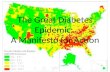
The Epidemic of Type 2 Diabetes During Childhood Francine Ratner Kaufman, M.D. Professor of Pediatrics The Keck School of Medicine of USC Head, Center for Diabetes and Endocrinology Childrens Hospital Los Angeles

The Epidemic of Type 2 Diabetes
Aug 20, 2015
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

The Epidemic of Type 2 Diabetes During Childhood
Francine Ratner Kaufman, M.D.Professor of PediatricsThe Keck School of Medicine of USCHead, Center for Diabetes and EndocrinologyChildrens Hospital Los Angeles

Natural History of Type 2 Diabetes
GeneticsusceptibilityEnvironmentalfactors
NutritionObesityPhysical inactivity
Hyperinsulinemia HDL-C TriglyceridesAtherosclerosisHypertension
AtherosclerosisHyperglycemiaHypertension
RetinopathyNephropathyNeuropathy
BlindnessRenal failureCHDAmputation
Onset ofdiabetes Complications
Disability
DeathOngoing hyperglycemiaIGTInsulin resistance

New-onset NIDDM diagnosed among youth ages 8-21 years at Arkansas Children’s Hospital
21
3
1
67
13
17
0
2
4
6
8
10
12
14
16
18
1988 1989 1990 1991 1992 1993 1994 1995
Year of Diagnosis
Num
ber
of P
atie
nts
Scott et al. Pediatr. 1997

Characteristics - Case Series of 578 Patients at Diagnosis with Type 2
Fagot-Camgagna et al J Pediatr 2000
• Mean Age 12-14 years
• Girls > Boys 1.7:1
• Obese BMI >85th %
• Minority Groups 94%
• Strong Family History 74-100%
• Acanthosis Nigricans 56-92%

Characteristics Case Series of 578 Patients at Diagnosis
• Diagnosis made by Symptoms, not Screening• HbA1c 10-13%• Weight loss 19-62%• Glucose in urine 95%• Ketosis 16-79% • DKA 5-10%• Absence of Islet Autoimmunity >85-95%• Preservation of C-peptide >0.8-1nmol/l
Campagna et al J Pediatr 2000

Acanthosis Nigricans

TREATMENT OF
TYPE 2 DIABETES IN
CHILDREN AND TEENS

Treatment Protocols Multidisciplinary Team
• Set Glycemic Targets
• Diabetes Education – Patient and Family
• Role of Intensive Lifestyle
• Pharmacotherapy
• Regimens Advocated– What are the outcome measures to
assess efficacy, effectiveness

TREATMENT GOALS
• Glucose control, HbA1c <7%– Eliminate symptoms of hyperglycemia – Reduce microvascular complications
• Maintenance of reasonable body weight
• Improve cardiovascular risk factors
• Improvement in physical and emotional well-being

Glycemic Targets*
ParameterParameter NormalNormal GoalGoal Action SuggestedAction Suggested
Fasting (or Fasting (or Preprandial) Preprandial)
GlucoseGlucose<100<100 < 120< 120 <80 or >140<80 or >140
PostprandialPostprandialGlucoseGlucose
<140<140 <180<180 >180>180
Bedtime GlucoseBedtime Glucose <120<120 90 to 15090 to 150 <90 or >160<90 or >160
HbAHbA1c1c(DCCT Method)(DCCT Method) <6%<6% <7%<7% >8%>8%
Glucose values are plasma (mg/mL).Glucose values are plasma (mg/mL).
*Combined WHO recommendations and ADA guidelines.DCCT=Diabetes Control and Complications Trial.

ROLE OF FAMILY IN MANAGEMENT
• African-American Family Study• Group 1, direct family supervision• Group 2, no direct supervision• Group 1 ending HbA1c = 7.1+ 0.8%• Group 2 ending HbA1c = 12.3 + 0.6%• P=<0.0005
Bradshaw, J Pediatr Endocrinol Meta 15, 2002

Intensive Lifestyle Rationale
• Lifestyle and environment are risk factors • Consensus - modifying lifestyle primary goal• Might lead to remission
BUT• Mixed results in adult studies
– More or less effective in kids?
• Labor intensive and expensive – Do they work in the “real world” and school ?

HbA1c Statistics for CHLA 2002Type 2:
n Average ± SD
All patients 100 8.0 ± 2.3
Males 44 8.3 ± 2.2
Females 56 7.8 ± 2.3
Age < 5 years 0
Age 5-10 years 3 6.0 ± 0.9
Age 11-16 years 71 8.0 ± 2.2
Age >16 years 26 8.3 ± 2.5


Mechanisms To Lower Glucose Stimulate
insulin secretion
muscle glucose uptake
Correct insulin
deficiency
glucose production
Retard carbohydrate
absorption
Insulin or insulin analogues X
Sulfonylureas X
Thiazolidinediones X X
Biguanides X X
Repaglanide X
Alpha-glucosidase inhibitors X

TYPE 2 DIABETES . . . A PROGRESSIVE DISEASE
Progressive Decline of -Cell Function in the UKPDS
0
20
40
60
80
100
10 9 8 7 6 5 4 3 2 1 0 1 2 3 4 5 6Years
-C
ell F
un
cti
on
(%
)
Adapted from UK Prospective Diabetes Study (UKPDS) Group. Diabetes. 1995; 44:1249-1258.
6-4

Treatment of Type 2 DM in Children
diet/exercisemonthly review x 3 mo
HbA1c <7%
FPG <120 mg/dl
continue
HbA1c>7%, FPG>120
metforminHbA1c>7% FPG>120
add sulfonylurea? TZD?
add insulin

DiagnosisDiagnosisAsymptomatic
Start with insulin and diet, exercise
Diet and exercise
Monthly review, A1c q 3 m
>7%>7%
Add metformin
Attempt toWean insulin
Add sulfonylureaSilverstein, RosenbloomJ Pediatr Endcrinol Metab, 13,2000
BG 250 mg/dlBG 250 mg/dl
Add Insulin
<7%<7%
>7%>7%
>7%>7%

SStudies to tudies to TTreat reat OOr r PPrevent revent PPediatric ediatric TType ype 22
DDiabetesiabetes((STOPP-T2DSTOPP-T2D))
The TODAY TrialThe TODAY Trial

STOPP-T2 TREATMENTPRIMARY AIM
To compare the efficacy of 3 treatment regimens– Metformin– Metformin + lifestyle– Metformin + TZD
On Time to Treatment Failure and on Glycemic Control

Outcome Measures• Glycemic Controls
• Insulin Sensitivity and Secretion
• Body Composition
• Fitness and Physical Activity
• Nutrition
• Microvascular complications
• CVD Risk
• Quality of Life
• Cost

How Do We Differentiate
Type 1 Diabetes from Type 2 Diabetes

Differentiation Between Type 1 and 2
• 48 with type 2 vs 39 with type 1
• Type 2
– Ethnicity, 1st degree relative, BMI>24, +C-peptide, acanthosis
Type 2 Type 1
DKA 33% 53%
C-peptide 2.2+2.2 ug/l 1.8+3.5 ug/l
Abs 8.1% ICA
30% GAD 35%IAA
Hathout et al Pediatrics 107e102,June,2001

Barriers to Accurate Classification
• 20-25% newly diagnosed TIDM obese
• > 15% of minority populations have FH T2DM baseline
• 3X increase FH of T2DM in patients with T1DM
• Overlap C-P measurements at onset & first year or so
• > 30% T2DM with ketosis at onset

CO-MORBIDITIES

ComorbiditiesPercent of Patients >8 years with
BP >97th PercentileType 1 Type 2
Systolic 3.4% 20.1%
Diastolic 1% 6%

Outcomes in First Nation Youth in Canada
Dean, et al, Diabetes, 2002
Young adults, 18-33 years of age, Diagnosed before age 17 years
Due to poor glycemic control 9% mortality rate 6.3% dialysis rate38% pregnancy loss
During 10-15 year observation period

100 PIMA CHILDREN & ADOLESCENTS
AT DIAGNOSIS
7% high cholesterol (>200 mg/dL)
18% hypertension (BP>140/90)
22% microalbuminuria (alb/Cr >30)
AFTER TEN YEARS [mean HbA1c 12%]
60% microalbuminuria
17% macroalbuminuria (alb/Cr >300)

Screening
Of Children and Youth for
Type 2 Diabetes
and Prediabetes

Who Should be Tested for Type 2- Case Finding
ADA/AAP RecommendationsDiabetes Care 23:2000
• Age > 10 years or onset of puberty• BMI > 85th%• First or Second Degree Relative• Race/Ethnic Group• Signs of Insulin Resistance –
– Acanthosis nigricans– Hypertension– PCOS– Dyslipidemia

Tests To Diagnose Diabetes
• FPG – Preferred • 2-h OGTT - Preferred• 2-h Postprandial or random post meal• HbA1c
• In context of health visit• Every 2 years

ADA/NIDDK Screening Recommendations For Prediabetes in
AdultsDiabetes Care, 25:2002
• Case Finding
• Test: – >45 years, BMI > 25 kg/m2 – <45 years with + FH, GDM, baby > 9 lbs,
dyslipidemia, hypertension, non-Caucasian – At 3 yr intervals, if negative

ADA/NIDDK Recommendations In Adults
Diabetes Care, 25:2002
• How to Test: – In context of health care visit
– FPG, 2-h OGTT
• Intervention: – Prediabetes counsel for weight loss and PA, Follow-
up counseling
– Monitor for DM q 1-2 years, CVD risk factors
– Avoid drug therapy

PreventionREDUCTION
In Obesity
Pharmacotherapyvs
Lifestyle

Agents that can be Used for Obesity
Agents that can be used for Obesity• Sibutramine
– Blocks central reuptake of norepinephrine, serotonin
– Suppresses appetite
– Increases energy expenditure
• Orlistat
– Inhibits pancreatic lipase
– Increases fecal fat loss

Prevention with Metformin
• Six month study in 29 obese, hyperinsulinemic adolescents, positive family history
• Randomized, double-blinded, placebo-controlled
• Freemark, Bursey, SPR, Boston, 2000. Freemark, Bursey Pediatrics 107:2001

Prevention with MetforminMetformin Placebo
P value
BMI 1.3% <0.05 2.3%
FPG 84.8 to
74.8
77.2 to
82.6
Fasting Insulin
31.3 to
19.3
<0.02 No change
No change
Insulin sensitivity
HbA1c
Lipids
Glucose Disposal

The Diabetes Prevention Program
A Randomized Clinical Trial to Prevent Type 2 Diabetes
in Persons at High Risk
The DPP Research Group

0 1 2 3 4
0
10
20
30
40Placebo (n=1082)Metformin (n=1073, p<0.001 vs. Plac)Lifestyle (n=1079, p<0.001 vs. Met , p<0.001 vs. Plac )
Percent developing diabetes
All participants
All participants
Years from randomization
Cu
mu
lativ
e in
cid
enc
e (
%)
Placebo Metformin
Lifestyle
Type 2 Diabetes PreventionType 2 Diabetes PreventionRisk reductionRisk reduction31% by metformin31% by metformin58% by lifestyle58% by lifestyle
The DPP Research Group, NEJM 346:393-403, 2002

Prevention of Type 2 with Lifestyle Intervention Tuomilehto, et al , Turku ADA 2000
• Intervention – 523 IGT, mean age 55, BMI 31
• Diet, exercise, frequent visits vs advice yearly
Weight
Loss
1st Year 2nd Year 4th Year
Intervention -4.2 -3.5 26 cases
10%
Control -0.8 -0.8 57 Cases
22%
Incidence of diabetes reduced – 58% (p=.0003)

PUBLIC HEALTH
RESPONSE

National Comprehensive Obesity-Diabesity Prevention Strategy
• Educational
• Behavioral
• Environmental
– Increase understanding and awareness– Change behavior– Ability to make the right choices

Key Targets
• Communities– Joint use schools, parks, libraries, organizations
• Workplace– Wellness programs, insurance,
• Government– Funding, policies
• Individual/Family– Behavior change
• Health Sector• Schools
– PE, nutrition services, health education

Breast Feeding
• Decrease in obesity• In Pima population, dose related decrease in
risk of type 2 with breast feeding• Most significant with exclusive breast feeding• Breast feeding regimen
– exclusive for 6 months– total for 12 months
Simmons D, Lancet 97, 157

Breast Feeding
• Native Canadian Population
• 4-Fold decrease in type 2 diabetes in adolescents
• Exclusive Breast Feeding
Young et al, Arch Pediatr Adolesc Med, 2002

Promotion of: RETURN TO ENERGY BALANCE
• Water intake
• Fruits and Vegetables
• Limiting Juice
• Avoiding Sugar Containing Sodas
• Decreasing Saturated Fat
• Near Eliminating High Density/Low Nutrient Foods

School Could Be A Setting For
• Public education
• Epidemiological studies
• Early intervention with at-risk groups
• Screening and early detection

SStudies to tudies to TTreat reat OOr r PPrevent revent PPediatric ediatric TType ype 22 DDiabetesiabetes((STOPP-T2DSTOPP-T2D))
• Population based trial
• Increase physical activity
• Nutrition promotion
• Social Marketing, Behavioral Component
• Biologic outcome measures – primary– Reduction in risk factors

CONCLUSIONS
• Why are Children Obese– Too much food, no activity
• Insulin Resistance and Relative Beta Cell Failure– Intrauterine environment, postnatal feeding
• Type 2 Diabetes– Symptomatic presentation, treatment algorithms,
screening
• Public Health/Advocacy – School policies, legislative agenda
– Concentrate on pre and perinatal periods
Related Documents