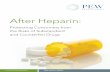
The Duke Heparin Protocol Implementation of Nurse Driven Heparin Protocol at Duke University Hospital Jordan Hildenbrand, MS2; Kimberly Hodulik PharmD, CACP, CPP; Adam Root PharmD; Jason Funaro PharmD; Dorothy Filippi MSN, RN, CCRN; Faryl Podolle RN; Susan Ashland RN; Megan Greenland PharmD; Noppon Setji MD; Nilesh Patel MD Departments of Medicine, Pharmacy, and Nursing, Duke University Hospital Technology • Lack of current EMR based decision support tools • Multiple processes and options for heparin ordering Nursing Phlebotomy • No timed labs at DUH • Delay from time of order to draw, exacerbated based on phlebotomist scheduling • Process potentially more complex than other nurse driven infusions • Variable experience based on nursing unit Physicians • Perceived low compliance with institutional policy • Delay to follow up and intervention on monitoring labs • Communication among team delayed • Variable experience with heparin Leadership • No structured education focused on heparin infusions • Policies difficult to find with current tools Pharmacy • High patient and team volume per PharmD • Variable local ordering cultures of heparin HEPARIN MANAGEMENT ERRORS FISHBONE DIAGRAM AIMS • The new Duke Heparin protocol will improve adherence with the dosing, timing, and communication required with the institutional nomogram • The new Duke Heparin protocol will decrease the time to therapeutic range for patients on heparin BACKGROUND • Patients are anticoagulated in the inpatient setting using heparin for reasons including deep vein thrombosis, acute coronary syndromes, and atrial fibrillation • Advantages of heparin are titratability, reversibility, and use in renal failure • Disadvantages include a narrow therapeutic window • Under-dosing, inconsistent adherence to nomogram, and delayed communication are barriers to ideal heparin dosing INTERVENTIONS • Formation of an inter-professional team, including leadership, nurses, physicians, and pharmacists • Assessment of current heparin management process, including ordering process (through Epic®), indications, frequency of use, and amount of oversight • Assessment of current factors leading to heparin management errors (see fishbone) and development of new heparin process map • Development of education program for 110 nurses regarding heparin indications, management, and complications • Development of new educational, policy and calculator tools through DukeCore.org/heparin • One-on-one training of all bedside nurses on heparin management process • Development of feedback process on all errors regarding heparin with nursing, pharmacy, and physician leads • Evaluate nomogram to potentially deliver faster times to therapeutic to patients • Expand the protocol to more units within Duke University Hospital • EPIC/EMR integration of decision support tools • Engage phlebotomy leadership in decreasing delays to aPTT draws • Re-evaluate nursing comfort as experience continues NEXT STEPS • General medicine nurses are engaged in delivering a safe heparin protocol to patients • Nursing protocols improve compliance with an institutional nomogram • Nurses and physicians deliver similar results in heparin titration • Nurses are comfortable in managing heparin infusions • Improved safety endpoints compared to before initiation • RNs respond quickly to aPTT values and make corresponding dose titrations CONCLUSIONS & LESSONS LEARNED OUTCOMES DEMOGRAPHICS Pre-Protocol (n=33) On-Protocol October -January (n=33) On-Protocol January-May (n=42) Indication DVT/PE 18 (55%) 19 (40%) 29 (69%) Atrial fibrillation /mechanical valve 11 (33%) 7 (21%) 9 (21%) ACS/MI 3 (9%) 5 (15%) 2 (5%) Stroke 0 (0%) 0 0 Other 1 (3%) 2 (6%) 2 (5%) PROCESS MEASURES Pre-Protocol Value On-Protocol Value (October-January) On-Protocol Value (January-May) # aPTTs per patient 4 4 4.6 Inappropriate Bolus Adjustments 53/177 (30%) 7/125 (6%) 33/192 (17%) Inappropriate Infusion Adjustments 70/177 (40%) 10/125 (8%) 36/192 (19%) Adjustments within 60 minutes of aPTT result 38/71 (54%) 54/70 (77%) 61/78 (78%) Mean time to RN adjustment 1.3 hours 0.7 hours 0.84 hours OUTCOMES Pre-Protocol Value On-Protocol Value (October-January) On-Protocol Value (January-May) Number of patients having therapeutic aPTTs 23/33 (70%) 21/33 (66%) 38/42 (90%) Time to Therapeutic (mean) 15.9 hrs 14.4 hrs 16.2 hrs SAFETY MEASURES Pre-Protocol Value On-Protocol Value (October-January) On-Protocol Value (January-May) Minor Bleeding 2 (6%) 4 (12%) 3 (7%) Major Bleeding 4 (12%) 5 (15%) 1 (2%) Recurrent Thrombus 0 0 0

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

The Duke Heparin ProtocolImplementation of Nurse Driven Heparin Protocol at Duke University Hospital
Jordan Hildenbrand, MS2; Kimberly Hodulik PharmD, CACP, CPP; Adam Root PharmD; Jason Funaro PharmD; Dorothy Filippi MSN, RN, CCRN; Faryl Podolle RN; Susan Ashland RN; Megan Greenland PharmD; Noppon Setji MD; Nilesh
Patel MDDepartments of Medicine, Pharmacy, and Nursing, Duke University Hospital
Technology• Lack of current
EMR based decision support tools
• Multiple processes and options for heparin ordering
Nursing Phlebotomy• No timed labs at
DUH• Delay from time of
order to draw, exacerbated based on phlebotomist scheduling
• Process potentially more complex than other nurse driven infusions
• Variable experience based on nursing unit
Physicians• Perceived low compliance
with institutional policy• Delay to follow up and
intervention on monitoring labs
• Communication among team delayed
• Variable experience with heparin
Leadership• No structured
education focused on heparin infusions
• Policies difficult to find with current tools
Pharmacy• High patient and
team volume per PharmD
• Variable local ordering cultures of heparin
HEPARIN MANAGEM
ENT ERRORS
FISHBONE DIAGRAM
AIMS• The new Duke Heparin protocol will improve adherence
with the dosing, timing, and communication required with the institutional nomogram
• The new Duke Heparin protocol will decrease the time to therapeutic range for patients on heparin
BACKGROUND• Patients are anticoagulated in the inpatient setting using
heparin for reasons including deep vein thrombosis, acute coronary syndromes, and atrial fibrillation
• Advantages of heparin are titratability, reversibility, and use in renal failure
• Disadvantages include a narrow therapeutic window• Under-dosing, inconsistent adherence to nomogram, and
delayed communication are barriers to ideal heparin dosing
INTERVENTIONS• Formation of an inter-professional team, including leadership,
nurses, physicians, and pharmacists• Assessment of current heparin management process,
including ordering process (through Epic®), indications, frequency of use, and amount of oversight
• Assessment of current factors leading to heparin management errors (see fishbone) and development of new heparin process map
• Development of education program for 110 nurses regarding heparin indications, management, and complications
• Development of new educational, policy and calculator tools through DukeCore.org/heparin
• One-on-one training of all bedside nurses on heparin management process
• Development of feedback process on all errors regarding heparin with nursing, pharmacy, and physician leads
• Evaluate nomogram to potentially deliver faster times to therapeutic to patients
• Expand the protocol to more units within Duke University Hospital• EPIC/EMR integration of decision support tools• Engage phlebotomy leadership in decreasing delays to aPTT draws• Re-evaluate nursing comfort as experience continues
NEXT STEPS
• General medicine nurses are engaged in delivering a safe heparin protocol to patients
• Nursing protocols improve compliance with an institutional nomogram
• Nurses and physicians deliver similar results in heparin titration• Nurses are comfortable in managing heparin infusions• Improved safety endpoints compared to before initiation• RNs respond quickly to aPTT values and make corresponding dose
titrations
CONCLUSIONS & LESSONS LEARNED
OUTCOMES
DEMOGRAPHICS Pre-Protocol (n=33)On-Protocol
October-January (n=33)
On-Protocol
January-May (n=42)
Indication
DVT/PE 18 (55%) 19 (40%) 29 (69%)
Atrial fibrillation
/mechanical valve11 (33%) 7 (21%) 9 (21%)
ACS/MI 3 (9%) 5 (15%) 2 (5%)
Stroke 0 (0%) 0 0
Other 1 (3%) 2 (6%) 2 (5%)
PROCESS MEASURES Pre-Protocol ValueOn-Protocol Value
(October-January)
On-Protocol Value
(January-May)
# aPTTs per patient 4 4 4.6
Inappropriate Bolus
Adjustments53/177 (30%) 7/125 (6%) 33/192 (17%)
Inappropriate Infusion
Adjustments70/177 (40%) 10/125 (8%) 36/192 (19%)
Adjustments within 60
minutes of aPTT result38/71 (54%) 54/70 (77%) 61/78 (78%)
Mean time to RN
adjustment1.3 hours 0.7 hours 0.84 hours
OUTCOMES Pre-Protocol ValueOn-Protocol Value
(October-January)
On-Protocol Value
(January-May)
Number of patients having
therapeutic aPTTs23/33 (70%) 21/33 (66%) 38/42 (90%)
Time to Therapeutic (mean) 15.9 hrs 14.4 hrs 16.2 hrs
SAFETY MEASURES Pre-Protocol ValueOn-Protocol Value
(October-January)
On-Protocol Value
(January-May)
Minor Bleeding 2 (6%) 4 (12%) 3 (7%)
Major Bleeding 4 (12%) 5 (15%) 1 (2%)
Recurrent Thrombus 0 0 0
Related Documents