Orthodontic Treatment, Including Transplanted Teeth and Dento-Alveolar Osteotomy, for Dental Ankylosis after Multidisciplinary Treatment for Rhabdomyosacroma of the Cheek: A Case Report and Review Seigo Ohba 1, 2 , Hitoshi Yoshimura 2 , Takiko Matsuura 2 , Kazuo Sano 2 1 Department of Regenerative Oral Surgery, Nagasaki University, Graduate School of Biomedical Sciences, Japan. 2 Division of Dentistry and Oral Surgery, Department of Sensory and Locomotor Medicine, Faculty of Medical Sciences, University of Fukui, Japan Abstract Multidisciplinary treatment for head and neck malignant tumors is often performed in children and adolescents. This treatment strategy may induce dental morphological aberrations and missing teeth, resulting in leading to problems with occlusions. A 14- year-old male underwent multidisciplinary treatment for rhabdomyosarcoma of his right cheek when he was three years old. He claimed a serious malocclusion. The hopeless teeth were extracted. Simultaneously, the bilateral lower first premolars were auto transplanted to the upper right canine and first premolar regions. Total orthodontic treatment was initiated six months after the surgery. Subsequently, a segmental osteotomy was performed because of dental ankylosis of the right upper central incisor. Finally, a good occlusion was created. Orthodontic treatment that includes the transplanted tooth after healing can create an ideal dental arch and good occlusion. If dental ankylosis is determined, a dentoalveolar osteotomy should be performed to create a good occlusion. Key Words: Multidisciplinary treatment, Tooth transplantation, Rhabdomyosarcoma, Dento-alveolar osteotomy, Dental ankylosis Introduction Multidisciplinary treatment, which combines tumor resection, chemotherapy (CT), and radiotherapy (RT) for malignant tumors in the head and neck region, is often performed in children and adolescents [1-3]. The outcomes of this treatment strategy have been reliable; however, there are a number of disadvantages accompanying this treatment, such as the disturbance of growth and development in the head and neck region [4]. Furthermore, because the tooth is affected negatively by CT and RT during its development, dental morphological aberrations and missing teeth can result [5]. One of the treatment options for a missing tooth is auto- tooth transplantation. This method is a quite reliable option, and its long-term survival rate is more than 90% [6-10]. There are two essential factors for the success of auto-tooth transplantation. One factor is an intact periodontal ligament [11], and the other is an appropriate size of the recipient site [12]. The risk factors for the failure of auto-tooth transplantation are age (40 years or more) and using a molar tooth as a donor [5]. However, there is no report that has examined the survival rate of auto-tooth transplantation at the irradiated region. According to previous reports describing dental implantation at the irradiated region [13-16], auto-tooth transplantation may succeed at the irradiated region if the total irradiation dose is less than 45 Gy. While the harmful effects of CT to the periodontium remain unclear, there are a number of reports that refer to the deleterious effects of RT to the periodontium [17,18]. In particular, the periodontal ligament has a high sensitivity to radiation. For instance, RT has been shown to expand the periodontal space [19] or to induce periodontal attachment loss, resulting in an increase in the occurrence of osteoradionecrosis [20].However, there is no report that has referred to the relationship between CT or RT and dental ankylosis. In this report, we describe a patient who had submitted to such a multidisciplinary treatment for arhabdomyosarcoma of his right cheek in childhood. For a dental morphological aberration and serious malocclusion, he underwent the extraction of the abnormal teeth and auto-tooth transplantation at the irradiated region. Subsequently, orthodontic treatment and dento-alveolar osteotomy for the dental ankylosis created a good occlusion. Case report This study received ethical approval from the institution. A 14-year old male visited the Department of Dentistry and Oral Surgery, University of Fukui Hospital, due to malocclusion (Figure 1). He had undergone a tumor resection when he was three years and had subsequently received CT (vincristine, actinomycin D, cyclophosphamide and cisplatin) and RT (Linac X-ray, total 44 Gy) for rhabdomyosarcoma of his right cheek, according to the Intergroup Rhabdomyosarcoma study- III protocol [2], one year after surgery. The patient has had no recurrences since submitting to the multidisciplinary therapy. According to routine examinations, including orthopantomograph (OPG) (Figure 2), cephalometric analysis (Table 1), and clinical findings, some problems had been observed, as listed below: • the first molar occlusal relationship wasclass III onthe right and class I onthe left • crowding of the bimaxillary anterior teeth due toa discrepancy between the size of the alveolar bone and the width of teeth • remaining upper right deciduous cuspid • labioclination of the bimaxillary incisors • short roots of theupper right lateral incisor, canine, premolars and theupper left lateral incisor • relatively short roots of theupper left central incisor, second premolar and theupper right central incisor Corresponding author: Seigo Ohba DDS, PhD, Department of Regenerative Oral Surgery, Nagasaki University, Graduate School of Biomedical Science, 1-7-1 Sakamoto, Nagasaki 852-8588 Japan, Tel: +81 95 819 7704; Fax: +81 95 819 7705; E-mail: [email protected] / [email protected] 318

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Orthodontic Treatment, Including Transplanted Teeth and Dento-AlveolarOsteotomy, for Dental Ankylosis after Multidisciplinary Treatment forRhabdomyosacroma of the Cheek: A Case Report and ReviewSeigo Ohba1, 2, Hitoshi Yoshimura2, Takiko Matsuura2, Kazuo Sano2
1Department of Regenerative Oral Surgery, Nagasaki University, Graduate School of Biomedical Sciences, Japan. 2Division ofDentistry and Oral Surgery, Department of Sensory and Locomotor Medicine, Faculty of Medical Sciences, University of Fukui,Japan
AbstractMultidisciplinary treatment for head and neck malignant tumors is often performed in children and adolescents. This treatmentstrategy may induce dental morphological aberrations and missing teeth, resulting in leading to problems with occlusions. A 14-year-old male underwent multidisciplinary treatment for rhabdomyosarcoma of his right cheek when he was three years old. Heclaimed a serious malocclusion. The hopeless teeth were extracted. Simultaneously, the bilateral lower first premolars were autotransplanted to the upper right canine and first premolar regions. Total orthodontic treatment was initiated six months after thesurgery. Subsequently, a segmental osteotomy was performed because of dental ankylosis of the right upper central incisor. Finally,a good occlusion was created. Orthodontic treatment that includes the transplanted tooth after healing can create an ideal dental archand good occlusion. If dental ankylosis is determined, a dentoalveolar osteotomy should be performed to create a good occlusion.
Key Words: Multidisciplinary treatment, Tooth transplantation, Rhabdomyosarcoma, Dento-alveolar osteotomy, Dental ankylosis
IntroductionMultidisciplinary treatment, which combines tumor resection,chemotherapy (CT), and radiotherapy (RT) for malignanttumors in the head and neck region, is often performed inchildren and adolescents [1-3]. The outcomes of this treatmentstrategy have been reliable; however, there are a number ofdisadvantages accompanying this treatment, such as thedisturbance of growth and development in the head and neckregion [4]. Furthermore, because the tooth is affectednegatively by CT and RT during its development, dentalmorphological aberrations and missing teeth can result [5].
One of the treatment options for a missing tooth is auto-tooth transplantation. This method is a quite reliable option,and its long-term survival rate is more than 90% [6-10]. Thereare two essential factors for the success of auto-toothtransplantation. One factor is an intact periodontal ligament[11], and the other is an appropriate size of the recipient site[12]. The risk factors for the failure of auto-toothtransplantation are age (40 years or more) and using a molartooth as a donor [5]. However, there is no report that hasexamined the survival rate of auto-tooth transplantation at theirradiated region. According to previous reports describingdental implantation at the irradiated region [13-16], auto-toothtransplantation may succeed at the irradiated region if the totalirradiation dose is less than 45 Gy.
While the harmful effects of CT to the periodontium remainunclear, there are a number of reports that refer to thedeleterious effects of RT to the periodontium [17,18]. Inparticular, the periodontal ligament has a high sensitivity toradiation. For instance, RT has been shown to expand theperiodontal space [19] or to induce periodontal attachmentloss, resulting in an increase in the occurrence ofosteoradionecrosis [20].However, there is no report that hasreferred to the relationship between CT or RT and dentalankylosis.
In this report, we describe a patient who had submitted tosuch a multidisciplinary treatment for arhabdomyosarcoma ofhis right cheek in childhood. For a dental morphologicalaberration and serious malocclusion, he underwent theextraction of the abnormal teeth and auto-tooth transplantationat the irradiated region. Subsequently, orthodontic treatmentand dento-alveolar osteotomy for the dental ankylosis createda good occlusion.
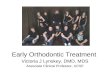
Case reportThis study received ethical approval from the institution. A14-year old male visited the Department of Dentistry and OralSurgery, University of Fukui Hospital, due to malocclusion(Figure 1). He had undergone a tumor resection when he wasthree years and had subsequently received CT (vincristine,actinomycin D, cyclophosphamide and cisplatin) and RT(Linac X-ray, total 44 Gy) for rhabdomyosarcoma of his rightcheek, according to the Intergroup Rhabdomyosarcoma study-III protocol [2], one year after surgery. The patient has had norecurrences since submitting to the multidisciplinary therapy.According to routine examinations, includingorthopantomograph (OPG) (Figure 2), cephalometric analysis(Table 1), and clinical findings, some problems had beenobserved, as listed below:
• the first molar occlusal relationship wasclass III ontheright and class I onthe left
• crowding of the bimaxillary anterior teeth due toadiscrepancy between the size of the alveolar bone and thewidth of teeth
• remaining upper right deciduous cuspid• labioclination of the bimaxillary incisors• short roots of theupper right lateral incisor, canine,
premolars and theupper left lateral incisor• relatively short roots of theupper left central incisor,
second premolar and theupper right central incisor
Corresponding author: Seigo Ohba DDS, PhD, Department of Regenerative Oral Surgery, Nagasaki University, Graduate Schoolof Biomedical Science, 1-7-1 Sakamoto, Nagasaki 852-8588 Japan, Tel: +81 95 819 7704; Fax: +81 95 819 7705; E-mail:[email protected] / [email protected]
318

Figure 1. Intraoral findings at his first visit.
Figure 2. Orthopantomography at his first visit.
Table 1. Cephalometric analysis before and after treatment. T1; pre-treatment, T2; before corticotomy, T3; at retainer setting.
Mean SD T1 T2 T3
Facial angle 85.07 5.76 87.3 87.7 87.9
Convexity 5.60 4.33 10.0 8.7 8.8
A-B plane -5.10 3.28 -4.9 -3.7 -4.1
SNA 81.82 3.09 86.4 85.8 86.1
SNB 78.61 3.15 81.4 81.7 81.8
Mandibular Plane 26.25 6.34 30.3 29.3 29.2
Y-axis 65.71 3.27 62.3 61.9 62.0
Occlusal Plane 9.52 4.01 7.1 9.2 8.2
Interincisal 129.66 8.99 99.9 122.7 124.0
U-1 to FH plane 108.94 5.62 129.2 116.2 114.9
L-1 to Mandibular plane 94.67 7.21 100.6 91.9 91.9
Based on the problems mentioned above and the patient’swishes, a treatment procedure was planned. Because thereason for his malocclusion was a discrepancy between thesize of the alveolar bone and the width of teeth, we extractedhis upper right lateral incisor, deciduous cuspid, canine andupper right first premolar and upper left lateral incisor, whichwere considered to be hopeless because of disabilities in theirroot development. Subsequently, the bilateral lower firstpremolars were extracted and transplanted into the region ofright upper canine and first premolar. These treatments
created the occlusion after that the bilateral upper lateralincisors and bilateral lower first premolars were lacking.Although the length of roots of the upper right central incisor,upper right second premolar and upper left central incisorwere relatively short, these teeth were considered to bemaintained. If the teeth had been lost, dental implants wouldhave been inserted. Root canal fillings of the auto-transplantedteeth were performed after three weeks (Figure 3), andorthodontic treatment was initiated two months post-surgery.
Figure 3. Intraoral findings when the root canal fillings of transplanted teeth were performed.
OHDM- Vol. 14- No.5-October, 2015
319

After two years, adento-alveolar osteotomy was performedat the upper right central incisor due to its dental ankylosis(Figure 4). A retainer was set six months later (Figure 5). No
root resorption, including at the transplanted teeth, wasobserved on OPG (Figure 6).
Figure 4. Intraoperative finding of the corticotomy before osteotomy (left) and after fixation with an absorbable plate (right).The bone particlewas filled into the gap.
Figure 5. Intraoral findings at setting of a retainer.
Figure 6. Orthopantomography one year after the orthodontictreatment. No root absorptions of transplanted teeth wereobserved.
DiscussionIt is well-known that both CT and RT adversely affect dentaldevelopment during the incipient stages, and the combinationof these two therapies increases the deleterious effects. Thepresent patient underwent a systemic CT and local RT for his
rhabdomyosarcoma. While he had hypoplastic roots for someteeth in the irradiated region, there were no abnormal teethoutside of this region. This finding meant CT did not providea sufficient side effect to create the abnormal teeth by itself;rather, RT alone or the combination of CT and RT may inducesuch abnormal teeth. There is no report that has clearly foundhow much irradiation is needed to produce such a dentalmorphological aberration. According to our case, 44 Gy mayinduce dental morphological aberrations when systemic CT isperformed simultaneously.
This case demonstrated that it is possible to transplant anauto-tooth at the irradiated region when the irradiation dose isless than 44 Gy, even if systemic CT is simultaneouslyperformed. It is also considered possible to performorthodontic treatment for the transplanted tooth if theperiodontal ligament regenerates and the bioactivity of the jawbone is maintained. When performing tooth transplantation, itis important to confirm that the irradiated region of the jawdoes not suffer from osteoradionecrosis. Marx et al. [19]suggested that RT damages the capillaries at the lesion,resulting in hypoxia due to the ischemic condition. Thus,osteoradionecrosis of the jaw (ORNJ) may be developed.ORNJ may occur when the irradiated dose is approximatelygreater than 50 Gy [15].In this case, the facial appearance wassymmetrical, and no bilateral developmental differences wereobserved at the maxilla according to lateral and frontalcephalogram. No canting of the maxilla was observed.Moreover, the development of the maxilla was not disturbedby RT, according to the normal development of the mandibleoutside of the RT field. Cephalometric analysis also impliednon-disturbed bone growth (Table 1). Therefore, the patient’sbone activity was considered to be unimpaired.
There is no report that has reviewed the success rate ofauto-tooth transplantation at the irradiated region. To predictwhether tooth transplantation is successful, the availability ofthe success rates of dental implants at the irradiated region isinformative. Colella et al. [16] reported that there is nosignificant difference in the implant success rate within 45Gy, and Dholam and Gurav [13] concluded that RT did notinfluence the implant treatment if the amount was less than 45
OHDM- Vol. 14- No.5-October, 2015
320

to 50 Gy. Moreover, Javed et al. [14] stated thatosseointegration is not affected by 50 to 65 Gy. According tothese previous reports, biological activity should beconsidered to be inhibited by more than a 45 Gy RT dose.Hence, auto-tooth transplantation was considered to have littlepossibility of succeeding in such cases. The preservation ofthe periodontal ligament is one of the essential factors tosuccessful auto-tooth transplantation. In this case, the donorteeth were considered not to be affected byRT because thedonor teeth existed outside the irradiation area. In fact, thedonor teeth were normal, and the periodontal ligament spacesof these teeth were observed on OPG.
While Fiorentino et al. [21] initiated orthodontic treatmentsix months after auto-tooth transplantation, Ziegler et al. [22]initiated orthodontic treatment four weeks after auto- toothtransplantation. Day [5] advocated that orthodontic treatmentshould be initiated 4-6 months after tooth transplantation. Onthe other hand, Kim et al. [6] reported that the soft tissuehealing was completed two to four months after auto-toothtransplantation. Although the timing of the initiation oforthodontic treatment after the auto-tooth transplantationvaries based on the previous reports, it is considered that themovement of the transplanted tooth should be initiated sixmonths after the auto-tooth transplantation, at which point theperiodontal membrane regenerates and the alveolar bone healscompletely [5]. We initiated post-surgical orthodontictreatment two months after transplantation, but thetransplanted teeth were moved six months post-surgery.
Park et al. [23] transplanted the tooth into a space providedduring orthodontic treatment based on previous predictions,creating a good occlusion. Moreover, dental implant treatmentis often performed instead of auto-tooth transplantation insimilar procedures. Because orthodontic treatment wasplanned in this case, auto-tooth transplantation was consideredbetter than dental implants due to its movability. Orthodontictreatment, including the transplanted teeth, provided a goodoutcome in this case.
RT sometimes affects the periodontium adversely[19,20,24,25]. Most reports have referred to periodontalattachment loss and damage to the periodontal ligament.Although there is no report that has specifically referred to therelationship between CT or RT and dental ankylosis, theupper right central incisor in this case showed dentalankylosis. In fact, orthodontic treatment was unable to movethe tooth. The tooth was considered to be affected by RT dueto its short root. Because the tooth had not had any episode ofperiodontal disease after CT/RT, the dental ankylosis wasconsidered to be caused by damage to the periodontalligament due to RT/CT. However, it was unclear why onlythis tooth showed dental ankylosis at the irradiated region.Dento-alveolar osteotomy was indicated, and a segment wasmoved to an ideal position with an ideal direction according tothe previous report [26]. No infected bone was observedduring surgery (Figure 4). The ideal dental arch wascompleted after surgery (Figure 5).
ConclusionRT and/or CT for tumors of the oral and maxillofacial regionoften induce abnormal events, such as missing teeth and
abnormal dental morphology. Moreover, a size discrepancycan occur between the dental arch and alveolar bone.Malocclusion can be observed in these cases, and orthodontictherapy may be needed. If there are hopeless teeth due to theside effects of RT/CT, these teeth are extracted and normalteeth are transplanted into the region. Orthodontic treatment,including the transplanted tooth, can create an ideal dentalarch and good occlusion. If dental ankylosis accompaniedwith CT/RT is observed and the bioactivity of jaw bone isnormal, dento-alveolar osteotomy is indicated for the creationof an ideal dental arch.
References1. Gillepsie MB, Marshall DT, Day TA, Mitchell AO, White
DR, et al. Pediatric rhabdomyosarcoma of the head and neck.Current Treatment Options in Oncology. 2006; 7: 13-22.
2. Crist W, Gehan EA, Raqab AH, Dickman PS, Donaldson SS,et al. The third intergroup rhabdomyosarcoma study. Journal ofClinical Oncology. 1995; 13: 610-630.
3. Maurer HM, Gehan EA, Beltangady M, Crist W, Dickman PS,et al. The Intergroup Rhabdomyosarcoma Study-II. Cancer. 1993;71: 1904-1922.
4. Terezakis SA, Wharam MD. Radiotherapy forrhabdomyosarcoma: indications and outcome. Clinical Oncology.2013; 25: 27-35.
5. Day PF, Kindelan SA, Spencer JR, Kindelan JD, Duggal MS.Dental trauma: part 2. Managing poor prognosis anterior teeth-treatment options for the subsequent space in growing patients.Journal of Orthodontics. 2008; 55: 143-155.
6. Kim E, Jung JY, Cha IH, Kum KY, Lee SJ. Evaluation of theprognosis and causes of failure in 182 cases of autogenous toothtransplantation. Oral Surgery Oral Medicine Oral Pathology OralRadiology and Endodontology. 2005; 100: 112-119.
7. Sugai T, Yoshizawa M, Kobayashi T, Ono K, Takagi R, et al.Clinical study on prognostic factors for autotransplantation of teethwith complete root formation. International Journal of Oral andMaxillofacial Surgery. 2010; 39: 1193-1203.
8. Waldon K, Barber KS, Spencer JR, Duggal MS. Indicationsfor the use of auto-transplantation of teeth in the child andadolescent. European Archives of Paediatric Dentistry. 2012; 13:210-216.
9. Lundberg T, Isaksson S. A clinical follow-up study of 278autotransplanted teeth. British Journal of Oral and MaxillofacialSurgery. 1996; 34: 181-185.
10. Czochrowska EM, Stenvik A, Bjercke B, Zachrisson BU.Outcome of tooth transplantation of premolars to replace maxillaryincisors: a comparison with natural incisors. American Journal ofOrthodontics & Dentofacial Orthopedics. 2002; 121: 110-119.
11. Andreasen JO, Paulsen HU. A long term study of 370autotransplanted premolars. European Journal of Orthodontics.1990; 12: 38-50.
12. Nethander G. Periodontal conditions if teeth autogeneouslytransplanted by a two-stage technique. Journal of PeriodontalResearch. 1994; 29: 250-258.
13. Dholam KP, Gurav SP. Dental implants in irradiated jaws: Aliterature review. Journal of Cancer Research and Therapeutics.2012; 8: S85-S93.
14. Javed F, Al-Hezaimi K, Al-Rasheed A, Alamas K, RomanosGE. Implant survival rate after oral cancer therapy: A review. OralOncology. 2010; 46: 854-859.
15. Ohba S, Yoshimura H, Kobayashi J, Ishimaru K, Matsuda S,et al. The influence of radiation therapy and hyperbaric oxygentherapy on osteoradionecrosis of the Jaw. Journal of Hard TissueBiology. 2013; 22: 147-152.
OHDM- Vol. 14- No.5-October, 2015
321

16. Colella G, Gannavale R, Pentenero M, Gandolfo S. Oralimplants in radiated patients: A systematic review. InternationalJournal of Oral & Maxillofacial Implants. 2007; 22: 616-622.
17. Silverman S Jr, Chierici G. Radiation therapy of oralcarcinoma. I. Effects on oral tissues and management of theperiodontium. Journal of Periodontology. 1965; 36: 478-484.
18. Ammajan RR, Joseph R, Rejeev R, Choudhary K,Vidhyadharan K. Assessment of periodontal changes in patientsundergoing radiotherapy for head and neck malignancy: A hospital-based study. Journal of Cancer Research and Therapeutics. 2013; 9:630-636.
19. Marx RE. Osteoradionecrosis: a new concept of itspathophysiology. Journal of Oral and Maxillofacial Surgery. 1983;41: 283-288.
20. Dreizen S, Daly TE, Drane JB, Brown LR. Oralcomplications of cancer radiotherapy. Postgraduate Medicine. 1977;61: 85-92.
21. Fiorentino G, Vecchione P. Multiple congenitally missingteeth: treatment outcome with autologous transplantation andorthodontic space closure. American Journal of Orthodontics &Dentofacial Orthopedics. 2009; 135: 375-379.
22. Ziegler S, Neukam FW. Regional odontodysplasia:Orthodontic treatment and transplantation of premolars. AmericanJournal of Orthodontics & Dentofacial Orthopedics. 2012; 142:710-719.
23. Park SY, Choi SC, Choi BJ, Kim SJ, Park JH. Theautotransplantations and orthodontic treatment of multiplecongenitally missing and impacted teeth. Journal of ClinicalPediatric Dentistry. 2012; 36: 329-334.
24. Brook AH. An epidemiological study of dental anatomies inEnglish schoolchildren with a detailed clinical and genetic study of aselected group. International Journal of Paediatric Dentistry. 2001;11: 171-178.
25. Mӧller P, Perrier M. Dento-maxillofacial sequelae in a childtreated for a rhabdomyosarcoma in the head and neck. Oral SurgeryOral Medicine Oral Pathology Oral Radiology and Endodontology.1998; 86: 297-303.
26. Yokoo S, Komori T, Watatani S, Shibuya Y, Komurasaki H,et al. Indications and procedures for segmental dentoalveolarosteotomy: a review of 13 patients. International Journal of AdultOrthodontics & Orthognathic Surgery. 2002; 17: 254-263.
OHDM- Vol. 14- No.5-October, 2015
322
Related Documents