ORIGINAL PAPER White Matter Integrity Following Traumatic Brain Injury: The Association with Severity of Injury and Cognitive Functioning Gershon Spitz • Jerome J. Maller • Richard O’Sullivan • Jennie L. Ponsford Received: 16 November 2012 / Accepted: 19 March 2013 Ó Springer Science+Business Media New York 2013 Abstract Traumatic brain injury (TBI) frequently results in impairments of memory, speed of information process- ing, and executive functions that may persist over many years. Diffuse axonal injury is one of the key pathologies following TBI, causing cognitive impairments due to the disruption of cortical white matter pathways. The current study examined the association between injury severity, cognition, and fractional anisotropy (FA) following TBI. Two diffusion tensor imaging techniques—region- of-interest tractography and tract-based spatial statistics— were used to assess the FA of white matter tracts. This study examined the comparability of these two approaches as they relate to injury severity and cognitive performance. Sixty-eight participants with mild-to-severe TBI, and 25 healthy controls, underwent diffusion tensor imaging analysis. A subsample of 36 individuals with TBI also completed cognitive assessment. Results showed reduction in FA values for those with moderate and severe TBI, compared to controls and individuals with mild TBI. Although FA tended to be lower for individuals with mild TBI no significant differences were found compared to controls. Information processing speed and executive abilities were most strongly associated with the FA of white matter tracts. The results highlight similarities and differences between region-of-interest tractography and tract-based spatial statistics approaches, and suggest that they may be used together to explore pathology following TBI. Keywords Cognition Á MRI Á DTI Á Traumatic brain injury Introduction Traumatic brain injury (TBI) results in long-lasting chan- ges to individuals’ independence, work capacity, and social functioning (Ponsford et al. 1995a, b). The most common impairments are those of memory, speed of information processing, and executive functions. Although cognitive impairments dissipate over the initial months in the majority of individuals with mild injuries, those with more severe injuries may display difficulties for years following injury (Dikmen et al. 1995; Draper and Ponsford 2008). Traumatic axonal injury (TAI) is one of the key patholo- gies following TBI—occurring as a result of acceleration, deceleration, and rotational forces—causing cognitive deficits due to the disruption of cortical and subcortical white matter pathways (Buki and Povlishock 2006; Gen- narelli et al. 1998; Povlishock and Christman 1994). The detection of TAI can be investigated using con- ventional MRI scans, in the form of haemorrhagic and non- G. Spitz (&) Á J. L. Ponsford School of Psychology and Psychiatry, Monash University, Clayton, Melbourne, VIC 3800, Australia e-mail: [email protected] G. Spitz Á J. L. Ponsford Monash-Epworth Rehabilitation Research Centre, Epworth Hospital, Melbourne, VIC, Australia J. J. Maller Central Clinical School, Monash University, Melbourne, VIC, Australia J. J. Maller Monash Alfred Psychiatry Research Centre, Alfred Hospital, Melbourne, VIC, Australia R. O’Sullivan Healthcare Imaging Services, Epworth Hospital, Melbourne, VIC, Australia 123 Brain Topogr DOI 10.1007/s10548-013-0283-0

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
ORIGINAL PAPER
White Matter Integrity Following Traumatic Brain Injury:The Association with Severity of Injury and Cognitive Functioning
Gershon Spitz • Jerome J. Maller •
Richard O’Sullivan • Jennie L. Ponsford
Received: 16 November 2012 / Accepted: 19 March 2013
� Springer Science+Business Media New York 2013
Abstract Traumatic brain injury (TBI) frequently results
in impairments of memory, speed of information process-
ing, and executive functions that may persist over many
years. Diffuse axonal injury is one of the key pathologies
following TBI, causing cognitive impairments due to the
disruption of cortical white matter pathways. The current
study examined the association between injury severity,
cognition, and fractional anisotropy (FA) following
TBI. Two diffusion tensor imaging techniques—region-
of-interest tractography and tract-based spatial statistics—
were used to assess the FA of white matter tracts. This
study examined the comparability of these two approaches
as they relate to injury severity and cognitive performance.
Sixty-eight participants with mild-to-severe TBI, and 25
healthy controls, underwent diffusion tensor imaging
analysis. A subsample of 36 individuals with TBI also
completed cognitive assessment. Results showed reduction
in FA values for those with moderate and severe TBI,
compared to controls and individuals with mild TBI.
Although FA tended to be lower for individuals with mild
TBI no significant differences were found compared to
controls. Information processing speed and executive
abilities were most strongly associated with the FA of
white matter tracts. The results highlight similarities and
differences between region-of-interest tractography and
tract-based spatial statistics approaches, and suggest that
they may be used together to explore pathology following
TBI.
Keywords Cognition � MRI � DTI � Traumatic brain
injury
Introduction
Traumatic brain injury (TBI) results in long-lasting chan-
ges to individuals’ independence, work capacity, and social
functioning (Ponsford et al. 1995a, b). The most common
impairments are those of memory, speed of information
processing, and executive functions. Although cognitive
impairments dissipate over the initial months in the
majority of individuals with mild injuries, those with more
severe injuries may display difficulties for years following
injury (Dikmen et al. 1995; Draper and Ponsford 2008).
Traumatic axonal injury (TAI) is one of the key patholo-
gies following TBI—occurring as a result of acceleration,
deceleration, and rotational forces—causing cognitive
deficits due to the disruption of cortical and subcortical
white matter pathways (Buki and Povlishock 2006; Gen-
narelli et al. 1998; Povlishock and Christman 1994).
The detection of TAI can be investigated using con-
ventional MRI scans, in the form of haemorrhagic and non-
G. Spitz (&) � J. L. Ponsford
School of Psychology and Psychiatry, Monash University,
Clayton, Melbourne, VIC 3800, Australia
e-mail: [email protected]
G. Spitz � J. L. Ponsford
Monash-Epworth Rehabilitation Research Centre,
Epworth Hospital, Melbourne, VIC, Australia
J. J. Maller
Central Clinical School, Monash University, Melbourne,
VIC, Australia
J. J. Maller
Monash Alfred Psychiatry Research Centre, Alfred Hospital,
Melbourne, VIC, Australia
R. O’Sullivan
Healthcare Imaging Services, Epworth Hospital,
Melbourne, VIC, Australia
123
Brain Topogr
DOI 10.1007/s10548-013-0283-0
haemorrhagic lesions (Scheid et al. 2003). However, con-
ventional scans tend to underestimate the extent of damage
(Arfanakis et al. 2002; Huisman et al. 2003; Rugg-Gunn
et al. 2001; Shenton et al. 2012; Toth et al. 2013). DTI is a
technique that is inherently well-suited for investigating
damage to white matter by quantifying the diffusion of
water molecules, providing a more accurate representation
of white matter disruption (Basser 1995; Basser et al.
1994). The directionality of water is used to infer the
integrity of white matter tracts; that is, diffusion should be
greater along the primary orientation of the tract, remaining
relatively restricted perpendicular to the fibre. Whilst DTI
enables the extraction of several meaningful indices of
fibre integrity, fractional anisotropy (FA) is the most
widely utilised for demonstrating the degree of direction-
ality of water diffusion.
Using DTI, widespread disruption of white matter has
been found following TBI. Even following mild TBI, indi-
viduals display white matter disruption both acutely and as
long as 7 years post-injury (Lipton et al. 2008; Lo et al. 2009;
Mayer et al. 2010; Miles et al. 2008; Niogi et al. 2008a). Not
surprisingly, significantly greater white matter disruption is
apparent in those with moderate and severe injuries (Benson
et al. 2007; Bigler et al. 2010; Kennedy et al. 2009; Kraus
et al. 2007; Kumar et al. 2009; Nakayama et al. 2006;
Newcombe et al. 2007; Salmond et al. 2006; Sidaros et al.
2008; Xu et al. 2007). Interestingly, whilst Kumar et al.
(2009) found a decrease in FA in the corpus callosum
between 9 days and 6 months post-injury, Sidaros et al.
(2008) reported increases in FA in several white matter tracts
between 8 weeks and 12 months post-injury. These findings
suggest that neural disruption may occur initially, followed
by axonal reorganisation or even regenerative processes at
later stages post-injury that may reflect change in function
following injury (Levin 2003).
Indeed, the integrity of white matter has been shown to
relate to cognitive processes following TBI (Bigler et al.
2010; Kraus, et al. 2007; Kumar, et al. 2009; Levin et al.
2010; Lo et al. 2009; Little et al. 2010; Niogi et al. 2008b;
Salmond, et al. 2006; Sugiyama et al. 2009). These studies
demonstrate that FA in several of the projection, com-
missural, and association white matter tracts is associated
with memory, whilst Niogi et al. (2008a, b) specifically
implicated the uncinate fasciculus. In addition, Lo et al.
(2009) found that reduced FA in several regions, particu-
larly the dorsolateral prefrontal cortex, was found to predict
executive functioning. In another study, Little et al. (2010)
found that FA in the thalamocortical projection fibres may
play a role in modulating executive ability, as well as
attention. The corona radiata has also been implicated in
attention (Kraus et al. 2007; Niogi et al. 2008b).
Techniques used to examine DTI largely fall under
region-of-interest (ROI) analyses, in which specific brain
regions are chosen a priori based on previous literature, and
voxel-based morphometry (VBM) approaches, which often
assess changes over the entire brain. ROI analysis provides
the opportunity for fine-grained analysis of tracts—both
quantitatively and qualitatively—that may be specifically
implicated in pathology and subsequent outcome. How-
ever, relying solely on ROI techniques poses the risk of
missing abnormal tracts, especially considering the heter-
ogeneous nature of TBI. Although VBM approaches offer
analysis of the entire brain, issues have been noted
regarding image alignment and the variable effect of spatial
smoothing (Ashburner and Friston 2000; Bookstein 2001;
Davatzikos 2004; Jones et al. 2002, 2005; Park et al. 2003).
Tract-based spatial statistics (TBSS) is a recently devel-
oped voxel-based technique that attempts to circumvent
these issues through the development of a white matter
skeleton, representing tracts common to all individuals in a
given study, which is applied to each individual’s image to
correct for residual misalignments (Smith et al. 2006).
TBSS has been used widely and utilised to demonstrate, for
example, that injury severity and cognitive functioning was
related to the integrity of white matter (Kinnunen et al.
2011). However, it is not known whether TBSS provides
results which are comparable with ROI approaches.
The current study examined whether white matter
changes following TBI were associated with injury sever-
ity, defined using days of post-traumatic amnesia (PTA). In
addition, the relationship between the integrity of white
matter and cognitive functions, including memory, infor-
mation processing speed, and executive functions was
investigated. Lastly, this is the first study to examine the
comparability of TBSS—providing an analysis of white
matter voxels over the entire brain—and ROI tractography
as they relate to the assessment of injury severity and
cognition following TBI.
Materials and Methods
Participants
Seventy-eight participants with mild to severe TBI were
recruited for the current study. Individuals with TBI were
excluded if they had previous history of TBI or other neuro-
logical disorder. Two TBI participants were excluded due to
severe brain pathology to avoid problems with image align-
ment. One TBI participant was excluded due to a large sub-
dural hematoma causing brain displacement to the left,
whereas the second participant was excluded due to wide-
spread hydrocephalus. In addition, eight individuals with TBI
were excluded due to large focal lesions, including four
individuals with large right frontal lobe contusions, one with
large left frontal contusion, two with bilateral frontal
Brain Topogr
123
contusions, and the last with an extensive fronto-temporal-
parietal contusion. The final TBI sample comprised 68 TBI
participants. Moreover, MRI scanning for the TBI group was
conducted on average 18.0 months post-injury (SD = 14.01,
range = 2.30–52.67). Twenty-five healthy controls—recrui-
ted by disseminating study flyers—with no prior neurological
or psychological disorders, were also included in the study.
Demographic information for TBI and control participants is
presented in Table 1. The overall TBI group was found to be
less educated and older, with a large proportion of males,
compared to controls. Therefore, subsequent comparisons
between TBI control and TBI participants controlled for,
gender, age, and education. A subsample of 36 TBI partici-
pants also completed cognitive tests, and did not differ from
the TBI participants for which cognitive assessment was not
present in terms of age, education, PTA, or gender. For this
subsample cognitive assessments and MRI scans were con-
ducted on average 4.6 (SD = 10.87, range = 0–55) days
apart.
Neuropsychological Assessment
Participants completed a number of neuropsychological
tests that collectively assessed memory, information pro-
cessing speed and executive functions, and which have
been shown to be sensitive to cognitive impairments fol-
lowing TBI (Draper and Ponsford 2008).
BIRT Memory and Information Processing Battery-List
Learning Subtest
The BIRT list learning test (Coughhlan et al. 2007)
assesses verbal recall and recognition. Participants recalled
a list of words over five trials. Total correctly recalled
words over the five learning trials were used as a measure
of ‘Total Recall’.
The Doors Test from the Doors and People Test
The doors test (Baddeley et al. 1994) is designed to assess
visual memory. This test required participants to recognise a
target door they have previously seen among three other
distractor doors not seen before. There were two trials, of 12
target doors, with the second trial using more similar dis-
tractors. The score for each trial ranges from 0 to 12 with an
overall score for the test ranging from 0 to 24. The two trials
were aggregated to form a measure of ‘Visual Memory’.
The Hayling Sentence Completion Test from the Hayling
and Brixton Tests
The Hayling sentence completion test (Burgess and Shallice
1997) assesses participants’ speed of initiation and response
inhibition abilities. This test comprises two sections, each
comprising 15 sentences with the last word missing. In the
first section (Hayling A) participants were required to finish
the sentence with a word that logically completed the sen-
tence as quickly as possible. In the second section (Hayling
B) participants were asked to complete the sentences with an
unrelated word. The overall scaled score—which incorpo-
rates the total time taken in parts A and B of the test, as well
as the number of errors—was used in the current study.
Controlled Oral Word Association Tests
The COWAT (Benton et al. 1994) is a measure of verbal
fluency and idea generation. Participants were required to
generate as many words as they could, beginning with a
specific letter, within a time span of one minute. The total
number of words generated was recorded for the letters C,
F and L.
Trail Making Test—Parts A and B
The TMT (Reitan and Wolfson 1988) measures processing
speed, attention, and mental flexibility, requiring partici-
pants to join numbers in sequence (Trails A) and to switch
between numbers and letters in sequence (Trails B) as
quickly as possible. In addition to the raw times for Trails
A and Trails B, a third variable was created by subtracting
Trails A time from Trails B, to quantify the executive
component of the TMT (Trails B–Trails A).
Digit Span Subtest of the Wechsler Memory Scale—Third
and Fourth Editions
The forwards and backwards digit span (Wechsler 1997,
2008) was used to assess participants’ immediate attention
span and working memory capacity. The number of correct
trials was recorded for the forward and backward
conditions.
Symbol Digit Modalities Test—Oral Version (SDMT)
The SDMT (Smith 1973) assesses processing speed. Par-
ticipants are provided with 90 s to verbalise to the exper-
imenter the correct number that belongs under a specific
symbol, based on the way they are paired in an index at the
top of the page. Total number of correct entries was used in
the current study.
Neuroimaging Acquisition
Neuroimaging was performed on a Siemens Magnetom
Verio 3 Tesla MRI scanner (Siemens Medical Imaging,
Erlangen, Germany). After a scout scan, an anterior
Brain Topogr
123
commissure posterior commissure (AC-PC) aligned axial
fluid attenuated inversion recovery (FLAIR) sequence was
acquired (repetition time = 8,500, echo time = 81, slice
thickness = 3.0 mm, field of view = 240 mm, matrix =
192 9 256, in-plane = 0.94 9 0.94 mm), followed by a
DTI sequence (TR = 5,500, TE = 110, 20 diffusion
encoding directions, number of excitations = 2, slice
thickness = 4.0 mm, field of view = 240 mm, matrix =
122 9 122, in-plane = 1.97 9 1.97 mm, b value = 1,000
s/mm2, one acquisition for each run with b = 0 s/mm2). In
addition, a 3D T1-weighted sequence was acquired in the
sagittal orientation [inversion time = 1,100 ms, repetition
Table 1 Descriptive statistics for and individuals with TBI, categorised by injury severity, and controls
Total TBI sample
(n = 68)
Mild TBI
(n = 10)
Moderate TBI
(n = 14)
Severe TBI
(n = 44)
TBI cognitive subsample
(n = 36)
Control
(n = 25)
N (%) N (%) N (%) N (%) N (%) N (%)
Gender (male) 56 (81.2) 7 (70) 12 (85.7) 37 (84.1) 29 (80.5) 11 (44)
Cause of injury
Car accident 35 (51.5) 4 (28.6) 4 (28.6) 27 (61.4) 17 (47.2)
Motorcycle 12 (17.6) 1 (10) 2 (14.3) 9 (20.5) 8 (22.2)
Pedestrian 6 (8.8) 2 (20.0) 2 (14.3) 2 (4.5) 2 (5.6)
Bicycle 6 (8.8) 1 (10) 4 (28.6) 1 (12.3) 5 (13.9)
Fall 6 (8.8) 1 (10) 1 (7.1) 4 (9.1) 4 (11.1)
Other 3 (4.5) 1 (10) 1 (7.1) 2 (2.3) 0 (0)
PTA categories
Mild (0–1 day) 10 (14.7) 4 (11.1)
Moderate
([1 to B7 days)
14 (20.6) 8 (22.2)
Severe ([7 days) 44 (64.7) 24 (66.7)
Worst GCS categories
Mild (13–15) 20 (31.7) 9 (27.3)
Moderate (9–12) 14 (22.2) 8 (24.2)
Severe (3–8) 29 (46.0) 16 (48.5)
Abnormal CT 57 (83.8) 10 (100) 8 (57.1) 39 (88.6) 29 (80.6)
Scan
Contusion 27 (39.7) 6 (60) 1 (7.1) 20 (45.5) 13 (36.1)
DAI 11 (16.2) 0 (0) 1 (7.1) 10 (22.7) 8 (22.2)
SAH 23 (33.8) 4 (40) 2 (14.3) 17 (38.6) 10 (27.8)
SDH 14 (20.6) 2 (20.0) 3 (21.4) 9 (20.5) 5 (13.9)
EDH 5 (7.4) 2 (20.0) 2 (14.3) 1 (2.3) 3 (8.3)
ICH 14 (20.6) 3 (30.0) 2 (14.3) 9 (20.5) 8 (22.2)
IVH 0 (0) 0 (0) 0 (0) 9 (20.5) 1 (2.8)
Mdn, M (SD)
range
Mdn, M (SD)
range
Mdn, M (SD)
range
Mdn, M (SD)
range
Mdn, M (SD)
range
Mdn, M (SD)
range
Age 35.41, 38.61 (14.64)
17–78
40.12, 39.63 (14.52)
18–62
33.55, 37.69 (14.06)
23–65
35.07, 38.67 (15.15)
17–78
41.76, 49.92 (13.36)
17–69
25.95, 30.26 (12.48)
18–69
Education 12.00, 12.36 (2.82)
6–20
12.00, 12.40 (2.68)
10–18
12.00, 12.69 (2.70)
8–18
12.00, 12.25 (2.94)
6–20
12.00, 12.94 (3.16)
6–20
15,00, 14.68 (1.51)
12–17
PTA (days) 12.00, 17.56 (19.29)
.1–105
10.50, 15.07
(15.45)
.1–82
Worst GCS 9.00, 8.76
3–15
10.00, 8.58
3–15
PTA post traumatic amnesia, GCS glasgow coma score, DAI diffuse axonal injury, SAH subarachnoid haemorrhage, SDH subdural haemorrhage, EDH
epidural haemorrhage, ICH intracerebral haemorrhage, IVH intraventricular haemorrhage
Brain Topogr
123
time = 1,930 ms echo time = 2.48 ms, resolution = 256
9 256 9 160, flip angle = 12�, field of view = 256 mm,
slice thickness = 1.00 mm (160 slices)].
Data Analysis
Tract-Based Spatial Statistics
The FMRIB Software Library (Smith et al. 2004) was used to
perform TBSS. Analyses were undertaken using the steps
outlined by Smith et al. (2006). Using both linear and non-linear
alignment, participants’ FA images were registered into stan-
dard space using the FMRIB58 FA template. The aligned
images were then averaged to reveal the white matter tracts
common to all participants; based on this image an FA skeleton
was created representing the centre of all white matter tracts. An
FA value of .2 was used as a threshold for the FA skeleton to
exclude tracts with high inter-individual variability as well as
those containing a high level of partial volume. Each partici-
pant’s aligned FA image was projected onto the FA skeleton to
correct for residual misalignments by calculating the difference
between the skeletonised tracts and the white matter tract
centres in each individual image. Voxelwise statistics were then
undertaken using the general linear model to compare differ-
ences in white matter FA between controls and TBI participants
and to regress the performance of each cognitive test on the FA
values of white matter tracts. The ‘randomise’ tool was used to
conduct significance testing, applying a threshold-free cluster
enhancement (Smith and Nichols, 2009) with 5,000 permuta-
tions, before a threshold of p\ .05 was applied. Comparisons
between TBI and control participants were controlled for age,
education, and gender, whereas analyses correlating FA values
with neuropsychological performance in the TBI group
covaried for gender, age, years of education, and time post injury.
Region-of-Interest Tractography
Diffusion images were reconstructed and directionally
encoded colour FA maps calculated using DTI studio (Jiang
et al. 2006). Eight ROIs were manually chosen a priori based
on previous studies: the corpus callosum (CC), left and right
superior longitudinal fasciculus (SLF), inferior longitudinal
fasciculus (ILF), posterior limb of the internal capsule
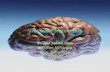
(PLIC), and the cingulate bundle. Representation of these
tracts is presented in Fig. 1. As shown in Fig. 2, ellipses
were placed on seed location in order to track each ROI
individually. Depending on the specific tract, ellipses were
placed when viewing the directionally encoded anisotropy
maps from sagittal, axial, or coronal orientations. As
explained by Mori and van Zijl (2002) and Mori et al.
(2005), tract reconstruction was performed using fiber
assignment by continuous tracking (FACT) method. Tracts
were linearly propagated based on the orientation of the
largest principal axis. Line propagation was discontinued
based on the standard criteria: that is, using the standard
anisotropy threshold of FA [.2 and an angle of change[75�between pixels. Lastly, the white matter atlas provided by
Mori et al. (2005) was used to assess the accuracy of tracked
ROIs. Average FA values for each of the a priori chosen
tracts were derived for each participant. Independent-sam-
ples t tests were undertaken to compare average FA of each
tract between control and TBI participants controlling for
age, education, and gender. To control for Type I error rate,
a Bonferroni correction was applied to the t tests performed
for each tract, such that the Bonferroni correction value was
now .008. For TBI participants only, Pearson correlations
were conducted, individually for each tract, to examine the
relationship between tract integrity and neuropsychological
performance. Correlation analyses controlled for gender,
age, level of education, and time post injury.
Results
Fractional Anisotropy is Associated with Injury
Severity
Both ROI tractography and TBSS approaches detected
differences in FA between control and TBI participants. As
Fig. 1 Representation of fibers assessed in DTIstudio in a sagittal, b coronal, and c axial planes. Red corpus callosum, Yellow cingulate bundles,
Brown superior longitudinal fasciuli, Green inferior longitudinal fasciculi, Blue internal capsules (Color figure online)
Brain Topogr
123
Fig. 3 shows, several of the ROIs differentiated signifi-
cantly between control and TBI participants. Moderate and
severe TBI participants displayed significantly lower CC
FA compared to controls and those with mild TBI. Severe
TBI participants were the only TBI group to display a
reduction in cingulate bundle FA, compared to control and
moderate TBI participants. Similarly, severe TBI partici-
pants were the only group to show reduced FA in the left
and right SLF compared to controls and mild TBI partici-
pants. However, this difference was not significant when
the Bonferroni-corrected p value was applied. Participants
with moderate and severe TBI displayed lower FA in the
left ILF, whereas in the right ILF severe TBI participants
displayed FA reductions compared to all other groups.
Moderate and severe TBI participants displayed reduced
FA in the left and right internal capsules compared to
controls and those with mild TBI. Although individuals
with mild TBI displayed a tendency to have lower FA
compared to controls, such as in the cingulate bundle and
internal capsules, none of the differences were statistically
significant.
The results of TBSS display similar patterns of white
matter injury compared to ROI tractography. That is, no
significant differences in FA were found between control
and mild TBI participants, whereas moderate and severely
injured TBI participants displayed significant widespread
reductions in FA. The reduction in FA as injury severity
increased can be seen in panel A of Fig. 4, wherein PTA
treated continuously is examined. That is, with greater
days of PTA reduced FA is present almost throughout the
entire brain. As displayed in panels C and D of Fig. 4,
compared to controls, individuals with moderate and
severe TBI displayed reduced FA in the CC, ILF, SLF,
cingulate bundle, as well as the PLIC. However, the TBSS
results show that reductions in FA may be present in only
specific parts of tracts, and may not be found over the
entire white matter bundle. Severe TBI participants were
found to have the most extensive reductions in FA, with
significant differences found compared to control, mild,
as well as moderate groups. However, as can be noted in
Fig. 4, the differences between moderate and severe TBI
groups was not as extensive as when comparing severe
TBI participants with controls or indivduals with mild
TBI (Fig. 5).
Neuropsychological Performance
Comparisons were made between TBI and control partic-
ipants, co-varying for level of education. After controlling
for education, participants with TBI displayed significantly
Fig. 2 Initial seed point
locations used to track fibers in
DTIStudio. a Initial seed point
for the posterior limb of the
internal capsule. b Initial seed
point for the corpus callosum.
c Initial seed point for the
inferior longitudinal fasciculus.
d Initial seed point for the
superior longitudinal fasciculus
(brown) and the cingulum
bundle (yellow) (Color figure
online)
Brain Topogr
123
poorer performance in total recall, and the SDMT. Table 2
displays the results of these comparisons.
Neuropsychological Performance is Related
to Fractional Anisotropy
Several associations were found between neuropsycho-
logical measures and FA, controlling for age, years of
education, time post injury, and gender. Using ROI trac-
tography, the COWAT verbal fluency was found to be
positively correlated with FA in the left SLF (r = .35,
p \ .05). Worse performance on the Hayling sentence
completion test part B was correlated with lower FA in the
left (r = -.39, p \ .05) and right (r = -.38, p \ .05)
SLF. Greater Hayling overall scaled score was significantly
correlated with higher FA in the left (r = .52, p \ .01) and
right (r = .50, p \ .01) SLF. Poorer performance on the
Trails B was related to lower FA in the right internal
capsule (r = -.41, p \ .05). Lastly, worse performance on
the SDMT correlated with lower FA in the CC (r = .37,
p \ .05) right SLF (r = .36, p \ .05), and the right ILF
(r = .35, p \ .05).
TBSS analyses examining the relationships between
cognition and FA revealed some similarities to those
obtained using the ROI approach. Lower Hayling overall
scaled score was related to reduced FA in parts of SLF.
Fig. 3 Injury group
comparisons using region-
of-interest tractography. Graphsdisplay scatter dot plots of FA
values for control, mild,
moderate, and severe groups.
p values have been derived from
ANCOVA, controlling for age,
gender, and years of education.
All p values below the .05
threshold were included;
however, only the p values
denoted with a remained
significant at the Bonferroni
corrected level of p \ .008. The
overlayed horizontal line plots
represent the mean and standard
error above and below the mean
Brain Topogr
123
However the Hayling overall scaled score was also related
to FA in the CC, ILF, and cingulum, and was almost
exclusively restricted to the left hemisphere. Moreover, the
SDMT displayed the strongest relationship with the ROI
tractography, which was also found to be the case in the
TBSS analyses. Similar to the Hayling overall scaled score,
performance on the SDMT was found to correlate with
FA in a more extensive network of tracts. These included
the left and right ILF, left and right SLF, CC, as well as the
cingulate bundle. Lastly, worse performance on the
DOORS visual memory test was related to FA in the TBSS
analyses, but not in the ROI analyses. The relationship
between the DOORS test and FA was similar to the Hay-
ling overall scaled score, being restricted to the left
hemisphere and being associated with sections of the ILF,
SLF, and CC.
Discussion
This study had three primary aims: to examine whether FA
of white matter tracts following TBI was associated with
the severity of the injury—defined using days of PTA,
whether cognitive performance was associated white mat-
ter FA, and lastly to investigate the comparability of ROI
and TBSS approaches. Overall, the findings indicated that
significantly lower FA is found in several white matter
tracts following moderate and severe TBI. Individuals with
mild injuries did not show significantly lower FA, com-
pared to controls, although trends were apparent in certain
cases and the lack of statistical significance may be due to
the small size of the mild TBI subsample in the current
study. Information processing and executive cognitive
abilities were found to be associated with several
Fig. 4 Tract-based spatial
statistics showing injury
severity group comparisons.
a Correlation analysis showing
the association between FA and
PTA measured continuously.
b Group comparisons between
controls and the TBI group as a
whole. c Group comparisons
between control and moderate
TBI participants. d Group
comparisons between control
and severe TBI participants.
e Group comparisons between
mild and severe TBI
participants. f Group
comparisons between moderate
and severe TBI participants.
Tract-based spatial statistics
were thresholded at p \ .05.
Higher intensity colours
represent lower p values. Axial
z coordinates are the same for
all slices and are represented
above the top comparison.
Tracts have been ‘thickened’ to
enhance visualisation of results
Brain Topogr
123
prominent white matter tracts. Interestingly, visual memory
was also associated with FA of several white matter tracts.
For the first time this study has compared ROI tractography
and whole-brain TBSS approaches, and results suggests
both similar and divergent patterns.
Demonstrated using both ROI and TBSS approaches,
the present findings showed that FA decreases with greater
injury severity. That is, all regions chosen a priori for
tractography analyses displayed reduced FA in individuals
with severe TBI compared to healthy controls. Although
differences were not as pronounced as in those with severe
injuries, participants with moderate TBI displayed lower
FA in all a priori tracked regions except for the SLF and
cingulate bundle. The TBSS analyses largely support the
ROI tractography approach. Moderate and severe TBI
participants displayed reduced FA compared to controls,
while individuals with severe TBI displayed the most
reduced FA compared to controls, mild, or moderate TBI
participants. Nevertheless, the TBSS results also highlight
that parts of white matter tracts—rather than the entire
bundle—may display reduced FA, which may go unnoticed
when conducting ROI tractography; for example, only
certain parts of the CC differed when comparing control
and moderate TBI participants, or when comparing mod-
erate and severe TBI participants.
Although a trend of lower FA was found between the
mild TBI group and healthy controls, no significant dif-
ferences were found, contrary to several previous studies
(Lipton et al. 2008; Lo et al. 2009; Mayer et al. 2010; Niogi
et al. 2008a, b). This may have been due to the small
sample of individuals with mild TBI which may have
resulted in low statistical power. This inconsistency in
study findings may also be due to differences in the time at
which participants were scanned, and in participant
recruitment criteria. Miles et al. (2008) scanned partici-
pants between one and 10 days post-injury, whereas Mayer
et al. (2010) scanned participants within 21 days following
injury. Since the greatest change to axonal structure and
function occurs in the immediate days following the injury,
scans of acute changes may more readily detect pathology.
Axonal pathology may be absent at follow-up, at least for
mild injuries due to axonal reorganisation (Bigler 2001;
Povlishock and Jenkins 1995; Povlishock and Katz 2005).
Indeed, when Miles et al. (2008) followed up participants
at 6 months post-injury, differences were no longer found
between healthy controls and individuals with mild TBI in
FA measures. Moreover, variability in the spatial distri-
bution of injury across studies, as well as between injury
severity groups, may in part explain these non-significant
group findings.
Furthermore, Mayer et al. (2010), Niogi et al. (2008a, b),
and Lipton et al. (2008) only included individuals that had
reported some form of post-concussive symptoms, includ-
ing cognitive difficulties. Since it has been widely noted
that cognition recovers for most of those with mild TBI
within the first 3 months after injury, it may be that the
Fig. 5 Tract-based spatial statistics showing areas of significant
correlation between FA and neuropsychological performance.
a Tract-based spatial statistics showing significant correlations
between FA and performance on the DOORS Test. b Tract-based
spatial statistics showing significant correlations between FA and
performance on the SDMT. c Tract-based spatial statistics showing
significant correlations between FA and performance on the Hayling
sentence completion test. Tract-based spatial statistics were threshol-
ded at p \ .05. Higher intensity colours represent lower p values.
Axial z coordinates are represented above each correlation. Tracts
have been ‘thickened’ to enhance visualisation of results
Brain Topogr
123
samples involved in these studies reflected the subgroup of
individuals that continue to show impairments (Dikmen
et al. 1995; Schretlen and Shapiro 2003). Indeed, Messe
et al. (2011) found that only those individuals with mild
TBI with residual neurobehavioural complaints demon-
strated poorer white matter integrity compared to healthy
controls. Moreover, recent studies suggest that standard
neuropsychological measures may not be sufficiently sen-
sitive to detect the subtle changes in FA following mild
TBI. For example, in their recent study, Geary et al. (2010)
found that deficits in learning strategy were associated with
reductions in FA following chronic mild TBI.
The relationship between white matter integrity and
cognitive abilities is further strengthened by the findings of
the current study, which show that prominent tracts
including the ILF, internal capsule, SLF, and the CC are
asssociated with information processing and executive
functions. However, memory was largely unrelated to the
integrity of white matter, with the exception of visual
memory, which showed an association with the left ILF,
SLF, and CC in the TBSS analyses. These findings differ
from other studies, which have found an association
between memory and the integrity of several white matter
tracts. For example Bigler et al. (2010) found the visual
memory was associated with FA in the right ILF and left
inferior fronto-occipital fasciculi (IFOF) whereas Kraus
et al. (2007) found that memory was related to FA in the
CC, forceps, sagittal stratum and IFOF.
However, it is also not surprising that memory was not
strongly associated with white matter integrity since tracts
primarily known to modulate memory, such as the fornices
and thalamic nuclei, were not examined in this study
(Aggleton 2008; Aggleton and Brown 1999; Metzler-
Baddeley et al. 2011). Even if these regions had been
considered a priori, the streamline tractography used in the
current study may not have been able to adequately
reconstruct these fibers, unlike what has been shown using
probabilistic tractography methods (Behrens et al. 2003;
Johansen-Berg et al. 2005). In addition, due to the high
level of uncertainty regarding fibre direction, and the dif-
ficulty in separating white and grey matter boundaries in
these regions, it is likely that these tracts were excluded as
part of the TBSS analyses in order to avoid difficulties in
interpretation (Smith et al. 2007). Imaging parameters such
as those used by Kinnunen et al. (2011), in which diffu-
sion-weighted data is collected in a greater number of
directions and using significantly reduced slice thickness
may need to be utilised to more reliably explore these
pathways.
Nevertheless, the significant associations between the
integrity of white matter tracts, information processing, and
executive functions is largely consistent with previous
research in this area. The finding that performance on the
COWAT, Hayling test, and SDMT was related to associ-
ation tracts—connecting posterior to anterior brain
regions—as well as the CC and frontal tracts is not
Table 2 Cognitive test performance comparisons between TBI and control participants
Measure TBI total cognitive
subsample
N = 36
TBI mild
N = 4
TBI moderate
N = 8
TBI severe
N = 24
Control
N = 25
Total TBI
vs control
Mdn, M (SD) Mdn, M (SD) Mdn, M (SD) Mdn, M (SD) Mdn, M (SD) t
Total recall 44.50, 43.72 (10.16) 44.00, 40.25 (14.15) 47.00, 48.12 (9.00) 45.00, 42.17 (9.85) 56.00, 55.36 (8.12) 4.01***
Visual memory 17.00, 16.61 (3.92) 18.00, 18.25 (3.30) 16.00, 17.00 (4.90) 17.00, 16.21 (3.73) 19.00, 19.00 (2.53) 1.87
Hayling—Time
A
6.00, 12.52 (14.06) 8.00, 8.25 (3.30) 7.50, 12.00 (11.46) 6.00, 13.45 (16.05) 6.00, 7.54 (5.18) -0.42
Hayling—Time B 23.00, 32.45 (29.55) 22.00, 20.50 (14.82) 14.50, 20.43 (20.25) 25.00, 38.45 (32.69) 18.50, 19.17 (11.48) -1.49
Hayling—scaled 6.00, 5.67 (1.49) 6.00, 5.75 (1.26) 6.00, 6.00 (1.53) 6.00, 5.55 (1.57) 6.00, 6.13 (.61) -.01
COWAT 36.50, 36.50 (13.32) 39.00, 39.50 (3.00) 36.50, 43.25 (17.08) 36.00, 33.75 (12.45) 43.50, 42.52 (9.33) 1.01
Trails A time 25.38, 28.86 (10.49) 29.92, 33.03 (11.41) 21.28, 24.58 (10.02) 27.52, 29.46 (10.52) 21.71, 23.47 (9.00) -1.01
Trails B time 60.34, 71.18 (32.92) 63.54, 74.19 (45.02) 60.34, 74.58 (53.04) 75.10, 69.48 (22.86) 53.04, 55.99 (23.74) -.97
Trails B–Trails A 36.00, 43.17 (28.33) 27.08, 41.16 (41.13) 39.60, 49.99 (43.50) 36.67, 41.27 (20.05) 29.05, 32.53 (18.45) -.72
Digit span:
forward
10.00, 10.23 (2.93) 9.00, 9.00 (.82) 8.00, 10.00 (3.82) 11.00, 10.52 (2.86) 11.00, 11.24 (2.45) .92
Digit span:
backwards
8.00, 8.23 (2.94) 7.00, 7.50 (3.00) 7.50, 9.00 (4.07) 8.00, 8.09 (2.56) 9.00, 9.68 (2.21) 1.13
SDMT 50.00, 50.67 (12.38) 55.00, 53.50 (7.72) 51.00, 55.75 (18.16) 50.00, 48.50 (10.49) 63.00, 62.84 (9.21) 3.15**
All comparisons between TBI and control participants were controlled for years of education
SDMT symbol digit modalities test, Hayling Hayling overall scaled score
* p \ .05; ** p \ .01; *** p \ .001
Brain Topogr
123
surprising given that these measures require the integration
of information across various modalities, speed of infor-
mation processing as well as executive functions. That is,
previous studies have highlighted the use of the CC—
especially the genu— as well as the association tracts that
connect occipital to frontal regions—including the SLF,
ILF— in modulating speed of information processing in
the general population (Bucur et al. 2008; Fling et al. 2011;
Konrad et al. 2009; Turken et al. 2008). Information is
initially received in the occipital visual areas before being
transmitted to frontal regions via the dorsal and ventral
streams (Foxe and Simpson 2002).
As a whole, the results are promising regarding the
comparability of ROI and TBSS approaches, both in terms
of their relationships with injury severity and cognitive
functioning. That is, both techniques delineated between the
severity of TBI, using PTA, whereby greater reductions in
FA were found with worse TBI severity. In addition, both
techniques indicated associations between FA, the SDMT
and Hayling test. However, there were also some notable
differences between the ROI and TBSS results. Namely,
whereas the ROI tractography was limited to the small
number of a priori selected regions, TBSS analysis offered
greater breadth of analysis. This difference was demon-
strated in the greater number of tracts associated with injury
severity and cognition in the TBSS analyses, compared to
the ROI approach. This was especially noticeable for the
associations with cognition. Whereas, only one or two ROIs
were related to cognitive performance for each measure,
TBSS analysis detected a significantly greater number of
associated tracts. A second difference is that TBSS is
capable of detecting differences anywhere along a tract, or
for only a section of the tract. This is especially critical for
the exploration of cognitive functions, as only sections of
larger tracts may be of interest. Due to the aforementioned
differences between the two techniques, it is suggested that
examination of white matter pathology may be applied in a
two-stage process. As occurred with the current findings, it
is likely that more frequently ROI tractography—when
restricted to whole white matter bundles—underestimates
the extensiveness of FA reductions following TBI. More-
over, specificity within white matter tracts is missing,
whereby only parts of the tracts may display reduced FA.
Whole-brain TBSS may be applied initially as a screening
measure with the intent of highlighting all significant
regions where white matter changes are found. A second
step may then be taken to explore these significant regions in
more depth using quantitative tractography. That is, TBSS
only captures significant change to the centres of white
matter tracts. Visualising regions using tractography pro-
vides more information, both quantitative and qualitative,
regarding the changes that have taken place, including any
disconnection between tracts and changes in structure.
The current study has some limitations regarding the
imaging protocol and methods of analysis. Firstly, due to
the clinical setting in which this study took place it was not
feasible to scan participants for an extended length of time,
which would have ensured diffusion-weighted acquisition
in a greater number of directions and at higher resolution.
To circumvent this limitation, larger white matter tracts
were the focus of study. However, as already discussed,
other tracts, located in more complex regions of the brain
but nevertheless related to function, were not explored. In
addition, the current study focused solely on FA as an
indicator of white matter integrity. Other indices, including
mean, radial, and axial diffusivity may have also revealed
associations of interest with injury severity and cognitive
functioning. The limitation inherent to the DTI method,
namely the difficulty dealing with crossing fibers, is of
concern especially given the DTI resolution used in the
current study. Additionally, although it is inferred in the
current study that reduced FA was specifically indicative of
abnormal connectivity, other changes following TBI may
also have an impact on FA. For example, it is not known to
what extent atrophic or neuroinflammatory changes or
increased extracellular space impacts on FA.
In conclusion, the current study showed significantly
reduced FA following moderate and severe TBI. Informa-
tion processing, executive abilities, and visual memory
were found to be related to FA of white matter tracts con-
necting the posterior to anterior cortices. For the first time,
both ROI tractography and TBSS techniques were used in a
TBI sample to examine how they pertain to injury severity
and cognitive functioning. The results suggested that using
these techniques in combination may derive better results
regarding detection of pathology following TBI.
Acknowledgments We thank all the staff of Healthcare Imaging
MRI facility at the Epworth Hospital, Melbourne, Victoria.
Conflict of interest The authors declare that they have no com-
peting financial interests.
References
Aggleton JP (2008) Understanding anterograde amnesia: disconnec-
tions and hidden lesions. Q J Exp Psychol 61:1441–1471
Aggleton JP, Brown MW (1999) Episodic memory, amnesia and
the hippocampal-anterior thalamic axis. Behav Brain Sci 22:
425–444
Arfanakis K, Haughton VM, Carew JD, Rogers BP, Dempsey RJ,
Meyerand ME (2002) Diffusion tensor mr imaging in diffuse
axonal injury. Am J Neuroradiol 23:794–802
Ashburner J, Friston KJ (2000) Voxel-based morphometry—the
methods. Neuroimage 11:805–821
Baddeley A, Emslie H, Nimmo-Smith I (1994) Doors and people.
Thames Valley Test Company, Bury St Edmunds
Brain Topogr
123
Basser PJ (1995) Inferring microstructural features and the physio-
logical state of tissues from diffusion-weighted images. NMR
Biomed 8:333–344
Basser PJ, Mattiello J, Lebihan D (1994) Mr diffusion tensor
spectroscopy and imaging. Biophys J 66:259–267
Behrens TEJ, Johansen-Berg H, Woolrich MW, Smith SM, Wheeler-
Kingshott CAM, Boulby PA et al (2003) Non-invasive mapping
of connections between human thalamus and cortex using
diffusion imaging. Nat Neurosci 6:750–757
Benson RR, Meda SA, Vasudevan S, Kou ZF, Govindarajan KA,
Hanks RA et al (2007) Global white matter analysis of diffusion
tensor images is predictive of injury severity in traumatic brain
injury. J Neurotrauma 24:446–459
Benton AL, Hamsher K, Rey GJ (1994) Multilingual aphasia
examination, 3rd edn. AJA Associates, Iowa Cita
Bigler ED (2001) The lesion(s) in traumatic brain injury: implica-
tions for clinical neuropsychology. Arch Clin Neuropsychol 16:
95–131
Bigler ED, McCauley SR, Wu TC, Yallampalli R, Shah S, MacLeod
M et al (2010) The temporal stem in traumatic brain injury:
preliminary findings. Brain Imaging Behav 4:270–282
Bookstein FL (2001) ‘‘Voxel-based morphometry’’ should not be used
with imperfectly registered images. Neuroimage 14:1454–1462
Bucur B, Madden DJ, Spaniol J, Provenzale JM, Cabeza R, White LE
et al (2008) Age-related slowing of memory retrieval: contribu-
tions of perceptual speed and cerebral white matter integrity.
Neurobiol Aging 29:1070–1079
Buki A, Povlishock JT (2006) All roads lead to disconnection?
Traumatic axonal injury revisited. Acta Neurochir 148:181–193
Burgess PW, Shallice T (1997) The Hayling and Brixton tests.
Thames Valley Test Company, Bury St Edmunds
Coughhlan AK, Oddy M, Crawford JR (2007) Birt memory and
information processing battery London. Brain injury rehabilita-
tion trust, Wakefield
Davatzikos C (2004) Why voxel-based morphometric analysis should
be used with great caution when characterizing group differ-
ences. Neuroimage 23:17–20
Dikmen SS, Machamer JE, Winn HR, Temkin NR (1995) Neuro-
psychological outcome at 1-year post head injury. Neuropsy-
chology 9:80–90
Draper K, Ponsford J (2008) Cognitive functioning ten years
following traumatic brain injury and rehabilitation. Neuropsy-
chology 22:618–625
Fling BW, Chapekis M, Reuter-Lorenz PA, Anguera J, Bo J, Langan J
et al (2011) Age differences in callosal contributions to cognitive
processes. Neuropsychologia 49:2564–2569
Foxe JJ, Simpson GV (2002) Flow of activation from v1 to frontal
cortex in humans: a framework for defining ‘‘early’’ visual
processing. Exp Brain Res 142:139–150
Geary EK, Kraus MF, Pliskin NH, Little DM (2010) Verbal learning
differences in chronic mild traumatic brain injury. J Int Neuro-
psychol Soc 16:506–516
Gennarelli TA, Thibault LE, Graham DI (1998) Diffuse axonal injury:
an important form of traumatic brain damage. Neuroscientist
4:202–215
Huisman TAGM, Sorensen AG, Hergan K, Gonzalez RG, Schaefer
PW (2003) Diffusion-weighted imaging for the evaluation of
diffuse axonal injury in closed head injury. J Comput Assist
Tomogr 27:5–11
Jiang H, van Zijl PCM, Kim J, Pearlson GD, Mori S (2006) Dtistudio:
resource program for diffusion tensor computation and fiber
bundle tracking. Comput Methods Programs Biomed 81:
106–116
Johansen-Berg H, Behrens TEJ, Sillery E, Ciccarelli O, Thompson
AJ, Smith SM et al (2005) Functional–anatomical validation and
individual variation of diffusion tractography-based segmenta-
tion of the human thalamus. Cereb Cortex 15:31–39
Jones DK, Griffin LD, Alexander DC, Catani M, Horsfield MA,
Howard R et al (2002) Spatial normalization and averaging of
diffusion tensor MRI data sets. Neuroimage 17:592–617
Jones DK, Symms MR, Cercignani M, Howard RJ (2005) The effect
of filter size on VBM analyses of DT-MRI data. Neuroimage
26:546–554
Kennedy MR, Wozniak JR, Muetzel RL, Mueller BA, Chiou HH,
Pantekoek K et al (2009) White matter and neurocognitive
changes in adults with chronic traumatic brain injury. J Int
Neuropsychol Soc 15:130–136
Kinnunen KM, Greenwood R, Powell JH, Leech R, Hawkins PC,
Bonnelle V et al (2011) White matter damage and cognitive
impairment after traumatic brain injury. Brain 134:449–463
Konrad A, Vucurevic G, Musso F, Stoeter P, Winterer G (2009)
Correlation of brain white matter diffusion anisotropy and mean
diffusivity with reaction time in an oddball task. Neuropsycho-
biology 60:55–66
Kraus MF, Susmaras T, Caughlin BP, Walker CJ, Sweeney JA, Little
DM (2007) White matter integrity and cognition in chronic
traumatic brain injury: a diffusion tensor imaging study. Brain
130:2508–2519
Kumar R, Husain M, Gupta RK, Hasan KM, Haris M, Agarwal AK
et al (2009) Serial changes in the white matter diffusion tensor
imaging metrics in moderate traumatic brain injury and corre-
lation with neuro-cognitive function. J Neurotrauma 26:481–495
Levin HS (2003) Neuroplasticity following non-penetrating traumatic
brain injury. Brain Inj 17:665–674
Levin HS, Wilde E, Troyanskaya M, Petersen NJ, Scheibel R,
Newsome M et al (2010) Diffusion tensor imaging of mild to
moderate blast-related traumatic brain injury and its sequelae.
J Neurotrauma 27:683–694
Lipton ML, Gellella E, Lo C, Gold T, Ardekani BA, Shifteh K et al
(2008) Multifocal white matter ultrastructural abnormalities in
mild traumatic brain injury with cognitive disability: a voxel-
wise analysis of diffusion tensor imaging. J Neurotrauma
25:1335–1342
Little DM, Kraus MF, Joseph J, Geary EK, Susmaras T, Zhou XJ et al
(2010) Thalamic integrity underlies executive dysfunction in
traumatic brain injury. Neurology 74:558–564
Lo C, Shifteh K, Gold T, Bello JA, Lipton ML (2009) Diffusion
tensor imaging abnormalities in patients with mild traumatic
brain injury and neurocognitive impairment. J Comput Assist
Tomogr 33:293–297
Mayer AR, Ling J, Mannell MV, Gasparovic C, Phillips JP, Doezema
D et al (2010) A prospective diffusion tensor imaging study in
mild traumatic brain injury. Neurology 74:643–650
Messe A, Caplain S, Paradot G, Garrigue D, Mineo J-F, Ares GS et al
(2011) Diffusion tensor imaging and white matter lesions at the
subacute stage in mild traumatic brain injury with persistent
neurobehavioral impairment. Hum Brain Mapp 32:999–1011
Metzler-Baddeley C, Jones DK, Belaroussi B, Aggleton JP, O’Sul-
livan MJ (2011) Frontotemporal connections in episodic memory
and aging: a diffusion MRI tractography study. J Neurosci
31:13236–13245
Miles L, Grossman RI, Johnson G, Babb JS, Diller L, Inglese M
(2008) Short-term DTI predictors of cognitive dysfunction in
mild traumatic brain injury. Brain Inj 22:115–122
Mori S, van Zijl PCM (2002) Fiber tracking: principles and strategies:
a technical review. NMR Biomed 15:468–480
Mori S, Wakana S, Van Zijl PCM (2005) MRI atlas of human white
matter. Elsevier, Amsterdam
Nakayama N, Okumura A, Shinoda J, Yasokawa YT, Miwa K,
Yoshimura SI et al (2006) Evidence for white matter disruption
Brain Topogr
123
in traumatic brain injury without macroscopic lesions. J Neurol
Neurosurg Psychiatry 77:6
Newcombe VFJ, Williams GB, Nortje J, Bradley PG, Harding SG,
Smielewski P et al (2007) Analysis of acute traumatic axonal
injury using diffusion tensor imaging. Br J Neurosurg
21:340–348
Niogi SN, Mukherjee P, Ghajar J, Johnson C, Kolster RA, Sarkar R
et al (2008a) Extent of microstructural white matter injury in
postconcussive syndrome correlates with impaired cognitive
reaction time: a 3t diffusion tensor imaging study of mild
traumatic brain injury. Am J Neuroradiol 29:967–973
Niogi SN, Mukherjee P, Ghajar J, Johnson CE, Kolster R, Lee H et al
(2008b) Structural dissociation of attentional control and mem-
ory in adults with and without mild traumatic brain injury. Brain
131:3209–3221
Park H-J, Kubicki M, Shenton ME, Guimond A, McCarley RW,
Maier SE et al (2003) Spatial normalization of diffusion tensor
MRI using multiple channels. Neuroimage 20:1995–2009
Ponsford J, Olver JH, Curran C (1995a) A profile of outcome: 2 years
after traumatic brain injury. Brain Inj 9:1–10
Ponsford J, Olver JH, Ng K (1995b) Prediction of employment status
2 years after traumatic brain injury. Brain Inj 9:11–20
Povlishock JT, Christman CW (1994) The pathobiology of traumat-
ically induced axonal injury in animals and humans: a review of
current thoughts. US Government Printing Office, Washington,
Dc
Povlishock JT, Jenkins LW (1995) Are the pathobiological changes
evoked by traumatic brain injury immediate and irreversible?
Brain Pathol 5:415–426
Povlishock JT, Katz DI (2005) Update of neuropathology and
neurological recovery after traumatic brain injury. J Head
Trauma Rehabil 20:76–94
Reitan RM, Wolfson D (1988) The Halstead–Reitan neuropsycho-
logical test battery. Neuropsychology Press, Tucson
Rugg-Gunn FJ, Symms MR, Barker GJ, Greenwood R, Duncan JS
(2001) Diffusion imaging shows abnormalities after blunt head
trauma when conventional magnetic resonance imaging normal.
J Neurol Neurosurg Psychiatry 70:530–533
Salmond CH, Menon DK, Chatfield DA, Williams GB, Pena A,
Sahakian BJ et al (2006) Diffusion tensor imaging in chronic
head injury survivors: correlations with learning and memory
indices. Neuroimage 29:117–124
Scheid R, Preul C, Gruber O, Wiggins C, von Cramon DY (2003)
Diffuse axonal injury associated with chronic traumatic brain
injury: evidence from t2*-weighted gradient-echo imaging at 3 t.
Am J Neuroradiol 24:1049–1056
Schretlen DJ, Shapiro AM (2003) A quantitative review of the effects
of traumatic brain injury on cognitive functioning. Int Rev Psych
15:341–349
Shenton ME, Hamoda HM, Schneiderman JS, Bouix S, Paternak O,
Rathi Y et al (2012) A review of magnetic resonance imaging
and diffusion tensor imaging findings in mild traumatic brain
injury. Brain Imaging Behav 6:137–192
Sidaros A, Engberg AW, Sidaros K, Liptrot MG, Herning M, Petersen
P et al (2008) Diffusion tensor imaging during recovery from
severe traumatic brain injury and relation to clinical outcome: a
longitudinal study. Brain 131:559–572
Smith A (1973) Symbol digit modalities test. Western Psychological
Services, Los Angeles
Smith SM, Nichols TE (2009) Threshold-free cluster enhancement:
addressing problems of smoothing, threshold dependence and
localisation in cluster inference. Neuroimage 44:83–98
Smith SM, Jenkinson M, Woolrich MW, Beckmann CF, Behrens TEJ,
Johansen-Berg H et al (2004) Advances in functional and
structural mr image analysis and implementation as fsl. Neuro-
image 23:S208–S219
Smith SM, Jenkinson M, Johansen-Berg H, Rueckert D, Nichols TE,
Mackay CE et al (2006) Tract-based spatial statistics: voxelwise
analysis of multi-subject diffusion data. Neuroimage 31:1487–1505
Smith SM, Johansen-Berg H, Jenkinson M, Rueckert D, Nichols TE,
Miller KL et al (2007) Acquisition and voxelwise analysis of
multi-subject diffusion data with tract-based spatial statistics.
Nat Protoc 2:499–503
Sugiyama K, Kondo T, Oouchida Y, Suzukamo Y, Higano S, Endo M
et al (2009) Clinical utility of diffusion tensor imaging for
evaluating patients with diffuse axonal injury and cognitive
disorders in the chronic stage. J Neurotrauma 26:1879–1890
Toth A, Kovacs N, Perlaki G, Orsi G, Aradi M, Komaromy H et al
(2013) Multi-modal magnetic resonance imaging in the acute
and sub-acute phase of mild traumatic brain injury: can we see
the difference? J Neurotrauma 30:2–10
Turken U, Whitfield-Gabrieli S, Bammer R, Baldo JV, Dronkers NF
et al (2008) Cognitive processing speed and the structure of
white matter pathways: convergent evidence from normal
variation and lesion studies. Neuroimage 42:1032–1044
Wechsler D (1997) Wechsler memory scale, 3rd edn. The Psycho-
logical Corporation, San Antonio
Wechsler D (2008) Wechsler adult intelligence scale, 4th edn.
Pearson, San Antonio
Xu J, Rasmussen IA, Lagopoulos J, Haberg A (2007) Diffuse axonal
injury in severe traumatic brain injury visualized using high-
resolution diffusion tensor imaging. J Neurotrauma 24:753–765
Brain Topogr
123
Related Documents