
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

By
Dr.Krishnakanth Reddy.P PG 2nd year
Dept of Paediatrics

Accumulation of extra pulmonary air within the
pleural cavity
Most commonly from leakage of air from the lung

Pneumothorax can be associated with
Serous effusion (Hydropneumothorax)
Blood ( Hemopneumothorax)
Purulent effusion ( pyopneumothorax)
Bilateral: After lung transplantation
Mycoplasma pneumonia
Tuberculosis

Spontaneous pneumothorax
Traumatic pneumothorax
Iatrogenic pneumothorax
Catamenial pneumothorax

Primary/ idiopathic: without trauma or underlying
disease • Familial cases have mutations in the folliculin
gene(FCLN) • Birt Hogg Dube syndrome • Marfans syndrome Ehler Danlos syndrome
Secondary - Complication of an underlying disease without trauma eg: pneumonia,emphysema,COPD,

Traumatic pneumothorax ◦ External chest trauma
◦ Abdominal blunt or penetrating trauma

Iatrogenic pneumothorax
◦ Thoracocentesis
◦ Trans thoracic needle aspiration
◦ Diagnostic or therapeutic procedures

Catamenial pneumothorax
◦ Prior to menses
◦ associated with diaphragmatic defects & pleural
blebs

In normal people, the pressure in pleural space is negative
during the entire respiratory cycle
Two opposite forces result in negative pressure in pleural
space: Inherent outward pull of the chest wall
Inherent elastic recoil of the lung

The negative pressure will be disappeared if any
communication develops
When a communication develops through the chest wall
between the atmosphere and the pleural space air will enter
the pleural space until the pressure gradient is eliminated or
the communication is closed


Negative pressure eliminated ◦ The lung recoil-small lung-volume decrease ◦ V/Q decrease-shunt increase
Positive pressure ◦ Compress blood vessels and heart ◦ Decreased cardiac output ◦ Impaired venous return ◦ Hypotension ◦ Shock
Result in ◦ Decrease in vital capacity ◦ Decrease in PaO 2

Abrupt onset
Symptoms proportional to Extent of lung collapse & Pre existing lung disease and Pressure gradient
Dyspnoea
Chest pain
Cyanosis

Respiratory distress
Chest Retractions – subcostal, intercostal, xiphoid
Deviation of trachea, heart towards unaffected side
Tympanic percussion note
Decreased / absent breath sounds

Chest X ray findings
Pleural line
No lung markings
The outer margin of visceral
pleura separated from the
parietal pleura by a lucent
gas space devoid of
pulmonary markings .

BTS (British thoracic society) The rim of air between the
pleura and the chest wall Small <1cm Moderate :1- 2cm Large >2cm
ACCP ( American college of chest
physicians) The apex-to-cupola distance Small <3cm Large ≥ 3cm

In difficult cases in whom the lungs are obscured by
overlying surgical emphysema
To differentiate a pneumothorax from suspected
bulla in complex cystic lung disease and congenital
lobar emphysema


Emphysema ( local or generalized)
Cystic formations
Diaphragmatic hernia
Compensatory overexpansion with contralateral
atelecatasis

Goals
promote lung expansion
To eliminate the pathogenesis
To prevent recurrence of pneumothorax

based on
Type of pneumothorax
Pathogenesis
Pneumothorax frequency
Extension of lung collapse
Severity of disease
Complication and concomitant underlying disease

Observation
Antibiotics
100% oxygen
Needle aspiration
Intercostal tube drainage
Chemical pleurodesis
Thoracoscopy
Surgical treatment

Treatment of the underlying pulmonary disease
should begin on admission and should be continued
throughout the course of treatment directed to the
lung pathology

Observation and no intervention ◦ If Small (<5%),moderate sized in an
otherwise normal child

INDICATIONS Secondary spontaneous pneumothorax Unstable pneumothorax Severe dyspnoea Lung collapse Open or tension pneumothoraces Frequent recurrent pneumothoraces If Simple aspiration or catheter aspiration drainage
is unsuccessful in controlling symptoms


Prerequisites : check for and correct bleeding
disorders
Position: The child is positioned supine or with the affected side up.
Site:The site of chest tube insertion is in the midclavicular line of second and third intercostal space or anterior axillary line of 5th and 6th intercostal space


Placement of underwater seal below the drain insertion site
Movement of water column
Vital data
Dressing to be changed daily
Monitor the insertion site for infection

Equal breath sounds
No hypoxemia
CXR to ensure expansion
No air leak
Trial tube clamping for 6 hrs
No drainage/accumulation of fluid in tube

Penetration of major organs Lung, stomach, spleen, liver,
heart and great vessels
Occur more commonly when a sharp metal trocar is
inappropriately applied
Pleural infection
Empyema
Surgical emphysema
Subcutaneous emphysema

Other interventions in treatment of pneumothorax

Indications
Persistent air leak Repeated pneumothorax Bilateral pneumothoraces Complicated with bullae Lung dysfunction Sclerosing agents -Tetracycline, Minocycline, Doxycline,
Talc, Erythromycin

Video-assisted thoracoscopic surgery (VATS) is a preferred
therapy for blebectomy, pleural stripping, pleural
brushing,decortication and instillation of sclerosing agents,
with somewhat less morbidity than occurs with traditional
open thoracotomy.

Indications
No response to conventional treatment
Persist air leak
Hemopneumothorax
Bilateral pneumothoraces
Thick pleura makes lung unable to re expansion
Multiple blebs or bullae

Pyopneumothorax, Hemopneumothorax
◦ Caused by aspiration or intercostal chest tube insertion ◦ Also results from necrotic pneumonia, lung abscess, or caseous pneumonia
Mediastinal and subcutaneous emphysema
Pneumomediastinum, Pneumocardium, , Pneumoperitoneum
Surgical emphysema

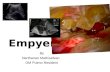
Pyopneumothorax (also known as infected
hydropneumothorax or empyemic hydropneumothorax)
is a pleural collection of pus and air.
It may be a variant of a thoracic empyema with air
containing components although the aetiology may be
different.

Clinical presentation
Chest pain
Fever
Cough
Dyspnoea

An air-fluid level
Loss of silhouette with the dome of diaphragm.
Presence of thick pleural lining strongly favours the pyopneumothorax

Ultrasound
Fine internal echoes in the pleural collection strongly suggests
infected fluid in appropriate clinical settings.
CT scan chest
CT will clearly depict the location of the collection as well as
thickening of pleura and underlying disease process (if any).

Differential diagnosis
Non-infected hydropneumothorax (no pleural thickening)
peripheral lung abscess
previous empyema with iatrogenic introduction of air (e.g.
drain insertion or diagnostic aspiration etc.)

Treatment of pyo-pneumothorax Large collections require intercostal drainage with
antibiotics.

Related Documents









![OrganizingPneumoniabyParagonimiasisandCoexistent ... · 2019. 7. 31. · hydropneumothorax, pulmonary nodules or air-space con-solidation, and cysts [1]. Of the nodular lesions, subpleural](https://static.cupdf.com/doc/110x72/6114ece483915b0c68374d20/organizingpneumoniabyparagonimiasisandcoexistent-2019-7-31-hydropneumothorax.jpg)

