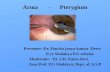
CHAPTER I INTRODUCTION A pterygium is an elevated, superficial, external ocular mass that usually forms over the perilimbal conjunctiva and extends onto the corneal surface. Pterygia can vary from small, atrophic quiescent lesions to large, aggressive, rapidly growing fibrovascular lesions that can distort the corneal topography, and, in advanced cases, they can obscure the optical center of the cornea. A pterygium commonly grows from the nasal side of the sclera. It is usually present in the palpebral fissure. It is associated with, and thought to be caused by ultraviolet-light exposure (e.g., sunlight), low humidity, and dust. 1

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

CHAPTER I
INTRODUCTION
A pterygium is an elevated, superficial, external ocular mass that usually
forms over the perilimbal conjunctiva and extends onto the corneal surface.
Pterygia can vary from small, atrophic quiescent lesions to large, aggressive,
rapidly growing fibrovascular lesions that can distort the corneal topography, and,
in advanced cases, they can obscure the optical center of the cornea.
A pterygium commonly grows from the nasal side of the sclera. It is
usually present in the palpebral fissure. It is associated with, and thought to be
caused by ultraviolet-light exposure (e.g., sunlight), low humidity, and dust.
1

CHAPTER II
LITERATURE REVIEW
2.1. Conjunctiva
The conjunctiva is the mucous membrane lining the eyelids and
reflecting onto the sclera of the anterior surface of the eye.1
A transparent mucous membrane, known as the conjunctiva, lines
the inner surface of the eyelids (palpebral conjunctiva) and covers the
sclera of the anterior portion of the eye (bulbar conjunctiva). The
conjunctiva is composed of a stratified columnar epithelium that contains
goblet cells overlying a basal lamina and a lamina propria composed of
loose connective tissue. Secretions of the goblet cells become a part of the
tear film, which aids in lubricating and protecting the epithelium of the
anterior aspect of the eye. At the corneoscleral junction, where the cornea
begins, the conjunctiva continues as the stratified squamous corneal
epithelium and is devoid of goblet cells. 1
Figure 1 Conjunctiva
2.2. Cornea
The cornea is the transparent, avascular, and highly innervated
anterior portion of the fibrous tunic that bulges out anteriorly from the
orb. It is slightly thicker than the sclera and is composed of five
histologically distinct layers1:
2

Corneal epithelium
Bowman's membrane
Stroma
Descemet's membrane
Corneal endothelium
The corneal epithelium, the continuation of the conjunctiva (a
mucous membrane covering the anterior sclera and lining the internal
surface of the eyelids), is a stratified, squamous, nonkeratinized
epithelium, composed of five to seven layers of cells, that covers the
anterior surface of the cornea. The larger superficial cells have microvilli
and exhibit zonulae occludentes. The remaining cells constituting the
corneal epithelium interdigitate with and form desmosomal contacts with
one another. Their cytoplasm contains the usual array of organelles along
with intermediate filaments. The corneal epithelium is highly innervated
by numerous free nerve endings. Mitotic figures are observed mostly near
the periphery of the cornea, with a turnover rate of approximately 7 days.
Damage to the cornea is repaired rapidly as cells migrate to the defect to
cover the injured region. Subsequently, mitotic activity replaces the cells
that migrated to the wound. The corneal epithelium also functions in
transferring water and ions from the stroma into the conjunctival sac.1
Bowman's membrane lies immediately deep to the corneal
epithelium. Electron micrographs reveal it to be a fibrillar lamina, 6 to 30
μm thick, composed of type I collagen fibers arranged in an apparently
random fashion. It is believed that Bowman's membrane is synthesized by
both the corneal epithelium and cells of the underlying stroma. Sensory
nerve fibers pass through this structure to enter and terminate in the
epithelium.1
The transparent stroma is the thickest layer of the cornea,
constituting about 90% of its thickness. It is composed of collagenous
connective tissue, consisting mostly of type I collagen fibers that are
arranged in 200 to 250 lamellae, each about 2 μm in thickness. The
3

collagen fibers within each lamella are arranged parallel to one another,
but fiber orientation shifts in adjacent lamellae. The collagen fibers are
interspersed with thin elastic fibers, embedded in ground substance
containing mostly chondroitin sulfate and keratan sulfate. Long, slender
fibroblasts are also present among the collagen fiber bundles. During
inflammation, lymphocytes and neutrophils are also present in the stroma.
At the limbus (sclerocorneal junction) is a scleral sulcus whose inner
aspect at the stroma is depressed and houses endothelium-lined spaces,
known as the trabecular meshwork, that lead to the canal of Schlemm.
The canal of Schlemm is the site of outflow of the aqueous humor from
the anterior chamber of the eye into the venous system.1
Descemet's membrane is a thick basement membrane interposed
between the stroma and the underlying endothelium. Although this
membrane is thin (5 μm at birth) and homogeneous in younger persons,
electron microscopy has demonstrated that it becomes thicker (17 μm)
and has cross-striations and hexagonal fiber patterns in older adults.1
The corneal endothelium, which lines the internal (posterior)
surface of the cornea, is a simple squamous epithelium. It is responsible
for synthesis of proteins that are necessary for secreting and maintaining
Descemet's membrane. These cells exhibit numerous pinocytotic vesicles,
and their membranes have sodium pumps that transport sodium ions
(Na+) into the anterior chamber; these ions are passively followed by
chloride ions (Cl-) and water. Thus, excess fluid within the stroma is
resorbed by the endothelium, keeping the stroma relatively dehydrated, a
factor that contributes to maintaining the refractive quality of the cornea.1
4

Figure 2 Cornea
2.3. Pterygium
2.3.1. Definition
Pterygium is a fibrovaskuler growth of conjunctiva which is
degenerative and invasive.2
2.3.2. Epidemiology
The prevalence rates of pterygium obtained for a number of
populations vary widely, from 1.2% in urban, temperate white
people3 to 23.4% in the black population of tropical Barbados.4
These study populations differ in race, latitude, and sun exposure,
but generally prevalence rates in the tropics are higher than at
temperate latitudes. Research in Indonesia in Riau showed 17.0%
prevalence of pterygium.5
5

2.3.3. Risk Factors
Risk factors that influence the occurrence of pterygium is:
1. Age
It is uncommon for patients to present with pterygium prior
to age 20 years. Patients older than 40 years have the highest
prevalence of pterygia.6
2. Ultraviolet light exposure
There is close relationship between pterygium and
ultraviolet rays in ophthalmology. The incidence of pterygium
is much higher in outdoor workers who are working for long
hours in the sun-belt area. Ultraviolet light which plays a role
in pterygium is ultraviolet B. UV-B rays can cause chronic
inflammatory reactions that formed fibrovaskular tissue.7
3. Geographic
Several surveys have shown that the countries nearer the
equator have higher rate of pterygium than the other regions,
the possible reason is due to stronger exposure to ultraviolet
rays.6
4. Gender
Pterygium are reported to occur in males twice as
frequently as in females.6
5. Hereditary
In black african, there was a positive family history of
pterygium in 36% of cases. In Australia 38% of patients
admitted for pterygium surgery compared with 8 - 12% of
controls admitted for other conditions had a family history of
the growth. In South Africa 30 - 35% of urban predominantly
white individuals who had attended an ophthalmic practice
because of pterygium had a positive family history.8
6. Microtrauma
6

Mikrotrauma because of certain particles such as cigarette
smoke, dust and sand is one of the risk factors for pterygium.
Mikrotrauma a trigger of chronic inflammation that causes the
occurrence of pterygium.6
2.3.4. Pathogenesis and Pathophysiology
A central process in pterygium pathogenesis is thought to
be matrix metalloproteinase (MMP) activation by ultraviolet light
(UV) and subsequent MMP activity against interstitial tissue. A
number of MMP’s are involved but MMP–1 is abundantly
expressed in pterygium.9
The pathophysiology of pterygia is characterized by
elastotic degeneration of collagen and fibrovascular proliferation,
with an overlying covering of epithelium. Histopathology of the
abnormal collagen in the area of elastotic degeneration shows
basophilia with hematoxylin and eosin stain. This tissue also stains
with elastic tissue stains, but it is not true elastic tissue, in that it is
not digested by elastase.6
2.3.5. Staging
Based on the degree of growth, the pterygium can be classified
into 4 stage10:
1. Stage 1
Fibrovaskular tissue growth confined to the limbus.
Figure 3 Stage 1 Pterygium
7

2. Stage 2
Fibrovaskular tissue growth has been through limbus but not
greater than 2 mm across the cornea.
Figure 4 Stage 2 Pterygium
3. Stage 3
Fibrovaskular tissue growth beyond 2 mm of the cornea, but
does not exceed the edge of the pupil of the eye.
Figure 5 Stage 3 Pterygium
4. Stage 4
Fibrovaskular tissue growth has been over the edge pupils.
Figure 6 Stage 4 Pterygium
8

Based on its location, pterygium generally classified into
unilateral and bilateral pterygium. Unilateral pterygium
pterygium is that only occurs in one eye, whereas bilateral
pterygium was found in both eyes. In addition, pterygium
pterygium also can be classified into the nasal, temporal, or nasal
and temporal part in one eye is commonly called kissing
pterygium.
Almost 97% pterygium in nasal. Only about 3% which is in
the temporal. In some cases, can be found kissing pterygium.The
predominance of pterygia on the nasal side is possibly a result of
the sun's rays passing laterally through the cornea, where it
undergoes refraction and becomes focused on the limbic area.
Sunlight passes unobstructed from the lateral side of the eye,
focusing on the medial limbus after passing through the cornea.
On the contralateral (medial) side, however, the shadow of the
nose medially reduces the intensity of sunlight focused on the
lateral/temporal limbus.9
2.3.6. Diagnosis
Patients with pterygia present with a variety of complaints,
ranging from no symptoms to significant redness, swelling, itching,
irritation, and blurring of vision associated with elevated lesions of
the conjunctiva and contiguous cornea in one or both eyes.11
The clinical presentation can be divided into 2 general
categories, as follows6:
One group of patients with pterygium can present with
minimal proliferation and a relatively atrophic appearance.
The pterygia in this group tend to be flatter and slow
growing and have a relatively lower incidence of recurrence
following excision.
9

The second group presents with a history of rapid growth
and a significant elevated fibrovascular component. The
pterygia in this group have a more aggressive clinical
course and a higher rate of recurrence following excision.
2.3.7. Complication
Complications of pterygium include visual impairment,
impaired eye movement, and dry eye. Visual impairment occurred
primarily in pterygium stage 3 and 4. Visual impairment in
pterygium mainly caused by the pull of the cornea, causing
astigmatism. Pterygium block the entry of light into the retina,
especially in pterygium who had passed the edge of the pupil of the
eye.6
Eyeball movement disorders can occur due to pterygium
causing adhesions and restrictions on movement of the eyeball.
Pterygium will cause the conjunctiva and sclera that loosely binds
become sticky so that movement of the eye becoming more
difficult. In addition, the existence of pterygium growth will cause
the area to the movement of the eyeball becomes smaller.6
Dry eye often occur in pterygium. This is caused by defects
of the tear film. Conjunctiva is one of the forming of the tear film.
Goblet cells in the conjunctiva will not produce a layer of tears if
the surface is covered by the pterygium. This is what causes dry
eye in the pterygium.6
2.3.8. Treatment
Patients with pterygia can be observed unless the lesions
exhibit growth toward the center of the cornea or the patient
exhibits symptoms of significant redness, discomfort, or alterations
in visual function. Pterygia can be removed for cosmetic reasons,
as well as for functional abnormalities of vision or discomfort.12
10

1. Medical Care
Medical therapy of pterygia consists of artificial tears/topical
lubricating drops as well as occasional short-term use of
topical corticosteroid anti-inflammatory drops when
symptoms are more intense.
Artificial tears provide topical ocular surface lubrication and
fill defects in the tear film, in patients with irregular corneal
surfaces and irregular tear films. These conditions are very
common in the setting of pterygium.
Topical corticosteroid is used to reduce inflammation on the
ocular surface and other ocular tissues. Corticosteroids can be
helpful in the management of inflamed pterygia by reducing
the swelling of the inflamed tissues of the ocular surface
adjacent to the lesions. 12
2. Surgical Care
Surgical care is indicated for stage 3 and stage 4 pterygium.
Removal of the pterygium involves surgical excision of the
head, neck and body of the pterygium. The body and base of
the pterygium are dissected with conjunctival scissors, while
the head and neck of the pterygium that has invaded the
cornea is often removed with a surgical blade. An attempt is
made to identify the plane of dissection, which facilitates
removal of the pterygium while keeping the underlying
corneal surface smooth. Remnant stromal attachments may be
smoothed out with the blade.
The surgical options available include the use of conjunctival
autograft, amniotic membrane transplant, and use of fibrin
glue.12
11

2.3.9. Prevention
Minimizing exposure to ultraviolet radiation should reduce
the risk of development of pterygia in susceptible individuals.
Patients are advised to use a hat or a cap with a brim, in addition to
ultraviolet-blocking coatings on the lenses of glasses/sunglasses to
be used in areas of sun exposure. This precaution is even more
important for those patients living in tropical or subtropical areas
or for those patients who are engaged in outdoor activities with a
high risk of ultraviolet exposure.6
2.3.10. Prognosis
The visual and cosmetic prognosis following excision of
pterygia is good. The procedures are well tolerated by patients,
and, aside from some discomfort in the first few postoperative
days, most patients are able to resume full activity within 48 hours
of their surgery.12
12

CHAPTER III
CASE
1. Patient identity
Name : Mr. K
Sex : Male
Age : 46 years old
Address : A. Yani 2 street Sungai Raya Kubu Raya
Ethnic : Melayu
Job : Laborer
Religion : Moslem
Patient was examined on Mei 23th, 2011
2. Anamnesis
a. Main complaint: blurry vision in right eye.
b. History of disease :
Patient complains blurry vision in right eye since 3 months ago, the left
eye did not. Both eyes red, itchy and watery. Patient work as a laborer for
construction of builing. He worked under the hot sun. His eyes are often
exposed to the splashes of cement.
c. Past clinical history: Patient claims that there is no history of the same
symptoms before.
d. Family history : There are no one of her family have the same complaint.
3. General Physical Assessment
General condition : good
Awareness : compos mentis
Vital Signs:
Heart Rate : 80x/minute
Respiration freq. : 18x/minute
Blood Pressure : 110/70 mmHg
13

Temperature : 36,5oC
4. Ophthalmological status
Visual acuity:
a. OD : 6/20F S – 0.75 C – 1.50 x 90o 6/6F
b. OS : 6/15 S – 0.75 C – 1.25 x 90o 6/6
OD OS
Right eye Left eye
ortho Eye ball position Ortho
ptosis (-), lagoftalmos
(-), edema (-)
Palpebra ptosis (-), lagoftalmos
(-), edema(-)
Redness (+),wing-like
growth from nasal
through limbus about 3
mm across the cornea.
Conjungtiva Redness (+), wing-like
growth from nasal
through limbus about 1
mm across the cornea.
Clear, edema (-) Cornea Clear, edema (-)
clear, deep COA clear, deep
Iris colour : brown
Pupil: circular, 3mm,
isokor, reactive to light
Iris and pupil Iris colour : brown
Pupil: circular, 3mm,
isokor, reactive to light
Clear Lens Clear
14

Clear Vitreous Clear
C/D ratio 0,4 Fundus C/D ratio 0,4
Eye ball movement
• Intraocular pressure (tonometry) : OD 13 mmHg, OS 14 mmHg
• Visual field test (confrontation) : normal
5. Resume
Patient complains of blurry vision in right eye since 3 months ago, the
left eye did not. Both eyes red, itchy and watery. Patient work as a laborer for
construction of builing. He worked under the hot sun. His eyes are often
exposed to the splashes of cement.
Vital signs of this patient are in normal range. Visual acuity of OD is
6/20F, after correction with S – 0.75 C – 1.50 x 90o 6/6F. Visual acuity of OS
is 6/15, after correction with S – 0.75 C – 1.25 x 90o 6/6. Conjunctiva of OD,
redness (+), wing-like growth from nasal through limbus about 3 mm across
the cornea. Conjunctiva of OS, redness (+), wing-like growth from nasal
through limbus about 1 mm across the cornea.
15
++
+
+
+
+
+
+
++
+
+
+
+
+
+
OD OS

6. Diagnose
Working Diagnose:
OD : Pterygium stage 3, myopia, pterygium induced astigmatism
OS : Pterygium stage 2, myopia, pterygium induced astigmatism
7. Plan for examination
- No plan for further examination.
8. Treatment:
- Non medicamentous: using of protective glasses, wear hat.
- Medicamentous: OC
o artificial tear 1-2 gtt prn, naphazoline eyedrop 0,1% 2-4 x 1gtt.
- Surgery: OD pterygium excision with conjunctival autograph.
9. Prognosis
OD
Ad vitam : bonam
Ad functionam : bonam
Ad sanactionam : dubia ad malam
OS
Ad vitam : bonam
Ad functionam : bonam
Ad sanactionam : dubia ad malam
16

CHAPTER IV
DISCUSSION
Mr. K, 46 years old, complains blurry vision in right eye since 3 months
ago, the left eye did not. Both eyes red, itchy and watery. Patient work as a laborer
for construction of builing. He worked under the hot sun. His eyes are often
exposed to the splashes of cement.
Abnormalities found in examination is redness and wing-like growth from
nasal through limbus in both eye. There is myopia and astigmatism in both eye
too. Working diagnose for this patient is pterygium based on the apparance of the
growth in conjunctiva, OD is pterygium grade 3, OS is pterygium grade 2. The
pterygium caused astigmatism in both eye.
Recomended therapy for this patient includes nonmedicamentous such as
wearing protective glasses and hat to protect from ultraviolet light and dust.
Medicamentous therapy for this patient is with artificial tear to lubricate the ocular
surface and to fill in defects in the tear film and topical vasoconstrictor to reduce
eye redness. Surgery is indicated for OD since the pterygium is grade 3.
17

CHAPTER V
CONCLUSION
Male, 46 years old, complaint blurry vision in right eye. Examination
reveal redness and wing-like growth in both eye. Working diagnose for this
patient is pterygium. The therapy include wearing protective glasses and hat,
artificial tear, topical vasoconstrictor and surgery.
18

REFERENCES
1. Gartner LP, Hiatt JL. Color Textbook of Histology. New York: WB Saunders,
2007.
2. Ilyas S. Ilmu Penyakit Mata edisi ketiga. Jakarta: Balai Penerbit FKUI, 2007.
3. Tan et al. Pterygium in white people of Melbourne, Australia. The British
Journal of Ophthalmology, 2003, 90(24):1201-5.
4. Saw et al. Pterygium in Barbados. The British Journal of Ophthalmology
2006; 92(02):909-914.
5. Tan et all. Epidemiology of pterygium on a tropical island in the Riau
Archipelago. Eye, 2006, 20 (8): 908-12.
6. Fisher JP, Trattler WB. 2011. Emedicine in Ophtalmology: Pterygium.
Dikunjungi pada 27 Mei 2011.
http://emedicine.medscape.com/article/1192527
7. Yan, et al. Relationship between the morbidity of pterygium and the duration
of ultraviolet rays exposure in Sanya, China. Chin Med J 2006; 119(15):1308-
1310.
8. Anguira P, Ntuli Sam, Carmichael T. Relationships of heredity and dry eye
with pterygia in black African patients. South African Medical Journal 2011;
101(2): 1.
9. Coroneo MT, et al. UVB Activated Pathways in Pterygium Pathogenesis.
Invest Ophthalmol Vis Sci 2005;46: 963-977.
10. Perhimpunan Dokter Spesialis Mata Indonesia (PERDAMI), Editor Tahjono.
Panduan Manajemen Klinik PERDAMI. Jakarta: CV Ondo, 2006.
11. Lang GK. Ophthalmology. A Short Textbook. New York: Thieme Stuttgart,
2000.
12. Leonard PK, et al. Current concepts and techniques in pterygium treatment.
Current Opinion in Ophthalmology 2007; 18:308–313.
19
Related Documents