Med Intensiva. 2017;41(4):252---259 www.elsevier.es/medintensiva SCIENTIFIC LETTERS Ventricular electrical storm after acute myocardial infarction successfully treated with temporary atrial overdrive pacing Tormenta eléctrica ventricular tras infarto agudo de miocardio tratado con éxito mediante sobreestimulación auricular temporal Dear Editor, A 53-year-old-caucasian man, ex-smoker, with past medical history of dyslipidaemia had an out-of-hospital successful cardiopulmonary resuscitation after cardiac arrest in ven- tricular fibrillation (VF) due to an anterior ST-elevation myocardial infarction (STEMI). A primary percutaneous coronary intervention (PCI) was performed with revascula- rization of the left anterior descending artery (LAD) using a drug eluting stent. The pre-discharge echocardiogram showed a left ventricular ejection fraction (LEVF) of 40%. The patient was discharged at 6th day. Five days later the patient was resuscitated after another cardiac arrest with documented VF. A repeated coronary angiography revealed acute LAD stent thrombosis. A ‘‘stent in stent’’ PCI of LAD was successfully performed. In the following hours the patient evolved into cardiogenic shock with a LVEF of 20%. Aminergic and inotropic support was started with norepinephrine, dopamine and dobutamine, as well as intra-aortic balloon pump and invasive mechan- ical ventilation. On the second day of hospitalization the patient presented several episodes of polymorphic ventri- cular tachycardia (VT), triggered by premature ventricular complexes (VPC), that rapidly degenerated into VF (Fig. 1). PR, QRS and QT intervals were normal. Intravenous amio- darone, esmolol, lidocaine, magnesium and midazolam were administered. Despite maintaining of combined antiar- rhythmic drugs (AAD) ventricular tachyarrythmias persisted, exhibiting the same pattern for VT/VF initiation. In order to suppress premature ectopic beats, it was decided to perform atrial overdrive pacing. This was accom- plished by using a temporary pacemaker, programmed at 85 bpm (heart rate before pacing was 60 beats per minute), with an active fixation catheter (Biotronik TC-116-Screw) placed in the right atrial appendage, by femoral approach (Fig. 2). After starting atrial pacing there was a complete sup- pression of VPC and no more VT episodes were observed. AAD were progressively weaned off while maintaining atrial pacing at the same rate and, although lidocaine was discon- tinued and amiodarone switched to an oral regimen, neither VPC nor VT/VF recurred. The electrocatheter was removed on the 8th day after implantation (four days after suspension of lidocaine and switching of amiodarone to oral regimen). Before discharge, the patient underwent a dual-chamber ICD implantation with the pacing rate programmed at 80 bpm, and two zones of tachycardia detection and corresponding therapies (VT zone: at 170 bpm; VF zone: at 210 bpm). Discussion The incidence of sustained ventricular arrhythmias (VA) in acute coronary syndromes (ACS) is 5---10%. 1 In the context of ischaemia, VPC, VT and VF can be secondary to an automatic or reentrant mechanism. 1,2 Myocardial ischaemia leads to changes in the ionic imbalance of cardiomyocytes, resulting in shorter duration of the action potential and less neg- ative resting membrane potential. 1 In this condition early and delayed triggers after depolarization may occur, induc- ing VPC and arrhythmogenic currents, especially from the ischaemic/reperfused to the non-ischaemic areas. 1,2 In our patient the VPC provoked ‘‘R-on-T’’ phenomenon, resulting in recurrent episodes of VT and VF (Fig. 1). Amiodarone blocks the depolarizing sodium currents and potassium channels responsible for conduction of repo- larizing currents inhibiting ventricular arrhythmias (VA) by influencing automaticity and re-entry, 3,4 and esmolol blocks sympathetic mediated triggering mechanisms under- lying VA. 2,5 Despite the combined AAD therapy, the patient maintained recurrent episodes of VT/VF and perfusion of lidocaine was started without obtaining electrical stability. 2,3,6 Temporary overdrive pacing has been pointed as an option for drug resistant ventricular arrythmias. 7,8 In recent European Society of Cardiology’s Guidelines for the man- agement of ventricular arrhythmias, transvenous catheter overdrive stimulation received a class IIa of recommenda- tions, level of evidence C, in cases of recurrent VA despite the use of anti-arrhythmic drugs. 3 Lower heart rate results in increased ventricular repo- larization heterogeneity and increases the possibility of an ectopic ventricular complex reaching reentrant tissue after refractory period. The heart rate increases with tem- porary pacing, shortens the interval between beats and Downloaded for Monica Teixeira ([email protected]) at Centro Hospitalar Lisboa Central from ClinicalKey.com by Elsevier on October 16, 2017. For personal use only. No other uses without permission. Copyright ©2017. Elsevier Inc. All rights reserved.

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

M
S
Vaiwp
Tamt
D
AhctmcrasT
caifwsaipccPdwre
dp8wp(
Downloa
ed Intensiva. 2017;41(4):252---259
www.elsevier.es/medintensiva
CIENTIFIC LETTERS
entricular electrical stormfter acute myocardial
After starting atrial pacing there was a complete sup-pression of VPC and no more VT episodes were observed.AAD were progressively weaned off while maintaining atrial
ptVooBiatD
Taiociaaii
r
plbblmos
oEaott
larization heterogeneity and increases the possibility ofan ectopic ventricular complex reaching reentrant tissue
nfarction successfully treatedith temporary atrial overdriveacing
ormenta eléctrica ventricular tras infartogudo de miocardio tratado con éxitoediante sobreestimulación auricular
emporal
ear Editor,
53-year-old-caucasian man, ex-smoker, with past medicalistory of dyslipidaemia had an out-of-hospital successfulardiopulmonary resuscitation after cardiac arrest in ven-ricular fibrillation (VF) due to an anterior ST-elevationyocardial infarction (STEMI). A primary percutaneous
oronary intervention (PCI) was performed with revascula-ization of the left anterior descending artery (LAD) using
drug eluting stent. The pre-discharge echocardiogramhowed a left ventricular ejection fraction (LEVF) of 40%.he patient was discharged at 6th day.
Five days later the patient was resuscitated after anotherardiac arrest with documented VF. A repeated coronaryngiography revealed acute LAD stent thrombosis. A ‘‘stentn stent’’ PCI of LAD was successfully performed. In theollowing hours the patient evolved into cardiogenic shockith a LVEF of 20%. Aminergic and inotropic support was
tarted with norepinephrine, dopamine and dobutamine,s well as intra-aortic balloon pump and invasive mechan-cal ventilation. On the second day of hospitalization theatient presented several episodes of polymorphic ventri-ular tachycardia (VT), triggered by premature ventricularomplexes (VPC), that rapidly degenerated into VF (Fig. 1).R, QRS and QT intervals were normal. Intravenous amio-arone, esmolol, lidocaine, magnesium and midazolamere administered. Despite maintaining of combined antiar-
hythmic drugs (AAD) ventricular tachyarrythmias persisted,xhibiting the same pattern for VT/VF initiation.
In order to suppress premature ectopic beats, it wasecided to perform atrial overdrive pacing. This was accom-lished by using a temporary pacemaker, programmed at5 bpm (heart rate before pacing was 60 beats per minute),ith an active fixation catheter (Biotronik TC-116-Screw)
laced in the right atrial appendage, by femoral approachFig. 2).ap
ded for Monica Teixeira ([email protected]) at Centro Hospitalar Lisboa CenFor personal use only. No other uses without permission. Copyright ©2017
acing at the same rate and, although lidocaine was discon-inued and amiodarone switched to an oral regimen, neitherPC nor VT/VF recurred. The electrocatheter was removedn the 8th day after implantation (four days after suspensionf lidocaine and switching of amiodarone to oral regimen).efore discharge, the patient underwent a dual-chamber ICD
mplantation with the pacing rate programmed at 80 bpm,nd two zones of tachycardia detection and correspondingherapies (VT zone: at 170 bpm; VF zone: at 210 bpm).
iscussion
he incidence of sustained ventricular arrhythmias (VA) incute coronary syndromes (ACS) is 5---10%.1 In the context ofschaemia, VPC, VT and VF can be secondary to an automaticr reentrant mechanism.1,2 Myocardial ischaemia leads tohanges in the ionic imbalance of cardiomyocytes, resultingn shorter duration of the action potential and less neg-tive resting membrane potential.1 In this condition earlynd delayed triggers after depolarization may occur, induc-ng VPC and arrhythmogenic currents, especially from theschaemic/reperfused to the non-ischaemic areas.1,2
In our patient the VPC provoked ‘‘R-on-T’’ phenomenon,esulting in recurrent episodes of VT and VF (Fig. 1).
Amiodarone blocks the depolarizing sodium currents andotassium channels responsible for conduction of repo-arizing currents inhibiting ventricular arrhythmias (VA)y influencing automaticity and re-entry,3,4 and esmolollocks sympathetic mediated triggering mechanisms under-ying VA.2,5 Despite the combined AAD therapy, the patientaintained recurrent episodes of VT/VF and perfusion
f lidocaine was started without obtaining electricaltability.2,3,6
Temporary overdrive pacing has been pointed as anption for drug resistant ventricular arrythmias.7,8 In recenturopean Society of Cardiology’s Guidelines for the man-gement of ventricular arrhythmias, transvenous catheterverdrive stimulation received a class IIa of recommenda-ions, level of evidence C, in cases of recurrent VA despitehe use of anti-arrhythmic drugs.3
Lower heart rate results in increased ventricular repo-
fter refractory period. The heart rate increases with tem-orary pacing, shortens the interval between beats and
tral from ClinicalKey.com by Elsevier on October 16, 2017.. Elsevier Inc. All rights reserved.

SCIENTIFIC LETTERS 253
A
B
C
D
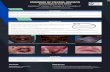
R on T
Figure 1 (A) R on T phenome; (B) R on T phenome, followed by ventricular ectopies; (C) ventricular tachycardia; (D) ventriculartachycardia degenerating into ventricular fibrillation.
ap
dpA
Down
decreases the likelihood of appearance of premature ven-tricular complexes and increases the likelihood of thesereaching pro-arrhythmic tissue in refractory period.
As right ventricular pacing can be deleterious for ventri-cular systolic function, and this patient presented a severeimpairment in LVEF without evidence of atrio-ventricular
conduction disturbances, electrical stimulation was per-formed in an uncommon way, using an active fixationtemporary pacing catheter placed in the right atrium. Theaim was to obtain intrinsic atrioventricular conduction withtspt
loaded for Monica Teixeira ([email protected]) at Centro Hospitalar Lisboa CFor personal use only. No other uses without permission. Copyright ©2
narrow QRS and avoid the deleterious effect of ventricularacing in a patient with cardiogenic shock.
Temporary pacing with an active fixation catheter isesigned to allow ventricular septal pacing, but alternativeacing points can also be obtained with this type of catheter.ttention should be given while placing this lead in loca-
ions other than ventricular septum. Positioning in the atrialeptum could be safer and avoid potential complications inatients where any perforation can be a severe complica-ion. The femoral approach may facilitate positioning of theentral from ClinicalKey.com by Elsevier on October 16, 2017.017. Elsevier Inc. All rights reserved.

254 SCIENTIFIC LETTERS
F r, pl(
lta
fd
epf
C
T
R
1
2
3
4
5
6
7
8
SL
P
∗
Downloa
igure 2 (A) Chest radiography showing active fixation catheteB) Inverted image.
ead in an atrial positioning but, due to longer intravenousrajectory and the exposed fixation helix, the right jugularpproach may be preferred.
The use of non-active fixation temporary pacing leadsor atrial pacing might be also considered but the risk ofislodgement is high.
In conclusion, temporary atrial overdrive pacing is anffective and safe treatment for resistant electrical storm inatients with severe impairment of left ventricular systolicunction.
onflict of interest
he authors have no disclosures.
eferences
. Piccini JP, Berger JS, Brown DL. Early sustained ventriculararrhythmias complicating acute myocardial infarction. Am J Med.2008;121:797---804.
. Gorenek B, Blomström Lundqvist C, Brugada Terradellas J, CammAJ, Hindricks G, Huber K, et al. Cardiac arrhythmias in acutecoronary syndromes: position paper from the joint EHRA, ACCA,and EAPCI task force. Europace. 2014;16:1655---73.
. Authors/Task Force Members, Priori SG, Blomström-Lundqvist C,Mazzanti A, Blom N, Borggrefe M, et al. 2015 ESC Guidelinesfor the management of patients with ventricular arrhythmias
and the prevention of sudden cardiac death: the Task Forcefor the Management of Patients with Ventricular Arrhythmiasand the Prevention of Sudden Cardiac Death of the Euro-pean Society of Cardiology (ESC) Endorsed by: Association forE2©
ded for Monica Teixeira ([email protected]) at Centro Hospitalar Lisboa CenFor personal use only. No other uses without permission. Copyright ©2017
aced in the right atrial appendage by femoral approach (arrow).
European Paediatric and Congenital Cardiology (AEPC). Eur HeartJ. 2015;36:2793---867.
. Wolfe CL, Nibley C, Bhandari A, Chatterjee K, Scheinman M.Polymorphous ventricular tachycardia associated with acutemyocardial infarction. Circulation. 1991;84:1543---51.
. Piccini JP, Hranitzky PM, Kilaru R, Rouleau JL, White HD, AylwardPE, et al. Relation of mortality to failure to prescribe beta block-ers acutely in patients with sustained ventricular tachycardiaand ventricular fibrillation following acute myocardial infarc-tion (from the VALsartan In Acute myocardial iNfarcTion trial[VALIANT] Registry). Am J Cardiol. 2008;102:1427---32.
. Piccini JP, Schulte PJ, Pieper KS, Mehta RH, White HD, Van de WerfF, et al. Antiarrhythmic drug therapy for sustained ventriculararrhythmias complicating acute myocardial infarction. Crit CareMed. 2011;39:78---83.
. Kurisu S, Inoue I, Kawagoe T, Ishihara M, Shimatani Y, MitsubaN, et al. Temporary overdriving pacing as an adjunct to antiar-rhythmic drug therapy for electrical storm in acute myocardialinfarction. Circ J. 2005;69:613---6.
. Yoshida T, Naito Y, Nishimura K. Temporary ventricular overdrivepacing for electrical storm after coronary artery bypass grafting.Gen Thorac Cardiovasc Surg. 2011;59:756---9.
. Aguiar Rosa ∗, M. Oliveira, B. Valente, P. Silva Cunha,
. Almeida Morais, R. Cruz Ferreira
Cardiology Department, Santa Marta Hospital, Lisbon,ortugal
Corresponding author.
-mail address: [email protected] (S. Aguiar Rosa).173-5727/2016 Elsevier Espana, S.L.U. and SEMICYUC. All rights reserved.
tral from ClinicalKey.com by Elsevier on October 16, 2017.. Elsevier Inc. All rights reserved.
Related Documents