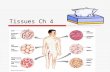
Tissues and Histology • Tissues - collections of similar cells with same embryonic origin performing a similar function

Tissues and Histology Tissues - collections of similar cells with same embryonic origin performing a similar function.
Jan 11, 2016
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Tissues and Histology
• Tissues - collections of similar cells with same embryonic origin performing a similar function


Tissues and Histology
• Tissues - collections of similar cells with same embryonic origin performing a function
• Tissue classification based on structure of cells, composition of noncellular extracellular matrix, and cell function
• Major types of adult tissues
– Epithelial
– Connective
– Muscle
– Nervous
• Histology: Microscopic Study of Tissues
– Biopsy: removal of tissues for diagnostic purposes
– Autopsy: examination of organs of a dead body to determine cause of death

I. Epithelial Tissue• Cellularity - Consists almost
entirely of cells• Covers body surfaces, lines
hollow organs, and forms glands– Outside surface of the body– Lining of digestive, respiratory
and urogenital systems– Heart and blood vessels– Linings of many body cavities
• Polarity - Has apical, basal, and lateral surfaces
• Rests on a basement membrane• Specialized cell contacts bind
adjacent cells together• Avascular - no blood vessels• Regenerative -Replaces lost cells
by cell division

Functions of Epithelia
• Protecting underlying structures; e.g., epithelium lining the mouth
• Acting as barriers; e.g., skin• Permitting the passage of substances; e.g.,
cells lining air sacs in lungs and nephrons in kidney
• Secreting substances; e.g., pancreatic cells• Absorbing substances; e.g., lining of stomach
and small intestine

Special Characteristics of Epithelia
Figure 4.1

Classification of Epithelium
• Number of layers of cells– Simple- one layer of cells. Each extends from
basement membrane to the free surface– Stratified- more than one layer. – Pseudostratified- tissue appears to be stratified,
but all cells contact basement membrane so it is in fact simple
• Shape of cells– Squamous- flat, scale-like– Cuboidal- about equal in height and width– Columnar- taller than wide

Classifications of Epithelia


Simple Squamous Epithelium
Figure 4.3a

Simple Cuboidal Epithelium
Figure 4.3b

Simple Columnar Epithelium
Figure 4.3c

Pseudostratified Ciliated Columnar Epithelium
Figure 4.3d

Stratified Epithelia
• Contain two or more layers of cells
• Regenerate from below
• Major role is protection
• Are named according to the shape of cells at apical layer

Stratified Squamous Epithelium
• Description– Many layers of cells – squamous in shape– Deeper layers of cells appear cuboidal or
columnar – Thickest epithelial tissue – adapted for
protection

Stratified Squamous Epithelium
• Specific types – Keratinized – contain the protective protein
keratin• Surface cells are dead and full of keratin
– Non-keratinized – forms moist lining of body openings

Stratified Squamous Epithelium
• Function – Protects underlying tissues in areas subject to abrasion
• Location – Keratinized – forms epidermis– Non-keratinized – forms lining of
esophagus, mouth, and vagina

Stratified Squamous Epithelium
Figure 4.3e

Transitional Epithelium
Figure 4.3h

Epithelium: Glandular
• A gland is one or more cells that makes and secretes an aqueous fluid
• Two types of glands formed by infolding of epithelium: – Endocrine: no contact with exterior of body; ductless; produce
hormones (pituitary, thyroid, adrenals, pancreas)– Exocrine: open to exterior of body via ducts (sweat, oil)
• Exocrine glands classified either by structure or by the method of secretion
• Classified by structure– Unicellular: goblet cells– Multicellular: sweat, oil, pituitary, adrenal

Multicellular Exocrine Glands• Classified on the basis of types of
ducts or mode of secretion• Types of ducts
– Simple: ducts with few branches
– Compound: ducts with many branches
• If ducts end in tubules or sac-like structures: acini. Pancreas
• If ducts end in simple sacs: alveoli. Lungs

Lateral Surface Features
• Tight junctions
• Desmosomes
• Gap junctions

Membrane Junctions: Tight Junction
• Integral proteins of adjacent cells fuse together• Completely encircle the cell and form an adhesion belt.• Form an impermeable junction.• Common near apical region

Lateral Surface Features – Cell Junctions
• Desmosomes – two disc-like plaques connected across intercellular space– Plaques of adjoining cells are joined by
proteins called cadherins – Proteins interdigitate into extracellular
space– Intermediate filaments insert into plaques
from cytoplasmic side

Membrane Junctions: Desmosome
Figure 3.5b
Linker proteins extend from plaque like teeth of a zipper.Intermediate filaments extend across width of cell.
• Common in superficial layers of skin; skin peels after a sunburn • Reduces chance of tearing, twisting, stretching

Membrane Junctions: Gap Junction
• Connexon proteins are trans- membrane proteins.• Present in electrically excitable tissues (heart, smooth muscle)

Basal Feature: The Basal Lamina
Noncellular supporting sheet between the epithelium and the connective tissue deep to it
Consists of proteins secreted by the epithelial cells
Functions: Acts as a selective filter, determining which
molecules from capillaries enter the epithelium Acts as scaffolding along which regenerating
epithelial cells can migrate
Basal lamina and reticular layers of the underlying connective tissue deep to it form the basement membrane

Epithelial cells
Basal lamina
Collagen fibers

Epithelial Surface Features
• Apical surface features – Microvilli – finger-like extensions of plasma
membrane• Abundant in epithelia of small intestine and kidney• Maximize surface area across which small
molecules enter or leave
– Cilia – whip-like, highly motile extensions of apical surface membranes
• Movement of cilia – in coordinated waves

Connective Tissue

Connective Tissue• Most diverse and abundant tissue• Main classes
– Connective tissue proper
– Cartilage
– Bone tissue
– Blood
• Characteristics– Vascular
– Nonliving extracellular matrix, consisting of ground substance and fibers
– Cells are not abundant as in epithelium

Connective Tissue: Embryonic Origin
Figure 4.5


Functions of Connective Tissue
• Enclose organs as a capsule and separate organs into layers - Areolar
• Connect tissues to one another - Tendons and ligaments.
• Support and movement - Bones• Storage and Insulation - Fat• Transport - Blood• Protection - Bone, cells of the immune
system

Structural Elements of Connective Tissue
• Ground substance – unstructured material that fills the space between cells
• Fibers – collagen– elastic– reticular
• Cells – fibroblasts– chondroblasts– osteoblasts– hematopoietic stem cells, and others

Connective Tissue Cells• Fibroblasts - secrete the proteins needed for fiber
synthesis and components of the extracellular matrix• Adipose or fat cells (adipocytes). Common in some
tissues (dermis of skin); rare in some (cartilage)• Mast cells. Common beneath membranes; along small
blood vessels. Can release enzymes in response to injury.• Leukocytes (WBC’s). Respond to injury or infection• Macrophages - Phagocytic; provide protection• Chondroblasts - form cartilage• Osteoblasts - form bone• Hematopoietic stem cells - form blood cells

Extracellular Matrix - ECM• ECM has 3 major components
1. Protein fibers 2. Ground substance 3. Fluid
• Protein fibers– Collagen fibers. Made of protein collagen. Strong,
flexible, inelastic; great tensile strength (i.e. resist stretch). Perfect for tendons, ligaments
– Elastic fibers. Made of protein elastin that resemble coiled springs. Found in lungs, large blood vessels
– Reticular fibers. Made from fine collagenous fibers; fill spaces between tissues and organs.

Ground Substance• Interstitial fluid within which are one or more of
the molecules listed below:– Hyaluronic acid: a polysaccharide. Very
slippery; serves as a good lubricant for joints. – Proteoglycans: protein and polysaccharide
complex. Able to trap large amounts of water.– Adhesive molecules: hold proteoglycan
aggregates together. • Functions as a molecular sieve through which
nutrients diffuse between blood capillaries and cells

Areolar Connective Tissue
Figure 4.12b

Adipose Tissue
Figure 4.12c

Reticular Connective Tissue
Figure 4.12d

Dense Irregular Connective Tissue
Figure 4.12e

Dense Regular Connective Tissue
Figure 4.12f

Connective Tissue: Cartilage• Composed of chondrocytes (cells) located in
matrix-surrounded spaces called lacunae. • Type of cartilage determined by components of
the matrix. • Firm consistency. • Ground substance: Proteoglycans and hyaluronic
acid complexed together trap large amounts of water (microscopic sponges). Allows tissue to spring back after being compressed.
• Avascular and no nerve supply. Heals slowly.Types of cartilage
– Hyaline– Fibrocartilage– Elastic

Hyaline Cartilage
Figure 4.12g

Elastic Cartilage
Figure 4.12h

Fibrocartilage
Figure 4.12i

Tissues and Aging• Cells divide more slowly • Collagen fibers become more irregular in structure, though
they may increase in number– Tendons and ligaments become less flexible and more fragile
• Elastic fibers fragment, bind to calcium ions, and become less elastic– Arterial walls and elastic ligaments become less elastic
• Changes in collagen and elastin result in – Atherosclerosis and reduced blood supply to tissues– Wrinkling of the skin– Increased tendency for bones to break
• Rate of blood cell synthesis declines in the elderly• Injuries don’t heal as readily


Bone Tissue
Figure 4.12j

Blood Tissue
Figure 4.12k

Muscle Tissue• Characteristics
– Cells are referred to as fibers– Contracts or shortens with force when
stimulated– Moves entire body and pumps blood
• Types– Skeletal:attached to bones– Cardiac: muscle of the heart. – Smooth: muscle associated with tubular
structures and with the skin. Nonstriated and involuntary.

Skeletal Muscle Tissue
Figure 4.14a

Cardiac Muscle Tissue
Figure 4.14b

Smooth Muscle Tissue
Figure 4.14c

Nervous Tissue
Figure 4.15

Tissues and Aging• Cells divide more slowly • Collagen fibers become more irregular in structure, though
they may increase in number– Tendons and ligaments become less flexible and more fragile
• Elastic fibers fragment, bind to calcium ions, and become less elastic– Arterial walls and elastic ligaments become less elastic
• Changes in collagen and elastin result in – Atherosclerosis and reduced blood supply to tissues– Wrinkling of the skin– Increased tendency for bones to break
• Rate of blood cell synthesis declines in the elderly• Injuries don’t heal as readily
Related Documents