THE KIDNEY, EXCRETION AND OSMOREGULATION BIOSYSTEMS MAINTENANCE – BIO242

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

THE KIDNEY, EXCRETION AND
OSMOREGULATION
BIOSYSTEMS MAINTENANCE – BIO242

TO KNOW
Important to differentiate between
Excretion, Secretion, and Egestion

EXCRETION & OSMOREGULATION EXCRETION- is the process of removing metabolic wastes
EXCRETION - maintains homeostasis by regulating the
chemistry of body fluids and maintaining body temperature.
EGESTION (DEFECATION) – is the removal of undigested
food from the gut and is not regarded as excretion because
the material taken into the gut through the mouth is not
made by the body itself.

EXCRETION & OSMOREGULATION
SECRETION – usually involves the
release of useful substances such as
hormones from cells.
A few waste products are secreted into
the kidney tubules during excretion.

NAME THE EXCRETORY STRUCTURES IN ORGANISMS
CAN ANYONE

EXCRETORY STRUCTURES
As an organism increase in complexity,
excretory organs develop to remove
excretory products from the body and
pass them to the external environment

EXCRETORY STRUCTURES Cell surface membrane Malpighian tubules AND Trachea Kidney Liver – formation of urea from excess
amino acids Lungs – only excretory organ for carbon
dioxide Skin – responsible for heat loss, water,
urea & salts

What are the common Excretory Products?
STUDENTS

EXCRETORY PRODUCTS
NITROGENOUS COMPOUNDS
OXYGEN
CARBON DIOXIDE
BILE PIGMENTS

OSMOREGULATION
Is the maintenance of constant osmotic
conditions in the body. It involves
regulation of the water content and solute
concentration of body fluids, particularly of
sodium, potassium and chloride ions.
(chapter 20 – pg 672)

EXCRETION & OSMOREGULATION
The metabolic activities of living
organisms result in the production of
waste materials

FUNCTIONAL SYSTEMS
food, water intake oxygen intake
elimination of carbon dioxide
Digestive System Respiratory System
Circulatory SystemUrinary System
elimination of excess watersalts, wastes
rapid transportto and from allliving cells
eliminationof foodresidues
nutrients,water,salts
carbondioxide
watersolutes
oxygen
Based on: Starr, C., Biology: Concepts and Applications, Brooks/Cole

AN EXCRETORY SYSTEM
WHY DO WE NEED

SIGNIFICANCE
Removal of unwanted by-products of metabolic pathways -
Removal of toxic wastes Regulation of ionic concentration of
body fluids Regulation of water content of body
fluids Regulation of pH

5.1 NITROGENOUS WASTE AND THE
FORMATION OF UREA
THE KIDNEY, EXCRETION AND OSMOREGULATION

WHERE DO THE NITROGENOUS WASTE
COME FROM?HOW DO WE GET RID OF IT?
STUDENTS

UREA FORMATION
DEAMINATION DETOXIFICATION

NITROGENOUS WASTE
Nitrogenous wastes products – produced by the
breakdown of proteins, nucleic acids and excess
amino acids.
The first products of the breakdown of excess amino
acids is ammonia (deamination)
nitrogenous wastes vary from the extremely toxic
ammonia to less toxic urea and the non-toxic uric
acid.
Pg 674

When protein is broken down in the body, it results in nitrogenous waste that must be eliminated from the body

Based on: Mader, S., Inquiry Into Life, McGraw-Hill
Protein

All 20 amino acids have a nitrogen group (NH2). When broken down for energy, the nitrogen group is converted to ammonia (NH3).
Examples of Amino Acids
Based on: Mader, S., Inquiry Into Life, McGraw-Hill

Ammonia is converted into urea by the liver. Urea is then transported in the blood to the kidneys where the urea is removed from the blood.
Circulatory System
Based on: Mader, S., Inquiry Into Life

Urea is less toxic than ammonia and can be transported in the blood to the kidney
H2N - C - NH2
urea
O

FORMATION OF URINEAmino acids in protein are broken down,
resulting in production of ammonia
Ammonia is converted to urea in liver
Urea travels in blood to kidneys, where removed from blood and incorporated
into urine

FORMATION OF URINE
INVOLVES 3 KEY PROCESSES
1. Ultrafiltration
2. Selective absorption
3. Secretion

THE KIDNEY
THE MAJOR EXCRETORY AND OSMOREGULATORY ORGAN

FUNCTIONS
Removal of metabolic waste
Regulation of water content of body
fluids
Regulation of pH of body fluids
Regulation of chemical composition

NAME THE STRUCTURES OF
THE KIDNEY
IMPORTANT TO KNOW THE LOCATION AND ALSO


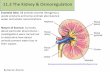
THE KIDNEY The kidneys are located within the muscular wall of
the middle back (just below the ribcage). The kidney receives blood from the aorta via the
renal arteries The renal veins returns blood to the posterior vena
cava The kidneys are the site of urine formation. The urine formed in the two kidney then travels
down the two ureters towards the urinary bladder where it is stored.
Urine exits the body by way of the single urethra.

Anatomy of the Kidney
Based on: Mader, S., Inquiry Into Life, McGraw-Hill


Structures of the Kidney Shows distinctly the cortex and medulla Cortex – covered by fibrous connective tissue
(capsule) Cortex contains the glomeruli, renal corpuscles,
and part of the nephron Medulla – contains tubular parts of the nephron
and blood vessels, which together form the renal pyramids
Pappilla – is the apex of each pyramid All pyramids projects into the pelvis which leads
into the ureter

Urinary System
Based on: Mader, S., Inquiry Into Life, McGraw-Hill

NEPHRONS
Two types
Cortical – short loops of Henle which just extends into the medullary
Deals with control of blood volume (under normal conditions of
water availability)
Juxtamedullary – have their renal corpuscles close to the junction of
the cortex and medulla
Have long loops of Henle
When water is short increase water retention occurs in the
juxtamedullary nephron


STRUCTURES OF THE NEPHRON
FUNCTION &


Each KIDNEY consists of 1 million NEPHRONS
Each nephron consists of a:GLOMERULUS (found in cortex)
forms a protein-free filtrate from bloodTUBULE (found in medulla)
processes the filtrate to form urine
Each TUBULE consists of several segments:Proximal tubuleLoop of HenleDistal Tubule
Collecting Ducts.


RENAL CORPUSCLES
GLOMERULUS RENAL CAPSULE (PODOCYTES –
CELLS WHICH ARE MODIFIED FOR FILTRATION) – 20% OF PLASMA IS FILTERED INTO THE CAPSULE
AFFERENT ARTERIOLE (TO) EFFERENT ARTERIOLE (FROM) FIRST STEP OF URINE FORMATION -
ULTRAFILTRATION

GLOMERULUS
Knot of capillaries, specially adapted for filtration
Diameter of the capillaries is far less than that of the arterioles, so as the blood enters the narrow capillaries pressure rises
Water and small solutes are squeezed out of the capillaries through the epithelium of the renal capsule and into the interior of the capsule

ULTRAFILTRATION Takes place through three layers
1. Endothelium of the blood capillary – very thin and perforated with thousands of pores.
2. Basement membrane of the blood capillaries (main filtration barrier) – red blood cells, platelets, and proteins are too large to pass
3. Epithelium of the renal capsule (made up of podocytes and filtration slits - foot like projection that are highly modified for filtration)
The filtered fluid in the capsule is called glomerular filtrate (GF)
GF – has a chemical composition similar to blood plasma. It contains glucose, amino acids, vitamins, ions, nitrogenous waste, some hormones and water

FACTORS AFFECTING THE GLOMERULAR FILTRATION RATE (GFR)
Hydrostatic pressure of the blood and the pressure of the glomerular filtrate
Solute potential (flow from afferent to efferent results in an increase in concentration of 20%)
Filtration rate can be increased by raising blood pressure
Dilating (vasodilation) of the afferent arteriole – reduces resistance to the flow of blood into the glomerulus
Increase resistance in the efferent arteriole by vasoconstriction

REABSORPTION (PROXIMAL CONVOLUTED TUBULE) Ultrafiltration 125cm3 per min 180 dm3 per day 1.5 dm3 of urine is produce a day 124cm3 is reabsorbed 80% of it is absorbed in the proximal
convoluted tubule Nephron selectively reabsorbs substances
for further use by the body Further waste substances maybe added by
secretion

Urine Formation by Nephron
Blood pressure forces water, glucose, amino acids and urea from capillaries into nephron
Glucose and amino acids are reabsorbed into blood from nephron
Some water is reabsorbed into blood
Urine is urea and salt concentrated in water

Nephron
Based on: Mader, S., Inquiry Into Life, McGraw-Hill


ANALYSIS OF FLUID IN THE NEPHRON By using small pipettes we can remove
fluids from different parts of the nephron and analyze its content to find out what effect the different part of the nephron have on the composition of fluid
Use of Inulin (not to be confused with Insulin) – Inulin fiber is a carbohydrate belonging to a class of compounds known as fructans. used as a tracer

ANALYSIS OF FLUID IN THE NEPHRON It is injected to the blood, where it’s filtered
into the nephron So as water is reabsorbed the concentration
of Inulin increases in proportion to the amount of water reabsorbed
Because Inulin fiber is resistant to digestion in the upper gastrointestinal tract it reaches the large intestine essentially intact
See page 686

OSMOREGULATION, ANTIDIURETIC HORMONE (ADH) AND THE FORMATION OF CONCENTRATED OR DILUTED URINE The precise control of solute potential is
achieved by the effect of ADH Diuresis – production of large amt of
urine Antidiuretics is the opposite So it has the effects of making urine
more concentrated Aka Vasopressin

ADH
When blood is concentrated ( little water has been drunk, excessive sweating or large amt of salt has been eaten.
This is detected by osmoreceptors in the hypothalamus (thirst center)
Impulses is passed to the pituitary gland where ADH is released
Travels in the blood to the kidney

ADH It increases permeability of the distal
convoluted tubules and collecting duct to water
By increasing the number of water channels,
Also increases permeability to urea in the collecting duct
As a result this creates an osmotic concentration that allows greater reabsorption from the thin descending limb

Figure 26.15a, b
The Effects of ADH on the DCT and Collecting Ducts

ADH
Opposite occurs when there is a high water intake
ADH is inhibited Walls of the distal convoluted tubule and
collecting duct becomes impermeable to water
As a result less water is reabsorbed and a large volume of diluted urine is excreted

ADH
Failure to release sufficient ADH leads to Diabetes insipidus
(large quantities of water is produced)
The fluid lost in urine has to be replaced by excessive drinking

Alcohol consumption suppresses the production of ADH by the pituitary. Why would this result in dehydration and a hangover?

Clinical significance of the presence of proteins in urine
During the process of kidney filtration, blood passes through the kidneys and works to filter out products that are considered to be waste.
During this process, it will allow protein and other nutrients to remain in the body. If these proteins overflow from the blood into the urine, it could indicate that the parts of the kidneys known as the "Glomeruli" are damaged.

Clinical significance of the presence of proteins in urine
This is actually considered to be a warning sign of a serious medical condition known as chronic kidney disease or CKD. This particular condition may occur when a person suffers from high blood pressure, inflammation to one or both kidneys, or even diabetes. Many medical professionals refer to chronic kidney disease as renal disease.

Clinical significance of the presence of proteins in urine The protein urine test measures the amount
of albumin (water soluble proteins) in the urine. Normally, there will not be detectable quantities.
When urine protein is elevated, you have a condition called proteinuria; this can be an early sign of kidney disease.
Albumin is smaller than most other proteins and is typically the first protein that is seen in the urine when kidney dysfunction begins to develop.

Clinical significance of the presence of glucose in urine
Glycosuria, also known as glucosuria, is the
presence of simple sugar or glucose in
the urine.
Blood glucose is normally filtered by
the glomerulus and reabsorbed in the proximal
tubules of the kidneys.
Only a very small amount of glucose is usually
excreted in the urine, approximately .01% or
less, which is not detected by most tests.

Clinical significance of the presence of glucose in urine
There are many possible causes of glycosuria; one common cause is diabetes mellitus.
Diabetes mellitus is a condition characterized by high sugar levels in the blood, also called hyperglycemia. Individuals suspected of having diabetes mellitus often have their urine tested for glycosuria.

TOMORROW’S TEST Uses of Inulin Peritubular capillary/ vasa recta DCT PCT Loop of Henle Substances absorbed by each structure Mode of transport within the nephron for
named substances Clinical significance of the presence of
protein and glucose in the urine.
Related Documents


![Osmoregulation and Excretion [Important words are in bold]](https://static.cupdf.com/doc/110x72/56649e895503460f94b8df70/osmoregulation-and-excretion-important-words-are-in-bold.jpg)