Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. Chapter 78 Drugs for Peptic Ulcer Disease

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. Chapter 78 Drugs for Peptic Ulcer Disease.
Dec 16, 2015
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc.
Chapter 78
Drugs for Peptic Ulcer Disease

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 2
Peptic Ulcer Disease
Definition Group of upper GI disorders Degrees of erosion of the gut wall Severe erosion can be complicated by
hemorrhage and perforation Cause
Imbalance between mucosal and aggressive factors

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 3
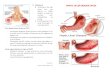
Fig. 78–1. The relationship of mucosal defenses and aggressive factors to health and peptic ulcer disease. When aggressive factors outweigh mucosal defenses, gastritis and peptic ulcers result.

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 4
Pathogenesis of Peptic Ulcers
Defensive factors Mucus
• Secreted cells of the GI mucosa• Forms a barrier to protect underlying cells from acid and pepsin
Bicarbonate• Secreted by epithelial cells of stomach and duodenum• Most remains trapped in the mucus layer to neutralize hydrogen
ions that penetrate the mucus Blood flow
• Poor blood flow can lead to ischemia, cell injury, and vulnerability to attack
Prostaglandins• Stimulate the secretion of mucus and bicarbonate

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 5
Pathogenesis of Peptic Ulcers
Aggressive factors Helicobacter pylori, also known as H. pylori
• Gram-negative bacillus that can colonize in the stomach and duodenum
• Lives between epithelial cells and the mucus barrier Escapes destruction by acid
• Can remain in GI tract for decades• Half of the world infected, but most people do not
develop symptomatic peptic ulcer disease (PUD)

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 6
Pathogenesis of Peptic Ulcers
Aggressive factors Helicobacter pylori, also known as H. pylori
(cont’d)• 60%–70% of patients with PUD have H. pylori infection• H. pylori may also promote gastric cancer• Duodenal ulcers are much more common among people
with H. pylori infection than among people who are not infected
• Eradication of the bacterium promotes healing of the PUD and minimized recurrence of PUD

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 7
Pathogenesis of Peptic Ulcers
Aggressive factors Nonsteroidal anti-inflammatory drugs (NSAIDs)
• Inhibit the biosynthesis of prostaglandins• Decrease blood flow, mucus, and bicarbonate
Gastric acid• Causes ulcers by directly injuring cells of the GI mucosa
and indirectly by activating pepsin• Increased acid alone does not increase ulcers but is a
definite factor in PUD Pepsin
• Proteolytic enzyme in gastric juice Smoking
• Delays ulcer healing and increases risk for recurrence

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 8
Pathogenesis of Peptic Ulcers
Summary of ulcer development Most common cause
• Infection with H. pylori (HP) is the most common cause of gastric and duodenal ulcers
• Additional factors must be involved: 50% harbor HP, but only 10% develop PUD
Second most common cause• NSAIDs

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 9
Overview of Treatment
Goals of drug therapy Alleviate symptoms Promote healing Prevent complications Prevent recurrence
Drugs do not alter the disease process; they create conditions conducive to healing

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 10
Classes of Antiulcer Drugs
Antibiotics Antisecretory agents Mucosal protectants Antisecretory agents that enhance mucosal
defenses Antacids

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 11
Three Ways Antiulcer Drugs Work
Eradicate H. pylori
(antibiotics)
Reduce gastric acidity
(antisecretory agents, misoprostol)
Enhance mucosal defenses
(sucralfate, misoprostol)

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 12
Drug Selection: H. pylori–Associated Ulcers
Antibiotics Should be given to all patients with
gastric/duodenal ulcers and documented H. pylori Antisecretory agents

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 13
Drug Selection: NSAID-Induced Ulcers
Prophylaxis Risk factors for ulcer development (older than 60
years, history of ulcers, high-dose NSAID therapy) Treatment
Proton pump inhibitors (PPIs) (eg, omeprazole) are preferred
Misoprostol is also effective, but can cause diarrhea
Antacids, sucralfate, and histamine2 receptor blockers are not recommended
Discontinue NSAIDs, if possible

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 14
Nondrug Therapy
Diet Traditional “ulcer diet” does not accelerate healing No convincing evidence indicates that caffeinated
beverages promote ulcers or delay healing Change eating pattern to 5–6 small meals a day
(reduces pH fluctuations) Avoid smoking, aspirin, other NSAIDs, and
alcohol if a trigger

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 15
Evaluation of Therapy
Monitor for relief of pain Keep in mind: cessation of pain and
disappearance of ulcer rarely coincide Pain may subside before complete healing or may
continue after healing Radiologic or endoscopic examination of
ulcer site H. pylori tests

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 16
H. pylori Tests
Noninvasive Breath test Serum test Stool test
Invasive Endoscopic specimen obtained and evaluated

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 17
H. pylori Treatment
Minimum of two antibiotics (up to three) prescribed to decrease risk of developing resistance Amoxicillin Clarithromycin Bismuth compounds Tetracycline Metronidazole Tinidazole

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 18
Antibiotic Regimen
2007 ACG updated guidelines for managing H. pylori Use minimum of two antibiotics, preferably three Antisecretory agent (PPI, H2 antagonist)
Barriers to compliance Can require up to 12 pills/day (14 days) GI side effects Expensive (about $200)

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 19
Histamine2-Receptor Antagonists
Cimetidine (Tagamet) Ranitidine (Zantac) Famotidine (Pepcid) Nizatidine (Axid)

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 20
Histamine2-Receptor Antagonists
First-choice drugs for treating gastric and duodenal ulcers
Promote healing by suppressing secretion of gastric acid
All four equally effective Serious side effects uncommon

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 21
Fig. 78–2. A model of the regulation of gastric acid secretion showing the actions of antisecretory drugs and antacids.

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 22
Cimetidine (Tagamet)
Pharmacokinetics Absorption slowed if taken with meals Crosses the blood-brain barrier with difficulty May cause some CNS side effects

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 23
Cimetidine (Tagamet)
Therapeutic uses Gastric and duodenal ulcers Gastroesophageal reflux disease (GERD) Zollinger-Ellison syndrome Aspiration pneumonitis Heartburn, acid indigestion, and sour stomach

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 24
Cimetidine (Tagamet)
Adverse effects Antiandrogenic effects CNS effects Pneumonia IV bolus: can experience hypotension and
dysrhythmias

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 25
Ranitidine (Zantac)
Shares many properties of cimetidine More potent, fewer adverse effects, causes fewer
drug interactions than cimetidine (and has less ability to cross CNS)
Adverse effects Significant ones uncommon Does not bind to androgen receptors

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 26
Ranitidine (Zantac)
Therapeutic uses Short-term treatment of gastric/duodenal ulcers Prophylaxis of recurrent duodenal ulcers Treatment of Zollinger-Ellison syndrome and
hypersecretory states Treatment of GERD

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 27
Famotidine (Pepcid)
Actions similar to those of ranitidine Therapeutic uses
Short-term treatment of gastric/duodenal ulcers Prophylaxis of recurrent duodenal ulcers Treatment of Zollinger-Ellison syndrome and
hypersecretory states Treatment of GERD Over-the-counter (OTC): to treat heartburn, acid
indigestion, sour stomach

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 28
Famotidine (Pepcid)
Adverse effects Does not bind to androgen receptors Possible increased risk for pneumonia caused by
elevation of pH

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 29
Nizatidine (Axid)
Actions much like those of ranitidine and famotidine
Therapeutic uses Duodenal/gastric ulcers GERD, heartburn, acid indigestion, and sour
stomach

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 30
Proton Pump Inhibitors Most effective drugs for suppressing secretion of
gastric acid Therapeutic uses: short term
Gastric/duodenal ulcers GERD
Well tolerated Selection of PPI based on cost and prescriber
preference Can increase the risk of serious adverse events,
including fracture, pneumonia, acid rebound, and possibly intestinal infection with Clostridium difficile

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 31
Omeprazole (Prilosec) First available proton pump inhibitor Actions and characteristics
Inhibits gastric secretion Short half-life Used for short-term therapy
Adverse effects Usually inconsequential with short-term use Headache Gastrointestinal effects Pneumonia Rebound acid hypersecretion C. difficile infection Gastric cancer

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 32
Other PPIs
Dexlansoprazole Rabeprazole Pantoprazole

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 33
Other Antiulcer Drugs
Sucralfate (Carafate) Misoprostol (Cytotec) Antacids

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 34
Sucralfate (Carafate)
Creates a protective barrier up to 6 hours Therapeutic uses
Acute ulcers and maintenance therapy Adverse effects
Constipation (in only 2% of patients) Drug interactions
Minimal Antacids may interfere with effects of sucralfate

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 35
Misoprostol (Cytotec)
Therapeutic uses Only approved GI indication is prevention of
gastric ulcers caused by long-term NSAID therapy Adverse effects
Most common: dose-related diarrhea (13%–40%) and abdominal pain (7%–20%)
Contraindicated during pregnancy: category X• Significant actions need to be taken to ensure that
pregnancy does not occur after therapy starts, and that patient is not pregnant at therapy initiation

Copyright © 2013, 2010 by Saunders, an imprint of Elsevier Inc. 36
Antacids
React with gastric acid to produce neutral salts or salts of low acidity Decrease destruction of the gut wall by
neutralizing acid May also enhance mucosal protection by
stimulating production of prostaglandins Except for sodium bicarbonate, antacids do
not alter systemic pH Use with caution in patients with renal
impairment
Related Documents