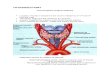
Nursing management of client on mechanical ventilator

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Nursing management of client on mechanical
ventilator

MECHANICAL
VENTILATOR
Mechanical ventilation is a life
saving intervention in the
emergency department. It
functions as a supportive
measure for patients during
acute illness.

INDICATIONS
• Failure of ventilation
1. Neuromuscular disease
2. Central nervous system disease
3. CNS depression
4. Musculoskeletal disease
5. Thoracic malformation/ trauma
• Disorders of pulmonary gas exchange
1. Acute respiratory failure
2. Chronic respiratory failure
3. Left ventricular failure
4. Pulmonary disease resulting in difusion or
perfusion abmornality

• An endotracheal
(ET)/tracheostomy tube is
needed for mechanical
ventilation.

Articles for intubation


Intubation procedure
• Head positioning
• The laryngoscope
• Endotracheal tube advancement
• Cuff inflation
• Conforming position
• Securing the tube
• NG tube insertion
• Connect to ventilator

Pre- ventilator preparations

1. Confirms physician’s orders
2. Washes hands
3. Selects, gathers and assembles
ventilator circuitry before bringing it to the
patientʼs bedside
4. Fills humidifier with sterile water (or
attaches HME to external circuit)
5. Introduces self, identifies patient

6. Explains procedure and confirms patient
understanding, if appropriate
7. Brings ventilator to bedside
8. Connects ventilator to test lung
9. Sets ventilator controls according to
physician orders
10.Connects ventilator to test lung
11.Confirms proper ventilator function

12. Connects patient to ventilator during the
expiratory phase
13. Fills ETT with air to minimal leak or to
appropriate cuff pressure by gauge
14. Checks for chest expansion and
bilateral breath sounds
15. Sets all alarm and monitoring functions

16. Uses respirometer to measure exhaled
tidal volume
17. Analyzes FIO2
18. Assesses patient response
19. Charts pertinent data
20. Draws or has drawn an ABG in 15-30
minutes
•

21. Readjusts ventilation parameters
according to ABG results
22. Repeats steps 18-21 until patient
stabilizes

Principles of nursing care
• Ensure Patient safety
– Patient assessment/Monitoring
– Prevent and treat complications
• Ensure Patient comfort
– Position
– Hygiene
– Feeding
– Management of stressors
– Pain and sedation management

ASSESSING THE EQUIPMENT
In monitoring the ventilator, the nurse should
note the following:
• Type of ventilator (such as volume-cycled,
pressure-cycled, negative-pressure)
• Controlling mode (such as controlled
ventilation, assist– control ventilation,
synchronized intermittent mandatory
ventilation)

• Tidal volume and rate settings (tidal
volume is usually 10 to 15 mL/kg; rate is
usually 12 to 16/min)
• FiO2 (fraction of inspired oxygen) setting
• Inspiratory pressure reached and pressure
limit (normal is 15 to 20 cm H2O; this
increases if there is increased airway
resistance or decreased compliance)

• Sensitivity (a 2-cm H2O inspiratory force
should trigger the ventilator)
• Inspiratory-to-expiratory ratio (usually 1:3
[1 second of inspiration to 3 seconds of
expiration] or 1:2)
• Minute volume (tidal volume × respiratory
rate, usually 6 to 8 L/min)
• Sigh settings (usually 1.5 times the tidal
volume and ranging from 1 to 3 per hour),
if applicable

• Water in the tubing, disconnection or
kinking of the tubing
• Humidification (humidifier filled with water)
and temperature
• Alarms (turned on and functioning
properly)
• PEEP and/or pressure support level, if
applicable. PEEP is usually 5 to 15 cm
H2O

Initial Ventilator Settings
1. Set the machine to deliver the tidal
volume required (10 to 15 mL/kg).
2. Adjust the machine to deliver the lowest
concentration of oxygen to maintain
normal PaO2 (80 to 100 mm Hg). This
setting may be high initially but will
gradually be reduced based on arterial
blood gas results.
3. Record peak inspiratory pressure.

4. Set mode (assist–control or synchronized
intermittent mandatory ventilation) and
rate according to physician order Set
PEEP and pressure support if ordered.
5. Adjust sensitivity so that the patient can
trigger the ventilator with a minimal effort
(usually 2 mm Hg negative inspiratory
force).

6. Record minute volume and measure
carbon dioxide partial pressure (PCO2),
pH, and PO2 after 20 minutes of
continuous mechanical ventilation.
7. Adjust setting (FiO2 and rate) according
to results of arterial blood gas analysis to
provide normal values or those set by the
physician.

8. If the patient suddenly becomes confused
or agitated or begins bucking the ventilator
for some unexplained reason, assess for
hypoxia and manually ventilate on 100%
oxygen with a resuscitation bag.

Trouble shoting alarams of ventilation
Display
message
Possible Cause Remedy
HIGH
CONTINOU
S
PRESSURE
CHECK
TUBING
AIRWAYS
PRESSURE
TOO HIGH
Airway is higher than set
PEEP plus 15 cm H2O for
more than 15 sec.
Disconnected pressure
transducer block pressure
transducer Water in
expiratory limb. Wet bacterial
filter clogged bacterial filter.
Kinked/blocked tubing.
Mucus or secretion plug in
ETT or airways client
coughing or fighting.
Check client, Check circuit
Check ventilator setting and
alarm limit.
Check ventilator internal
replace filter, remove water
from tubing Check heater
wire. Refer to service.
Check client, Check
ventilator setting and alarm
limit.

Display
message
Possible Cause Remedy
LIMITED
PRESSURE
EXPRIED
MINUTE
VOLUME TOO
HIGH
EXPRIED
MINUTE
VOLUME TOO
LOW
Kinked/blocked Mucus in
tubing coughing / fighting
patient.
Increased client activity
ventilator auto cycling.
Improver alarm setting low
flow transducer.
Low spontaneous client
breathing activity. Leakage
in cuff. Improver alarm
setting.
Check client, Check ventilator
setting and alarm limit.
Check client Check trigger
sencesitivity and alarm
setting. Dry the flow
transducer.
Check client cuff pressure
circuit pause time and
graphics.

Display
message
Possible Cause Remedy
EXPRIED MINUTE
VOLUME DISPLAY
READS
APNEA ALARM
PEEP/CPAP & OR
PLATEAV
PRESSURE FAILS
TO BE MAINTAIN
Flow transducer faulty
Circuit disconnected from
client
Time between two
consecutive insperatory
effort exceeds.
Adult : 20 sec.
Pead : 15 sec.
Neonate : 10 sec
Leakage in cuff and client
circuit Improper alarm limit
setting.
Replace flow transducer
connect Y piece to
client.
Check client and
ventilator setting
Check cuff pressure
Check client circuit
check pause time and
graphics to verify
consider more
ventilatory support .

Initial Patient assessment
• Airway
• Stability/Patency of ETT
• Length of fixing
• CXR
• Breathing
• Chest expansion, breath sounds, synchrony
• Circulation
• Colour, warmth of extremities, pedal pulses

Systems assessment
• CVS
• CNS
• Renal function
• Gastro intestinal
• Metabolic
• Skin
• Color,pulse,HR,BP
• Sedation ,paralysis
• Urine output
• Abdominal distension,
gastric
aspirates,bowel
sounds
• Temperature,blood
sugar levels
• Integrity,pressure
sores

Position
• Compared to supine position,
semirecumbent positioning (head of bed
elevation > 30degree) reduces the
frequency and risk for nosocomial
pneumonia

Prevent and treat complications
•The use of thrombo prophylaxis is
effective for preventing deep venous
thrombosis (DVT).
•The use of peptic ulcer disease (PUD)
prophylaxis reduces the risk of upper
gastro-intestinal bleeding.
•Patients should have secretion
checks at least 2 hourly and be
suctioned if required. Each patient with
tracheostomy should receive adequate
humidification.
• This should be checked and
documented 2 hourly. Inner tube
should be removed, checked for
secretion build up, cleaned, and
replaced 4 hourly.

Prevent and treat complications
• Availability of safety equipment relating to
tracheostomy should be checked at the
beginning of each shift.
• (S-Suction catheter/apparatus; A-Airway; L-
Laryngoscope; T-Tube-Endotracheal and
tracheostomy tubes; Bougie; T tracheal dilator;
Laryngeal mask airway (LMA).
• Cuff pressure should be checked during each
shift.
• It is to be kept at 20 cm H2O pressure. Dressing
and tape should be changed once a day.

Humidification
• Inspired gas
temperature 35-37 0
C
• Maintain waterlevel
• Circuit
condensate/empty
water trap

Patient comfort
• HOB elevation 30-450
• Repositioning /Passive
limb exercises
• Pain control and
sedation
• Prevent pressure sores
• Wound care
• Hygiene-Eye
care/Mouth care, Body
care

Feeding
• Enteral feeding always!!
• Check position of NGT
• Continuous /Bolus
feeds
• Assessing feed
intolerance?
• Interruption of feeds
• Feeding in prolonged
ventilation

Endotracheal suctioning
• Two nurses/ Physician in sick patients
• Top up sedation
• Hand hygiene/Sterile gloves

Care during suctioning
• Preoxygenation, sedation, and
reassurance are necessary before suction
to avoid suction-induced hypoxemia.
• Diameter of suction catheter should not
exceed half of the inner diameter of the
airway. Larger catheters can cause
mucosal trauma. A smaller catheter may
be ineffective at removing secretions

• It is necessary to pre-measure the suction
catheter insertion distance for 0.5-1 cm
past the distal end of the endotracheal or
tracheostomy tube (same sized new
endotracheal/tracheostomy tube may be
used for this purpose).
• Suction gauge should be adjusted to 80-
120mm Hg. Hypoxia, trauma, and
atelectasis, can result from suctioning with
negative pressure > 150mm Hg.

• Hyperoxygenating the patient before and
after suctioning will decrease the chance
of hypoxia related dangers (cardiac
arrhythmias, bradycardia, seizures,
cardiac arrest).
• Squeezing the manual ventilating bag 4-6
times with 100% O2 before suctioning will
help open the alveoli and lessen
desaturation.

Nursing diagnosis
• Impaired gas exchange related to
underlying illness, or ventilator setting
adjustment during stabilization or weaning.
• Ineffective airway clearance related to
increased mucus production associated
with continuous positive-pressure
mechanical ventilation


• Risk for trauma and infection related to
endotracheal intubation or tracheostomy
• Impaired physical mobility related to
ventilator dependency
• Impaired verbal communication related to
endotracheal tube and attachment to
ventilator
• Defensive coping and powerlessness
related to ventilator dependency

COLLABORATIVE PROBLEMS/ POTENTIAL
COMPLICATIONS
• Alterations in cardiac function
• Barotrauma (trauma to the alveoli) and
pneumothorax
• Pulmonary infection
• Sepsis

VAP prevention bundle
• Daily sedation vacation
• All patients will be assessed for weaning
and extubation each day
• Avoid supine position aiming to have the
patient at least 30 head up
• Prevent aspiration of gastric contents
• Use chlorhexidine as part of daily mouth
care

• Frequent suctioning of subglottic
secretions in patients on ventilators
• Stress ulcer prophylaxis / Reduce
colonization of aero digestive tract

Altered skin integrity
• Reposition second hourly to
prevent pressure sores and joint
stiffness and deformities
• Provide range of motion
exercises.
• Skin should be kept dry
• Use alpha bed
• ET tube should be repositioned at
alternate sides of the mouth to
prevent pressure ulcers.
• NG tube should be fixed in such a
way as to minimize pressure on
the nares and plaster should be
changed daily

WEANING
• Physician orders
• Reverse paralysis
• Decrease sedation
• Stop feeds/4 hrs/start MF
• Decrease in RR/spontaneous modes
• Preventing airway edema
• Is the patient comfortable?

Weaning parameters
• Awake& alert
• PEEP 5cmH2O
• PaO2>60 mmHg on Fio2 50%
• Pao2 acceptable with PH of 7.35-7.45
• Spontaneous inspiratory force of at least
20 cm of H2O
• Stable vital signs
• Adequate nutrition

Factors to correct before weaning starts
• Acid base abnormality
• Altered level consciousness
• Anaemia
• Arrhythmia
• Decreased cardiac out put
• Electrolyte abnormality
• Fluid imbalance

• Hyperglycemias
• Infection
• Renal failure
• Protein loss
• Shock
• Sleep deprivation

COMPLICATIONS
Cervical spine injury
in patients with
unstable cervical
spine,
Esophageal
intubation,
Right main bronchial
intubation,
Aspiration of gastric
contents
Perintubation :-
laryngeal trauma,
Pharyngeal trauma,
Tracheal or bronchial
rupture,
Epistaxis,
Tooth trauma,
Arrhythmias
Bronchospasm

During mechanical ventilation
Endotracheal tube
obstruction,
Airway drying leading
to inspissations of
airway secretions,
Endotracheal tube
migration,
Self extubation,
Cuff leak,
Ventilator induced
lung injury------
barotraumas
volutrauma
biotrauma

Evidence based practice

CONCLUSION
• Patients on ventilator need constant
observation and skilled care to protect,
restore and maintain their health. Nursing
care challenging, compassionate care is
the corner stone of nursing management
of ventilator patient .

Thank you
Related Documents