“as a newly qualified nurse, it also helped me to understand about venous insufficiency. I don’t feel so scared when I’m in the LU clinic” - CSN “I often have no access to Doppler results in the patients house. If they have a passport I can see it before I apply compression” - SCN 2017 My Venous Leg Ulcer : Patient Passport Liz Ettridge, Tissue Viability Nurse, Tissue Viability and Wound Therapy Service, Medway Community Healthcare. Introduction The number of leg ulcer patient in the UK continues to grow and with this comes additional strain on the health service, both in terms of capacity and in service provision (Guest et al 2017). Leg ulcer care may be carried out by a range of clinicians in the healthcare setting including leg ulcer specialist nurses, community nurses and practice nurses (Guest et al 2017). There is also a need to encourage patient empowerment through better knowledge of their conditions and greater involvement in their own care as mentioned in the five year forward view (NHS England 2015). As is common in the UK, the remit for care of patients with leg ulcers at Medway Community Healthcare (MCH) lies within the community nursing service. This includes running the leg ulcer clinics and seeing housebound patients. The difficulty in recruitment and retention of community staff has had an impact on lower limb management within Medway Community Healthcare. Tissue Viability provide in house training aimed at new staff in order to manage the issues of staff education in leg ulcer management, however due to poor staff retention there is a lack of expertise among community nurses. Method Local Tissue Viability Teams have implemented Pathways of Care for leg ulcers to help guide nurses, however, staffing problems often meant leg ulcer clinics are staffed with inexperienced nurses who are not always confident to effectively educate patients. Often the only person in attendance at every visit is the patient, therefore there is a need to invest in patient education to fully understand their leg problem and need for compression therapy, to enable full partnership in their management including the assessment process and plan of care. MCH have in the past introduced patient passports for pressure ulcers and catheter care, to enable education and continuity of care between health care settings. In order to address some of the issues mentioned above MCH developed “My venous leg problem passport” which was introduced in similar way to those already in use. The idea of the passport is to bring all the key elements of patient leg ulcer management together in one document. The passport contains patient education, including the rationale for the assessment, treatment options and aftercare. It is intended to enable the patient to have the understanding to take ownership of their chronic condition (expert patient). There is also an area to document the Doppler result and compression details and when and how to seek help. It is designed for the patient to be able to fill in their own details, to prevent added pressure on nursing time. The patient can show the passport to any health care professional in other settings, such as hospital admissions or while travelling, to give patient the confidence that their plan of care is being continued. L&R have sponsored the idea, giving valuable advice and produced laminated booklets the size of a passport. Wounds UK, Harrogate 2017. This e-poster was kindly produced by L&R. Results The booklets were first introduced to our champion link community nurses, while undertaking a level 6 lower limb module in March 2017. They then promoted their use and cascaded to all community nurses. On evaluation, they have proved very popular with patients and staff, particularly in the 4 leg ulcers clinics across the organization. It is too early to see if has impacted of healing rates. 'it really helped me to remember what the nurse explained about my leg problem.” - Patient I know what treatment I’m supposed to have so can let the new nurses know” - Patient Conclusion The booklets were first introduced to our champion link community nurses, while undertaking a level 6 lower limb module in March 2017. They then promoted their use and cascaded to all community nurses. On evaluation, they have proved very popular with patients and staff, particularly in the 4 leg ulcers clinics across the organization. It is too early to see if has impacted of healing rates. “I love them, all my patients have them now and I often quiz them on their knowledge” - Champion

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
“as a newly qualified nurse, it also helped me to understandabout venous insufficiency.
I don’t feel so scared when I’m in the LU clinic” - CSN
“I often have no access toDoppler results in the patientshouse. If they have a passport I can see it before I applycompression” - SCN
2017
My Venous Leg Ulcer : Patient Passport Liz Ettridge, Tissue Viability Nurse, Tissue Viability and Wound Therapy Service, Medway Community Healthcare.
Introduction
The number of leg ulce
r patient in the UK con
tinues
to grow and with this
comes additional strain
on the
health service, both in
terms of capacity and
in
service provision (Gue
st et al 2017). Leg ulce
r care
may be carried out by
a range of clinicians i
n the
healthcare setting incl
uding leg ulcer specia
list
nurses, community nurs
es and practice nurse
s
(Guest et al 2017). Th
ere is also a need to
encourage patient em
powerment through b
etter
knowledge of their co
nditions and greater
involvement in their ow
n care as mentioned in
the
five year forward view
(NHS England 2015).
As is common in the U
K, the remit for care o
f
patients with leg ulcer
s at Medway Commun
ity
Healthcare (MCH) lies
within the community
nursing
service. This includes
running the leg ulcer c
linics
and seeing housebou
nd patients. The difficu
lty in
recruitment and reten
tion of community staf
f has
had an impact on lowe
r limb management wit
hin
Medway Community H
ealthcare. Tissue Viabi
lity
provide in house trainin
g aimed at new staff i
n order
to manage the issues
of staff education in le
g ulcer
management, howeve
r due to poor staff rete
ntion
there is a lack of exper
tise among communit
y
nurses.
MethodLocal Tissue Viability Teams have implemented Pathways ofCare for leg ulcers to help guide nurses, however, staffingproblems often meant leg ulcer clinics are staffed withinexperienced nurses who are not always confident to effectivelyeducate patients.
Often the only person in attendance at every visit is the patient,therefore there is a need to invest in patient education to fullyunderstand their leg problem and need for compression therapy,to enable full partnership in their management including theassessment process and plan of care. MCH have in the pastintroduced patient passports for pressure ulcers and cathetercare, to enable education and continuity of care between healthcare settings.
In order to address some of the issues mentioned above MCHdeveloped “My venous leg problem passport” which wasintroduced in similar way to those already in use.
The idea of the passport is to bring all the key elements ofpatient leg ulcer management together in one document.
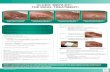
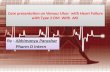
The passport contains patient education, including the rationalefor the assessment, treatment options and aftercare. It isintended to enable the patient to have the understanding to takeownership of their chronic condition (expert patient). There isalso an area to document the Doppler result and compressiondetails and when and how to seek help. It is designed for thepatient to be able to fill in their own details, to prevent addedpressure on nursing time. The patient can show the passport toany health care professional in other settings, such as hospitaladmissions or while travelling, to give patient the confidence thattheir plan of care is being continued.
L&R have sponsored the idea, giving valuable advice andproduced laminated booklets the size of a passport.
Wounds UK, Harrogate 2017. This e-poster was kindly produced by L&R.
ResultsThe booklets
were first introduced to our
champion link
community nurses, while un
dertaking a level 6 lower limb
module in March 2017. The
y then promoted their use a
nd
cascaded to all community n
urses. On evaluation, they h
ave
proved very popular with pa
tients and staff, particularly i
n
the 4 leg ulcers clinics acros
s the organization. It is too e
arly
to see if has impacted of hea
ling rates.
'it really helped me to rememberwhat the nurse explained about
my leg problem.” - Patient
I know what treatment I’msupposed to have so can let thenew nurses know” - Patient
ConclusionThe booklets were first introduced to our champion linkcommunity nurses, while undertaking a level 6 lower limbmodule in March 2017. They then promoted their use andcascaded to all community nurses. On evaluation, they haveproved very popular with patients and staff, particularly inthe 4 leg ulcers clinics across the organization. It is too earlyto see if has impacted of healing rates.
“I love them, all my patients have them now and I often quiz
them on their knowledge”- Champion
Related Documents