hormonal therapy has been designed to suppress estrogen synthesis, thereby inducing atrophy of ectopic endometrial implants or interrupting the cycle of stimulation and bleeding. Manipulation of the endogenous hormonal milieu is the basis for the medical management of endometriosis. Basis For The Medical Management
- 56. The treatment of endometriosis with continuous low-dose monophasic combination contraceptives ( for 6 to 12months) was originally used to induce pseudopregnancy caused by the resultant amenorrhea and decidualization of endometrial tissue. In addition, the subsequent amenorrhea induced by oral contraceptives could potentially reduce the amount of retrograde menstruation (one of the many risk factors proposed in the etiology of endometriosis). Oral Contraceptives
- 57. Pathologically, oral contraceptive use is associated with decidualization of endometrial tissue, necrobiosis, and possibly absorption of the endometrial tissue . Unfortunately, there is no convincing evidence that medical therapy with oral contraceptives offers definitive therapy. Instead, the endometrial implants survive the induced atrophy and, in most patients, reactivate after termination of treatment. Any low-dose combination oral contraceptive containing 30 to 35 mg of ethinyl estradiol used continuously can be effective in the management of endometriosis
- 58. Progestins may exert an anti endometriotic effect by causing initial decidualization of endometrial tissue followed by atrophy. They can be considered as the first choice for the treatment of endometriosis because they are as effective as danazol or GnRH analogues and have a lower cost and a lower incidence of side effects than these agents. Progestins
- 59. Medroxyprogesterone acetate (150 mg) given intramuscularly every 3 months is effective for the treatment of pain associated with endometriosis. Megestrol acetate has been administered in a dose of 40 mg/d with good results . Other treatment strategies have included dydrogesterone (20 to 30 mg/d, either continuously or on days 5 to 25) and lynestrenol (10 mg/d).
- 60. Local progesterone treatment with a levonorgestrel- releasing intrauterine system for 12 months has resulted in a significant reduction in dysmenorrhea, pelvic pain, and dyspareunia.
- 61. Progesterone antagonists and progesterone receptor modulators may suppress endometriosis based on their antiproliferative effects on the endometrium, without the risk for hypo-estrogenism or bone loss that occurs with GnRH treatment Progesterone Antagonists
- 62. Mifepristone Mifepristone (RU-486) is a potent antiprogestagen with a direct inhibitory effect on human endometrial cells and, in high doses, an antiglucocorticoid action . The recommended dose for endometriosis is 25 to 100 mg/d. mifepristone, 50 to 100 mg/d, reduced pelvic pain and induced 55% regression of the lesions without significant side effects .
- 63. Gestrinone Gestrinone is a 19-nortestosterone derivative with androgenic, antiprogestagenic, antiestrogenic, and antigonadotropic properties. It acts centrally and peripherally to free testosterone and sex hormonebinding globulin levels (androgenic effect), serum estradiol values to early follicular phase levels(antiestrogenic effect), mean LH levels, and obliterate the LH and follicle-stimulating hormone (FSH) surge (antigonadotropic effect). Gestrinone causes cellular inactivation and degeneration of endometriotic implants but not their disappearance . The standard dose has been 2.5 mg twice a week 6-9 months.
- 64. Pharmacologic properties of danazol include suppression of GnRHor gonadotropin secretion, direct inhibition of steroidogenesis, increased metabolic clearance of estradiol and progesterone . The multiple effects of danazol produce a high- androgen, low-estrogen environment that does not support the growth of endometriosis, and the amenorrhea that is produced prevents new seeding of implants from the uterus into the peritoneal cavity Danazol
- 65. start treatment with 400 mg daily (200 mg twice a day) and increase the dose, if necessary, to achieve amenorrhea and relieve symptoms . local danazol treatment using a vaginal danazol ring (1,500 mg) has been shown to be effective for pain relief in deeply infiltrative endometriosis without the classic danazol sideeffects, or detectable serum danazol levels, while allowing ovulation and conception
- 66. GnRH agonists bind to pituitary GnRH receptors and stimulate LH and FSH synthesis and release. However, the agonists have a much longer biologic half-life (3 to 8 hours) than endogenous GnRH (3.5 minutes), resulting in the continuous exposure of GnRH receptors to GnRH agonist activity. This causes a loss of pituitary receptors and downregulation of GnRH activity, resulting in low FSH and LH levels. Consequently, ovarian steroid production is suppressed, providing a medically induced and reversible state of pseudomenopause. A direct effect of GnRH agonists on ectopic endometrium is also possible because expression of the GnRH receptor gene has been documented in ectopic endometrium and because direct inhibition of endometriosis cells has been demonstrated in vitro. Gonadotropin-releasing Hormone Agonists
- 67. These agents include leuprolide(leuporide 3.75 mg im monthly), buserelin, nafarelin, histrelin, goserelin, deslorelin, and triptorelin. These drugs are inactive orally and must be administered intramuscularly, subcutaneously, or by intranasal absorption. The best therapeutic effect is often associated with an estradiol dose of 20 to 40 pg/mL (75 to 150 pmol/L). These so-called depot formulations are attractive because of the reduced frequency of administration and because nasal administration can be complicated by variations in absorption rates and problems with patient compliance
- 68. Aromatase Inhibitors-anastrozole, 1 mg/d, Selective Estrogen Receptor Modulators-Raloxifen OTHER
- 69. Modulation of Cytokines- 1recombinant human TNF-abinding protein effectively inhibits the development of endometriosis and endometriosis-related adhesions 2.immune-enhancing modulators loxoribine and levamisole Nonhormonal Medical Therapy
- 70. Antiinflammation- leukotriene receptor antagonists oral pentoxifylline,
- 71. Based on published studies, medroxyprogesterone acetate, danazol, gestrinone,and GnRH agonists have similar efficacy in resolution of the laparoscopically documented disease and in pain alleviation . Disadvantages of medical therapy over surgical therapy include the high cost of hormone preparations, the high prevalence of side effects, and the higher recurrence rate of endometriosis Efficacy of Medical Treatment
- 72. Conception is either impossible or contraindicated during medical treatment of endometriosis. There is no evidence that medical treatment of minimal to mild endometriosis leads to better chances of pregnancy than expectant management
- 73. Recurrence Endometriosis tends to recur unless definitive surgery is performed. The recurrence rate is about 5% to 20% per year, reaching a cumulative rate of 40% after 5 years. The rate of recurrence increases with the stage of disease, the duration of follow-up, and the occurrence of previous surgery . The likelihood of recurrence appears to be lower when endometriosis is located only on the right side of the pelvis than when the left side is involved
- 74. The treatment of endometriosis-related infertility is dependent on the age of the woman, the duration of infertility, the stage of endometriosis, the involvement of ovaries, tubes, or both in the endometriosis process, previous therapy, associated pain symptoms, and the priorities of the patient, taking into account her attitude toward the disease, the cost of treatment, her financial means, and the expected results. Assisted reproduction, including controlled ovarian hyperstimulation with intrauterine insemination, IVF, and GIFT, may be options for infertility treatment in addition to surgical reconstruction and expectantmanagement. IVF is the method of choice when distortion of the tuboovarian anatomy contraindicates the use of superovulation with intrauterine insemination or GIFT. Assisted Reproduction and Endometriosis
- 75. Conclusion Endometriosis is a chronic, costly disease requiring long-term, multidisciplinary treatment Profound personal and economic impact underscores urgent need for continued research and improvement in diagnostic and treatment modalities Timely intervention and appropriate, multifactorial treatments may restore quality of life, preserve or improve fertility, and lead to long-term effective management in absence of permanent cure
Related Documents