Traumatic Brain Traumatic Brain Injury: Injury: Challenging Challenging Behavior Behavior Anastasia Edmonston MS CRC TBI Projects Director Maryland Traumatic Brain Injury Project MD Mental Hygiene Administration

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Traumatic Brain Injury:Traumatic Brain Injury: Challenging BehaviorChallenging Behavior
Anastasia Edmonston MS CRCTBI Projects Director
Maryland Traumatic Brain Injury ProjectMD Mental Hygiene Administration

What We will Cover Today
• Brain Anatomy-form and function
• Brain Injury-how many & who is affected
• Types of Brain Injury

What We will Cover Today
• The Physical, Cognitive and Emotional/Behavioral Aftermath of Brain Injury
• TBI Screening Tool• Brain Injury and Co-occurring
disorders

What We will Cover Today
• Strategies for Supporting Individuals with Brain Injuries
• Resources Available Statewide, Regionally and Nationally

Skull AnatomyThe skull is a rounded layer of bone designed to protect the brain from penetrating injuries.
The base of the skull is rough, with many bony protuberances.
These ridges can result in injury to the temporal and frontal lobes of the brain during rapid acceleration.
Bony ridges

Skull Anatomy
Injury to frontal lobe from contact with the skull

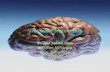
Lobes of the Cerebrum
Frontal lobe
Parietallobe
Occipitallobe
TemporalLobe
LimbicLobe

The Frontal LobeThe frontal lobe is the area of the brain responsible for our “executive skills” - higher cognitive functions.
These include:
• Problem solving• Spontaneity• Memory• Language• Motivation• Judgment• Impulse control• Social and sexual behavior.

Frontal Lobe InjuryThe frontal lobe of the brain can be injured from direct impact on the front of the head.
During impact, the brain tissue is accelerated forward into the bony skull. This can cause bruising of the brain tissue and tearing of blood vessels.
Frontal lobe injuries can cause changes in personality, as well as many different kinds of disturbances in cognition and memory.

Prefrontal CortexThe prefrontal cortex is involved with intellect, complex learning, and personality.
Injuries to the frontal lobe can cause mental and personality changes.

The Developing Brain
• Children’s brains do not reach their adult weight of 3 pounds until they are 12 years old
• The brain, and most importantly, the brain’s frontal lobe region does not reach it’s full cognitive maturity till individuals reach their mid twenties

The Developing Brain
• The Frontal Lobe houses our executive skills, these include; judgement, problem solving, mental flexibility, etc.
• The Frontal Lobe is very vulnerable to injury
• Damage to the Frontal Lobe any where along the developmental continuum can impact executive skill functioning

Temporal LobeThe temporal lobe plays a role in emotions, and is also responsible for smelling, tasting, perception, memory, understanding music, aggressiveness, and sexual behavior.
The temporal lobe also contains the language area of the brain.

Temporal Lobe InjuryThe temporal lobe of the brain is vulnerable to injury from impacts of the front of the head.
The temporal lobe lies upon the bony ridges of the inside of the skull, and rapid acceleration can cause the brain tissue to smash into the bone, causing tissue damage or bleeding.

Parietal LobeThe parietal lobe plays a role in our sensations of touch, smell, and taste. It also processes sensory and spatial awareness, and is a key component in eye-hand co-ordination and arm movement.
The parietal lobe also contains a specialized area called Wernicke’s area that is responsible for matching written words with the sound of spoken speech.

Side Impact Injuries May Impact the Parietal Lobe
Injuries to the right or left side of the brain can occur from injuries to the side of the head.
Injuries to this part of the brain can result in language or speech difficulties, and sensory or motor problems.

Occipital Lobe
The occipital lobe is at the rear of the brain and controls vision and recognition.

Occipital Lobe DamageOccipital lobe injuries occur from blows to the back of the head.
This can cause bruising of the brain tissue and tearing of blood vessels.
These injuries can result in vision problems or even blindness.

The Limbic SystemThe limbic system is the area of the brain that regulates emotion and memory. It directly connects the lower and higher brain functions.

Coup-Contra Coup InjuryA French phrase that describes bruises that occur at two sites in the brain.
When the head is struck, the impact causes the brain to bump the opposite side of the skull. Damage occurs at the area of impact and on the opposite side of the brain.

Diffuse Axonal Injury
Brain injury does not require a direct head impact. During rapid acceleration of the head, some parts of the brain can move separately from other parts. This type of motion creates shear forces that can destroy axons necessary for brain functioning.
These shear forces can stretch the nerve bundles of the brain.

Diffuse Axon Injury is a very serious injury, as it directly impacts
the major pathways of the brain.

The Neuron
Dendrites:Collects information from other neurons
Cell Body
Axon:Transmits information to other neurons.

Definitions• Traumatic Brain Injury is an insult to the
brain caused by an external physical force• Diffuse Axonal Injury the tearing and
shearing of microscopic brain cells• Acquired Brain Injury is an insult to the
brain that has occurred after birth, for example; TBI, stroke, near suffocation, infections in the brain, anoxia

Incidence of TBI CDC 2004
In the United States, at least
1.4 million sustain a TBI each year(That we know about)

What are the Costs of TBI? CDC 2006
Direct medical costs and indirect costs such as lost productivity of
TBI totaled an estimated 60 billion in the United States in 2000. (That is
equal to the cost of building the international space center or 60
times the net worth of Oprah Winfrey )Jean Langlois of the CDC

About 3.17 Million American civilians (more than 1.1% of
population, live with the consequences of traumatic
brain injuryCDC in Journal of Head Trauma
Rehabilitation 2008 (Vol. 23, No. 6, pp 394-400)

What Might it Feel Like
Handwriting&
Processing Exercise

Incidence of TBI CDC 2004Of those 1.4 million..
• 51,000 die;• 290,000 are hospitalized; and • 1,224,000 million are treated
an released from an emergency department

““Reframed, the numbers Reframed, the numbers nauseate. In America alone, nauseate. In America alone,
so many people become so many people become permanently disabled from a permanently disabled from a brain injury that each decade brain injury that each decade they could fill a city the size of they could fill a city the size of
Detroit……...Detroit……...

……..Seven of these cities are Seven of these cities are filled already. A third of their filled already. A third of their citizens are under fourteen citizens are under fourteen
years of age.”years of age.”
From Head Cases, Stories of Brain Injury and its Aftermath
Michael Paul Mason2008 published by Farrar, Straus and Giroux

Brain Injury and Children
• According to the BIAA, Brain Injury is the leading cause of death and disability among children
• Approximately 470,000 TBI’s occur among children 0-14 years old a year
• Brain injuries account for over 90% of emergency department visits in children 0-14 years old CDC Report “Traumatic Brain injury in the United States January 2006

Brain Injury and Concussionin Children
• In sports alone, 300,000 + concussions are “estimated” to occur annually
• For every 1 concussion in the NFL, there are 5,650 youth injuries
• Sports associated with concussion: soccer, football, lacrosse, hockey, horseback riding, cheerleading…….. Gerard Gioia, Ph.D., Children’s National Medical Center in remarks at the BIAMD conference 2005

Other potential Neurotoxins that may impact the brain
• Exposure to lead paint• Regarding exposure to alcohol in utero,
according to Dr. Jacobson of Wayne State University “We found more serious cognitive impairment in relation to alcohol than cocaine or other drugs, including marijuana and smoking” From “Fetal Brains Suffer Badly From Effects of Alcohol” NYT 11.4.03

To UnderscoreThe Developing Brain
• Children’s brains do not reach their adult weight of 3 pounds until they are 12 years old
• The brain, and most importantly, the brain’s frontal lobe region does not reach it’s full cognitive maturity till individuals reach their mid twenties

This is important to keep in mind because…..
The Adult Consumer you are serving in your program may have
suffered a brain injury as a child

Causes of TBI CDC 2006
Falls, 28%
Motor Vehicle-Traffic, 20%
Struck By/Against, 19%
Assault, 11%
Unknown, 9%
Other, 7%
Pedal Cycle (non MV), 3%
Suicide, 1%
Other Transport, 2%

Who is at the Highest Risk of TBI? 2005
• Males 1.5 times as likely as females to sustain a TBI
• Two age groups most at risk are 0-4 year olds and 15-19 year olds
• The elderly, 75 and older from falls• African Americans have the highest
death rate from TBI

What about those with unidentified TBI?
Adapted from MCHB webcast, Wayne Gordan, Ph.D 5.21.08
• 425,000 people treated by MDs in office visits Langlois 2004
• 90,000 treated in other types of outpatient settings Langlois, 2004
• Uncounted injuries on the playground, on the playing fields, from falls in the home, assaults, domestic violence, returning veterans, etc. etc. etc…...

The Scope of the Problem
• Distribution of Severity:
– Mild injuries = 80%(LOC < 30 min, PTA ,1 hour)
– Moderate = 10 - 13%(LOC 30 min-24 hours, PTA 1-24 hours)
– Severe = 7 - 10%(LOC >24 hours, PTA >24 hours)

The Importance of Post Traumatic Amnesia
PTA is the period of time after injury when a
person is unable to lay down new memories…
for example

“That first morning, wow, I didn’t want to move, I was thankful that nothing’s
broken, but my brain was all scrambled” Ryan Church, NYT 3/10/08
“All he remembers from the collision with Anderson is the
aftermath, being helped off the field by two people, although he said he did not know who they were until he saw a photograph
later” Ben Shpigel NYT reporter

The Faces of Brain Injury
A short video by the Brain Injury Association of Florida

Possible Changes-Physical• Motor skills/Balance• Hearing• Vision• Spasticity/Tremors• Speech• Fatigue/Weakness• Seizures• Taste/Smell

Possible Changes-Thinking• Memory• Attention• Concentration• Processing• Aphasia/receptive
and expressive language
• Executive skills• Problem solving• Organization• Self-Perception• Perception• Inflexibility• Persistence

Possible Changes-Personality and Behavioral
• Depression• Social skills problems• Mood swings• Problems with emotional control• Inappropriate behavior• Inability to inhibit remarks• Inability to recognize social cues

Personality and Behavioral cont..
• Problems with initiation• Reduced self-esteem• Difficulty relating to others• Difficulty maintaining relationships• Difficulty forming new relationships• Stress/anxiety/frustration and reduced
frustration tolerance

A memory deficit might look like trouble remembering or it might
look like…… (Capuco & Freeman-Woolpert)
• She frequently misses appointments-avoidance, irresponsibility (for example...)
• He says he’ll do something but doesn’t get around to it (for example...)
• She talks about the same thing or asks the same question over and over-annoying perservation
• He invents plausible sounding answers so you won’t know he doesn’t remember (for example…)

An attention deficit might look like trouble paying attention or
it might look like …(Capuco & Freeman-Woolpert)
• He keeps changing the subject• She doesn’t complete tasks• He has a million things going on and
none of them ever gets completed (for example…)
• When she tries to do two things at once she gets confused and upset

A deficit in executive skills might look like the inability to plan and organize or it might look like...
(Capuco & Freeman-Woolpert)
• Uncooperativeness, stubbornness
• Lack of follow through• Laziness• Irresponsibility

Unawareness might look like… (Capuco & Freeman-Woolpert)
• Insensitivity, rudeness• Overconfidence• Seems unconcerned about the extent of her
problems• Doesn’t think she needs supports• Covering up problems (“everything’s fine…”)• Big difference in what he thinks and what everyone
else thinks about his behavior• Blaming others for problems, making excuses

Lack of AwarenessA common and difficult to remediate
hallmark of a brain injury

Levels of AwarenessCrossen et.al (1989) J Head Trauma Rehabilitation
• Intellectual Awareness-individual is able to understand at some level, that a particular function or functions is impaired. A greater level of intellectual awareness is required to recognize some common thread in the activities in which they have difficulty
• Emergent Awareness-individual is able to recognize a problem when it is actually happening. To do so, they must recognize a problem exists (intellectual awareness), and realize when it occurs
• Anticipatory Awareness-individual is able to anticipate a problem will occur and plan for the use of a particular strategy or compensation that will reduce the chances that a problem will occur, e.g. keep and refer to a calendar to support memory for daily schedule

The Relationship Between Brain Injury and Mental
Health

Depression• Depression is the most common Axis I
psychiatric disorder after TBI followed by alcohol abuse, panic disorder, specific phobia and psychotic disorders (Gordon et. al 2004)
• A 50 yr.. Follow-up of 1,198 WWII vets found that 520 had incurred a TBI. 18.5% of vets with brain injuries had a life time prevalence of major depression verses 13.4% rate of depression among on brain injured vets (Holsinger et.al 2002)

The Post -Concussive Syndrome and PTSD Dr. Paul McClelland
• Increased startle response; especially to loud sounds
• Irritability• Avoidance of many social events• Intolerance of new situations

Organic Personality Disorder & Anti-Social or Hysterical Personality Traits Dr. Paul McClelland
• Decreased impulse control• Labile and superficial affect• Impaired insight and self awareness• Decreased empathy and social
awareness• Impaired initiative (Depression?)

Partial Seizures & Panic Attacks or Dissociative States
Dr. Paul McClelland
• Most common type of post-traumatic epilepsy• Temporal lobe damage and complex partial
seizures• “Spells” starting suddenly & lasting a few
minutes• Olfactory (smell) or gustatory (taste)
hallucinations• Déjà vu or jamais vu• Micropsia, macropsia and other symptoms

Obsessive-Compulsive Traits after TBI: Pre-Existing Conditions or Adaptation to
Cognitive Deficits & Other Changes? Dr. Paul McClelland
• Compulsive behaviors as adaptations for memory loss
• Temper tantrums and other adaptations• Non-pharmacological management of
brain-injured patients

Other Mental Health Disorders Related to TBI
• PTSD is noted in some individuals following TBI even if there is no memory of the incidence (Klein, Caspi 2003)
• Rapid cycling bipolar is rare but noted in the literature for individuals with temporal lobe damage (Murai, Fujimoto 2003)
• Psychotic syndromes occur more frequently in individuals who have had a TBI then in the general population (McAllister, Ferrell 2002)

TBI & Suicide• “The risk of attempted or completed suicide in
neurological illness is strongly related to depression, feelings of hopelessness or helplessness, and social isolation” (Arciniegas & Anderson, 2002)
• Simpson and Tate (2002) screened 172 individuals for suicidal ideation and hopelessness. Findings using the Beck Suicide Ideation and Hopelessness Scales found 35%felt hopeless and 23%expressed suicide ideation. 18% had attempted suicide post injury

Individuals with or without a history of brain injury often share identical risk factors for suicide
Teasdale & Engberg 2001
• Young Adults• Males• Substance Abuse• Other psychosocial
disadvantages

Teasdale & Engberg’s population study of 145,440 Danes post TBI:• Followed individuals with concussion, skull fractures
and cerebral contusions or traumatic intracranial hemorrhages (lesions) for 15 years
• Incidence of suicide among all three groups higher compared to general population
• Presence of a co-occurring substance abuse diagnosis increased suicide rates among all three groups
• Significantly greater risk for suicide found among those with lesions than those with concussion or fracture
• Rate of suicide was 1% over a 15 year period

Subsequent Studies…..Simpson & Tate
• A 2003 study found of 172 individuals post TBI, 17%attempted suicide over a period of 5 years
• A 2005 study of 172 individuals with a hx of brain injury found that those with comorbid post injury history of psychiatric/emotional disturbance and substance abuse were 21 times more likely to attempt suicide post injury

Why Screen?
What other TBI Screening efforts have found

2000 Epidemiological Study of Mild TBI J. Silver of NYU, cited in WSJ by Thomas
Burton 1.29.08 http://online.wsj.com/article/SB120156672297223803.html?
mod=googlenews_
• 5,000 interviewed • 7.2% recalled a blow to the head
w/unconsciousness or period of confusion
• Follow up testing found; 2x rate of depression, drug and alcohol abuse
• Elevated rates of panic and and obsessive-compulsive DO

Brain Injury in the Correctional Setting-Nationally CDC website 2008
• According to jail and prison studies,25-87% of inmates report having experienced a TBI-this compared with 8.5% of the general population
• Prisoners with a history of TBI may also experience mental health disorders (including; severe depression, anxiety, substance abuse)

Brain Injury in the Correctional Setting-Nationally
CDC website 2008
• Woman inmates who are convicted of a violent crime are more likely to have sustained a pre-crime TBI or some other form of physical abuse
• Women with substance abuse disorders have an increased risk for TBI compared with women in the general population

In Maryland- Screening Results from the MD TBI Post Demo II
Project-2005– Summary of TBI Incidence Among all Screened at 7
public mental health agencies in Frederick and Anne Arundel counties
– N=190– 39% no reported history of TBI (78)– 58.94% of individuals with a history of TBI (112)– 35.78% of individuals with a history of a single incidence of
TBI (68)– 23% of individuals with a history of 2 or more TBIs (44)

Details-County Detention Center 2005
– N=41– Single TBI= 16– 2 or more incidents of TBI= 14– No history of TBI= 11– 73% screened reported a history of TBI

County Detention Center 2008
– N=25 (16 male, 9 female)– 22 reported possible TBI(s)– Single TBI=10– 2 or more incidents of TBI= 12– No History of TBI =3– 88% screened reported a history of TBI

TBI in a County Jail Population
Slaughter et. al Brain Injury 2003
• 69 randomly selected inmates• 60 (87%) reported TBI over their lifetime• 25 (36%) reported TBI in the prior year• Later group had worse anger and
aggression scores, trend towards poorer cognitive test results and higher prevalence of psychiatric DO then those w/out TBI in prior year

Brain Injury in the Correctional Setting-Nationally
CDC website 2008
• According to jail and prison studies,25-87% of inmates report having experienced a TBI-this compared with 8.5% of the general population
• Prisoners with a history of TBI may also experience mental health disorders (including; severe depression, anxiety, substance abuse)

Brain Injury in the Correctional Setting-Nationally
CDC website 2008
• Woman inmates who are convicted of a violent crime are more likely to have sustained a pre-crime TBI or some other form of physical abuse
• Women with substance abuse disorders have an increased risk for TBI compared with women in the general population

Brain Injury & ViolenceDomestic Violence
• Greater than 90% of all injuries secondary to domestic violence occur to the head, neck or face region (Monahan & O’Leary 1999) Adapted from The Alabama Department of Rehabilitation Services DV Training
• Corrigan et.al., (2003) found that of 167 individuals treated for domestic violence related health issues, 30% experienced a loss of consciousness on at least one occasion, 67% reported residual problems that were potentially TBI related
• Valera and Berenbaum, (2003) assessed 99 battered women. Of these, 57 had brain injured related symptomatology

Homelessness & Brain InjuryA little studied population,
however…..• A University of Miami study found that 80% of 60
homeless individuals had high incidence of neuropsychological impairment
• Researchers in Milwaukee found possible cognitive impairment in 80% of 90 homeless men evaluated.
• Dr. LaVecchia of the MA Statewide Head Injury Program reported in 2006 that of 140 homeless individuals evaluated, 83.6% of males and 16.4% of females had an acquired brain injury
• Other studies in the UK and Australia show similar rates of brain injury among homeless individuals

Correlation between TBI & Homelessness
Hwang et.al 10.7.08 Canadian Medical Journal
• 904 homeless individuals surveyed• Lifetime Prevalence of TBI-53%, more
common among men than women surveyed
• Rates 5 or more times greater than the 8.5% lifetime prevalence in general population and consistent w/ prison studies

TBI & Homelessness“For Veterans, A Weekend Pass From Homelessness”from the New York Times 7.26.09, Erick Eckholm
Human service professionals will be seeing increasing numbers of returning service members in need of services over the next few years

“….The ranks include young men like Kenneth Kunce, 26, who suffered a traumatic brain injury when his Humvee was hit by a roadside bomb in Iraq. The injury left him disorientated, jumpy and temperamental. When he came home he started using Ecstasy and alcohol, he said he
lost his wife and more than one job. He said he was grateful to the Veterans Affairs hospital for
providing speech and physical therapy, but added that he still had trouble coping with
noises and anger.Mr. Kunce, who sometimes lost his train of
thought as he spoke to this reporter, is living out of his car.”

The HELPS Brain Injury Screening Tool
(see handout)
The original HELPS tool developed by M. Picard, D. Scarisbrick, R. Paluck, 9.1991
Updated by the Michigan Department of Community Health

HELPS• Have you ever Hit your Head or
been Hit on the Head?• Prompt individual to think about;
TBI at any age, MVAs. Assaults, Sports injuries, Service related injuries, Shaken baby and/or adult

HELPS• Were you ever seen in the
Emergency room, hospital, or by a doctor because of an injury to your head?
• Explore the possibility of “unidentified traumatic brain injury” many do not present in medical settings

HELPS• Did you ever Lose consciousness or
experience a period of being dazed and confused because of an injury to your head?
• Remember, a LOC isn’t required for someone to develop symptoms subsequent to a blow to the head. “alteration of consciousness” AKA post traumatic amnesia (PTA). At this point, the interviewer may consider asking the individual if they have had multiple mild TBI

HELPS• Do you experience any of these Problems in
your daily life since you hit your head?• You want to know when any problems began
(or began to be noticed) Remember, lack of awareness is a hallmark of brain injury, you might ask if anyone close to the individual has made any observations regarding changes in function.

HELPS• Headaches• Dizziness• Anxiety• Depression• Difficulty
concentrating• Difficulty
remembering
• Difficulty reading, writing, calculating
• Poor problem solving• Difficulty performing
your job/school work• poor judgement (being
fired from job, arrests, fights, relationships affected)

HELPS• Any significant Sickness?• Acquired Brain Injury (ABI) can result in many
of the same functional impairments as traumatic brain injury (TBI). For example, brain tumor, meningitis, West Nile virus, stroke, seizures, toxic shock syndrome, aneurysm, AV malformation, any history of anoxic injury, e.g. heart attack, near drowning, carbon monoxide poisoning can all result in multiple deficits

Scoring the HELPS Positive for a possible Brain Injury when the
following three are identified:• An event the could have caused a brain injury
(YES to H, E, or S), and• A period of loss of consciousness or altered
consciousness after the injury or another indication that the injury was severe (YES to L or E), and
• the presence of 2 or more chronic problems listed under P that were not present before the injury.

Scoring the HELPS• A positive screening is not sufficient to diagnose TBI
as the reason for current symptoms and difficulties-other possible possible reasons need to be ruled out
• Some individuals could present exceptions to the screening results, such as people who do have TBI-related problems but answered “no” to some questions
• Consider positive responses within the context of the person’s self-report and documentation of altered behavioral and/or cognitive functioning

Additional comments and observations of the interviewer• Any visible scars?• Walks with a limp?• Uses a cane or walker?• Has a foot brace?• Limited use of one hand?• Appears to have difficulty focusing vision?• Difficulty answering questions?• Answers are unorganized and/or rambling• Becomes easily distracted, agitated or is
emotionally labile

What you are looking for…..And Why
• Any reported or suspected functional difficulties that are interfering with home, work or community activities
• With the identification a history of brain injury, professionals can better support the individuals served and make informed referrals to brain injury specialists when appropriate

Remember, for most, Brain Injury is:
• -A loss of Self• -A loss of future• -loss of possibilities

“I had a job, I had a girl, I had something going mister
in this world…………”
A 10 year survivor of a TBI quoting a Bruce Springsteen
song when describing what he had lost because of his injury

A compromised brain can lead to compromised behavior,
further adding to social isolation and social failure
The following slides 3 are adapted from Webcast:
sponsored by the Health Resources and Services Administration’s
Federal TBI Program Web castJuly 27, 2006

Speakers:• Harvey E. Jacobs, Ph.D., Licensed
Clinical Psychologist/Behavioral Anaylist• Marty McMorrow, Director of National
Business Dev., The MENTOR Network• Jane Hudson, JD., senior Staff Attorney,
National Disability Rights Network

Behavioral Statistics
• Approximately 90% of all people who experience severe disability following brain injury experience some emotional or psychiatric distress
• 40% continue to demonstrate behavioral difficulty five years post injury

Behavioral Statistics
• 25% experience behavior dysfunction that interferes with other activities of daily life
• 3%-10% experience severe behavioral dysfunction that may require intensive professional and residential intervention (~3,000-9,000 new people per year)

Research findings regarding Behavior Problems after TBI• “Aggressive behavior is associated
with presence of major depression, frontal lobe lesions, poor premorbid social functioning and a history of alcohol and substance abuse” Tateno et.al J of Neuropsychiatry Clin. Neuroscience 2003

Research findings regarding Behavior Problems after TBI• Research conducted by Wood and Liossi in
2006 reports “it is tentatively suggested that significant impairment in verbal memory and visuospatial abilities against a background of diminished executive-attention functioning is associated with the development of aggression after brain injury,especially when other risk factor such as low premorbid IQ, low socioeconomic status, and male gender are present” J of Neuropsychiatry Clin. Neuroscience

Research findings regarding Behavior Problems after TBI• “Impairments in recognizing the
emotional state of others may underlie some of the problems in social relationships that these patients experience……TBI patients were found to be impaired on emotional recognition compared to the control patients both early after injury and one year later” Ietswaart et. al. Neuropsychologia, 2007

According to McMorrow, Jacobs and Hudson; HRSA
Webcast July 27, 2006 “Almost all people who experience
disability following brain injury are not inherently aggressive or assaultive. However, for some people, when
challenges are not properly addressed this can result in…”

-Lack of responsiveness to requests-Property destruction-Verbal or physical aggression-Violation of personal or sexual boundaries-Wandering or flight-Self harm/self abuse/suicide

“Neurobehavioral Challenges” According to McMorrow, Jacobs and Hudson
are caused by: • Pre-injury history• Post-Injury learning and experiences• Inability to negotiate “difficult” situations• Others’ not recognizing the basic
challenges to an individual with TBI, and• Not providing proper treatment

With the Proper Supports:
• -A renewed sense of self• -A future can be imagined• -New possibilities can be
created

Strategies

Attention is the ability to stay focused on a specific topic or task. It is critical to successful participation in
purposeful activity.
The next 10 slides are from the Rhode Island BIA presentation “Brain Injury: A
Practical Training for Caregivers”

Attention Gain and encourage eye contact when
appropriate. Use an opening statement such as “Are you
ready to get started” to gain the consumer’s attention before explaining an activity or giving directions.
Be specific and clear. Avoid lengthy or vague explanations.
Slow down when you speak. It is very difficult to listen carefully to someone who is talking at a fast pace.
Limit interruptions when possible.

Attention Minimize environmental distractions
(competitive background noise, cluttered work areas and cluttered walls).
Present information in an organized fashion.
Pause to allow the consumer to process or to finish taking notes before moving to the next direction or to a new piece of information.

Attention Encourage a steady work pace. Rushing can
result in an increase in mistakes or in skipping an important step in an activity.
Breakdown assignments into smaller more manageable portions.
Provide a task breakdown or assist the consumer in developing a task breakdown for specific activities

Attention Avoid overwhelming the consumer. Don’t plan
on covering large amounts of information in a single session.
When assigning tasks that the consumer will be expected to complete independently, begin with simple activities. Progress to more difficult or complicated tasks if the consumer is successful with the simple activities.

Attention If you notice that the consumer is beginning to lose
focus, give a cue to redirect to task, or ask if they need a short break.
Provide positive feedback when the individual is performing well or requesting to use appropriate modifications or strategies during a session.
When finishing an instructional session, help the consumer to review the material that was covered. Place emphasis on any follow up activities the consumer is supposed to complete independently.

AttentionTo pay attention, we must be awake and alert, this is referred to as arousal level. Under normal circumstances our central nervous system automatically keeps the
arousal level regulated. As a result of brain injury clients may experience lethargy or
sluggishness referred to as a state of under arousal. Or they may appear to be ‘hyper’ or
over stimulated known as a state of over arousal. In some cases the use of sensory
stimulation, relaxation or focusing techniques can be helpful. Responses to sensory input
can vary from person to person.

Attention Use an appropriate volume and tone of voice for the
individual consumer. A softer voice may be more tolerable to someone who is over stimulated. A louder voice with extra emphasis on key words may be helpful to someone who is under aroused.
Determine if the use of white noise or environmental sound machines is helpful.
Use high intensity white light or bright natural light for individuals who are under aroused, dimmed lighting for those who are over aroused.

Attention Play background music that the individual
finds helpful when paying attention to a particular activity, or for relaxation (soft soothing music, upbeat or rhythmic music).
Include breaks into the daily schedule to listen to short guided meditation or relaxation tapes.
Pause between activities or during lengthy activities to take a few deep breaths.

Attention Movement such as gentle use of a rocking
chair, or brisk movement can help to regulate arousal.
Joint and muscle stimulation experienced during weight bearing or resistive exercises can also assist with regulation of arousal.
Encourage participation in a regular exercise program or activity such as Yoga or Tai Chi when appropriate.

The Benefits of Exercise Post Injury
TBI Consumer Report # 2 TBI Central MT. Sinai Model Program
• Those who exercise had fewer physical, emotional and cognitive complaints. E.g. sleep problems, irritability, forgetting and being disorganized
• Non-exercisers complained of more cognitive problems or symptoms than those who exercise
• Exercisers with TBI were less depressed• Exercisers viewed themselves as healthier• Exercisers were often engaged in school, work, and “got
around” the community more freely• Exercisers had more severe brain injuries than the non-
exercisers, suggesting that a severe injury does not prevent engaging in exercise

Memory functions are complicated and sensitive. Memory is frequently
the first function to be notably impaired and one of the last
functions to be regained in the recovery process.
The next 32 slides are adapted from the Rhode Island BIA
presentation “Brain Injury: A Practical Training for
Caregivers”

MemoryMemory Systems can significantly improve client follow through and
independence when used on a regular basis. When a new system is
introduced a ‘repetitive training’ and cueing period is recommended to
reinforce consistent use. Systems can be updated to accommodate for improvements in memory, or for
changing needs.

Memory• When designing a memory system: Define the goals or exact needs the system will be
meeting. Designate separate sections based on specific
needs. Use a format and style that the individual prefers. Encourage use of one system that is taken
everywhere. (technology!) See Tony Gentry, Ph.D. OTR/L’s website: www.vcu.edu/partnership/pda/Jobcoach

Memory Timers, wrist watch alarms or talking watches
can provide prompts.
Use check off sheets (this allows the individual to self-monitor and reference back).
Post simple reminder signs for prompts to turn off appliances, lights, etc.
Label drawers and cupboard fronts indicating their contents.

Memory Post step by step directions for appliances
such as the coffee maker, microwave etc. Post-it notes for extra reminders, for example
place a post it note on the memory book as a reminder to check the ‘to do’ list if there is a critical item on the schedule the next day.
Provide written or picture based instructions in addition to verbal instructions.

Memory Color code folders, storage containers, or calendar
entries to help with recall and identification. Use tape recorders to record meetings or
appointments. Provide repetitive training or instruction when
reintroducing functional activities into the daily schedule, and with all activities that require new learning.
Encourage note taking at meetings, appointments, etc.

Memory Pocket “Voice it” recorders can be used to
record reminders throughout the day.
Use the home answering machine to leave “reminders to self”.
Have a back up plan. For instance, in addition to strategies for remembering keys, have a contingency plan with extra keys available at accessible locations (neighbors, friends, etc.)

Problem SolvingProblem solving is used for completion of a wide range of activities throughout the day.
Many activities are sequenced; performed by using a step by step approach. Cues can
support consumer participation in activities Written or picture task breakdowns can be used during early training or as a prop for
independent task completion as the consumer progresses.
Strategies and approaches can also be developed to help consumers with higher level
or abstract problem solving skills.

Problem Solving/Sequencing example
• Squat Pivot Transfer • 1)Park- at an angle along the mat, left front of the
wheelchair touching the mat.• 2)Lock both wheels• 3)Check your locks• 4)Flip up left arm rest• 4)Scoot your bottom forward• 5)Feet flat on the floor 8 -10 inches apart, left foot
forward• 6)Hands- Left hand on the mat, Right hand on the
chair arm• 7)Push on arms, lift up bottom, pivot onto the mat

Problem SolvingState Problem:_________________________List 3 solutions: 1)_____________________
2)_____________________
3)_____________________
Solution 1 Solution 2 Solution 3
Pros Cons Pros Cons Pros Cons
Describe the most logical and effective solution based on the
above:________________________________ _____________________________________

Impulsivity
Impulsivity is often a consequence of injury to the frontal lobes.
Impulsivity can have a negative impact on independent living, particularly
when life changing decisions are made without carefully thinking things
through.

ImpulsivityChange Plan
What change do I want to make?____________________Why do I want to make the change?_________________
Change Not Changing Pros Cons Pros Cons
List step for
change:1)________________2)______________3)________________4)________________5)___________
___
Who could help me?_________________________________What might interfere with my change?
___________________How would I evaluate success?
_______________________

InitiationPoor initiation, a decreased ability to initiate or begin activities, can be a
consequence of brain injury. Initiation deficits are often misinterpreted,
caregivers may assume the consumer doesn’t care or that they aren’t
motivated. Damage to any one of several different areas of the anterior
part of the brain can result in deficits in this area.

Initiation Many individuals respond well to structure and
consistent routines. When preparing daily and weekly schedules be
specific. Designate specific times for activities to be performed. In addition to using a general concept such as clean-up the kitchen, indicate specific tasks for example: put dishes in the dishwasher, wipe off the table, wash the counter.
Begin with lighter demands that promote success. The difficulty of demands can be increased when the consumer demonstrates consistent follow through with the easier activities.

Initiation Encourage consumer participation when
developing schedules. Provide training and cues when introducing a
new or updated schedule. Accept close approximations of the desired
behavior when changes are initially instituted. Use positive reinforcement for all successful
follow through. Engage the consumer in a problem solving
approach when addressing areas of difficulty.

Communication
Communication is very complex and involves processing of both verbal and nonverbal information. Individuals may
have receptive deficits, difficulty understanding specific words or with
the way in which words are presented. They may have expressive deficits,
difficulty remembering a word, or with pronouncing words correctly when
speaking

Communication Receptive Deficits:
• Slow your rate of speech
• Simplify sentence structure, be clear and concise
• Pause between sentences or topics to allow for processing
• Repeat key words or concepts
• Rephrase as needed
• Summarize information frequently

Communication
Expressive Deficits: Do not expect an immediate response to a question or
statement. Pause to allow the individual time to prepare their response.
• Accept gestures and pantomime in addition to verbal speech.
• Ask yes/no questions, avoid questions that require lengthy or detailed answers.
• Provide extra time for consumers who are using augmentative communication devices.
• Accept written answers or drawings.

Hearing/Central Auditory Processing
When there is trauma to the temporal lobe area, individuals may experience a change in the ability to hear sound or in the ability to process auditory (sound) input. Once sound is detected by the ear, the brain processes what was heard on multiple levels. Individuals with central auditory processing deficits may have difficulty with:
Filtering out competitive background noise Noticing the differences between similar sounds or
words Maintaining attention on a speaker who is giving a
presentation on complicated information or when listening to a long presentation.
Remembering information as it is processed.

Hearing/Central Auditory Processing
Reduce or eliminate background noise. Instruct the client to directly face the speaker to
maximize on visual speech cues. Increase the volume of the speaker’s voice in relation
to the surrounding background noise at presentations or meetings. Provide a speaker microphone or assisted listening device.
Speakers should avoid covering their mouth, shouting or over-enunciating words.
Consider referring for an audiological evaluation to determine if hearing aides or specialized alerting devices would be beneficial.

Vision Vision is an extremely important source of sensory information. The eyes send many
messages to the brain, the brain must interpret all of the incoming messages. There can be problems with coordinated movements
of the eyes and/or with the brains ability to process and interpret information accurately. Deficits can range from mild to severe. Even subtle deficits can affect the individuals ability
to work on visual tasks and should be addressed.

Vision Use enlarged print. Print on yellow instead of white paper or use a yellow
acetate overlay on documents to increase contrast. A book mark or ruler can be used to help with staying
on the line when reading or scanning for information. Change florescent lights to high intensity white lights,
or increase natural light. Simplify forms; determine if extra spacing, grid lines,
bold print or bold lines are helpful.

Vision Use a cut out guide to isolate sentences or words. When consumers are working on near vision tasks
for long periods, have them take short breaks to shift their gaze to distant objects to decrease eye fatigue.
Refer to a vision care professional trained in working with acquired brain injury for thorough assessment of vision related complaints.
Refer for adaptive technology assessment for computer modification or low vision technology when appropriate.

Activity ToleranceFatigue is a common complaint after brain injury. It is more difficult for individuals with brain injury to compensate for their deficits
when they are over tired.Consumers may need more sleep than they did before they were injured. They may not
be able to tolerate a very busy schedule. It is important to consider energy conservation
and work simplification when preparing daily and weekly schedules.
In some cases they may have sleep disturbances; the physician should be
consulted if a consumer is unable to get to sleep or stay asleep during the appropriate
hours.

Activity ToleranceWhen developing a plan to manage fatigue:Carefully review the current schedule with
the consumer.Make a list of the most important activities, those that must be done on a daily or weekly basis, and plug them into the new schedule (Some activities may need to be eliminated
when revising a schedule).Schedule activities that are more difficult or
demanding throughout the week. Don’t schedule all heavy or difficult activities on a
single day.

Activity ToleranceAlternate between light or low demand activities and high demand more difficult
activities on the daily schedule.
Determine if there are certain times during the day that the consumer is at his or her ‘best’ try to schedule important or priority
activities at those times.
Determine what times of the day the consumer is usually more fatigued, schedule
only light activities or rest periods during these times.

Activity Tolerance Encourage consumers to increase their use of
accommodations and strategies or provide extra supports during the times of day that they are usually more fatigued.
Avoid rushing, schedule enough time for each activity to be performed at a steady and reasonable pace.
Remember that cognitive activities can be very tiring for some consumers. You will need to observe how each individual responds to different activities.

Considerations for Plan Development
Each plan must be developed on a case by case basis to meet the individuals needs.
Always include the client in development of the plan when possible.
Each consumer may present with a wide variety of strengths and challenges.
Individuals may have deficits in multiple areas. Because a consumer does do well in some areas
does not mean they should automatically be expected to do well in all areas.

Considerations for Plan Development
Limitations in each deficit area may require specific accommodations.
Some deficits may not be obvious when your first meet the consumer.
Recovery can vary greatly from individual to individual. Consumers may need extra support to realize they can’t compare their recovery with that of other brain injury survivors.
Because recovery can continue for some time the plan may need to be changed and updated on a regular basis to meet the consumer’s changing needs.

Additional Considerations It is important that consumer is motivated to work on
the goals that have been developed. Always consider the consumer’s input when developing
goals. If the team has developed goals that are different from
the consumer’s, be sure to explain what the purpose and potential value of working on those goals might be. Discuss how the goals developed by the team may compliment or support the consumer’s personal short and long term goals.
Keep the discussion focused on identifying goals and activities that offer the opportunity for success.

Potential Disruptive BehaviorsNot all brain injury survivors will experience difficulty with social
behavior. However, TBI survivors who have had severe frontal lobe injury or who have been more recently injured may exhibit disruptive behaviors. You
may observe:
•Social judgment errors •Threatening comments
•Inappropriate sexual comments or advances

Potential Disruptive BehaviorsIn most cases these behaviors are not intentional but rather the result
of poor inhibition and judgment. These behaviors, although
upsetting are not usually meant to be harmful, and can be addressed
by using a consistent team approach.

The next 10 slides are adapted from the New
Hampshire Project Response presentation “Changes After Brain
Injury”

Environmental Triggers for Behavioral Problems
• Too much stimulation• Rapid pacing• Lack of predictability and clear structure• Overwhelming physical and cognitive
demands• Negative social input

Note: if you manage the environment, you can
prevent many problems

Guidelines For Behavior Management
• Increase rest time. Fatigue is a common problem.
• People have limited coping skills. Reduce stress.

Guidelines For Behavior Management
• Keep the environment simple. People with brain injuries are easily overstimulated
• Decrease interruptions and distractions• Be consistent• Decrease surprises

Guidelines For Behavior Management
• Keep instructions simple, concrete.• If the person has problems processing
language, try gesturing or cueing.• Write things down.

Guidelines For Behavior Management
• Give feedback and set goals• Feedback should be direct, caring,
nonjudgmental, but not subtle• Avoid criticism• Give supportive encouragement• Have a positive attitude • Use the “feedback” sandwich

Guidelines For Behavior Management
• Be calm, cool, and friendly during an incident• This can reduce agitation• Avoids reinforcing misbehavior• Redirection works. When the person is upset,
agitated, aggressive, focus attention on some other topic, task, person.
• Provide choices

Guidelines For Behavior Management
• Decrease chance of failure• Keep success rate above 80%• Watch for frustration• Behavioral momentum• Expect the unexpected. People with brain injuries can
have great variability from day to day. Mood swings are common. People with TBI are sensitive to changes, disruptions in routine, lack of sleep, alcohol, minor illnesses, fatigue, other stressors.

KEEP IN MIND…
Progress can be inconsistent and unpredictable
• What works today may not work tomorrow, but may work the following day
– Reduced stamina and fatigue may persist– Impairment of memory may hinder new
learning– Transitions may be especially difficult

Prevention, Prevention, Prevention
• Communicate expectations• Recognize internal and environmental
triggers, plan strategies• Provide clear structure and predictable
routines• Maintain realistic expectations• Help peers learn to alter interactions to
avoid triggers

Additional Strategies
From the MD TBI Project

Most Strategies address more than one cognitive and or behavioral deficit

Strategies
Spontaneous restoration of functioning occurs most rapidly and dramatically in
the first year following a brain injury.Generally speaking, the greater the
time from the injury the more rehabilitation efforts will focus on
compensation

Environmental &
Internal Aides
Creative cognitive strategies will employ both kinds of aids depending
on individual need

Environmental, AKA Prosthetic external memory strategies and
devicesChanging or modifying the
environment to support and/or compensate for a injury imposed
deficitFor Example: labeling kitchen
cabinets

InternalThe strategy is “in your head”
For Example:“I have to work the memory
muscle by counting everything, like how many times I pedal when
I am on a bike”Actor George Clooney discussing the use of internal memory strategies in The
London Sunday Times10. 23.05

Oftentimes a strategy can transition with practice from the external to the internal
For Example:Preparing remarks on paper with “pauses” written in to slow down impulsive speech can eventually segue into a internal strategy, “At the end of every 2-3 sentences, I
will take a breath and check in with my listener”

Strategies can help individuals compensate for
the physical barriers imposed by a brain injury
For Example:Prism glasses may be prescribed
to address double vision after injury just as bifocals are
prescribed for many after age 40

Strategies• Use of a template for routine tasks, on the job,
at home• Use of a high lighter (RED)• Use of ear plugs to increase attention, screen
out distractions (Parente & Herman 1996)• Partitions/cubicles, at work, quiet space at
home• Model tasks e.g. turning on a computer and
accessing email

Strategies• Use of pictures, for faces/names, basic
information, for step-by-step procedures, e.g. making coffee
• Use of a timer, to track breaks at work, the time minimum technique, allocated time to puzzle over a problem or vent a frustration
• Books on tape, movies, keep the subtitles (for processing content in the case of memory and comprehension problems and increase awareness of nonverbal cues/communication)

Strategies• Car Finder-low tech, install a longer radio
antenna with a day-glow flag, high tech, Design Tech International by DAK Corp.
• Electronic pill boxes/blister packs with day of the week labels
• Review schedule each day• Post signs on the wall etc. (use
pictures/symbols for low literacy skills)• Try to “routinize” the day as much as possible

Teach a variety of strategies for individuals to incorporate into their
daily routines Michelle Rabinowitz OTR/L
• Safety checklist (e.g. for use of stove)reinforces attention
• Checklists- “things to do before leaving the house” (turn off all the appliances?, lock all the doors?, did I take my morning medications? turn down the heat/turn off the air conditioner?, do I have money or keys?, where am I going?, how will I get there? What time should I leave? Etc.) Very good for routine tasks, reinforces memory
• Place visual cues in the environment (cupboard labels, written directions, calendars, list of emergency phone numbers) reinforces memory

Memory StrategiesAdapted from:
Parente & Herman in Retraining Cognition 1996 Aspen Publishers

SOLVE Mnemonic
• “S” (S)pecify the problem• “O” (O)options-what are they?• “L” (L)isten to advice from others• “V” (V)ary the solution• “E” (E)valuate the effect of the
solution, did it solve the problem?

Organizing the EnvironmentConsistency, accessibility, separation,
grouping, proximity• Consistency-put things in the same place, keys,
wallet etc.• Accessibility-things that are commonly used, keep
them physically close, in the kitchen, in the office• Separation-put things in logically distinct locations.
Clothes, mail• Grouping-put things that are used together in the
same area, raincoat & umbrella• Proximity-cooking utensils near the stove

Setting GOALS Executive Skills Training
• G” (G)o over your goals every day-helps memory and awareness
• “O” (O)rder your goals-short and long term• “A” (A)sk yourself two questions each day:
“what did I do today to achieve my goals?” and “What could I have done differently to achieve my goals”
• “L” (L)ook at your goals each day. Post goals and progress on the wall, refrigerator etc.

Listening Skills• “L” (L)ook at the person-focus on
nonverbal aspects of communication• “I” (I)nterest yourself in the
conversation- use “social fillers” e.g “I see”, “Tell me more”
• “S”(S)peak less than half the time-decrease the chance of getting off topic

Listening Skills continued
• “T” (T)ry not to interrupt or change the topic-stick to the topic at hand
• “E” (E)valuate what is being said. Question the content, do not blindly accept what is being said
• “N” (N)otice body language and facial expression-train this skill via use of pictures or scenes from movies, TV

Try these techniques in groups or as focus of individual sessions.
During groups utilize a peer feedback component

More Thoughts on Listening Skills
• An area where reduced cognitive skills can be misinterpreted as poor interpersonal skills
• No one likes a “noisy listener”• Poor listening skills can be impacted by
anxiety (about memory, social skills etc.)• Relaxation techniques can be helpful (breath
in slowly over 7 breaths, hold for 4-7 counts, exhale over 7, repeat as necessary)

Strategies for Injury Imposed Barriers
Watch this scene from the 2007 Movie The Lookout
What are the character’s barriers?
What are the strategies he is using to compensate?

Brain Injury the Long Term Consequences
Follow the injury and recovery of Iraq veteran, “Toggle”, a character in the
Doonesbury comic strip. Gary Trudeau accurately depicts blast injury, living with motor, visual, and speech and language deficits (especially aphasia) and PTSD as
Toggle picks up his life post injury.
http://www.doonesbury.com/strip/dailydose/
http://www.doonesbury.com/strip/dailydose/

References• Slides 3-21 adapted from Dr. Mary Pepping of the University of
Idaho’s presentation The Human Brain: Anatomy,Functions, and Injury
• Corrigan JD. (1995). Substance Abuse as a Mediating Factor in Outcome from Traumatic Brain Injury. Archives of Physical Medicine and Rehabilitation Vol. 76, April: 302-309
• Bombardier, CH., Temkin, NR., Machamer, J., Dikmen SS.(2003), The Natural History of Drinking and Alcohol-Related Problems After Traumatic Brain Injury Archives of Physical Medicine and Rehabilitation Feb;84(2):185-91.
• Bombardier C., Davis, C. (2001). Screening for Alcohol Problems Among Persons with TBI. Brain Injury Source. Fall 16-19.
• Corrigan J., et. al (1998) Utilities for Community Professionals. Ohio Valley Center for Brain Injury Prevention and Rehabilitation

Resource Coordination in Maryland
• Charlotte Wisner, Resource Coordinator for Frederick & Washington Counties, call 301-682-6017
• Lauren Dorsey, Resource Coordinator for Baltimore & Howard Counties, call 301-529-1508
• Catherine Reinhart Mello, Resource Coordinator for Montgomery County, call 301-586-0900
• Any questions regarding resource coordinator or free training on brain injury related topics, call Anastasia Edmonston, Project Director 410-402-8478

RESOURCES• Brain Injury Association of America 703-236-
6000, www.biausa.org• Brain Injury Association of Maryland 410-448-
2924, www.biamd.org• Ohio Valley Center For Brain Injury Prevention
and Rehabilitation, 614-293-3802, www.ohiovalley.org. Excellent SA TX resource & information
• www.headinjury.com. Good resource for memory aides and tips

The Michigan Department of Community Health
Web-Based Brain Injury Training for Professionals
www.mitbitraining.orgThis free training consists of 4 module that
take an estimated 30 minutes each to complete. The purpose of the training is
twofold, to “ensure service providers understand the range of outcomes” following
brain injury and to “improve the ability of service providers to identify and deliver
appropriate services for persons with TBI”

ResourcesThe University of Alabama Traumatic Brain Injury
Model System has created the UAB Home Stimulation Program. This program offers many activities for use by individuals with brain injuries, their families and
the professionals who work with them. The activities are designed to help support cognitive skills and can be done in the home setting. The Home Stimulation
Program can be accessed from the Internet at htt://main.uab.edu/show.asp?durki=49377. For
further information contact: Research Services, Dept. of Physical Medicine and Rehabilitation, University of
Alabama at Birmingham, 619 19th St. S SRC 529, Birmingham, AL 35249-7330/ 206-934-3283.

ResourcesRehabilitation Research and Training
Center on Traumatic Brain Injury Interventions & New York Traumatic
Brain Injury Model System at the Mount Sinai School of Medicine and
the Mount Sinai Rehabilitation Research and Training Center
www.mssm.edu/tbinet

Recommended Reading
• I am the Central Park Jogger: A Story of Hope and Possibility by Trisha Meili, 2003
• Every Good Boy Does Fine: A Novel by Tim Laskowski, 2003
• Over My Head: A Doctor’s Own Story of Head Injury from the Inside Looking Out by Claudia Osborn, 2000

A Product of the Maryland TBI Partnership Implementation Project, a collaborative effort
between the Maryland Mental Hygiene Administration, the Mental Health
Management Agency of Frederick County and the Howard
County Mental Health Authority2006-2009
Support is provided in part by project H21MC06759 from the Maternal and Child Health Bureau (title V, Social
Security Act), Health Resources and Services Administration, Department of Health and Human Service
This is in the public domain. Please use and distribute widely.
Related Documents