Value Stream Mapping and the Journey of the Northern ACS Patient Ronnalea Hamman, MSc. Lean Leader, imPROVE Provincial Health Services Authority Barbara Hennessy RN, MN, CCN(C) Regional Coordinator, Cardiac and Cerebrovascular Services Northern Health Julie Dhaliwal, BA CYC (cert) Manager, Medical Services, University Hospital of Northern BC Northern Health

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
Value Stream Mapping and the Journey of the Northern ACS Patient
Ronnalea Hamman, MSc.Lean Leader, imPROVEProvincial Health Services Authority Barbara Hennessy RN, MN, CCN(C)Regional Coordinator, Cardiac and Cerebrovascular ServicesNorthern Health Julie Dhaliwal, BA CYC (cert)Manager, Medical Services, University Hospital of Northern BCNorthern Health
© Provincial Health Services Authority
Objectives
1. Understand the process of Value Stream Mapping • Theory• Tool• Application in an Agency Setting
2. Review the process of a provincial Value Stream Map• Home to Home Journey of the Northern Health Patient through tertiary
cardiac services.
3. Review initial improvements from a provincial Value Stream.
• Discharge Preparation of the Northern Cardiac Patient
© Provincial Health Services Authority
Value Stream Map
A value stream map is a management tool for a cross-functional team to look at value streams rather than at discrete operations.
© Provincial Health Services Authority
Benefits
• Patient/Family-centric• Data-driven• Forces participants to discuss how they see the value stream• Drives consensus as to how all perspectives are represented along
the value stream• It is an alignment tool that allows people to understand and improve
processes• Provides a framework to see, learn and act together
© Provincial Health Services Authority
Value Stream Management
Value Stream Management
Daily Management
Unit UnitUnitUnitUnit
Unit UnitUnitUnitUnit
Unit UnitUnitUnit
UnitUnit
Strategy Deployment
Director Director
Program ProgramProgramProgramProgram
Exec
© Provincial Health Services Authority
How does it differ from process mapping?• Flowcharting techniques to understand a process.• Multiple perspectives define the process boxes (not from
patient POV).• Does not identify value added components.
Pick up mail
Open & date stamp
Triage- Type 1 contact- Detox- Children- Symptomatic
X-rayReport?
Request abnormal X-ray report
All documents received
Yes
No
Hold unmatched
Enter Radiology
report
No
Yes
X-ray or CD?
X-ray
Check CD- name- report
CD
Onsite or Offsite
Pull previous record
Request offsite record
Enter into iPHISCheck iPHIS for previous
recordX-ray or CD?
Radiologist Review
X-ray
Review by Dr. Elwood
Yes
No
Yes
Normal / Abnormal
File X-ray
939 & Normal report
939
939 & abnormal X-ray
Normal
Abnormal
CD
Batch CDs, read in Reading room
Normal / Abnornal
Dictation
Check “No Evidence” Box
Normal
Abnormal
Separate Field Ops & Vancouver
X-rays
File copy return
Normal / Abnormal
939 & Tape
Transcribe into iPHIS
Enter “No Evidence” into
iPHIS
Normal
Abnormal
Dictated 939sSend Referral in
iPHISGenerate
Validation Sheet
Enter treatment required into iPHIS
Outbox to Pharmacy
Enter end date into iPHIS
Send pick & yellow copies to Health
Units
Outstanding referrals iPHIS
Previous Files?Request
Discharge Summary
Proof narratives
Discard extra copies
Create small envelop &
withdraw card
File 939
Validate printed report
Upd?Update iPHIS report
Print narratives
Yes
Print upd report
Separate- health units-physicians
Pre-addressed, pre-stamped
envelop Mail
Withdraw envelop & mail
CDMatch CD &
939
To VGH for Radiology
Radiologist review
Date stamp upon arrival
Enter Radiology report into
iPHIS
To Dr. Elwood for
review
More dictations?
File CDFile 939Initial
comments
No
Yes
© Provincial Health Services Authority
How does it differ from patient journey mapping?• Focus is on patient experience and how care is received.• Visualizes complexity of patient journey.• Identifies touch points in the patient care.
© Provincial Health Services Authority
Building the Current State VSM
1. Customer and quantifiable customer requirements
2. Supplier or Inputs
3. Processes
4. Data
5. Communication and Information Flow
6. Timeline and Summary with Value Stream Metrics
© Provincial Health Services Authority
Building the Current State
1. Who is your customer and what are some quantifiable customer requirements?
The customer is the recipient of the output or the outcome of your value stream.
The customer defines value delivered by the value stream.
Examples: • Total Length of Stay• Delays• % Complete and Accurate• Rework• Sentinel or safety events
© Provincial Health Services Authority
Building the Current State
Define the Basic Processes
• Start and finish• Altitude
© Provincial Health Services Authority
Building the Current State
Add Data Boxes
• Cycle time for each process• Amount of time between processes• # of People / Hours• Input Requirements (% Complete and Accurate)• Output Requirements (% Complete and Accurate)
© Provincial Health Services Authority
Building the Current State
• Add the communication flows to and from the process to external resources and back.
• Add a summary timeline to show the total amount of work time (value added or necessary work) and delay time (non-value added work).
© Provincial Health Services Authority
Value
Compare the customer requirements to value stream performance:
• Are you meeting requirements?• Length of Stay• Clinic Appointment Time• Value-added service (no delays or waiting)
• Are you meeting quality requirements?• Complete Discharge Plan• Medication Reconciliation• Quality Rounds
© Provincial Health Services Authority
Flow
Review unnecessary delays.
• Clear triggers for subsequent steps.• Rework• Excessive handoffs• Interruptions• Requirements for decisions and approvals• Duplication of work
© Provincial Health Services Authority
Work
Review how quality and safety are built into each process.
• Standards governing each process (no standards, unclear standards, incorrect standards).
• Passing work on with checkpoints for completeness and accuracy.
© Provincial Health Services Authority
Future State
Vision of a future state
- Set Value Stream Goals- Reduction of Time = increased throughput, increased
efficiencies, - Reduction of Time by elimination or reduction of waste.- Reduction of Defects
© Provincial Health Services Authority
Bridge from Current to Future
• Kaizen Ideas• Focus:
• Value• Flow• Work
• Set your improvement agenda• Manage your improvement agenda and set a clear line
of site from your improvement to your goals.• Establish and manage an action plan.• Revisit the value stream (after each improvement and
annually)
© Provincial Health Services Authority
Value Streams in Practice
Common Issues• Team Capacity (3 day exercise)• Data (current and ongoing monitoring)• Long process value streams (i.e. mental health)• Sponsorship (ownership)• Alignment of VSM goals with department/agency/health
authority/MoH goals
© Provincial Health Services Authority
Home to Home Journey of the NH Patient through Tertiary Cardiac Services
© Provincial Health Services Authority
• 95% of these patients travel to Vancouver for diagnosis and treatment.
• There is a delay in transferring these patients to get access to a higher level of care.
• There is often a delay in transferring these patients back home.
• Care must be coordinated across three health authorities.
• The improvements in this value stream potentially have a broader application to all rural remote cardiac patients.
• Support provided by Shared Care & Specialist Services Committees’ Health Authority Redesign Funding
Why this patient group?
© Provincial Health Services Authority
Building Current State
Customer: • Northern health urgent ACS patient.
Customer Requirements: • Timely access to a higher level of care.• No delay in transfer.• Coordinated communication and transfer of information.• Timely return to home community.
© Provincial Health Services Authority
Building Current State
Interviews
ObservationsHEARTis Data
69 Interviews in 5 health authorities and BCEHS
Triage CoordinatorsDaily Triage CallUtilization MeetingsNorthern Health Processes• Time to Referral Acceptance• Time to Transfer
# Cath Referrals/Site# PCI/Surgery/Site
• Add Data and Metrics:
© Provincial Health Services Authority
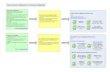
Bridge to Future State
Limitations and Challenges• Scoping and Focus not clear enough to fully define
future state and set clear value stream goals.• Limited authority to make changes within health
authorities.• Tight timeline: November to March• Large group with varied experience with value stream
mapping process.
© Provincial Health Services Authority
Bridge to Future State
1 2 3 1 2 3 1 2 3
Northern Health Northern HealthCardiac SiteBEHS
© Provincial Health Services Authority
Improvement Agenda
Change in Value Stream Purpose1. Standardize the referral form. In order to:
•Decrease the time between “time of referral” and “acceptance date”;•Eliminate overproduction by triage coordinators (multiple phone calls);•Decrease the % of incomplete referrals
2. Standardize the patient journey information and education.
In order to:•Decrease the time between “date of intervention” and “time of discharge”;•Decrease the # of patients “unprepared” for discharge.
3. Standardize the referral process with the Patient Transfer Network .
In order to:•Decrease the time between “time of referral” and “time of transfer”;•Reduce rework and overproduction by the triage coordinators;
© Provincial Health Services Authority
• Planes, trains and snowmobiles…understanding how our Province can work better together
• January 2014 a provincial project team was identified
• Team met weekly by teleconference to get to know one another and to identify the focus of the during the Improvement Workshop - April 29-May 1
Patient Discharge Planning WorkshopApril 29 – May 1
© Provincial Health Services Authority
Outcomes
Primary Outcome:Reduce the time between intervention to discharge from 8.5 days to 6 days.
Process Outcome:Patients arrive “prepared” at a cardiac site.
© Provincial Health Services Authority
Problem Statement 1
Length of stay in cardiac site increases due to amount of patient preparation required for discharge at the cardiac site for a safe return home.
Hypothesis: A “prepared” patient upon entering the cardiac site will have a shorter length of stay.
© Provincial Health Services Authority
Solutions
1. Standardized Northern Health Checklist and Patient Preparation Package.
2. Standardized Northern Health Cardiac Patient Transfer Plan that involves patient, family and provider to prepare for transfer to cardiac site.
© Provincial Health Services Authority
Pilot Trial – NH Cardiac Patient Transfer
• Standard packages - pilot project from July to September 2014:– Prince George– Vanderhoof– Terrace– Dawson Creek
• All 5 Cardiac Sites participated in pilot project and collected tracking form when patient arrives. – Patients are prepared when arriving to cardiac site.
• Continuing to monitor primary outcome with CSBC:– Reduction of time between intervention and discharge.
© Provincial Health Services Authority
Project Team - What did we learn?
• Given the opportunity – you can improve provincial processes collaboratively.
• Greater understanding of the size, complexity and challenges faced by Northern Health.
• Greater communication about expectations between health authorities across patient journey.
• Clarity of how to develop and improve provincial forms (who owns them and who is accountable?)
• Understanding of the work that was happening in other health authorities on our shared patient populations.
• Difficulty in finding standard measurements and language across province.
© Provincial Health Services Authority
Working better Together
• Listen to understand verses Listen to respond
• What were the ingredients that contributed to our team working successfully as a high functioning team in such a short period of time…
• The team listened to understand one another and the various barriers and frustrations that were both unique to each HA and collectively as a larger health care system
• The individual triage co coordinators shared the lengths they went to get people home who had arrived in Vancouver with no clothes, shoes, ID or money
© Provincial Health Services Authority
Understanding the Geography
• What contributed to understanding the barriers that each Health Authority was experiencing was the time we gathered around the NH map
• Stories, experiences and understanding the NH Connections bus routes provided context to why patients had difficulty in getting home and why we as a group had to come up with a way to have patients return safely home with the travelling required in the North…planes, trains and snowmobiles!
• NH is 2/3 of the province we have less population than the lower mainland but our geography is far reaching with barriers to access in the remote areas such as Fort Ware and other remote communities.
• Its actually easier to get to Puerto Vallarta than it is to get a patient home from Vancouver to Terrace
© Provincial Health Services Authority
Next Steps
• Pilot project results were presented to the NH Cardiac and Cerebrovascular Services Working Group in October 2014 o request a next step for working towards an NH Regional process beyond the Pilot sites.
• Make this package standard for all of Northern Health
© Provincial Health Services Authority
Value Stream Mapping as a Provincial Tool• The ‘home to home’ patient value stream allows a
system focus to anchor problem solving.
• Creating time for frontline staff to design and trial processes that cross health authorities is proving efficient and beneficial to “get the work done.”
• Standardization and collection of data and processes across health authorities is a challenge.
• Sponsorship at each health authority is crucial for sustainment of improvements at this level.
Related Documents