An Investigation into White Matter Small Vessel Disease Using Susceptibility-Weighted and Perfusion Magnetic Resonance Imaging by Farhang Jalilian A thesis submitted in conformity with the requirements for the degree of Master’s of Science Department of Medical Biophysics University of Toronto © Copyright by Farhang Jalilian 2014

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

An Investigation into White Matter Small Vessel Disease Using Susceptibility-Weighted and Perfusion Magnetic
Resonance Imaging
by
Farhang Jalilian
A thesis submitted in conformity with the requirements for the degree of Master’s of Science
Department of Medical Biophysics University of Toronto
© Copyright by Farhang Jalilian 2014

ii
An Investigation into White Matter Small Vessel Disease Using
Susceptibility-Weighted and Perfusion Magnetic Resonance
Imaging
Farhang Jalilian
Master’s of Science
Department of Medical Biophysics University of Toronto
2014
Abstract
Cerebral Small Vessel Disease (CSVD) is the most prevalent neurological condition among
elderly adults and is associated with increased risk of stroke and dementia. CSVD manifests as
regions of white matter hyperintensity on T2-weighted MRI. This thesis examines the role that
susceptibility-weighted imaging (SWI) can play in understanding CSVD by developing an
automated and quantitative procedure that isolates the venous anatomy. The prominence of veins
as seen on SWI throughout white matter and also in areas not affected by the disease were found
to be positively correlated with CSVD lesion burden. Furthermore, a shared anatomical
correspondence between the lesions and the venous vasculature was found. The increased
prominence of veins could reflect the pathophysiological changes associated with CSVD such as
ischemia, hemodynamic impairment and venous collagenosis. The use of novel neuroimaging
techniques to characterize CSVD can improve our current understanding and may be useful in
monitoring and treating the disease.

iii
Acknowledgments
When I first started my graduate work little I knew that my experience at Sunnybrook Research
Institute and the Medical Biophysics department would help me to rediscover my passion.
Throughout this journey, I was fortunate to have the help and support of many indivuals for
whom I have great respect.
Firstly, I should thank my Supervisor Dr. Bradley J MacIntosh for his inspiration and perspective
towards life.
Secondly, I would like to thank the members of my advisory committee, Drs. Philip Beatty,
Anne Martel and John Sled for their expert knowledge, support, and their extraordinary
understanding.
Thirdly, I would like to acknowledge the previous and current lab members and staff at Canadian
Partnership for Stroke Recovery, Sunnybrook Health Sciences Centre and Medical Biophysics
Department: David Crane, Ilia Makedonov, Ekaterina Tchistiakova, Christopher Scott, A. Saeed
Rajab, Dr. Andrew Robertson, Zahra Shirzadi, Dr. Arron Metcalfe, Dr. Walter Swardfager, Dr.
Fu-Qiang Gao, Courtney Berezuk, Alicia McNeely, Farrell Leibovitch, Ana Mersov, Merle
Casci, Dr. Mariam Afshin, Anoop Ganda, Tina Binesh and Hirad Karimi. Specifically, I would
like to thank David Crane for his great spirit and helps in every step of my project.
I should also acknowledge the help and support of my mentors and my friends. Those who have
helped me with either coming and staying in my life, or leaving and teaching me a lesson
indirectly. Those with whom I have spent time, those who are and will be in my memories: Dr. P.
Barmby, Dr. M. Drangova, Dr. R. Holt, Dr. S. Basu, Mr. A. Dianat-Far, Ebad, Sina, Maryam,
Araz, Nima, Amir, Mina, Alireza, Navid, Arash, Omid, Pedram, Bahar, Sara, Pooyan,
Mehrnoush, Shannon, Hirad and Niloufar.
Lastly, I would like to thank my parents, grandparents, my sister and my family for their
sacrifices and support.

iv
Table of Contents
Acknowledgments.......................................................................................................................... iii
Table of Contents........................................................................................................................... iv
List of Tables ................................................................................................................................. vi
List of Figures ............................................................................................................................... vii
List of Abbreviations .......................................................................................................................x
1 Background .................................................................................................................................1
1.1 Cerebral Small Vessel Disease (CSVD) ..............................................................................1
1.1.1 White Matter Hyperintensities.................................................................................1
1.1.2 Etiology and Consequences of WMHs....................................................................2
1.1.3 Geometrical Location of White Matter Hyperintensities.........................................5
1.2 Overview of Magnetic Resonance Imaging: Principles and Relevant Techniques .............5
1.2.1 Basic Principles of MRI...........................................................................................6
1.2.2 Contrast in MRI .......................................................................................................8
1.2.3 Susceptibility-weighted Imaging (SWI) ................................................................10
1.2.4 Clinical Applications of SWI.................................................................................14
1.3 Cerebral Venous Vasculature ............................................................................................17
1.3.1 Normal Anatomy ...................................................................................................17
1.3.2 Interpretation of Venous Signal on SWI................................................................18
1.4 Arterial Spin Labelling (ASL) ...........................................................................................19
1.5 Image Analysis: A Synopsis of Registration and Segmentation Techniques ....................20
1.5.1 Image Registration .................................................................................................21
1.5.2 Image Segmentation...............................................................................................21
2 Methods.....................................................................................................................................23
2.1 Participants.........................................................................................................................23

v
2.2 MRI Image Acquisition .....................................................................................................24
2.3 Image Processing ...............................................................................................................25
2.3.1 Brain Segmentation................................................................................................25
2.3.2 Venous Segmentation ............................................................................................27
2.3.3 Visual Rating of White Matter Hyperintensities ...................................................29
2.3.4 CBF Measurement: ROI and Voxel-wise Approaches..........................................30
2.4 Statistics .............................................................................................................................31
3 Results .......................................................................................................................................32
3.1 ROI Comparison ................................................................................................................32
3.2 Vein Fraction in WM.........................................................................................................33
3.3 Vein Fraction Results Based on the Visual Rating Scale ..................................................34
3.4 CBF Measurements............................................................................................................36
4 Discussion and Future Work.....................................................................................................38
4.1 Shared Anatomical Location..............................................................................................38
4.2 Prominence of Veins Reflects Pathophysiological Changes in CSVD .............................39
4.3 Perfusion Findings: Evidence and Implications ................................................................41
4.4 From Structural to Physiological Imaging: A Search for New Imaging Markers of CSVD.................................................................................................................................42
4.5 Limitations and Future Work.............................................................................................43
5 Conclusion ................................................................................................................................45

vi
List of Tables
Table 1: Demographic data on participants .................................................................................. 24
Table 2: The distribution of age, gender and WMHs across ARWMC groups. ........................... 35

vii
List of Figures
Figure 1: WMHs in two 80 year old patients. WMHs are best visualized on T2 weighted fluid
attenuated inversion recovery (FLAIR) images. Left: minor amounts of WMHs voxels. Right:
more pronounced WMHs in both periventricular and deep WM regions (Adopted from Debette
et al. 2010). ..................................................................................................................................... 2
Figure 2: A) The radiofrequency field B1 applied in the transverse direction and tuned to the
Larmor frequency so as to rotate the magnetization. B) Behaviour as seen from a rotating frame
of reference. (Adopted from Nishimura 1996) ............................................................................... 7
Figure 3: Precession of the magnetization vector in the xy-plane and generating an emf, which is
detected by the receiver coils. (Adopted from Nishimura 1996).................................................... 7
Figure 4: A general example of an ES pulse sequence where gradients lobes with areas of –A and
+2A are added prior and after each readout to shift the echo by one TR interval. ....................... 14
Figure 5: A typical SWI from a healthy participant. The hypointense lines are the cerebral veins.
....................................................................................................................................................... 15
Figure 6: 59 year old patient with sudden onset of right hemiparesis and speech deficit. A. MRA
shows lack of time of flight signal in the distal M1 segment of the left MCA. B and C. SWI
shows prominent subcortical veins within the left MCA territory suggestive of increased
deoxyhemoglobin in the draining veins. D) The regional CBF is reduced on the affected
hemisphere (Adopted from Mittal et al. 2009). ............................................................................ 16
Figure 7: Anatomy of the cerebral vasculature A) A coronal venogram shows a network of deep
medullary veins (DMV) draining the WM into subependymal veins near the lateral ventricle. B)
A coronal brain slice showing the normal arterial branching. [Adopted from Okudera et al. 1999]
....................................................................................................................................................... 17
Figure 8: Anatomy of deep medullary veins. A venogram map obtained from manually
segmenting a SWI images, performed by an expert neuroanatomist, demonstrates the rich venous
network around the ventricles. Colours from red to purple correspond to the level of the vessel

viii
along the z-axis from bottom to top. [Courtesy of Fuqiang Gao, Sunnybrook Research Institute].
....................................................................................................................................................... 18
Figure 9: Steps in ASL image acquisition. Left: Spins in the arterial blood (carotid artery) is
tagged before reaching the imaging plane. Right: A control image is obtained without inverting
the magnetization of the arterial blood. ........................................................................................ 20
Figure 10: An example of WMHs and tissue segmentations. A. A FLAIR image B. A T1-
weighted image C. Tissue segmentation delineating GM (green), NAWM (blue) and WMHs
(light blue)..................................................................................................................................... 26
Figure 11: A. Study-specific T1-weighted group template. B. WMHs probability map in the
group template constructed from averaging template acquired subjects’ WMHs masks. C. Group
template acquired NAWM mask is the “relative complement” of the binarized WMHs mask with
respect to the WM (i.e. voxels that are in the WM but do not belong to WMHs mask). ............. 27
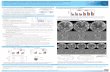
Figure 12: ARWMC rating scale. A. ARWMC Score 1; Focal lesions around the horn of lateral
ventricles (arrows). B. ARWMC Score 2; Periventricular lesions are becoming confluent
(arrow), and multiple deep WMHs are present (arrowhead). C. ARWMC Score 3; diffuse
involvement; periventricular WMHs are extending into the deep WM and vice versa................ 29
Figure 13: A. The mean CBF perfusion image B. The binary mask used in the voxel-wise
analysis showing voxels with SNR>1. ......................................................................................... 30
Figure 14: Top: the tissue class ROIs (B) was used to mask the venogram (A). Bottom: Vein
fraction in different tissue ROIs.................................................................................................... 32
Figure 15: Vein fraction vs. WMHs at the level of LV (top) and vs. global WMHs (bottom). C &
D are provided as context in support of the use of WMHs at of the LV. ..................................... 34
Figure 16: Comparison of WMHs, GM CBF, WM vein fraction and vein fraction in NAWM
mask among ARWMC scores....................................................................................................... 36
Figure 17: Voxel-wise analysis results shows a region (11 voxels; shown in blue) with reduced
perfusion. The background grey-scale image is the MNI152 T1 template................................... 37

ix
Figure 18: Association between WMHs and veins. The middle diagram shows the overlay of the
WMHs and the vein schematically. thin arrows=vein; think arrows=WMHs (Adopted from Gao
et al. 2008). ................................................................................................................................... 39

x
List of Abbreviations
3D three dimentional 2D two dimensional AD Alzheimer’s disease ANCOVA analysis of covariance ANOVA analysis of variance ARWMC age-related white matter changes ASL arterial spin labelling BET Brain Extraction Tool BOLD blood oxygen level-dependent
CADASIL cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy
CBF cerebral blood flow CCM cerebral cavernous malformations CMRO2 cerebral metabolic rate of oxygen CSF cerebrospinal fluid CSVD cerebral small vessel disease CT computed tomography CVST cerebral venous sinus thrombosis DOF degrees of freedom DTI diffusion tensor imaging DVA developmental venous angiomas ES echo shifted FLAIR fluid attenuated inversion recovery FLEX fuzzy lesion extractor
FMRIB Oxford Centre for Functional Magnetic Resonance Imaging of the Brain
FSL FMRIB Software Library GLM general linear model GM gray matter HRBV high-resolution BOLD venographic LV lateral ventricle MCA middle cerebral artery MMD moyamoya disease MNI Montreal Neurological Institute MOCA Montreal cognitive assessment tool MRI magnetic resonance imaging MS multiple sclerosis NAWM normal appearing white matter OEF oxygen extraction fraction PD proton density

xi
PET positron emission tomography PLD post label delay ppm part per million QSM quantitative susceptibility mapping RF radiofrequency ROI region of interest SNR signal-to-noise ratio SPECT single-photon emission computed tomography SVD small vessel disease SWI susceptibility-weighted imaging TBI traumatic brain injury TE echo time TIA transient ischemic attack TR repetition time TRUST T2-Relaxation-Under-Spin-Tagging WM white matter WMH white matter hyperintensity

1
“He who cannot draw on three thousand years is living from hand to mouth.”
Johann Wolfgang von Goethe
1 Background
1.1 Cerebral Small Vessel Disease (CSVD)
Small Vessel Disease (SVD) is a multi-organ vascular disease phenomenon that is associated
with human aging and affects the brain, eyes, and kidneys, for example. Cerebral Small Vessel
Disease (CSVD) is associated with structural and functional changes in the brain, principally in
the connective white matter (WM), in the form of ischemic lesions. White matter
hyperintensities (WMHs) are one of the most common manifestations of CSVD. The WMH
appearance on diagnostic imaging is in contrast to subcortical infarcts, lacunes, perivascular
spaces or cerebral micro bleeds 1. Sometimes referred to as “covert strokes”, WMHs are named
“hyperintensity” because of their bright signal intensity appearance as seen on some radiological
images. CSVD is considered to be the most common neurological disorder. Its high prevalence is
predominantly due to the fact that age is the most important risk factor for developing the
disease. The prevalence of CSVD increases dramatically with age; from approximately 6% to
7% at age 60 to 28% at age 80 2. WMHs are often incidental findings and in up to 89% of
individuals no history of stroke or transient ischemic attack exists 2.
1.1.1 White Matter Hyperintensities
The term WMHs to denote white matter CSVD pathology stems from the fact that WMHs are
readily apparent on T2-weighted magnetic resonance (MR) images, like the FLuid Attenuated
Inversion Recovery (FLAIR) sequence. WMHs can also be detected with reduced sensitivity on
CT, as areas of low attenuation and on proton density (PD) and T1-weighted MRI where they
appear hyper-intense and hypo-intense respectively. The prevalence of WMHs ranges from 11-
12% in adults at the age of 64, and increases with age to about 94% at the age of 84 3. Clinically
WMHs are associated with 1) cognitive decline (lower attention and information processing

2
speed and impaired executive function 4–6 2) increased risk of depression 7,8, gait problem 9, and
most notably increased chance of dementia and stroke 3.
There are several terms that are often used interchangeably to describe WMHs; this is an
unfortunate consequence of the development of the literature in this field. A systematic review of
940 studies by Wardlaw and colleagues in 2013 revealed that there are as many as 50 different
terms that have been used to describe WMHs, including leukoaraiosis, white matter lesions,
white matter changes, and white matter disease 1. This position paper recommends WMHs be
defined as white matter hyperintensities of presumed vascular origin.
Figure 1: WMHs in two 80 year old patients. WMHs are best visualized on T2 weighted fluid
attenuated inversion recovery (FLAIR) images. Left: minor amounts of WMHs voxels. Right:
more pronounced WMHs in both periventricular and deep WM regions (Adopted from Debette
et al. 2010).
1.1.2 Etiology and Consequences of WMHs Leukoaraiosis is derived from the Greek word leuko, “white” and araios, “rarefaction”. WMHs
(leukoaraiosis) were first described as radiological findings in 1986 10 and was later followed by
attempts to provide a pathological description 1. The etiology of WMHs is not completely
understood, however there are histopathological, epidemiological, and physiological studies that
provide important information.

3
WMHs tend to accumulate in the deep white matter and regions around the lateral ventricle
(periventricular WM). Deep medullary arteries provide the main blood supply to these regions.
The limited number of arteries that supply blood to the deep white matter with little collateral
supply along with their susceptibility to vascular pathology make the deep WM more vulnerable
to ischemia. Also, these vessels are among the longest in the brain and often become tortuous
and compromises cerebral blood flow.
From a pathological perspective, endothelial damage caused by various factors such as
hypertension may lead to vessel wall thickening and narrowing of the vessel lumen in arteries
supplying the WM. Endothelial damage may also result in the disruption of the blood brain
barrier. Consequently, blood plasma and other substances that cannot pass the blood brain barrier
may penetrate to the brain tissue and damage the cells. Histopathological studies of WMHs have
found evidence of demyelination, loss of glial cells axon damage and spongiosis 11. It has been
suggested that the incomplete infarcts (i.e. demyelination, axonal and oligodendrocytes damage)
are the consequences of impaired haemodynamics and subsequent ischemia 12,13. A number of
vascular pathologies are also shown to be associated with WMHs including tortuous arterioles,
and periventricular venous collagenosis. Overall, there is ample evidence that WMHs is driven,
at least in part, by chronic ischemia.
Aside from arterial dysfunction, there is a form of venopathy that has also been observed in the
periventricular regions of patients with WMHs. First described by Moody and Brown, the
periventricular venous collagenosis is manifested by deposition of collagen in the venous walls
resulting in intramural thickening and stenosis of veins 14. It has been shown that venous
collagenosis increases with age and is positively correlated with the severity of periventricular
WMHs 14,15. Venous collagenosis can result in ischemia via two mechanisms 1) increasing
vascular resistance and 2) leakage of fluid resulting in vasogenic edema (vessel leakage) 16. It has
also been suggested that venous collagenosis may cause the veins to dilate and result in “venous
insufficiency”, a condition characterized by impaired venous flow and damaged vessel function 16.
Global changes in cerebral physiology support the notion that WMHs are caused by underlying
ischemia. Investigation of alterations of cerebral blood flow (CBF) in patients with WMHs using
neuroimaging started in early 1990s 17. More recently Marstand et al. and O’Sullivan et al. have

4
used contrast-enhanced MRI to study CBF in WMHs and NAWM of elderly cohorts 18–20. The
common findings of the studies that have investigated CBF in relation to WMHs are that 1)
relative to age matched controls, the WMH cohorts have lower CBF both globally and in their
NAWM and 2) in individuals with WMHs, CBF is lower in the lesions compared to NAWM.
Apart from CBF measurements, the hypothesis that WMHs are ischemic in nature have been
tested more directly via measurements of oxygen extraction fraction (OEF), defined as the
fraction of oxygen taken out from the blood at the level of capillaries, and cerebral metabolic rate
of oxygen (CMRO2) using positron emission tomography (PET). Meuguro and colleagues have
shown that when a group of 21 adults with periventricular WMHs are divided into two groups
with mild and more severe lesion loads, the group with more severe WMHs has lower gray
matter CBF, and higher OEF compared to the first group 21. Hatazawa et al. have studied
asymptomatic patients with WMHs and normal controls and have found reduced CBF and higher
OEF in the WM of the patient group compared to the control. WMHs and its relationship with
hemodynamic measures in symptomatic patients have also been investigated. Patients with a
dementia as well as WMHs have higher cerebral cortex OEF and lower CBF compared to
hypertensive controls suggesting that hemodynamic impairment in the cortex could be related in
parts to the “disconnection of neural fibers in deep WM” 22. Yamaji and others have reported that
Alzheimer’s disease (AD) patients with WMHs have lower regional WM and GM CBF and
higher OEF compared to patients with AD alone 23. Similarly, in a group of patients with lacunar
stroke Nezu et al. demonstrated a reduction in CBF and CMRO2 and an increased OEF in
patients with severe WMHs compared to those with mild WMHs 24. Lastly, it has repeatedly
been reported that among patients with carotid artery occlusive disease, those with WMHs tend
to have lower CBF and higher OEF compared to WMHs-negative patients, which suggests that
hemodynamic impairment plays a role in pathogenesis of WMHs 25–27. The increased OEF can
be viewed as an attempt to maintain oxygen delivery to tissues due to impaired haemodynamic.
The observation that WMHs are associated with problems in grey matter (GM) is notable. WM
consists of glial cells and axons and is responsible for the transmission of neural signals between
different brain regions. Therefore, structural or functional impairment of WM can negatively
affect the information processing speed and tasks that require complex communication across the
brain. The association between WMHs and GM hypoperfusion is less clear, but it may be related
to the fact that both WMHs and GM hypoperfusion are consequences of a systemic brain injury.

5
Overall, it is reasonable to conclude that WMHs are associated with reduced CBF and increased
OEF. In the hypoperfused state the OEF should increase as a compensatory mechanism to meet
metabolic demand, hence preserving CMRO2. As the CBF falls further, uncoupling between
oxygen delivery and metabolic rate occurs, resulting in a decrease of CMRO2, which highlights
the condition when increased OEF cannot compensate the effects of reduced CBF. A decrease in
CMRO2 is often associated with loss of neuronal functionality and cognitive decline.
1.1.3 Geometrical Location of White Matter Hyperintensities
WMHs are typically formed around the horns of the lateral ventricles (See Figure 1). These
periventricular lesions tend to grow larger and spread towards the lateral wall of the ventricles
and then into the deep white matter (i.e. closer to the grey matter). Other than these
periventricular WMHs, some lesion are formed in the deep white matter far away from the
ventricles. In general, the bigger and the more confluent the lesions the more severe they are.
Age related WMHs have a specific pattern. The deep white matter in the temporal lobe almost
never has any WMHs, except in more rare cerebrovascular conditions 28. A hereditary form of
covert stokes known as cerebral autosomal dominant arteriopathy with subcortial infarcts and
leukoencephalopathy (CADASIL) is one example where WMHs are diffuse in many white
matter regions, including the temporal lobe.
1.2 Overview of Magnetic Resonance Imaging: Principles and Relevant Techniques
This section briefly discusses the general principles of magnetic resonance imaging (MRI) and
the imaging techniques that are used in this thesis, namely susceptibility-weighted imaging
(SWI), and arterial spin labeling (ASL).

6
1.2.1 Basic Principles of MRI
While a complete and accurate description of MR physics requires quantum mechanics, a
classical description can adequately explain the majority of macroscopic events. This section
uses this classical treatment to briefly describe the basics of MRI.
Atoms with an odd number of protons and/or an odd number of neutrons have a property known
as nuclear spin angular momentum. This spin angular momentum is a vector quantity and is
often called simply the spin. It can be visualized as a charged particle spinning around an axis
producing a magnetic field similar to that of a bar magnet. In the human body, the hydrogen (H)
atom, with a single proton, is highly abundant and the most studied atom that possess a spin that
is used to generate an MRI signal. In the absence of an external magnetic field, the spins of
individual atoms are oriented in random directions resulting in zero magnetization (the vector
sum of spins is zero). When an external magnetic field B0 is applied, the spins exhibit two
important behaviours. First, the spins that were randomly oriented now tend to align in the
direction of the external magnetic field (the z direction by convention) producing a net
magnetization M. Second, the individual spins also precess around the axis of the of external
magnetic field with a resonance frequency known as the Larmor frequency, ω, which is
proportional to the applied magnetic field and a unique atom specific constant known as the
gyromagnetic ratio γ. The following equation represents the relationship between the Larmor
frequency, the external magnetic field and the gyromagnetic ratio:

7
Figure 2: A) The radiofrequency field B1 applied in the transverse direction and tuned to the
Larmor frequency so as to rotate the magnetization. B) Behaviour as seen from a rotating frame
of reference. (Adopted from Nishimura 1996)
In the presence of an only constant B0, the spins continue to precess at the Larmor frequency and
no change in the magnetization vector is observed. In order to obtain an MR signal, the
equilibrium state of spins should be disturbed. This is done by applying a radiofrequency
magnetic field B1 at the resonant frequency of the spins in the x-y (transverse) plane. The
application of this radiofrequency pulse moves the spins out of equilibrium, and rotates the net
magnetization towards the x-y plane (see Figure 2). The amount of rotation depends on the
strength and duration of B1. When the pulse is turned off, the magnetization continues to precess
at the Larmor frequency and also starts to return back to its equilibrium state along the z-axis
characterized by the longitudinal time constant T1. While the longitudinal magnetization is
recovering along the z axis, the transverse magnetization decay due to spin-spin interactions
resulting in the dephasing of the spins. The rate at which this dephasing takes place is given by
T2 transverse relaxation time. These processes are independent of each other and are briefly
explained in the following subsections.
The rotating magnetization induces an electromotive force (emf) in a receiver coil based on the
Faraday’s law of induction. This MR signal is then used to reconstruct images. However the MR
signal is not recorded immediately after flipping the magnetization into the transverse plane. The
signal is measured after a short period of time known as the echo time or TE (time to echo). The
choice of TE is of critical importance since it contributes to the type of contrast that we see in the
final image.
Figure 3: Precession of the magnetization vector in the xy-plane and generating an emf, which is
detected by the receiver coils. (Adopted from Nishimura 1996)

8
The RF receiver coil(s) in MRI record the total signal generated by all the spins in an excited
region. Since the excitation done by B1 is not spatially selective, spatial localization is required
and is obtained by using linear gradients. This process starts with the selective excitation of a
slice in one direction (z direction for example) via the application of slice selective gradient Gz.
Then the application of an RF pulse excites the magnetization and rotates it toward the xy plane.
During the decay of this magnetization and while a signal is being detected a second gradient in
the x direction is applied which is known as the frequency-encoding gradient. The strength of
this gradient is linearly changing as a function of x. As a result, different spins at different x
positions now precess at different frequencies. This frequency encoding implicates that the
precession frequency can be used to distinguish the spatial location of the spins in the x
direction. Lastly, to localize the spins in the y direction a third gradient known as the phase
encoding gradient is applied. This results in a phase offset among spins in the y direction. This
gradient is turned on with a constant strength prior to the detection of the MR signal. Then the
frequency-encoding gradient is applied and the signal is detected simultaneously. The process is
then repeated with different Gy strengths. It should be noted that the method described above is
only one of the common ways of applying the gradient in MRI.
1.2.2 Contrast in MRI
Image contrast in MRI is due to the fact that biological tissues have unique relaxation time
constants, which results in differences in the evolution of their magnetization and hence the MR
signal. The relaxation time is a property of a material and its surrounding tissues and therefore is
fixed. In this section the T1 and T2 relaxation constants and their significance in MRI is briefly
discussed.
1.2.2.1 T1 Relaxation Time
The T1 relaxation time (also known as longitudinal or spin-lattice relaxation time) is related to
the rate at which spins transfer their energy to the surrounding after the administration of the RF
pulse. The faster the spins transfer their energy the faster they return to their lowest energy state
along the z direction. Immidiately after the RF excitation pulse the length of the transverse

9
magnetization decays and consequently the longitudinal component of the magnetization (Mz)
recovers to its pre-excitation state as given by the following equation.
After a while another RF pulse is applied and the longitudinal magnetization is flipped into the
transverse plane again and the same recovery follows. The time interval between two
consecutive excitations is known as the repetition time or TR. When the frequency of the motion
(translational, vibrational and rotational) of protons matches the Larmor frequency the maximum
energy transfer takes place. In the body the motional frequencies of hydrogen protons in fat is
almost equal to the Larmor frequency of hydrogen. Therefore fat has the greatest ability to
transfer energy to its surrounding hence the shortest T1.
1.2.2.2 T2/T2* Relaxation Times
After the adminesteration of an RF pulse and while the longitudenal magnetization is being
recovered along the z direction, the tranverse magnetization undergoes an independent form of
decay. Immidiately after the RF pulse, all the spins that constitute the transverse magnetization
are in phase (i.e. rotating with the same angular velocity). However, as time goes by the spins
dephase which and therefore their vector sum decreases. The dephasing process is a result of two
phenomena namely the spin-spin interaction and magnetic field inhomogeneities. The former is
explained by the T2 time constant while the latter denoted by the T2’ relaxation time. The
overall rate of dephasing can be written as:
and the magnetization in the x-y plane decys base on the following:
where t is the time after excitation.

10
1.2.3 Susceptibility-weighted Imaging (SWI)
Susceptibility-weighted magnetic resonance imaging (SWI), as we know it today, is a recently
new imaging technique, first described in 1997 by Reichenbach and Haacke, and has gained
clinical use in the past decade 29,30. Historically, it was known as the high-resolution BOLD
venographic (HRBV) technique where BOLD stands for the blood oxygenation level-dependent.
Later on, when it was used in clinical applications, the term AVID BOLD was coined to the
technique where AVID stands for the application of venographic imaging to diagnose disease.
The term susceptibility-weighted imaging or SWI was suggested in 2004 to highlight the broader
application of the technique, which goes beyond the visualization of the cerebral veins 31. It is
entirely appropriate to view the development of SWI in parallel with the BOLD fMRI technique
for functional brain activation. In the former case, acquisition time is dedicated towards spatial
resolution, whereas in the latter case BOLD volumes are acquired repeatedly, i.e. every
2seconds, at the expense of spatial resolution.
Magnetic susceptibility χ is an intrinsic property of materials that describes the degree of
magnetization of an object when placed in an external magnetic field and is given by
where M is the induced magnetization, and H is the external magnetic field.
The relationship between induced magnetic field inside an object and the external magnetic field
can be written as

11
where is permeability [N.A-2], is permeability in vacuum and is equal to 4π×10-7 N.A-2 and
is the relative permeability. The above equation shows that the induced magnetization M is
proportional to both susceptibility and the magnetic field.
Materials with susceptibility of greater than zero are called paramagnetic and substances with
negative susceptibility are called diamagnetic. Changes in magnetic susceptibility result in
magnetic field inhomogeneity which in turn affects the T2* relaxation of the nuclei. It has been
shown that the blood T2* is a quadratic function of oxygen saturation (Y), but can be estimated
as a linear function over a wide range of Y 32. For blood with oxygen saturation of Y the signal as
a function of echo time can be written as
The change in magnetic susceptibility not only changes the signal intensity on the T2 or T2*
weighted image, but also results in the changes in the phase of the MR signal. The measured
phase is proportional to the local change in the magnetic field and also to the echo time (TE).
Starting with the Larmor equation
The phase can be written as
and the phase difference between two tissues after a time of TE would be
€
Δϕ = ΔωTEΔϕ = (γΔB)TEΔϕ = γ (ΔχB0)TE
Different tissue types and structures in the brain have different magnetic susceptibilities, which
can result in local a magnetic field inhomogeneity. For example, hemoglobin has two
oxygenation states depending on whether it is bounded to oxygen or not. When bounded to
oxygen, the oxyhemoglobin is slightly diamagnetic compared to most brain tissues. The state
where the oxygen is not bounded to the hemoglobin is deoxyhemoglobin and is paramagnetic

12
compared to surrounding brain tissue. The deoxygenated blood, which is more abundant in the
cerebral veins (with oxygenation levels of approximately 60%) than in cerebral arteries (with
oxygenation levels that are close to 100%), has Δχ ≈ 0.27 ppm 33 compared to surrounding
tissue. This susceptibility difference of the venous blood is the basis of SWI venography. When
vessels are modelled as infinitely long cylinder (as an approximation of long cerebral veins with
diameter much smaller than their length), the magnetic field between the vein and the
surrounding can be written as
€
ΔB = 2π⋅ Δχ⋅ B0 ⋅ cos2θ −
13
⎛
⎝ ⎜
⎞
⎠ ⎟ ⋅ (1−Y )⋅ Hct
where Δχ is the susceptibility difference between deoxygenated and oxygenated blood, B0 is the
strength of the main magnetic field, θ is the angle the angle between B0 and the blood vessel, Y is
the oxygen saturation of the blood inside the vessel, and Hct is the hematocrit34,35. For a cerebral
vein, which is running parallel to the magnetic field, the TE that results to the maximum phase
difference can be calculated. Setting Y = 0.7, Hct = 0.40, and Δχ=0.27×10-6, as suggested by
Koopmans and colleagues, the TE that corresponds to a phase difference of π (i.e. maximum
signal cancelation on the phase image) is equal to 28 ms 35. When θ ≠ 0, the situation becomes
more complicated due to the contribution of extravascular magnetic field components in addition
to the above intravascular field difference and the analytical calculation becomes nontrivial 34,35.
SWI is a gradient echo imaging technique. A conventional SWI is performed at high spatial
resolution (i.e. in plane voxel dimensions are less than 1 mm), with 3D imaging (i.e. phase
encoding in two directions), and with flow compensation in all three directions (i.e. x, y and z).
SWI is fairly unique in MRI because both magnitude and phase signals are used in the
reconstruction to form the susceptibility-weighted composite image. The reason for this is based
on the following: changes in magnetic susceptibility lead to changes in local magnetic field.
These field inhomogeneity result in two notable effects. First, a reduction of T2* relaxation time
which corresponds to areas of lower signal intensity on a magnitude image. Second, a phase shift
is observed compared to the surrounding regions as reflected by the phase image. SWI is
designed primarily to produce an impressive magnitude image and the phase image is used to
accentuate the magnitude tissue differences. Therefore, the acquisition parameters are chosen
such that the final image would be of adequate quality.

13
SWI post-processing is based on the following. First the phase images are unwrapped, where
multiples of 2π are added or subtracted such that the 2π discontinuities in the phase images are
removed. Then macroscopic magnetic field variations, which arise from sources such as
background field inhomogeneity, are removed by applying a high pass filter. The unwrapped
filtered phase image now has high frequency phase variations corresponding to local areas of
changes in magnetic susceptibility.
The filtered phase mask, which has values between -π and π, is now used to create a so-called
“phase filter”, which is designed to enhance the contrast of the magnitude image. The phase
mask f(x), suppresses voxels with certain phase and is usually designed in the following manner:
The phase mask defined above has values between zero and one. If a voxel has a phase shift of –
π it will be completely suppressed, whereas those with values between –π and 0 are partially
suppressed. This phase mask is then multiplied by the magnitude image, ρ(x), a number of times
to provide a unique form of contrast. It has been shown that four times multiplication produces
the optimal contrast for detection of cerebral veins 36. The resultant composite image (i.e. f 4(x)
ρ(x)) is called the susceptibility-weighted image.
SWI produces images that are T2* weighted, hence it requires an image acquisition with a long
TE. In conventional gradient echo imaging a long TE results in longer TR hence increasing the
acquisition time. When long TE in combination with fast imaging is desired, echo-shifted (ES)
pulse sequences could be employed where TE is longer than TR. In a simple ES gradient echo
pulse sequence, modified gradient lobes are applied such that the gradient echo will be formed
with a minimum delay of one TR hence making the TR shorter than TE and decreasing the scan
duration (See Figure 4).

14
Figure 4: A general example of an ES pulse sequence where gradients lobes with areas of –A
and +2A are added prior and after each readout to shift the echo by one TR interval (Adopted
from Bernstein et al. 2004 37).
1.2.4 Clinical Applications of SWI
MR venography with deoxygenated haemoglobin as an intrinsic contrast agent and with the use
of both phase and magnitude images began with the work of Reichenbach and Haacke in 1997 38.
Subsequently, the feasibility of MR venography at 3T was shown by Reichenbach et al. in 2000 34. Figure 5 shows a typical SWI image at 3T, where deep medullary veins are clearly
distinguishable. Since 2004 there has been a unified understanding of SWI processing techniques
and major MRI vendors have adopted the SWI sequence 31. SWI has established its position in
clinical settings as well. Nowadays, SWI has clinical application in both adult and paediatric
neuroimaging. This section focuses mostly on the clinical applications of SWI in adults. An in
depth review of the clinical application of SWI in children has been written by Tong 39.

15
Figure 5: A typical SWI from a healthy participant. The hypointense lines are the cerebral veins.
To date SWI has been used in following settings to provide additional or complementary
information: traumatic brain injury (TBI), hemorrhagic disorders, stroke, cerebral autosomal
dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL), multiple
sclerosis (MS), vascular malformations and venous disease such as cerebral cavernous
malformations (CCM), developmental venous angiomas (DVA), and cerebral venous sinus
thrombosis (CVST), brain tumours, amongst other diseases. A complete review of the literature
is beyond the scope of this thesis. This section briefly comments on the studies that are more
relevant to CSVD.
The literature shows that MS is the clinical population that has garnered the most attention from
SWI research. Multiple sclerosis (MS) is a condition in which the utility of SWI has been studied
extensively. MS is an inflammatory disease of the brain and spinal cord. Demyelinated plaques
are the hallmark of MS and are often presented as WM lesions in the subcortical and
periventricular regions. MS researchers have focused on the structure of the lesions to better
characterize the disease. Pathological studies have shown that MS lesions are veno-centric.
Therefore detecting a central veins within MS lesions could serve as a biomarker. SWI has
successfully revealed that most MS lesions exist around a vein and it is demonstrated that the
percentage of lesion with a central vein as detected on SWI can serve as a diagnostic marker of
MS with high sensitivity and modest specificity 40,41. Furthermore it has been reported that the

16
visibility of veins decreases in periventricular WM in MS patients, and this observation was
reported to correlate with the lesion load 42–44. Others theorize that this finding is the result of
decreased oxygen utilization and oxygen extraction in MS, which leads to a lower
deoxyhemoglobin concentration in the draining veins, diminishing the visibility of them 42,44.
SWI is sensitive in detecting hemorrhages and has been used in assessing stroke. When the
arterial blood flow is impaired, due to thromboembolism for example, the deoxyhemoglobin
content of the draining veins increases. This results in more prominent veins in the area of
impaired perfusion as seen on SWI. An example of the utility of SWI in assessing acute cerebral
ischemia is shown in Figure 6.
Figure 6: 59 year old patient with sudden onset of right hemiparesis and speech deficit. A. MRA
shows lack of time of flight signal in the distal M1 segment of the left MCA. B and C. SWI
shows prominent subcortical veins within the left MCA territory suggestive of increased
deoxyhemoglobin in the draining veins. D) The regional CBF is reduced on the affected
hemisphere (Adopted from Mittal et al. 2009 45).
Lastly, is the clinical utility of SWI to study moyamoya diseases (MMD), a relatively rare brain
condition except among Asian populations. MMD is characterized by constriction of the terminal
braches of the internal carotid arteries leading to development of abnormal collateral vessel
networks. The word moyamoya is derived from a Japanese word meaning “puff of smoke”
explaining the appearance of these collateral vessels. Patients with MMD suffer from impaired
perfusion, lower cerebrovascular reserve, and have increased oxygen extraction. It is shown that
the prominence of vein increases in MMD patients that suffer from TIA and infarct. These
findings suggest that the increased visibility of draining veins of the deep white matter is an

17
indication of increased oxygen extraction, or venous stasis, both of which are in parts of the
characteristics of misery perfusion 46.
1.3 Cerebral Venous Vasculature
1.3.1 Normal Anatomy
Cerebral veins are divided based on their location and direction of blood flow into two groups:
superficial and deep. The superficial venous system begins in the WM 1-2 cm below the cortex
and consists of short vessels that direct the blood towards the skull and join the pial veins. The
veins of the deep system are responsible for draining the white matter. The deep medullary veins
originate below the superficial veins, travel in an opposite direction towards the ventricles and
join the subependymal veins near the lateral ventricles. At the level of the lateral ventricles, the
deep medullary veins run parallel to each other joining the subependymal veins at almost right
angle. They are highly visible on SWI images and attention is paid to their appearance in this
thesis for a few reasons, namely their consistent anatomical location and their proximity to
WMH lesions. These veins (purple in the image below) have been the subject of investigation in
MS, stroke and moyamoya disease and have been described based on their prominence, numbers
and density.
Figure 7: Anatomy of the cerebral vasculature A) A coronal venogram shows a network of deep
medullary veins draining the WM into subependymal veins near the lateral ventricle. B) A
coronal brain slice showing the normal arterial branching. [Adopted from Okudera et al. 1999 47]

18
Figure 8: Anatomy of deep medullary veins. A venogram map obtained from manually
segmenting a SWI images, performed by an expert neuroanatomist, demonstrates the rich venous
network around the ventricles. Colours from red to purple correspond to the level of the vessel
along the z-axis from bottom to top. [Courtesy of Fuqiang Gao, Sunnybrook Research Institute].
1.3.2 Interpretation of Venous Signal on SWI
The vessel size, and the concentration of deoxyhemoglobin both contribute to the visibility of a
vein on SWI. In addition, in SWI the ability to detect a vein depends on the voxel size as well. It
has been shown that axial images are most sensitive in detecting veins that are perpendicular to
the main magnetic field when non-isotropic voxels are chosen with the slice thickness being
larger than the in-plane resolution.
The deoxyhemoglobin content of veins is modulated by at least two factors namely the oxygen
extraction fraction and the blood flow. Increased oxygen extraction fraction increases the
concentration of deoxyhemoglobin which results in increased magnetic field inhomogeneity,
spin dephasing and signal loss. The cerebral blood flow can also alter the oxygenation level of
the veins. For example, Sedlacik and others have shown that an increase in CBF results in an
increase of the oxygenation of cerebral veins from approximately 0.5 to 0.7 48. Therefore, it is
plausible to postulates that decreased CBF leads to an increase in the deoxyhemoglobin content

19
of the veins increasing their prominence. This has been demonstrated in the context of acute
stroke as mentioned in section 1.2.4.
All in all, while the increased visibility of the veins as detected on SWI is multifactorial, it could
represent a combination of increased oxygen extraction fraction, reduced CBF, venous stasis and
venous dilation 39, all which have been associated with CSVD and WMHs as discussed
previously in section 1.1.2.
1.4 Arterial Spin Labelling (ASL)
Cerebral blood flow (CBF) is a robust physiological entity that is affected in many neurological
conditions. It is defined as the volume of the blood going through a region per unit time and is
often measured in (millilitres of blood)/(100 gram of brain tissue)/(minute). This section briefly
discusses CBF quantification.
CBF can be measured using nuclear imaging (SPECT and PET) and MRI. Perfusion imaging
makes use of a tracer of some sort that flows with the blood and passes through tissues. If the
inflow and outflow rate of the tracer to and from the tissue are known, then the amount of tracer
that remains within the tissue at any given time would be proportional to the CBF.
Arterial Spin Labelling (ASL) is a non-invasive MR technique that uses magnetically labelled
water as a tracer to perform perfusion imaging. To obtain ASL images the arterial blood is
magnetically labelled prior to getting into the region in which measurement is going to be
performed (i.e. the imaging plane). This tagging process is done by using a radiofrequency
inversion pulse, which inverts the net magnetization of the water molecules (by 180 degrees).
The labelled blood now travels for some time (transit time) to reach the imaging plane where
water molecules with inverted spins are exchanged with the water molecules of the tissue. With
the arrival of inverted spins the net magnetization of the tissue is reduced hence altering the
tissue’s T1. An image is now acquired which is known as the tagged image. A greater flow to a
volume of interest corresponds to a greater change in the magnetization. Next a so-called control
image is acquired in which the magnetization of the arterial blood is not inverted. Subtracting the

20
control image from the tag image results in a map of magnetization change, which can be
thought as a map of the concentration of tracer, which is in turn proportional to CBF.
Figure 9: Steps in ASL image acquisition. Left: Spins in the arterial blood (carotid artery) is
tagged before reaching the imaging plane. Right: A control image is obtained without inverting
the magnetization of the arterial blood.
1.5 Image Analysis: A Synopsis of Registration and Segmentation Techniques
With the advance of neuroimaging, access to tremendous amount of data, and a paradigm shift
from qualitative approaches to more quantitative analysis, advanced image analysis techniques
have evolved and are used routinely in clinical and non-clinical settings. For example, a
multimodal approach towards neuroimaging has resulted in availability of multiple images for
which the analysis requires fast and robust inter and intra subject registrations. Similarly, to
obtain fast and accurate automatic segmentation of various tissue types and structures, and to
acquire quantitative measures such as disease burden, reliable and readily available segmentation
and quantification tools are needed. This section briefly comments on the basics of the
techniques used frequently in this thesis.

21
1.5.1 Image Registration
In image analysis, registration is the process of aligning multiple images in a common coordinate
system. The task is to find a transformation that when applied to an image, would align it to
another image. Often this is treated as an optimization problem. A cost function is defined which
characterizes the goodness of the registration. The more similar the two images after registration
the lower the value of the cost function. Therefore, minimizing the cost function results in the
desired transformation, which produces the best registration. The cost functions used in MR
image registration are often intensity based meaning that they rely on intensity patterns.
Examples of this class of cost functions include Correlation Ratio and Mutual Information.
The transformation used to register images can be divided into two groups namely linear and
non-linear. Linear transformations are global which means that they affect the entire image in the
same manner. Also known as affine transformations, they preserve the lines and planes, keeping
parallel lines parallel. A linear transformation with 6 degrees of freedom (DOF), known as rigid
body, involves translation and rotation in 3 directions. This type of transformation is often being
used for inter-subject registration, for instance when a subject’s FLAIR image needs to be
registered to its own T1 anatomical image. Affine transformation with 12 DOF has 6 additional
DOF (3 scaling and 3 skews/shears) in addition to those of a rigid body transformation and is
often used for initializing a non-linear registration. Non-linear transformations use more than 12
DOF, and can be local meaning that they warp different regions of the image differently. Often
following an affine transformation, they are used to perform between subject registrations.
1.5.2 Image Segmentation
This thesis does not focus on developing image segmentation algorithms. It rather aims to utilize
such techniques to obtain quantitative measures. However, it would be useful to comment on a
specific algorithm, which has been used in this work to perform vessel segmentation.
As mentioned in section 1.2.4, the utility of SWI as a venography technique has been established
previously. While the investigation of venous vasculature is often limited to visual inspection
and grading, a number of vessel segmentation algorithms have been employed to perform more
quantitative analyses. These methods can be classified into two categories namely thresholding
approaches, and feature based techniques. The former of these techniques relies on the fact that

22
the veins are hypointense on the SWI images and they try to isolate the veins with repeated
thresholding. On the other hand, the feature-based techniques are designed to identify the vessels
based on their structure namely their tubular nature. One such technique, which aims to enhance
vessel structures, is the Frangi algorithm49.
This algorithm uses the eigenvalues of the Hessian matrix (generated by the second derivatives
of the image intensities in three spatial directions) to assess local orientation and consequently to
locally determine the “vessel likeness”. It follows from geometric analysis of the Hessian that the
eigenvectors in 3D correspond to three orthonormal directions, which describe the second order
structure of the image. In the case of a vessel, the eigenvalue along the direction of the vessel
will be small denoting a small intensity variations. The intensity variation perpendicular to the
vessel direction is on the other hand significant and is represented by a large eigenvalue.
Therefore, for an ideal tubular structure one eigenvalue should be close to zero and the others
should be large.
In the 2D Frangi algorithm, two terms are defined to distinguish vessels from other structures in
the image. First, a blobness measure is defined as the ratio of the two eigenvalues. Second, to
eliminate background structures, a second order “structureness” is defined as the sum of the
squares of the eigenvalues. For pixels in the background this term would be small since they
have small eigenvalues due to lack of contrast. Finally, a “vessel likeness” function is defined
which relates the blobness and structureness measures into an estimate of vessel likeness. The
segmentation method is explained in more detail in section 2.3.2.

23
“Everything we call real is made of things that cannot be regarded as real.” Niels Bohr
2 Methods As mentioned in Chapter 1, CSVD is associated with impaired perfusion, increased oxygen
extraction fraction (OEF) in the WM, and venous pathology manifested as venous stasis and
dilation among others. Moreover, the prominence of veins as seen on susceptibility weighted
imaging (SWI) has been associated with increased concentration of deoxyhemoglobin in the
veins secondary to increased OEF and impaired perfusion.
Therefore, SWI is well suited to study and characterize the cerebral effects of SVD, namely
because it provides imaging contrast that relates to venous anatomy and physiology that are
consistent with the spectrum of SVD pathologies. In the current chapter the methodology used to
facilitate the use of SWI and other imaging techniques to advance our current understanding of
CSVD is introduced. It is hypothesized that pathophysiological changes associated with CSVD
affect the prominence of the draining veins of the white matter as seen on SWI.
2.1 Participants
This thesis focused on a cohort of elderly individuals with suspected underlying CSVD. These
adults typically report having subjective memory complaints and were recruited to participate in
research from the cognitive neurology clinic at Sunnybrook Health Sciences Centre. The data
presented in this chapter is part of a longitudinal project that attempts to predict the expansion of
WMH on the basis of cerebrovascular reactivity patterns (study was funded by the Canadian
Stroke Network). A sample of 25 patients for whom SWI with adequate image quality was
available was included in this study. Inclusions criteria included known WMHs based on
previous neuroimaging findings or medical history suggestive of having WMHs. Exclusion
criteria included: individuals with CADASIL, Alzheimer’s disease, history of severe carotid
stenosis, and cortical infarcts. Cognitive screening was performed by a trained psychometrist
using Montreal Cognitive Assessment test (MOCA). The Research Ethics Board at Sunnybrook
Research Institute approved the study and informed consents were obtained from the
participants. The demographic information of the cohort is presented in Table 1.

24
Participant Demographics (N=25) Mean±std* (Median) %
Age (years) 73.2±9.3 (72.8)
Women 44 (11/25)
MoCA 24.2±4.6 (24) 24
Hypertension
CADASIL
Stroke, TIA
Diabetes
48 (12/25)
0 (0/25)
8 (2/25), 4 (1/25)
12 (3/25)
*std: standard deviation
Table 1: Demographic data on participants
2.2 MRI Image Acquisition
Patients were scanned on a Philips 3.0T Achieva MRI system using a body coil transmission and
an eight-channel head coil at Sunnybrook Research Institute. A comprehensive imaging protocol
including T1-weighted, FLAIR, PC-ASL and SWI was implemented.
T1-weighted anatomical images were acquired with TE =2.3 ms, TR = 9.5 ms, flip angle = 8°,
256x164 matrix, 0.94x1.2x1.2 mm3 voxel size, and a total time of 8:26 min. T1-weighted images
were used for tissue type segmentation (i.e. grey matter, white matter and cerebrospinal fluid).
T2-weighted FLAIR images were acquired for visualization and delineation of WMHs. Imaging
parameters for axial FLAIR included TE=125 ms, TR=9000 ms, flip angle=90°, TI=2800 ms,
FOV=24 cm, matrix size of 240x217, voxel dimensions of 1x1.1x3 mm3, and an acquisition
duration of 5:30 minutes.
SWI was acquired using a 3D shifted echo sequence (i.e. TE>TR; see section 1.2.3) with TE=41
ms, TR=29 ms, flip angle of 15°, FOV=23 cm, 460x365 matrix, voxel size of 0.48x0.48x2.8

25
mm3 and scan duration of 4:51 min. The scanner produced the post-processed SWI image using
the conventional approach (i.e. 4 times multiplication of the phase mask with the magnitude
image).
Pseudo-continuous arterial spin labelling (ASL) was performed to obtain perfusion using echo
planar imaging. Scan parameters were: TE=9.7 ms, TR=4000 ms, 18 slices, 64x64 matrix,
3x3x5 mm3 voxels. Thirty-five control and tag pairs were obtained with the labelling plane 80
mm below the imaging volume (i.e. label offset=80mm and prescribed over the internal carotid
and vertebral arteries), post label delay (PLD) of 1600 ms and label duration of 1650 ms, leading
to a total acquisition time of 4:48 min. For absolute CBF quantification a reference ASL scan
was acquired with TE=20ms, TR=10000 ms, 18 slices, 64x64 matrix, and 3x3x5mm3 voxels.
ASL images were co-registered using FMRIB’s motion correction tool, MCFLIRT. The tagged
images were then subtracted from the controls and their time average was calculated. The ASL
reference image was used to measure the magnetization of the arterial blood (M0) by using an
exponential decay model. The CBF in mL/100g/min was calculated using the following
equation:
where 60 provides units of sec/minute, 100 provides units of 100 g of tissue, ∆M is the ASL
signal difference between label and control image, α=0.83 is the labelling efficiency, M0 is the
equilibrium magnetization image, PLD=1.60s is the post-label delay, TE=0.020s is the echo time
of the ASL images, T1,b=1.68s is the T1 of arterial blood, T*2,t=0.06s the effective relaxation time
of GM tissue
2.3 Image Processing
2.3.1 Brain Segmentation The brain segmentation was done using the FSL software package and a number of shell and
MATLAB scripts developed in-house. FSL is a comprehensive set of tools for neuroimaging
developed by Oxford Centre for Functional MRI of the Brain (FMRIB), Oxford, England. The

26
image processing in this thesis started with the extraction of the brain from the skull on T1-
weighted images using the FMRIB's Brain Extraction Tool (BET). The skull stripped T1 images
were then used to classify the different tissue types (GM, WM and CSF) using FMRIB's
Automated Segmentation Tool (FAST). WMHs were automatically segmented on the FLAIR
images using the Fuzzy Lesion EXtractor (FLEX) algorithm, which uses a combination of
intensity thresholding and fuzzy c-mean clustering approaches to segment WMHs (Gibson et al.
2010). Total WMHs volumes were reported as the lesion volume normalized by intracranial
volume to account for the difference in head size 50. Additionally, WMHs at the level of lateral
ventricles (LV-WMHs) were reported as the percentage of the WM with WMH lesions. The
tissue classes (GM, NAWM, WMHs and CSF) were registered to the subjects’ SWI spaces using
FMRIB’s Linear Image Registration Tool (FLIRT) with 7 DOF 51,52. All of the co-registered
images were visually inspected to ensure proper alignment. Vein fraction analysis (as described
later) was performed in the participant’s native SWI space. Figure 10 shows an example of
WMHs and tissue segmentations obtain from the respective FLAIR and T1-weighted images.
Figure 10: An example of WMHs and tissue segmentations. A. A FLAIR image B. A T1-
weighted image C. Tissue segmentation delineating GM (green), NAWM (blue) and WMHs
(light blue).
T1-weighted images were used to construct a study-specific template using Advanced
Normalization Tools (ANTs). This template is shown in Figure 11. A. WMHs in the subject
space were registered to this group anatomical template using the FMRIB’s nonlinear image
registration tool (FNIRT). The WMHs in the group template for different subjects were averaged
to obtain a probability map (Figure 11. B). The T1-weighted group template was segmented into

27
WM, GM, and CSF and the NAWM mask in the group template was obtained by subtracting the
group WMHs probability map from the WM tissue mask. The WMHs was binarized prior to
subtraction to ensure that the group NAWM mask was lesion free (Figure 11. C). This NAWM
mask in the group template ROI was then registered back to subjects’ native T1 space using an
inverse nonlinear transformation.
Figure 11: A. Study-specific T1-weighted group template. B. WMHs probability map in the
group template constructed from averaging template acquired subjects’ WMHs masks. C. Group
template acquired NAWM mask is the “relative complement” of the binarized WMHs mask with
respect to the WM (i.e. voxels that are in the WM but do not belong to WMHs mask).
2.3.2 Venous Segmentation
A 2D implementation of a vein segmentation algorithm, referred to as the Frangi algorithm, was
used to isolate voxels from within veins on the SWI images. An in-house MATLAB script was
used to load the SWI images and perform the Frangi vessel enhancement on a slice-by-slice
fashion. A likeliness function was used to enhance delineation of vessels and is defined in the
following form:
€
ν =
0 if λ2 < 0,
exp −R2
B
2β2
⎛
⎝ ⎜
⎞
⎠ ⎟ (1− exp −
S2
2c 2
⎛
⎝ ⎜
⎞
⎠ ⎟
⎧
⎨ ⎪
⎩ ⎪
where λ1 and λ2 are the eigenvalues of the Hessian matrix with |λ2| > |λ1|, RB is the blobness
measure defined as λ1/ λ2, S is the “structureness” measure and is defined as . The

28
local second order information of the image is described by an ellipse. The direction and length
of the semi-axes of this ellipse are given by the eigenvectors and the magnitude of the
eigenvalues of the Hessian.
The filter used four user-defined inputs. These inputs are explained in the following. Two real
numbers (β and c) are used as thresholds, which control the sensitivity of the vesselness filter to
the “blobness” and “structureness” measures, respectively. The default values of 15 and 500
were used for β and c, respectively, as suggested by Frangi et al. 1998. These choices were
reported to perform well by others 53 and were empirically verified further in this thesis. It should
be noted that the blobness measure introduce here is “grey-level” invariant and remains constant
under intensity rescaling. Also it is expected that the c threshold can remain fixed for a given
application when imaging is done under a standard protocol 49. The Frangi algorithm was
implemented over a range of spatial scales with the goal of optimizing the identification of
tubular structures of different sizes. The spatial scale of the filter was varied iteratively from 0.1
to 1 mm with 0.1 increments 53. Note that this scale size did not determine the actual diameter of
the vessels detected. It only represented the standard deviation of Gaussian kernel used in
calculating the Hessian. It was found that the choice of scale increments did not alter the
segmentation result noticeably as long as the maximum scale did not exceed unity.
The vessel enhancement was followed by a global threshold to obtain binary venogram maps. In
the final analysis only three slices (8.4 mm) at the level of lateral ventricle were used, due to
anatomical orientation and consistency of the deep medullary veins in this location. This was
also consistent with previous choices of slice selection in the literature. For example Zivadinov
et al., Ge et al., and Horie et al. used volumes of interest defined by axial slabs with a thickness
of 10, 8 and 6 mm, respectively.
WM, NAWM, WMHs and GM masks along with the template acquired NAWM masks were
transferred into the native SWI space for every subjects as explained previously. The vein
fraction was then calculated as the number of vein voxels in an ROI divided by the volume of the
ROI . The summary vein fraction value (expressed as %) was used as the dependent variable and
an association was tested with WMHs lesion burden. In a secondary analysis, vein fraction was
used as the independent variable to determine whether within-group differences in vein fraction
contribute to regional difference in perfusion.

29
2.3.3 Visual Rating of White Matter Hyperintensities
While the quantification of WMHs using volumetric techniques provide a quantitative measure
that is related to the disease severity, visual rating scales are also used frequently and notably in
clinical radiology settings. These rating scales provide fast and easy to interpret assessment that
can be further evaluated on the basis of their anatomical location (i.e. deep versus
periventricular). These ratings have a good agreement with quantitative measures and are known
to complement those approaches 1. Among many visual rating scales, the Age Related White
Matter Changes scale (ARWMC), also known as the modified Fazekas scale (named after a
prolific Austrian neurologist Franz Fazekas), is commonly used due to its ease of use and
interpretation 49. In this study, the ARWMC rating scale was used to assign a score based on the
size and arrangement of WMHs as explained in the following. Score 0 represented the absence of
WMHs on the FLAIR image. A score of 1 was assigned when focal lesions were present. This
included small caps around the horn of the lateral ventricles or a “pencil-thin” lining adjacent to
the lateral ventricles. When WMHs began to become confluent a score of 2 was given. Lastly,
score 3 corresponded to “diffuse involvement” in multiple WM regions. This ARWMC scale
was used to rate the WMHs as seen on the FLAIR images. Representative images of individuals
with scores 1 – 3 are shown in Figure 11.
Figure 12: ARWMC rating scale. A. ARWMC Score 1; Focal lesions around the horn of lateral
ventricles (arrows). B. ARWMC Score 2; Periventricular lesions are becoming confluent
(arrow), and multiple deep WMHs are present (arrowhead). C. ARWMC Score 3; diffuse
involvement; periventricular WMHs are extending into the deep WM and vice versa.

30
2.3.4 CBF Measurement: ROI and Voxel-wise Approaches
To measure the CBF in GM, the T1-weighted acquired tissue mask was transformed into the
ASL space. The ASL CBF images were then masked and the mean CBF values were calculated
in the GM tissue ROI. The subjects’ CBF images were registered into the study-specific template
using non-linear transformation. To look at the effect of WMHs and vein fraction on CBF, a
general linear model (GLM) design was used in a voxel-wise fashion. The CBF images in the
group template were used to create a 4D image and an FSL program known as randomise was
used to implement the voxel-wise analysis with 5000 permutations. Age and sex were included
in the GLM as covariates of no interest. Voxels with a signal-to-noise ratio (SNR) greater than 1
across the group were included in this analysis to restrict testing to voxels that were consistently
detected across the group. SNR was calculated as mean divided by standard deviation. To
identify the significant voxels in the voxel-wise analysis, a combination of the intensity threshold
of puncorrected<0.005 and a cluster size threshold of 10 voxels was used. Significant voxels from
the study-specific template were localized on the MNI152 template (ICBM152 non-linear 6th
generation) using a non-linear transformation. Figure 13 shows the mean CBF image, and the
binary SNR mask used in the voxel-wise analysis.
Figure 13: A. The mean CBF perfusion image B. The binary mask used in the voxel-wise
analysis showing voxels with SNR>1.

31
2.4 Statistics The normality of the measured variables was tested using the Shapiro-Wilk test and the p<0.05
was used as the significant threshold. The assumption of the homogeneity of variances was
tested using the Leven’s F test in conjunction with the assumption of normality prior to
conducting an analysis of variance (ANOVA) to compare means. Adjusted F statistics provided
by the Welch and the Brown-Forsythe tests were used when the assumption of the homogeneity
of variances was violated. To test the association between vein fraction measures and WMHs or
CBF, partial correlations were calculated with age and sex included as covariates. To test for the
age and gender differences among ARMWC groups, a chi square test was performed. To
compare the means while controlling for the differences in the covariates, an analysis of
covariates or ANCOVA was performed. The assumptions of normality, and homogeneity of
variance were also tested to ensure correct interpretation of the results of ANCOVA. All the
statistical analyses were performed using SPSS (IBM, Armonk, New York) and MATLAB
(Mathworks, Natick, MA).

32
“Is there any knowledge in the world which is so certain that no reasonable man could doubt it?”
Bertrand Russell
3 Results Patient demographic is presented in Table 1. The median MOCA score was found to be 24
(mean±standard deviation = 24.2±4.6). This score was between the suggested average scores for
normal controls and mild cognitive impairment (27.4±2.2 and 22.1±3.1 respectively) based on
MCOA normative data (http://www.mocatest.org/normative_data.asp).
3.1 ROI Comparison
The vein fraction was calculated as the number of vein voxels in an ROI divided by the volume
of the ROI. An ROI analysis was performed to look at the differences in vein fraction among
ROIs. The vein fraction in GM, NAWM and WMHs is shown in Figure 14.
Figure 14: Top: the tissue class ROIs (B) was used to mask the venogram (A). Bottom: Vein
fraction in different tissue ROIs.

33
The Shapiro-Wilk test revealed that the vein fraction (independent variable) was normally
distributed in GM (p=0.95) and NAWM (p=0.24). However, the distribution of WMH vein
fraction was not normal (p=0.02)1. The Levene’s F test showed that the variance in vein fraction
between ROIs was significantly different (p=007) hence violating the assumption of the
homogeneity of variance. Due to these violations caution should be exercised when performing
the one-way ANOVA to compare the mean vein fraction in different ROIs. It is known that when
the sample sizes are equal the one-way ANOVA is robust with respect to the violation of its
assumptions. Furthermore, robust tests of equality of means, including Welch’s test and Brown–
Forsythe test, were conducted which accommodate for deviations from the assumptions of
ANOVA. The ROI analysis showed that the vein fraction was significantly different between
tissue types (F=43.9, df=2, p<0.001; pBrown-Forsythe<0.001). The vein fraction in WMHs and GM
was significantly higher compared to NAWM (Tukey HSD test, p<0.001). No significant
difference was found between vein fraction in GM and WMHs (p=0.8).
3.2 Vein Fraction in WM
The vein fraction in the white matter was assessed using two different approaches: 1) vein
fraction in the entire WM and 2) vein fraction in the group template acquired NAWM. Note that
in the former case the vein fraction estimate is based on both WMH and NAWM forms of WM
whereas the latter is the vein fraction exclusively in NAWM (i.e. SVD “disease free”). The
Shapiro-Wilk test failed to reject the null hypothesis that the vein fraction was normally
distributed for both WM and template acquired NAWM (p=0.21 and p=0.64 respectively). No
gender difference (p=0.73 and p=0.76) and no association with age (p=0.22 and p=0.66) were
found for either of the vein fraction estimates. A regression analysis revealed a significant
positive correlation between vein fraction in the WM and WMHs lesion burden (r=0.55,
p=0.007, after adjusting for sex and age as covariates). To account for the possible effect of
WMHs on vein count, the vein fraction was measured in the group template acquired NAWM. A
significant positive correlation was found between NAWM vein fraction and WMHs measured at
1 The Kolmogorov-Smirnov test with Lilliefors Significance Correction showed that WMHs vein fraction was
normally distributed (p>0.05). The Shapiro-Wilk test is often more conservative than the Kolmogorov-Smirnov.

34
the level of lateral ventricle (LV) (r=0.47, p=0.025, after adjusting for sex and age as covariates).
These results are shown in Figure 15.
Figure 15: Vein fraction vs. WMHs at the level of LV (top) and vs. global WMHs (bottom). C
& D are provided as context in support of the use of WMHs at of the LV.
3.3 Vein Fraction Results Based on the Visual Rating Scale
The ARWMC scores of the subjects ranged from 1 to 3 (i.e. mild to severe WMHs) with no
subject having a score of 0 (i.e. absence of WMHs) (Table 2). The participants were separated in
groups based on their ARWMC score. A Chi square test was used to test the null hypothesis that
the ARWMC groups did not have significantly different gender proportions, which revealed no
gender difference (χ2=0.94, p=0.63). The age difference among the groups was not significant as
assessed by a one-way ANOVA (F=1.74, p=0.20). The WMHs lesion burden, CBF, and vein
fractions were normally distributed within the groups (Shapiro-Wilk test, p>0.1). The
homogeneity of variance within the groups was examined using the Levene’s F test, which

35
confirmed the equality of the variances for all dependent variables (p>0.6) except for WMHs
(p=0.004).
ARWMC Rating Scale
Score 1 Score 2 Score 3
N 6 12 7
Age (mean±std) 69.2±5.3 76.6±9.7 70.7±10.8
Female (%) 3/6 (50%) 6/12 (50%) 2/7 (29)
WMHs (cc) (mean±std) 1.78±1.27 17.30±9.89 35.50±21.19
Table 2: The distribution of age, gender and WMHs across ARWMC groups.
The analysis of covariates (ANCOVA) showed that a higher ARWMC score is associated with
significantly higher amount of WMHs (F=10.9, df=2, p=0.0006). The total GM CBF was found
to decrease with increasing ARWMC score, however this was not statistically significant
(p=0.52). The ARWMC score was a significant predictor of both WM vein fraction and vein
fraction in NAWM mask (F=4.02, p=0.03 and F=5.08, p=0.02 respectively). The group analysis
is shown in Figure 16.

36
Figure 16: Comparison of WMHs, GM CBF, WM vein fraction and vein fraction in NAWM
mask among ARWMC scores.
3.4 CBF Measurements
The average CBF was 51.4±15.4 mL/100g/min (mean±std) in GM. On average, the GM CBF
was found to be greater in women compared to men (58.8±13.9 vs 45.6±14.4 mL/100g/min) and
the difference was statistically significant (p=0.03). No correlation between GM CBF and age
was found after correcting for sex (p=0.7). Furthermore, GM CBF was not significantly
correlated with either WMHs or vein fractions (p=0.16 and p=0.44 respectively). The result of
the voxel-wise analysis for voxels with puncorrected<0.005 and a minimum cluster size of 10 voxels
is shown in Figure 17. A negative relationship was found between WM vein fraction and
perfusion to an area in proximity to left opercular cortex and insula with WMHs, age and sex
included as covariates. No voxels survived when correction for multiple comparisons was
performed using FMRIB’s threshold-free cluster enhancement algorithm.

37
Figure 17: Voxel-wise analysis results shows a region (11 voxels; shown in blue) with reduced
perfusion. The background grey-scale image is the MNI152 T1 template.

38
“The measure of greatness in a scientific idea is the extent to which it stimulates thought and opens up new lines of research.”
Paul Dirac
4 Discussion and Future Work The previous chapter demonstrated that susceptibility-weighted imaging (SWI) can be used
along side FLAIR and ASL perfusion neuroimaging MRI to study cerebral small vessel disease
white matter hyperintensities. Prominence of veins on SWI has been used previously as an
indication of a hemodynamic and/or metabolic condition of the brain. In this thesis, vein fraction
(number of veins in an ROI normalized to the volume of the ROI) was used to study the WM in
CSVD, where I found that the vein fraction was significantly higher in WMH regions compared
to NAWM, which suggests a shared anatomical correspondence between the lesions and the
venous vasculature. In addition, I found that the vein fraction throughout the WM and also in
areas not affected by the disease were both positively correlated with the CSVD lesion burden.
The vein fraction was also associated with reduced perfusion in left lateralized region in
proximity of insular cortex and operculum cortex. Parts of this work have been presented orally
at the Imaging Network Ontario Symposium (Toronto, ON, March 2014) and the International
Society of Magnetic Resonance in Medicine conference (Milan, Italy, May 2014).
4.1 Shared Anatomical Location
It is well known that accumulation of WMHs follows a somewhat consistent pattern: lesions tend
to occur around the ventricles either near the horns or along the lateral walls 54. More confluent
lesions are localized within the so-called “watershed” areas where the arterial supply is limited
and the brain is more susceptible to ischemic injury. This “preferential localization” has been
implicated in the pathophysiology of the WMHs.
The periventricular region where most of the WMHs tend to accumulate is drained by a rich
network of deep medullary veins. Previously, Gao and colleagues used proton density (PD) MRI
and T2-weighted MRI to investigate the deep medullary veins in focal WMHs and have
suggested that the overlap of lesions and veins implicate venous pathology (See Figure 18). The
current study showed quantitatively that there is a higher vein fraction within the lesions

39
compared to NAWM. While no causational relationship can be drawn by this, or previous
analyses, it is reasonable to postulate that venous vasculature can be involved in the underlying
pathology of CSVD. Such involvement could be a result of venous collagenases, which has been
proposed to cause dilation of the veins leading to venous insufficiency and consequently
resulting in vessel leakage and vasogenic oedema 16.
A higher vein fraction in WMH lesions alone could be driven predominantly by anatomical
coincidence rather than the ischemic nature of the lesions. Nevertheless, this shared anatomical
location between veins and WMHs is important for two reasons. First, the veins that are draining
the WMHs may reflect physiological changes that can be used to assess the lesion and the overall
health of the brain. Second, it provides a basis for investigating the role that venous pathology
may play in the aetiology of the CSVD.
Figure 18: Association between WMHs and veins. The middle diagram shows the overlay of the
WMHs and the vein schematically. thin arrows=vein; think arrows=WMHs (Adopted from Gao
et al. 2008 55).
4.2 Prominence of Veins Reflects Pathophysiological Changes in CSVD
As described in more detail previously, the main source of contrast in SWI is the variation of
tissue susceptibility. In SWI venography, the higher concentration of the paramagnetic
deoxyhemoglobin inside the veins increases the local magnetic field inhomogeneity and leads to
the hypointense appearance of the veins. The increased prominence of the deep medullary veins
is thought to reflect an increased deoxyhemoglobin concentration.

40
In this study, a significant positive correlation between WMHs volume (as a measure of CSVD
burden) and the prominence of the veins was found. In other words, subjects with more severe
disease burden were more likely to have prominent deep medullary veins on SWI. Previously, it
has been known that WMHs are associated with increased oxygen extraction fraction and
impaired perfusion in the WM 20,21, both of which reduce the oxygen saturation of the draining
veins and result in higher deoxyhemoglobin level. Therefore, it can be concluded that the
prominence of the vein metric is reflecting ischemic pathophysiological changes associated with
CSVD. It is important to note that prominence of the vein is not entirely driven by the veins in
the WMHs lesions. When the vein fraction in a template-acquired NAWM ROI was assessed, we
observed similar findings. This ROI limits the analysis to the regions that are lesion free across
the entire cohort. The prominence of vein metric in this ROI still explains the severity of CSVD.
In other words, problems associated with CSVD are not limited to the lesion and are manifested
in the NAWM as well.
It was somewhat surprising that the prominence of the vein did not show a significant association
with age in this cohort, which may have been influenced by the age range that was studied.
Future work could investigate SWI venous anatomy over the lifespan to test the theory that the
venous integrity decreases with age.
Despite increased oxygen extraction fraction and impaired perfusion (i.e. ischemia), another
mechanism that can contribute to the increased prominence of veins on SWI is venous
collagenosis. Venous collagenosis is the process of thickening of the wall of the veins due to
collagen deposition. The interaction between this type of venous pathology and hemodynamic
impairment is unclear. However it seems plausible that venous collagenosis can contribute to the
ischemia via venous stasis and slow and inadequate drainage of the deep white matter. As
mentioned previously, it has been suggested that venous collagenosis results in the dilation of the
veins 16 and would make them more visible on SWI. While the mechanism of this dilation is not
known entirely, it has been shown that venous collagenosis correlates positively with the severity
of WMHs 14. Hence the increased prominence of veins as a function of WMHs can be attributed,
at least in part, to venous collagenosis as well. All in all, individuals with more severe CSVD
have a more ischemic WM with arterial and venous problems. Prominence of vein can be used as
a metric that reflects important and relevant pathophysiological changes that are associated with
CSVD.

41
4.3 Perfusion Findings: Evidence and Implications
The perfusion results showed that the GM CBF was significantly higher in women compared to
men. This observation is in agreement with other perfusion studies using a variety of techniques
including ASL and SPECT 56–59. The reason for the CBF difference between men and women is
not completely understood however a number of theories have been proposed to explain this
difference. First, the lower level of haematocrit in women can decrease the oxygen carrying
capacity of the blood and can also reduce the blood viscosity, both of which necessitate a higher
CBF 59. Another explanation is that the CBF per 100 g of brain tissue is higher in female to
compensate their lower brain mass 56. Furthermore, other physiological differences such as
higher cardiac output compared to the body’s surface area, can result in a higher systemic and
cerebral blood flow 56.
The voxel-wise perfusion analysis showed that the left insular grey matter perfusion was
negatively correlated with the vein fraction in white matter. The insula (also known as the insular
cortex) is a brain structure involved in a number of important functions in consciousness,
emotion, motor control and autonomic regulations. An example of an autonomic nervous system
function is regulating and control of cardiovascular function. The insula is an important
communication hub in the brain since it is connected to frontal, parietal, and temporal cortex, and
limbic areas 60. The frontal operculum, lateral and posterior orbital cortex, the orbitofrontal
cortex, and the prefrontal cortex are also connected to the insula 60.
The preliminary finding of left insular hypoperfusion in this thesis may be related to
hemodynamic changes in CSVD. Injury to the left insula has been implicated with adverse
cardiac function. For example, Laowattana and colleagues have found association between left
insular stroke and worse cardiac outcome and lower cardiac wall motion 61. Importantly, it has
been observed that stroke patients with lesions affecting the right insula are more susceptible to
cardiac arrhythmias and have higher sympathetic activity leading to sudden death. On the other
hand, those with lesion involving the left insula more often have vasodepressor responses (i.e.
bradycardia and hypotension) 62. In general, failure in the autonomic function is associated with
impaired cerebral autoregulation and consequently reduced CBF. The involvement of insula in
CSVD is unclear, however, Caroli et al. have shown in 2007 that mild cognitive impairment
(MCI) patients with high WMHs have hypoperfusion in the left insula and superior temporal

42
gyrus compared to those with low amount of WMHs. The lower perfusion in the insular region
may also be related to previous findings by Rossi and colleagues who showed there was an
association between WMHs and the loss of insular tissue volume 63. It is also known that insula
is involved in processes related to language and working memory. The fact that the insula is
involved in autonomic regulation and cognitive function, both of which are affected in CSVD,
makes it an attractive target in relation to the assessment of CSVD. Thus insular perfusion, as an
intriguing imaging marker may contribute to a better understanding of CSVD.
Lastly, a note should be made regarding the criteria for identifying significant voxels in the
voxel-wise perfusion analysis. While correcting for multiple comparisons is a necessary step
aimed to reduce type I errors, imposing extremely conservative statistical thresholdings to
achieve this goal comes at a cost of increasing type II errors (i.e. failure to detect a true positive).
It has been suggested that using an intensity threshold of p<0.005 in combination with cluster
size threshold of 10 voxels result in a balance between type I and type II errors 64. Avoiding the
type II error (at the cost of increasing the chance of type I error) is reasonable in the context of
establishing novel relationships, such as the CBF findings presented in this thesis. Nevertheless,
findings should always be interpreted with caution and replication studies shall be conducted to
verify the robustness of the results.
4.4 From Structural to Physiological Imaging: A Search for New Imaging Markers of CSVD
Using the FLEX algorithm on FLAIR images, I imposed a conventional binary classification for
voxels in white matter: classifying them as hyperintense or not. The former corresponds to a
WMHs lesion while the latter is called “normal appearing” white matter (NAWM). Therefore the
assessment of WM in the context of CSVD lesions is dichotomous. One might argue that this
approach does not entirely reflect the pathophysiology of CSVD. For instance, while a
volumetric measure of WMHs can be an important metric in assessing the disease severity, it
provides little information about the so-called “healthy” NAWM. Since the development of
WMHs is a gradual process in aging, and because the WMHs lesions are thought to be
irreversible, the assessment of NAWM may provide a window for therapeutic intervention. The
concept that NAWM is also affected by CSVD is supported by a number of studies. MR imaging

43
using diffusion tensor MRI (DTI) has revealed higher mean diffusity and lower fractional
anisotropy in the NAWM of the patients with leukoaraiosis compared to age-matched controls 65.
More recently, Makedonov et al. used resting-state BOLD MRI and showed that the NAWM has
a greater cardiac pulsatility and physiological noise in a CSVD cohort compared to elderly
controls 66.
The notion that WMHs are primarily asymptomatic and are merely relegated to a radiological
finding has been pervasive in the literature, but this is being challenge by more recent work. It
can be said that WMHs as seen on T2/FLAIR images, however, lacks sensitivity to gradual
changes of the WM. To overcome this limitation, dynamic metrics that reflect the structure or
physiology of WM should be employed. The prominence of vein is one of such metric. The
assessment of veins not only highlights the anatomical significance of the venous vasculature,
but also provides information regarding the ischemic nature of CSVD, which are in agreement
with known CSVD pathologies. In this regard, it provides a novel approach to characterize the
effects of small vessel disease white matter hyperintensities in the brain. Furthermore, the
positive association between the WMHs and the prominence of vein in an NAWM ROI with
consistent anatomical location within the cohort provides evidence that the metric can
characterize WM that appears healthy, but is in fact affected to some degree in association with
the CSVD. In other words, the prominence of vein metric is an attempt to move beyond the
WMHs lesions.
4.5 Limitations and Future Work
A limitation of this work is the lack of age-matched controls. Since the population sample came
from the participants of a cerebrovascular reactivity study with the inclusion criterion of previous
WMHs, a comparison with age matched healthy controls was not possible. However, it should be
noted that despite the absence of age-matched control, the WMHs volume had a wide dynamic
range, making it conducive to a categorical sub-grouping, with approximately equal number of
participants in the low and high WMHs groups (i.e. ARWMC scores of 1 and 3 respectively).
Therefore, the participants with lower WMHs burden are in fact comparable to what would be
expected among a healthy age-matched population. Also this study was cross-sectional, hence it
does not allow to investigate causal relationship between observations.

44
Another aspect of this thesis that could be seen as a limitation was the focus on radiological
concepts and findings. While WMHs have other clinical manifestations, such as cognitive
dysfunction and gate problems, this thesis did not investigate these brain behaviours. As a result
the clinical utilities of the prominence of vein and other physiological measures such as
perfusion in clinical workup of CSVD patients are unclear. Nonetheless, the prominence of vein
remains a useful metric in better characterizing the CSVD and hence improves our current
understating of its pathophysiology.
Research on CSVD can greatly benefit from more direct assessment of tissue oxygenation. When
combined with perfusion imaging, brain oxygenation mapping can provide a better
understanding of the pathophysiology of CSVD as well as examining the prognosis. While SWI
provides detailed visualization of cerebral veins and allows evaluating venous oxygenation by
inference, the technique is essentially semi-quantitative (i.e. relative intensity units) and does not
provide purely quantitative information. Recently, quantitative susceptibility mapping (QSM)
has been introduced which uses MR phase images to produce quantitative susceptibility maps.
These susceptibility maps provide 3D venograms that are independent of vessel orientation 67.
Future developments in QSM are aiming to derive oxygen saturation maps based on the
susceptibility maps, which can then be used as a new source of contrast to assess different tissue
types including WMHs and NAWM. The local measurement of venous oxygen saturation
provides specific information about local oxygen delivery and tissue oxygen consumption. In
addition, MRI can be used to measure global venous oxygenation. Susceptibility-based oxymetry
(without the use of susceptibility maps) can reliably measure the venous oxygenation in large
veins such as the internal jugular vein 68. More recently, Lu and Ge have suggested the T2-
Relaxation-Under-Spin-Tagging (TRUST) MRI technique which is capable of measuring blood
oxygen saturation in the sagittal sinus 69. TRUST is in principle similar to ASL but instead of
tagging the blood in the arteries the venous blood is tagged. While this technique provides the
oxygen saturation in only the large terminal veins, such global assessments can complement
local measurements of oxygen saturation. A combination of oxygenation mapping techniques
can be useful in developing oxygenation agents 70, which may be of potential importance for the
treatment of CSVD in the future.

45
5 Conclusion This study used susceptibility-weighted imaging (SWI) and ASL perfusion imaging, in
combination with conventional structural imaging (i.e. FLAIR and T1-weighted), to advance our
cuurent understanding of CSVD in patients with WMHs. A shared anatomical location was
observed between WMHs and venous vasculature. Furthermore, the SWI prominence of veins
indicated the severity of CSVD which may be a consequence of venous hemodynamic
impairment and ischemia. The prominence of vein metric along with the shared anatomical
correspondence between veins and lesions highlights the potential importance of the venous
vasculature in both aetiology and prognosis of CSVD.

46
Bibliography
1. Wardlaw JM, Smith EE, Biessels GJ, et al. Neuroimaging standards for research into
small vessel disease and its contribution to ageing and neurodegeneration. Lancet Neurol.
2013;12(8):822-38. doi:10.1016/S1474-4422(13)70124-8.
2. Thompson CS, Hakim AM. Living Beyond Our Physiological Means Small Vessel
Disease of the Brain Is an Expression of a Systemic Failure in Arteriolar Function : A
Unifying Hypothesis. 2009:322-330. doi:10.1161/STROKEAHA.108.542266.
3. Debette S. The clinical importance of white matter hyperintensities on brain magnetic
resonance imaging : systematic review and. 2010:1-9. doi:10.1136/bmj.c3666.
4. Tarvonen-Schröder S, Röyttä M, Räihä I, Kurki T, Rajala T, Sourander L. Clinical
features of leuko-araiosis. J. Neurol. Neurosurg. Psychiatry 1996;60(4):431-6. Available
at:
http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1073899&tool=pmcentrez&re
ndertype=abstract.
5. Van Gijn J. Leukoaraiosis and vascular dementia. Neurology 1998;51(3 Suppl 3):S3-8.
Available at: http://www.ncbi.nlm.nih.gov/pubmed/23117721.
6. Grueter BE, Schulz UG. Age-related cerebral white matter disease (leukoaraiosis): a
review. Postgrad. Med. J. 2012;88(1036):79-87. doi:10.1136/postgradmedj-2011-130307.
7. Herrmann LL, Le Masurier M, Ebmeier KP. White matter hyperintensities in late life
depression: a systematic review. J. Neurol. Neurosurg. Psychiatry 2008;79(6):619-24.
doi:10.1136/jnnp.2007.124651.
8. Teodorczuk a, Firbank MJ, Pantoni L, et al. Relationship between baseline white-matter
changes and development of late-life depressive symptoms: 3-year results from the
LADIS study. Psychol. Med. 2010;40(4):603-10. doi:10.1017/S0033291709990857.
9. Starr JM, Leaper SA, Murray AD, et al. Brain white matter lesions detected by magnetic
resosnance imaging are associated with balance and gait speed. 2003:94-99.
10. Pantoni L. Leukoaraiosis: from an ancient term to an actual marker of poor prognosis.
Stroke. 2008;39(5):1401-3. doi:10.1161/STROKEAHA.107.505602.

47
11. Brown WR, Moody DM, Thore CR, Anstrom J a., Challa VR. Microvascular changes in
the white mater in dementia. J. Neurol. Sci. 2009;283(1-2):28-31.
doi:10.1016/j.jns.2009.02.328.
12. Pantoni L. Review Cerebral small vessel disease : from pathogenesis and clinical
characteristics to therapeutic challenges. 2010:689-701.
13. Marstrand JR, Garde E, Rostrup E, et al. Cerebral Perfusion and Cerebrovascular
Reactivity Are Reduced in White Matter Hyperintensities. Stroke 2002;33(4):972-976.
doi:10.1161/01.STR.0000012808.81667.4B.
14. Moody M, Brown W, Challa V, Anderson R. Periventricular Association Venous
Collagenosis : with Leukoaraiosis ’. Radiology 1995:469-476.
15. Brown WR, Moody DM, Challa VR, Thore CR, Anstrom JA. Venous collagenosis and
arteriolar tortuosity in leukoaraiosis. 2002;204:159-163.
16. Black S, Gao F, Bilbao J. Understanding white matter disease: imaging-pathological
correlations in vascular cognitive impairment. Stroke. 2009;40(3 Suppl):S48-52.
doi:10.1161/STROKEAHA.108.537704.
17. Kobari M, Meyer JS, Ichijo M. Leuko-araiosis, cerebral atrophy, and cerebral perfusion in
normal aging. Arch. Neurol. 1990;47(2):161-165. Available at:
http://www.scopus.com/inward/record.url?eid=2-s2.0-0025189994&partnerID=tZOtx3y1.
18. Marstrand JR, Garde E, Rostrup E, et al. Cerebral Perfusion and Cerebrovascular
Reactivity Are Reduced in White Matter Hyperintensities. Stroke 2002;33(4):972-976.
doi:10.1161/01.STR.0000012808.81667.4B.
19. Sullivan O. Reduced cerebral blood flow in white matter in ischaemic ... 2000.
20. O’Sullivan M, Lythgoe DJ, Pereira a C, et al. Patterns of cerebral blood flow reduction in
patients with ischemic leukoaraiosis. Neurology 2002;59(3):321-6. Available at:
http://www.ncbi.nlm.nih.gov/pubmed/12177363.
21. Meguro K, Hatazawa J, Yamaguchi T, et al. Cerebral circulation and oxygen metabolism
associated with subclinical periventricular hyperintensity as shown by magnetic resonance
imaging. Ann. Neurol. 1990;28(3):378-83. doi:10.1002/ana.410280313.
22. Ibayashi S, Irie K, Kitayama J, Nagao T, Kitazono T. Ischemic brain metabolism in
patients with chronic cerebrovascular disease: Increased oxygen extraction fraction and
cerebrospinal fluid lactate. J. Stroke Cerebrovasc. Dis. 2000;9(4):166-171.

48
23. Yamaji S, Ishii K, Sasaki M, et al. Changes in cerebral blood flow and oxygen metabolism
related to magnetic resonance imaging white matter hyperintensities in Alzheimer’s
disease. J. Nucl. Med. 1997;38(9):1471-1474.
24. Nezu T, Yokota C, Uehara T, et al. Preserved acetazolamide reactivity in lacunar patients
with severe white-matter lesions: 15O-labeled gas and H2O positron emission tomography
studies. J. Cereb. Blood Flow Metab. 2012;32(5):844-50. doi:10.1038/jcbfm.2011.190.
25. Herholz K, Heindel W, Rackl A, et al. Regional cerebral blood flow in patients with
leuko-araiosis and atherosclerotic carotid artery disease. Arch. Neurol. 1990;47(4):392-
396. Available at: http://www.scopus.com/inward/record.url?eid=2-s2.0-
0025349703&partnerID=tZOtx3y1.
26. Yamauchi H, Fukuyama H, Nagahama Y, et al. Brain arteriolosclerosis and hemodynamic
disturbance may induce leukoaraiosis. Neurology 1999;53(8):1833-1838. Available at:
http://www.scopus.com/inward/record.url?eid=2-s2.0-0033544409&partnerID=tZOtx3y1.
27. Derdeyn CP, Khosla A, Videen TO, et al. Severe hemodynamic impairment and border
zone-region infarction. Radiology 2001;220(1):195-201. Available at:
http://www.scopus.com/inward/record.url?eid=2-s2.0-0034977375&partnerID=tZOtx3y1.
28. O’Sullivan M, Jarosz JM, Martin RJ, Deasy N, Powell JF, Markus HS. MRI
hyperintensities of the temporal lobe CADASIL. 2001.
29. Reichenbach J, Venkatesan R, Yablonskiy D, Thompson M, Lai S, Haacke E. Theory and
application of static field inhomogeneity effects in gradient-echo imaging. J. Magn.
Reson. Imaging 1997:226-279.
30. Reichenbach JR, Venkatesan R, Schillinger DJ, Kido DK, Haacke EM. Small vessels in
the human brain: MR venography with deoxyhemoglobin as an intrinsic contrast agent.
Radiology 1997;204(1):272-277. Available at:
http://www.scopus.com/inward/record.url?eid=2-s2.0-0030981629&partnerID=tZOtx3y1.
31. Haacke EM, Reichenbach JR. Susceptibility Weighted Imaging in MRI: Basic Concepts
and Clinical Applications.; 2011. doi:10.1002/9780470905203.
32. Li D, Wang Y, Waight DJ. Blood oxygen saturation assessment in vivo using T2*
estimation. Magn. Reson. Med. 1998;39(5):685-90. Available at:
http://www.ncbi.nlm.nih.gov/pubmed/9581597.

49
33. Spees WM, Yablonskiy DA, Oswood MC, Ackerman JJH. Water proton MR properties of
human blood at 1.5 Tesla: Magnetic susceptibility, T1, T2*, T2, and non-Lorentzian
signal behavior. Magn. Reson. Med. 2001;45(4):533-542.
34. Reichenbach JR, Barth M, Haacke EM, Klarhöfer M, Kaiser WA. High-Resolution MR
Venography at 3.0 Tesla. J. Comput. Assist. Tomogr. 2000;24(6):949-957.
35. Koopmans PJ, Manniesing R, Niessen WJ, Viergever MA, Barth M. MR venography of
the human brain using susceptibility weighted imaging at very high field strength.
2008:149-158. doi:10.1007/s10334-007-0101-3.
36. Haacke EM, Xu Y, Cheng YN, Reichenbach R. Susceptibility Weighted Imaging ( SWI ).
2004;618:612-618. doi:10.1002/mrm.20198.
37. Bernstein A, Kevin FK, Zhou XJ. Handbook of MRI Pulse Sequences.; 2004:702-801.
38. Reichenbach J, Venkatesan R, Schillinger D, Kido D, Haacke E. Smallvesselsinthehuman
brain: MR venography with deoxyhemoglobin as an intrinsic contrast agent. Radiology
1997;(204):272-277.
39. Tong KA, Ashwal S, Obenaus A, Nickerson JP, Kido D, Haacke EM. Susceptibility-
Weighted MR Imaging : A Review of Clinical Applications in Children. 2008:9-17.
doi:10.3174/ajnr.A0786.
40. Tallantyre EC, Dixon JE, Donaldson I, et al. Ultra-high-field imaging distinguishes MS
lesions from asymptomatic white matter lesions. Neurology 2011;76(6):534-9.
doi:10.1212/WNL.0b013e31820b7630.
41. Quinn MP, Kremenchutzky M, Menon RS. Venocentric Lesions: An MRI Marker of MS?
Front. Neurol. 2013;4(July):98. doi:10.3389/fneur.2013.00098.
42. Ge Y, Zohrabian VM, Osa E, et al. Diminished Visibility of Cerebral Venous Vasculature
in Multiple Sclerosis by Susceptibility- Weighted Imaging at 3 . 0 Tesla. 2009;1194:1190-
1194. doi:10.1002/jmri.21758.
43. Zivadinov R, Poloni GU, Marr K, et al. Decreased brain venous vasculature visibility on
susceptibility-weighted imaging venography in patients with multiple sclerosis is related
to chronic cerebrospinal venous insufficiency. 2011.
44. Beggs CB, Shepherd SJ, Dwyer MG, et al. Sensitivity and specificity of SWI venography
for detection of cerebral venous alterations in multiple sclerosis. 2012:793-801.
doi:10.1179/1743132812Y.0000000048.

50
45. Mittal S, Wu Z, Neelavalli J, Haacke E. Susceptibility-weighted imaging: technical
aspects and clinical applications, part 2. AJNR. Am. J. Neuroradiol. 2009;30(2):232-52.
46. Horie N, Morikawa M, Nozaki A, Hayashi K, Suyama K, Nagata I. “Brush Sign” on
susceptibility-weighted MR imaging indicates the severity of moyamoya disease. Am. J.
Neuroradiol. 2011:1697-1702.
47. Okudera T, Huang Y, Fukusumi A, Nakamura Y, Hatazawa J, Uemura K. Micro-
angiographical studies of the medullary venous system of the cerebral hemisphere.
Neuropathology 1999;19(1):93-111.
48. Sedlacik J, Kutschbach C, Rauscher A, Deistung A, Reichenbach JR. Investigation of the
influence of carbon dioxide concentrations on cerebral physiology by susceptibility-
weighted magnetic resonance imaging ( SWI ). Neuroimage 2008;43:36-43.
doi:10.1016/j.neuroimage.2008.07.008.
49. Frangi AF, Niessen WJ, Vincken KL, Viergever MA. Multiscale vessel enhancement
filtering 1 Introduction 2 Method. 1998.
50. MP S, RH B, R Z, R B. Correction for intracranial volume in analysis of whole brain
atrophy in multiple sclerosis: the proportion vs. residual method. Neuroimage
2004;(22):1732-1743.
51. Jenkinson M, Smith S. A global optimisation method for robust affine registration of brain
images. Med. Image Anal. 2001;5(2):143-56. Available at:
http://www.ncbi.nlm.nih.gov/pubmed/11516708.
52. Jenkinson M, Bannister PR, Brady JM, Smith SM. Improved optimisation for the robust
and accurate linear registration and motion correction of brain images. Neuroimage
2002;17(2):825-841.
53. Koopmans PJ, Manniesing R, Niessen WJ, Viergever MA, Barth M. MR venography of
the human brain using susceptibility weighted imaging at very high field strength.
MAGMA 2008;21(1-2):149-58. doi:10.1007/s10334-007-0101-3.
54. Holland CM, Smith EE, Csapo I, et al. Spatial distribution of white-matter hyperintensities
in Alzheimer disease, cerebral amyloid angiopathy, and healthy aging. Stroke.
2008;39(4):1127-33. doi:10.1161/STROKEAHA.107.497438.
55. Gao F, Gaal S van, Levy-Cooperman N, et al. Does variable progression of incidental
white matter hyperintensities in Alzheimer’s disease relate to venous insufficiency?
Alzheimer’s Dement. 2008;4(4):T368–T369.

51
56. Rodriguez G, Warkentin S, Risberg J, Rosadini G. Sex Differences in Regional Cerebral
Blood Flow. J. Cereb. Blood Flow Metab. 1988;8(6):783-9.
57. Gur RE, Gur RC. Gender differences in regional cerebral blood flow. Schizophr. Bull.
1990;16(2):247-54. Available at: http://www.ncbi.nlm.nih.gov/pubmed/8896772.
58. Parkes LM, Rashid W, Chard DT, Tofts PS. Normal cerebral perfusion measurements
using arterial spin labeling: reproducibility, stability, and age and gender effects. Magn.
Reson. Med. 2004;51(4):736-43. doi:10.1002/mrm.20023.
59. Liu Y, Zhu X, Feinberg D, et al. Arterial spin labeling MRI study of age and gender
effects on brain perfusion hemodynamics. Magn. Reson. Med. 2012;68(3):912-22.
doi:10.1002/mrm.23286.
60. Caroli A, Testa C, Geroldi C, et al. Brain perfusion correlates of medial temporal lobe
atrophy and white matter hyperintensities in mild cognitive impairment. J. Neurol.
2007;254(8):1000-8. doi:10.1007/s00415-006-0498-z.
61. Laowattana S, Zeger SL, Lima JAC, Goodman SN, Wittstein IS, Oppenheimer SM. Left
insular stroke is associated with adverse cardiac outcome. Neurology 2006;66(4):477-83;
discussion 463. doi:10.1212/01.wnl.0000202684.29640.60.
62. Welch KMA, Caplan LR, Reis DJ, Siesjö BK, Weir B. Primer on Cerebrovascular
Diseases.; 1997.
63. Rossi R, Boccardi M, Sabattoli F, et al. Topographic correspondence between white
matter hyperintensities and brain atrophy. J. Neurol. 2006;253(7):919-27.
doi:10.1007/s00415-006-0133-z.
64. Lieberman MD, Cunningham W a. Type I and Type II error concerns in fMRI research:
re-balancing the scale. Soc. Cogn. Affect. Neurosci. 2009;4(4):423-8.
doi:10.1093/scan/nsp052.
65. O’Sullivan M, Summers PE, Jones DK, Jarosz JM, Williams SCR, Markus HS. Normal-
appearing white matter in ischemic leukoaraiosis: A diffusion tensor MRI study.
Neurology 2001;57(12):2307-2310. Available at:
http://www.scopus.com/inward/record.url?eid=2-s2.0-0035956516&partnerID=tZOtx3y1.
66. Makedonov I, Black SE, Macintosh BJ. BOLD fMRI in the white matter as a marker of
aging and small vessel disease. PLoS One 2013;8(7):e67652.
doi:10.1371/journal.pone.0067652.

52
67. Haacke E, Tang J, Neelavalli J, Cheng Y. Susceptibility Mapping as a Means to Visualize
Veins and Quantify Oxygen Saturation. J. Magn. Reson. Imaging 2011;32(3):663-676.
doi:10.1002/jmri.22276.Susceptibility.
68. Fernández-Seara MA, Techawiboonwong A, Detre JA, Wehrli FW. MR susceptometry for
measuring global brain oxygen extraction. Magn. Reson. Med. 2006;55(5):967-73.
doi:10.1002/mrm.20892.
69. Lu H, Ge Y. Quantitative evaluation of oxygenation in venous vessels using T2-
Relaxation-Under-Spin-Tagging MRI. Magn. Reson. Med. 2008;60(2):357-63.
doi:10.1002/mrm.21627.
70. Christen T, Bolar DS, Zaharchuk G. Imaging brain oxygenation with MRI using blood
oxygenation approaches: methods, validation, and clinical applications. AJNR. Am. J.
Neuroradiol. 2013;34(6):1113-23. doi:10.3174/ajnr.A3070.
Related Documents