INTRODUCTION TO RADICAL PROSTATECTOMY: Surgical Treatment for Prostate Cancer Dr. Alan So Associate Professor Dept of Urologic Sciences Vancouver Prostate Centre University of British Columbia Chair, GU Tumour Group at BC Cancer Biography: A graduate of the University of Alberta, Dr. So came to the Prostate Centre as a Clinical Fellow in 2002, following completion of his residency at Dalhousie University. His current research focuses on discovery and development of novel agents to treat bladder cancer as well as development of the mechanisms of treatment resistance in renal cell carcinoma. Currently, he is associate professor at the University of British Columbia and Vancouver Prostate Centre. As well, leads the Clinical Trials Unit at the Vancouver Prostate Cancer, is the Fellowship Director of the Uro-oncology Program at UBC, and is the Chair of the GU Tumour Group at the BC Cancer.

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

INTRODUCTION TO RADICAL PROSTATECTOMY:
Surgical Treatment for Prostate Cancer
Dr. Alan So
Associate Professor
Dept of Urologic Sciences
Vancouver Prostate Centre
University of British Columbia
Chair, GU Tumour Group at BC Cancer
Biography:
A graduate of the University of Alberta, Dr. So came to the Prostate Centre as a
Clinical Fellow in 2002, following completion of his residency at Dalhousie University.
His current research focuses on discovery and development of novel agents to treat
bladder cancer as well as development of the mechanisms of treatment resistance in
renal cell carcinoma. Currently, he is associate professor at the University of British
Columbia and Vancouver Prostate Centre. As well, leads the Clinical Trials Unit at
the Vancouver Prostate Cancer, is the Fellowship Director of the Uro-oncology
Program at UBC, and is the Chair of the GU Tumour Group at the BC Cancer.

OVERVIEW
This presentation will cover the following:
• Anatomy of the prostate
• Description of Radical Prostatectomy
• Open Radical Prostatectomy
• Laparoscopic Robotic Assisted Radical Prostatectomy
• Discussion of the Possible Side Effects of Radical Prostatectomy
• Follow-up after surgery

What is a Radical Prostatectomy
•“Radical” refers to surgery performed to remove cancer
•Radical prostatectomy is the removal of the prostate to treat prostate cancer and involves removal of:
•Prostate
•Seminal Vesicles
•Vas deferens
•Sometimes lymph nodes in the pelvis

ANATOMY OF THE PROSTATE

WHERE IS THE PROSTATE LOCATED?
The prostate gland is located deep
in the pelvis
• Below the bladder
• In front of the rectum
• Behind the pubic bone
• Surrounds the urethra
prostate
rectum
pubic bone
urethra
bladder

Who is best suited for a radical prostatectomy
•Men with disease that is confined to the prostate
•Medically fit for surgery
•> 10 year life expectancy
•Final decision: Informed Patient’s Choice

“LOCALIZED” PROSTATE CANCER
• When there is no evidence that the cancer has spread beyond
the prostate gland, it is considered “localized”. Localized
disease is:
• Treatable
• Slow growing in most men, which allows for time to choose a
treatment strategy
• We do not perform “radical prostatectomy” when prostate cancer has
spread, as this does not treat the cancer that has already spread

Tests Performed Prior to Surgery
•Sometimes, when there is suspected metastases (symptoms, high PSA or high Gleason Score) tests are performed before surgery:
•Bone Scan (to assess if cancer has spread to the bone)
•CT Scan (to assess if cancer has spread to the lymph nodes or other organs)
•MRI may also be ordered to help with surgical planning (nerve sparing)

SURGICAL OPTIONS FOR PROSTATECTOMY
• Open surgery (radical prostatectomy, RP)
• Laparoscopic Robotic assisted surgery (robotic RP)
• Laparoscopic RP
• Perineal

Advantages of surgery
•Overall well tolerated
•Excellent long term results
•Lymph nodes can be sampled
•Assessment of the prostate by the pathologist
•Avoidance of “aging” urinary problems

Other terminology:
•Nerve-sparing: the blood vessels and nerves that promote penile erections are left behind in the body and not taken out with the prostate
•Pelvic lymph node dissection: the lymph nodes surrounding and close to the prostate are taken out
The “Obturator” nodes are the ones usually taken out in
those at risk of having cancer spread to them

-Step 1: Removal of Prostate Gland, seminal vesicles, lymph nodes
-Step 2: Reconnection of the bladder to the urethra
Steps of surgery:

OPEN RP VS ROBOTIC RP
Incision for open
prostatectomy
Incisions for Laparoscopic
Prostatectomy

ROBOTIC PROSTATECTOMY
da Vinci® Surgical System
• 3-D visualization
• Surgeon direct instruments’ movements using
console controls
Compared to open surgery:
• Less bleeding
• Potential for earlier recovery of urinary control
• Reduced “scarring” of bladder / urethra
connection (called bladder neck contracture)

WHAT TO EXPECT AFTER SURGERY
• Hospital stay is usually 1 night
• Minimal to moderate discomfort
• Catheter in the penis to drain urine: 1-
2 weeks
• 3-6 weeks off work (depending on
type of work, more for manual or
physically active jobs)

ADVANTAGES of SURGERY
• Generally well tolerated, recovery within 4-8 weeks in most
• Lymph nodes can be sampled to check for spread of cancer
• Assessment by a pathologist of the entire prostate
• Removal of cancer in the prostate may have long term benefit as well
as short term psychological advantages
• Sometimes other additional treatments, such as radiation with or
without hormone therapy, are also required
• Removal of the prostate prevents benign prostatic hypertrophy (BPH)
related urinary problems

SIDE EFFECTS RELATED TO SURGERY
• Erectile dysfunction (ED):
- Depends on age and functional level before surgery
- Younger men with full function have the best chance at
recovery
- May also experience penile shortening

Erectile Dysfunction is due to damage to the erectile nerves
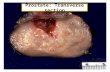
Cross-Section of Prostate
Rectum
Neurovascular Bundles of
Walsh
Prostate

Surgical Approach
•Sparing of nerves maximizes return of normal erections
•This approach may not be possible is there is :•Significant volume of tumor in the area of the nerves
•High grade tumor (aggressive disease) in the area of the nerves
•Climax and penile sensation not affected- just penile rigidity

MANAGING ERECTILE DYSFUNCTION
• Sometimes called sexual or penile rehabilitation
• Treatments may include:
• Medications
• Intraurethral suppositories
• Penile injections
• Vacuum devices
• Penile implants

SIDE EFFECTS RELATED TO SURGERY
• Incontinence:
• most experience incontinence during the first 3 months
• 1 in 10 men continue to have some level of stress
incontinence past a year but total loss of control is rare

MANAGING URINARY INCONTINENCE
• Although long-term incontinence may be rare, a majority of men
post-operatively will have some leakage of urine with straining /
coughing etc. (Stress incontinence)
• Management is initially conservative with Kegel Exercises to
strengthen the pelvic floor muscles
• Pelvic floor physiotherapy and biofeedback can be helpful to
maximize recovery
• If incontinence persists, surgical option may be helpful

Other potential rare side effects
• Blood transfusion: < 5 %
• Bladder neck scarring: rare
• Rectal injury: rare

HOW DO WE KNOW WHETHER TREATMENT IS WORKING?
Follow up visits
• PSA
• Expect it to be very low, if not
undetectable, 3 months after surgical
treatment
• After surgery, PSA should be undetectable

WHAT IF MY CANCER REOCCURS?
• Some of these treatment options can be explored, depending upon the
initial treatment and the nature of the recurrence, e.g.:
• Radiation to the pelvis
• Androgen deprivation

Conclusion
•Prostate cancer surgery for cure is called radical prostatectomy
•Surgery can be performed in those with localized disease
•There are different ways to perform radical prostatectomy
•There are some side effects that may be associated with surgery which can be treated with by your Urologist

Knight Cancer Instituteat Oregon Health & Science University
Advances In Radiation Therapy for Prostate Cancer
Arthur Y. Hung, M.D.
Associate Professor
Dept of Radiation Medicine
Knight Cancer Institute
Oregon Health & Science University
Biography:
Arthur Hung, M.D. is an associate professor of radiation
medicine and a associate professor of ophthalmology as well
as serves as medical director of the Radiation Therapy
Training Program. He received his medical degree at The
Ohio State University. Dr. Hung joined the faculty in 2002
after finishing his residency at the University of Texas – MD
Anderson Cancer Center.
His research is focused on developing and refining the latest
technology to deliver radiation with more effectiveness and
less toxicity than ever before possible and clinical interests
are in cancers of the genitourinary tract, gastrointestinal tract,
hepatobiliary system, soft tissue sarcomas, and melanomas.

Knight Cancer Instituteat Oregon Health & Science University
Advances in Radiation Therapy
• What is radiation?
• How does it work?
• How is the radiation delivered?
– External beam radiation
– Brachytherapy
– Intraoperative radiation
• Stereotactic Body Radiation Therapy
– as primary treatment for prostate cancer
– as treatment for metastatic prostate cancer

Knight Cancer Instituteat Oregon Health & Science University
Concepts of Radiation

Knight Cancer Instituteat Oregon Health & Science University
The Biological Effect of Radiation
• Radiation therapy uses high-energy electro-magnetic
energy, like radiowaves, microwaves, & visible light
• Ionizing Radiation damages DNA in rapidly dividing cells

Knight Cancer Instituteat Oregon Health & Science University
Radiation Damages DNA

Knight Cancer Instituteat Oregon Health & Science University
Normal Tissue repairs DNA Damage

Knight Cancer Instituteat Oregon Health & Science University
Advances in Radiation Therapy
Goal of treatment is to deliver radiation to just the prostate
• focusing the radiation on only the tumor eliminating collateral damage
to normal tissue
– External beam radiation
• Linear Accelerator
• Proton Therapy
• Stereotactic Body Radiation
– Internal Radiation
• Prostate Brachytherapy
• HDR Brachytherapy
– Intraoperative Radiation

Knight Cancer Instituteat Oregon Health & Science University
External Beam Radiation

Knight Cancer Instituteat Oregon Health & Science University
Modern Linear Accelerator

Knight Cancer Instituteat Oregon Health & Science University
Traditional Radiation Therapy

Knight Cancer Instituteat Oregon Health & Science University
Targeting Prostate Cancer with Radiation

Knight Cancer Instituteat Oregon Health & Science University
Focusing the Radiation
CT-Guided Targeting

Knight Cancer Instituteat Oregon Health & Science University
Intensity Modulated Radiation Therapy
IMRT

Knight Cancer Instituteat Oregon Health & Science University
Elekta Versa HD Accelerator

Knight Cancer Instituteat Oregon Health & Science University
Radiation Beam Shaping

Knight Cancer Instituteat Oregon Health & Science University
Cyberknife

Knight Cancer Instituteat Oregon Health & Science University

Knight Cancer Instituteat Oregon Health & Science University

Knight Cancer Instituteat Oregon Health & Science University

Knight Cancer Instituteat Oregon Health & Science University
Brachytherapy

Knight Cancer Instituteat Oregon Health & Science University
Prostate Brachytherapy

Knight Cancer Instituteat Oregon Health & Science University
Prostate Brachytherapy

Knight Cancer Instituteat Oregon Health & Science University
Brachytherapy

Knight Cancer Instituteat Oregon Health & Science University
Intraoperative Radiation

Knight Cancer Instituteat Oregon Health & Science University
Intrabeam – Intraoperative Radiotherapy

Knight Cancer Instituteat Oregon Health & Science University
Complete Treatment
System
No room shielding
Mobile--use in multiple
operating rooms
6 MeV - 12 MeV
3 – 10 cm Field Size
10 Gy/min dose rate
Mobile IOERT Solution

Knight Cancer Instituteat Oregon Health & Science University

Knight Cancer Instituteat Oregon Health & Science University
Stereotactic Body Radiation Therapy
SBRT
• What is it?
– a radiation technique where advanced treatment delivery and
radiation planning technology are used to deliver HIGH doses per
day in a safe and effective manner
– also known as Stereotactic Ablative Body Radiation therapy
(SABR)
– we use our technical capabilities to deliver radiation at the highest
level of accuracy and reproducibility
– 5 or less treatments

Knight Cancer Instituteat Oregon Health & Science University
Stereotactic Body Radiation Therapy
• SBRT can be used as primary radiation therapy for prostate cancer
– instead of a prostatectomy
– instead of daily treatments for 5-9 weeks
• SBRT can be used to target metastases from various cancers
– delay progression of disease
– delay starting more aggressive systemic therapies

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary treatment for prostate cancer
• 5 fractions
– conventional fractionation (39 – 45 treatments)
– moderate hypofractionation (20 – 28 treatments)
• First U.S. trial reported in 2007 with acceptable toxicity
– initial results: 4 year biochemical freedom from relapse 90%
– 33.5 Gy / 5 fractions
– GI toxicity (37.5%)
• bleeding, discomfort, mucous discharge
• no Grade 3 or higher

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancerHow does it compare in a randomized trial?
• PACE-B
– international phase 3 randomized non-inferiority trial
– between 2012 – 2018, 874 men randomly allocated to:
• standard treatments: 78 Gy over 39 fx / 62 Gy over 20 fx
• versus SBRT: 36.25 Gy over 5 fractions

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancerPACE-B
• Standard Fractionation (20 – 39) • SBRT (5 fractions)

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancerPACE-B

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancerPACE-B

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancerPACE-B

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancer
Scandinavian HYPO-RT-PC
• 1200 patients from 2005 – 2015 randomly assigned
– conventional fractionation (78 Gy / 39 fractions)
– ultra-hypofractionation (42.7 Gy / 7 fractions)
• median f/u 5 years, freedom from biochemical failure 84% both arms

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancer
Scandinavian HYPO-RT-PC Figure 3: Urinary toxicity and patient-reported problems

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancer
Scandinavian HYPO-RT-PC Figure 4: Bowel toxicity and patient-reported problems

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancer
bowel protection – SpaceOAR hydrogel

Knight Cancer Instituteat Oregon Health & Science University
SBRT as primary radiation treatment for prostate cancer
bowel protection – SpaceOAR hydrogel

Knight Cancer Instituteat Oregon Health & Science University
SBRT for Oligometastases
Oligo- From the Greek ‘oligos’, few, scanty
• Traditional treatment of patients with metastatic disease has been
based on systemic therapies that aim to delay progression and extend
life, but not to eradicate the disease completely.
• The oligometastatic paradigm suggests that in some patients,
metastatic disease is not widespread and may be constrained to
develop in only a small number of sites.
• This paradigm suggests that patients with oligometastases might be
amenable to a curative treatment approach.

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSABR-COMETStereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers: a
randomised phase 2, open-label trial
• 99 patients randomized to control (standard treatment) vs. radiation
– 1 – 5 metastatic lesions
– original tumor: breast, colorectal, lung, prostate, other

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSABR-COMETStereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers: a
randomised phase 2, open-label trial

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSABR-COMETStereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers: a
randomised phase 2, open-label trial

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSABR-COMETStereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers: a
randomised phase 2, open-label trial
• median overall survival
– 25 months for control (standard treatment)
– 41 months for SABR
• Adverse events of Grade 2 or worse
– 9% control
– 29% SABR
• 4.5% treatment-related deaths
– radiation pneumonitis, pulmonary abscess, gastric ulcer

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSTOMP Surveillance or Metastasis-Directed Therapy for Oligometastatic Prostate Cancer Recurrence
• 62 patients randomly assigned to standard treatment or
metastasis-directed therapy
– 3 or fewer lesions on PET
– metastasis-directed therapy
• surgery to remove disease
• or SBRT (30 Gy over 3 fractions)
– primary endpoint: Can metastasis-directed therapy delay the
need to start ADT
– ADT start: symptomatic progression, > 3 metastases, or local
progression of baseline-detected metastases

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSTOMP Surveillance or Metastasis-Directed Therapy for Oligometastatic Prostate Cancer Recurrence
• @ 3 years of f/u
– 30% Metastasis-Directed Therapy
had not started ADT
– no grade 2 to 5 toxicity
– QOL similar at baseline and 3-
month and 1-year

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesSTOMP Surveillance or Metastasis-Directed Therapy for Oligometastatic Prostate Cancer Recurrence
• @ 3 years of f/u
– 25% with biochemical recurrence-
free survival in the metastasis-
directed group
• median ADT-free survival
– 13 months in surveillance group
vs.
– 21 months for the metastasis-
directed therapy group

Knight Cancer Instituteat Oregon Health & Science University
SBRT for OligometastasesORIOLE Outcomes of Observation vs. Stereotactic Ablative Radiation for Oligometastatic Prostate Cancer
• Phase 2 study (1 - 3 metastases)
• 64 men randomized 2:1 to
receive SABR or observation
• primary outcome was
progression @ 6 months
• Progression-Free Survival
– observation 5.8 months
– SABR not yet reached (p=0.005)

Knight Cancer Instituteat Oregon Health & Science University
Advances in Radiation Technology
• Radiation technology has enabled better targeting
–IMRT
–SBRT
• Targeted Therapy with Radiation = – Reduced Toxicity
– Better Tumor Control
Preserving Quality of Life while eradicating cancer.

Knight Cancer Instituteat Oregon Health & Science University
Advances In Radiation Therapy
for Prostate Cancer
Arthur Hung, M.D.

Julie N. Graff, MD
Section Chief of Hematology/Oncology
VA Portland Health Care System
Associate Professor of Medicine
Knight Cancer Institute
Oregon Health & Science University
Biography:
Dr. Graff went to medical school at George Washington University where she received her MD with distinction in 2003. She moved to Portland, OR,
and completed residency and fellowship at the Oregon Health & Science University in 2009. Since that time, she has been on the faculty at the Knight
Cancer Institute OHSU and on the staff at VA Portland Health Care System, where she has been the chief of hematology/oncology since 2018.
Dr. Graff focuses on helping patients with cancer live well. She sees patients with genitourinary cancers, such as prostate, kidney, bladder and
testicular cancers, but her research is on prostate cancer. She has designed and implemented many clinical trials that have resulted in some dramatic
results. She became internationally recognized for her work in immunotherapy in prostate cancer. This work has spun off into multiple trials. In 2018,
she earned a prestigious $1M Movember Challenge Award from the Prostate Cancer Foundation to study the effect of manipulation of the gut
microbiota on responses to immunotherapy in Veterans with advanced prostate cancer. The correlative work for this first-in-field research is led by co-
principal investigators Dr. Amy Moran (immunologist) and Dr. Karen Sfanos (molecular pathologist). The critical work of understanding the genetic
underpinnings of the biopsied tumors is led by Reid Thompson, MD, PhD. Together they hope to enhance prostate cancer responses to
immunotherapy.
Dr. Graff is passionate about education and mentors multiple learners, ranging from pre-medical students to assistant professors. She is the recipient
of resident and fellowship teaching awards. She is also very interested in diversity of leadership and is heading an effort to help female junior faculty in
hematology/oncology. Also, she is incredibly passionate about giving Veterans the best cancer care in Oregon and beyond.



No evidence of disease:Nothing on imagingPSA undetectable
PSA Recurrence:Nothing on imagingPSA detectable
Metastatic Cancer:Spread on imagingPSA detectable
Adapted from Saylor. Journal of Clinical Oncology 2011; 29(27): 3705.

*Some disagreement

This study included 1997 men who had a radical prostatectomy at Johns Hopkins between 1982 and 1997. They were followed for a mean of 5.3 years (range of 0.5-15 years).
Of the 1997 men, 315 (15%) had a biochemical recurrence, defined as a PSA ≥ 0.2 mg/ml. Eleven of them received early hormonal therapy and were not included in this analysis.
Pound. JAMA 1999; 28 (17): 1591.

Pound. JAMA 1999; 281 (17): 1591.

Pound. JAMA 1999; 281 (17): 1591.


Those you can
see
Those you can
feel
Other
Weight gain Hot flashes Bone density
loss
Muscle loss Fatigue Lipid changes
Hair pattern
changes
Depression Decreased
insulin
sensitivity
Fat
redistribution
Mental slowing Heart
disease(?)
Testicle/penis
size decrease
Anemia


• Statistics
• Some may not do well
• Gleason 8, 9, 10
• Pre-treatment PSA >
2.0 ng/ml
• Negative margins
• PSA doubling time ≤ 10
months
• Seminal vesicle
invasion




Bicalutamide plus radiation versus radiation alone





Active Surveillance
Albertsen, P. C. et al. JAMA 2005;293:2095-2101.


*Until 1999, PSA ≤15 and Gleason ≤3+4 were used.

Romero-Otero J, et al. Int J Urol 2015; Epub Nov 2015

Romero-Otero J, et al. Int J Urol 2015; Epub Nov 2015

Laurence Klotz et al. JCO 2015;33:272-277


Mark Garzotto, MDProfessor of Urology and Radiation Medicine, OHSU Knight Cancer InstituteUrology Section Chief, VA Portland HCS
Multidisciplinary Care of High-Risk Localized Prostate Cancer
Biography:Dr. Garzotto has a long standing interest in trying to refine the diagnostic approaches to the detection of prostate cancerincluding incorporation of MRI and novel statistical methods such as machine learning. His research group identified theViet Nam war-era defoliant, Agent Orange as a risk factor for aggressive prostate cancer. He is considered an expert inthe design of novel treatment regimens for locally advanced prostate cancer including combination therapy such aschemoradiation and immuno-hormonal regimens. He is the Chief of the Urology at the Portland VA Medical Centerwhere he also serves as the Lead Investigator for the VA NAVIGATE Program that conducts NCI-sponsored trials formultiple cancer types. Understanding the molecular drivers of cancer is a prime interest of his, as he feels thisknowledge is essential to the pursuit of improved outcomes for patients. He has a strong interest in teaching as he feelsthe future of medicine is dependent on the continued growth in knowledge. He has been awarded the DepartmentFaculty Teacher of the Year Award several times.

Cancer Statistics, 2020:
Trends in Male Cancer Mortality, US 1930-2017
CA: A Cancer Journal for Clinicians, Volume: 70, Issue: 1, Pages: 7-30, First published: 08 January 2020,
DOI: (10.3322/caac.21590)
PSA introduced

Prostate Cancer Heterogeneity: Not One Disease
http://prostate-cancer.org/the-gleason-score-a-significant-biologic-manifestation-of-prostate-cancer-aggressiveness-on-biopsy/Modern Pathology (2004) 17, 292–306, advance online publication, 13 February 2004; doi:10.1038/modpathol.3800054

Prostate Cancer Disease State at Initial Diagnosis(SEER Incidence Cases, 2008-2017)
https://seer.cancer.gov/ SEER*ExplorerCooperberg et al. JCO 2010Tilki et al. J Urol 193:1970, 2016
Low
Intermediate
High/Very High
0
10
20
30
40
50
60
70
80
Localized Regional Distant
Perc
ent

High-risk Localized Prostate CancerNCCN Guidelines 2020
Feature NCCN High-RiskNo more than 1 feature
NCCN Very High-Risk2 or 3 High risk features, OR
Stage T3a (extracapsular) T3b (Seminal Vesicle)T4 (adjacent structures)
PSA > 20 ng/mL N/A
Gleason 8 - 10 Primary 5 (ie 5+3, 5+4, 5+5)
# Cores N/A > 4 cores Gleason 8-10
https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf

How is High-risk Localized Prostate Cancer Treated?


T1-2 WHO 3 orT3-4,N0-1
Randomized (n=415)
Radiotherapy +adjuvant goserelin
3.6 mg (n=207)
Radiotherapy Alone(n=208)
Hormonal Therapyat progression
EORTC 22863 Radiotherapy + Adjuvant ADT vs Radiotherapy Alone
Study Design
EORTC = European Organization for Research and Treatment of Cancer
Radiation: 50 Gy over 5 weeks + 20 Gy over 2 weeks
ZOLADEX 3.6 mg sc every 4 weeks starting day 1 of radiation and continuing for 3 years
Cyproterone acetate: 150 mg po qd for 1 month starting 1 week prior to ZOLADEX
Median follow-up at 45 months
and 66 months
Bolla M et al. NEJM 1997; 337(5)295-300; Bolla M et al. Lancet. 2002;360:103-108.

EORTC 22863: Radiation ± ADT for 3 yrs. Overall Survival 66-Month Follow-up
Bolla M et al. Lancet. 2002;360:103-108.
Overa
ll S
urv
ival
(%)
Combined Treatment
Radiotherapy Alone
0 1 2 3 4 5 6 7 8
Log-rank test p < .0001
Hazard ratio 0.51
(95% Cl: 0.36-0.73)
100
90
80
70
60
50
40
30
20
10
0
O N
81 208 199 177 146 106 70 46 30 16
50 207 197 183 166 142 93 71 43 24
Number
at Risk
Time Since Randomization (Years)

RTOG 0521: Docetaxel Chemotherapy After Radiation Treatment
StageGleasonscore PSA
Any T stage
≥9 <150
7-8 ≥20-150
≥T2 8 <20
Arm 1
AndrogenSuppression (24 mos)
+External RT (8 wks)
HighRisk
Randomize
Arm 2
AndrogenSuppression (24 mos)
+External RT (8 wks)
+Docetaxel beginning 4 wks after RT
(6 cycles)

RTOG 0521: Overall Survival
4 yr OS 93% vs. 89%
HR 0.70 (90%CI: 0.51-0.98)
Rosenthal et al JCO, 2019

SPCG-4: Surgery Results in Improved Cancer Survival and Reduction in Metastatic Spread
45% decrease in cancer death
46% reduction in metastatic disease
Bill-Axelson et al. NEJM 364:18, 2011Bill-Axelson et al. NEJM 379:2319, 2018

PIVOT: Surgery vs. ObservationProstate CA Deaths:high-risk disease
NEJM 367: 203-213, 2012

Rationale for Upfront Therapy Prior to Surgery
• Early treatment of metastatic disease
• Improved local control
• Rapid assessment of tumor response

Pre-operative Use of Novel Anti-Androgens in Intermediate and High-risk PCA
Treatment Duration Endpoint
TAPS (N=35)(NCT00298155)
LHRH+dutasteride ±bicalutamide ±ketoconazole
3 mo. Tissue Androgens
NeoAbi (N=58)(NCT00924469)
Abiraterone (3 vs. 6 mo) + LHRH
3 vs 6 mo. Tissue androgens
Neo-Enza (N=52)(NCT01547299)
Enzalutamide ± LHRH + Dutasteride
6 mo. Path CR
NeoAbiEnza (N=75)(NCT02268175)
Enzalutmide + LHRH ±Abiraterone
6 mo. Path CR or Minimal Residual disease

Path Outcomes from Neoadjuvant ADT with Enza/Leuprolide (EL) ± Abi/Pred (ELAP)
Parameter ELAP (n=50) EL (N=25)
Stage
P0 10% 8%
Min. Residual Dz. 20% 8%
T2 40% 36%
T3a/b 50% 56%
Node + 10% 12%
SM+ 18% 12%
ECE 46% 52%
SV+ 18% 28%
Upstaging 42% 60%
McKay et al JCO, 2019

Further Advances Will Require Multidisciplinary Approach
• Advanced Imaging
• Incorporation of Genomics
• Novel Therapeutics
– Anti-androgens
– Small Molecule Inhibitors
– Immunotherapy

OHSU Advanced Imaging Research Center
• Director: Charles Springer, PhD
• Bruker 12T MRI
• Siemens 7T MRI
• Siemens 3T
Li et al. J Magn Reson. 2016

PCA is heterogeneous but has a low mutational burden
Rubin et al. Cold Spring Harb Perspect Med, 2018Lawrence et al Nature 2013

Harnessing the Immune System:The Case for Checkpoint Inhibitors
http://www.onclive.com/publications/contemporary-oncology/2014/February-2014/Immune-Checkpoint-Blockade-in-Cancer-Inhibiting-CTLA-4-and-PD-1PD-L1-With-Monoclonal-Antibodies

Stress-induced Immunogenic Cell DeathConverting a Tumor from “Cold” to “Hot”
Radogna et al Biochem Pharm 2018Mercader et al PNAS, 2001Ochoa de Olza Lancet Oncology, 2020

Drug Treatment
• Pembrolizumab 200 mg IV Q/3 weeks
• Enzalutamide 160 mg po QD x 16 weeks
• GNRH agonist x 4 months
Radical Prostatectomy + node dissection at 16 weeks• pathologic CR
• pathologic Staging
• correlative studies
Pre-operative pembrolizumab plus intensive androgen axis blockade prior to
prostatectomy for high risk localized prostate cancer
High/Very-high-risk Prostate Cancer (N=32)• Gleason grade > 8-10
• PSA > 20 ng/ml
• Clinical stage T3a (resectable) Objectives:
Primary: pCR, safety/tolerability
Secondary:
pCR by PD-1 status,
clinical and biochemical recurrence
HRQOL
fecal microbiome correlates
Funding: Merck, AstellasNCT03753243

Conclusions: High-Risk Prostate CA
• Early Detection is key to attaining dz. control
• Effective therapies are available, but are not yet optimal
• Treatment combinations administered by a Multidisciplinary team holds great promise

Related Documents