Pn. Anwarul Hidayah Zulkifli FB 1020

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Pn. Anwarul Hidayah ZulkifliFB 1020

Founder of Homeostasis concept Claude Bernard (mid 1800’s): stability of
various physiological functions, i.e. body temperature, heart rate and blood pressure La fixite du milieu interieur (the constancy of
the internal environment) Walter Cannon (1929): created the word
“homeostasis” to describe the regulation of internal environment. Homeo: same/similar (internal environment is
maintained within a range of values rather than at exact fixed value.
Stasis: condition

Cannon’s proposed variables that are under homeostatic control Environmental factors that affect
cells --~osmolarity, temperature and pH
Materials for cell needs (nutrients, water, sodium, calcium,
inorganic ions, oxygen and internal secretions having general and continuous affects)
IF A BODY FAILS TO MAINTAIN HOMEOSTASIS OF THE VARIABLES, THEN NORMAL FUNCTION IS DISRUPTED AND A
DISEASE STATE/PATHOLOTICAL CONDITION RESULTED.

Homeostasis Steady state The process of keeping the internal body environment
in a steady state (maintaining constancy of the internal environment), when the external environment is changed.
Is a process of maintaining constant physical and chemical factors within an internal body environment.
Internal environment: the environment surrounding the cells (tissue fluids that fills the spaces between the cells).
Physical factors: temperature, blood pressure, osmotic pressure.
Chemical factors: pH value, concentration of sugar and salt



BASIC FEATURES OF HOMEOSTASIS

Questions asked relating to homeostasis Referring to “Adaptive Significance” Why does a certain function help an
animal survive in a particular situation? What structures and mechanisms evolved
in our anatomy and physiology that enable us to survive in hostile environment?
E.g. humans are large, mobile, terrestrial animals whose bodies maintain relatively constant water content living in dry, highly variable external environment.

Problems faced: Most body cells are not that tolerant of
changes in their surroundings Thus, they are similar to early organisms
that lived in tropical seas: salinity, oxygen content and pH vary a little; light and temperature cycle.
As organisms evolved and migrated from the ancient seas estuaries freshwater environments land (need to encounter highly variable external environments)

Rains dilute salty water + habituated organisms must cope with the influx of water into their body fluids.
Terrestrial organisms constantly lose internal water to the dry air around them need to keep internal environment relatively stable

BENEFITS OF HOMEOSTATIC CONTROL1. Life of the organism becomes less dependent on
the external environment.
2. Organism can live in a wider range of habitats, and the species can live in areas with variable conditions.
3. Organism can increase or decrease the metabolic rate of its body according to its requirements.
4. Enables more efficient and economical metabolic reactions because the total substrate used and the products formed, as well as the respective rates of reaction, are accurately coordinated.

PATHOLOGICAL CONDITIONS
Internal causes External causes Abnormal growth of cells
(cancer/benign tumor) Production of antibodies
by the body against its own tissues (autoimmune diseases)
Premature death of cells/failure of cell processes.
Inherited/genetic disorders
Toxic chemicals Physical trauma Foreign invaders such
as viruses and bacteria

Importance of ECF in homeostasis Watery internal environment of
multicellular animals extracellular fluid (ECF)
ECF serves as transition between an organism’s external environment and intracellular fluid inside cells.
ECF serves as a buffer zone between external part of the body and most cells of the body

When ECF composition varies outside its normal range of values, compensatory mechanisms activate and return the fluid to normal state
E.g. when a person drink a large volume of water, dilution of ECF triggers a mechanism that causes kidneys to remove excess water and protect cells from dilution.

Homeostasis Internal conditions vary, but always
within relatively narrow limits. Hormone-controlled homeostatic
mechanism, there is significant time-lag before corrective mechanism can be activated. It takes times for protein synthesis to
commence, the hormone to diffuse into the blood stream and for it to circulate around the body and take effect.

Law of mass balance
Amount of substance in the body is to remain constant, any gain = loss
Total amount (load) of substance x in the body = intake + production – excretion – metabolism
Maintain mass balance via: Excrete material (elimination of material
from the body via urine, feces, lungs, or skin)
Metabolize substance to different substance

Sensor
(receptor)
Effector
Control centre
Internal environme
ntExternal
environmental
Input feedback
Output
Figure: Homeostatic circuit
Detect changes
Execute changes
Defines changes and
triggers action


Negative Feedback Positive Feedback
maintain a constant value (set point).
Fluctuation from set level/set point in motion changes return to original value.
internal factors are controlled by antagonistic effectors
Have “push-pull” action-Increasing activity of one
effector is accompanied by decrease in the other
Involves: change in internal factor level detection by receptors activation of effectors restoring factors to its set point
a change in some variable causes a reaction which increases that change.
Steady state sets off a series of changes that intensify the changes
steady state causes changes that intensify (rather than reverse) the changes

Negative feedback
Fig. 38-5, p.381 (Solomon)

Positive feedback: Hemorrhage

Positive feedback: Contraction during childbirth


REGULATION OF BODY TEMPERATURE
PHYSICAL FACTORS

thermoregulation Antagonistic effectors involved Process of maintaining body temperature
within certain limits despite changes in surrounding temperature
Temperature change detected by hypothalamus in brain
Animals have different structural, behavioral, and physiological strategies
Animals that Maintain a fairly constant body temperature
(birds and mammals): Homeotherm Have a variable body temperature: Poikilotherm

Balancing Heat Loss and Gain Radiation: emission of electromagnetic waves by
all objects warmer than absolute zero.
Evaporation: removal of heat from the surface of a liquid that is losing some of its molecules as gas.
Convection: transfer of heat by movement of air or liquid past a surface
Conduction: direct transfer of thermal motion (heat) between molecules of objects in direct contact with each other

Insulation reduces the flow of heat between an
animal and its environment sources of insulation include hair, feathers
and layers of fat formed by adipose tissue. •Raising fur or feathers in reaction to coldness. This action traps a thicker layer of air, thereby increasing the insulating power of the fur or feather layer.•To repel water that would reduce insulating capacity of feathers or fur•Secreting oily substances, such as the oils that birds apply to their feathers during preening/grooming.•Humans rely on fat for insulation.•Goose bumps (vestige of hair raising) formation in human in reaction to coldness or scared•Blubber (very thick layer of insulating fat) in marine mammals such as walruses and whales to maintain body core temperatures of about 36-38°C without requiring much more food energy.

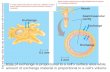
Countercurrent Heat Exchange Flow of adjacent fluids in opposing directions
that maximizes transfer rates of heat or solutes. Heat transfer involves an antiparallel
arrangement of blood vessels. It occurs among many birds, mammals, certain
sharks, bony fishes, and insects. As warm blood passes through arteries, it
transfers heat to the colder blood returning from the extremities in the veins.
Due to countercurrent blood flow in arteries and veins, heat transfer occurs along the entire length of the exchanger.

In the flippers of a dolphin, each artery is surrounded by several veins in a countercurrent arrangement, allowing efficient heat exchange between arterialand venous blood.
Canada
goose
Artery Vein
35°C
Blood flow
Vein
Artery
30º
20º
10º
33°
27º
18º
9º
Pacific
bottlenose
dolphin
2
1
3
2
3
Arteries carrying warm blood down the legs of a goose or the flippers of a dolphin are in close contact with veins conveying cool blood in the opposite direction, back toward the trunk of the body. This arrangement facilitates heat transfer from arteries to veins (black arrows) along the entire length of the blood vessels.
1
Near the end of the leg or flipper, where arterial blood has been cooled to far below the animal’s core temperature, the artery can still transfer heat to the even colder blood of an adjacent vein. The venous blood continues to absorb heat as it passes warmer and warmer arterial blood traveling in the opposite direction.
2

Thermoregulation When body temperature rises,
Erector muscles relax hairs lie flat against the skin, no longer trapping air, allowing
more heat to be lost by radiation (radiation: heat transfer from body to air)
Dermal blood vessels dilate Sweat glands are stimulated into vigorous secretory activity. Evaporation of sweat from skin surface dissipates body heat Body cools down thus preventing overheating.
When the external environment is cold, Erector muscle attached to your hair follicles contract,
which made your hairs stand, trapping air. Dermal blood vessels constricted. This causes the warm
blood to bypass the skin temporarily and allows skin temperature to drop to that of the external environment.
Shivering: involuntary shuddering contractions of the skeletal muscles, effective in increasing body temperature, muscle activity produces large amounts of heat.
Enhance thyroxine (thyroid gland) and adrenaline (adrenal gland) release increases the metabolic rate.



THERMONEUTRAL ZONE
Range of external (environmental) temperatures in which a naked man can survive without losing or producing heat.
27-31°C 27°C: lowest/critical temperature Body temperature changes are
compensated for, mainly by adjustment in blood flow (e.g. vasoconstriction and vasodilation)

Heat can be acquired by: Basal metabolic processes produce approximately
100 kcal of heat per hour or 1 kcal/kg/h body temperature raised by 1.1°C/h if the heat dissipating mechanisms are nonfunctional.
Strenuous physical activity can increase heat production more than 10-fold to levels exceeding 1000 kcal/h.
Fever, shivering, tremors, convulsions, thyrotoxicosis, sepsis, sympathomimetic drugs, and many other conditions
heat dissipation, including conduction, convection, and radiation.


Vasodilation of cutaneous blood vessels Blood flow in the skin increases, facilitating heat
loss.
Vasoconstriction of cutaneous blood vessels Blood flow in the skin decreases, lowering heat
loss. Blood is restricted to deep body areas and largely
bypasses the skin. The skin is separated from deeper organs by a
layer of insulating subcutaneous (fatty) tissue, heat loss reduced.
Vasodilation and vasoconstriction
Restriction blood flow to the skin for a brief period is not a problem , but if prolonged exposure to very cold weather, skin cells deprived of oxygen and nutrients begin to die. This extremely serious condition is called frostbite.

In humans, the hypothalamus
(the ventral/ underside part of the vertebrate forebrain), Contains a group of nerve
cells that function as a thermostat
Thermostat inhypothalamusactivates coolingmechanisms.
Sweat glands secrete sweat that evaporates, cooling the body.
Blood vessels
in skin dilate:capillaries fillwith warm blood;heat radiates fromskin surface.
Body temperaturedecreases;thermostat
shuts off coolingmechanisms.
Increased body temperature (such as when exercising
or in hot surroundings)
Homeostasis:Internal body temperature
36–38CBody temperature
increases;thermostat
shuts off warmingmechanisms.
Decreased bodytemperature
(coldsurroundings)
Blood vessels in skin
constrict, diverting bloodfrom skin to deeper tissues and reducing heat lossfrom skin surface.
Skeletal muscles rapidlycontract, causing shivering,which generates heat.
Thermostat inhypothalamusactivateswarmingmechanisms.
Figure 40.21: The thermostat function of the hypothalamus in human thermoregulation
Pg 839 ,Campbell textbook
*
*

38
Homeostasis: body temperature regulation

CONSEQUENCES: FAILURE TO THERMAL ADJUSTMENT Heat stress : body can no longer cope
with excessively high temperature. Feel dizzy or suffer from heat collapse. Dehydration may result due to heat
exhaustion. Heat stroke and characterized by
breakdown of temperature regulation mechanism body core temperature 42°C or higher may result to irreversible damage to cells and proteins coma
Robert S Helman (2010). Heatstroke. eMedecine

Heat illness/heat stroke Minor heat related illnesses: heat edema, heat rash (ie,
prickly heat), heat cramps, and tetany, as well as heat syncope and heat exhaustion.
Heatstroke is the most severe form of the heat-related illnesses and is defined as a body temperature higher than 41.1°C (106°F) associated with neurologic dysfunction. Exertional heatstroke (EHS) : occurs in young
individuals who engage in strenuous physical activity for a prolonged period of time in a hot environment.
Classic nonexertional heatstroke (NEHS) more commonly affects sedentary elderly individuals, persons who are chronically ill, and very young persons.

Cases of heatstroke In the United States, Centers for Disease
Control and Prevention reported: 8,015 deaths were attributed to excessive heat
exposure (summer) from 1979-2003 average of approximately 334 deaths per year. 1700 deaths were attributed to heat (1980)
Heatstroke is uncommon in subtropical climates and commonly affects people who undertake a pilgrimage to Mecca, especially when the pilgrims arrive from a cold environment.
In India (1998): more than 2600 deaths in 10 weeks.

COLD STRESS
Cold stress: body can no longer cope with the effect of cold.
Cause severely reduced blood circulation which deprives the tissue s of nutrients and normal metabolic reactions fail.
Chilblains (perniosis) may develop due to exposure to cold and humidity.
Tissues may freeze (destructive effects of the formation of extracellular ice crystals) need to be gently warmed.

exposure damages capillary beds in the skin, which in turn can cause redness, itching, blisters, and inflammation.
Chilblain

Frostbite
temperature of the skin or extremities dips below freezing, the water and liquids inside and between cells begin to crystallize.
As the water freezes, the microscopic ice crystals rupture and kill cells, causing irreversible tissue damage.

ECTOTHERMS ENDOTHERMS
body temperature depends on temperature of environment
Use behavioral strategies to adjust body temperatures
Benefits of ectothermy very little energy used to
maintain the metabolic rate ectotherms can survive on
less food
Disadvantage of ectothermy activity limited by daily and
seasonal temperature
Include most invertebrates, fishes, amphibians, and reptiles
Have homeostatic mechanisms regulate body
temperature within a narrow range
37oC or 98.6oF Benefits of endothermy
high metabolic rate constant body
temperature allows higher rate of enzyme activity
active even in low winter temperatures
Disadvantage of endothermy high energy
Include birds and mammals

BLOOD GLUCOSE REGULATION
CHEMICAL FACTORS

Blood Glucose regulation
Figure 41.3
STIMULUS:Blood glucose
level risesafter eating.
Homeostasis:Blood glucose level
90 mg/100 mL
STIMULUS:Blood glucose
level dropsbelow set
point.
1 When blood glucose level rises, the pancreas secretes insulin, a hormone, into the blood.
Glucagon promotesthe breakdown of
glycogen in theliver and the
release of glucoseinto the blood,
increasing bloodglucose level.
4
When blood glucose level drops, the pancreas secretes the hormone glucagon into the blood.
3
Insulin enhances the uptake of glucose in body cells and stimulates the liver and muscle cells to store glucose as glycogen. As a result, blood glucose level drops.
2
Hyperglycemic
Hypoglycemic
-cells
-cells


Pancreas
Blood glucose concentration is controlled by the pancreas
Pancreas has Glucose receptor cells, which monitor
the concentration of glucose in the blood Endocrine cells (called the Islets of
Langerhans), which secrete hormones. -cells: secrete the hormone, glucagon -cells: secrete the hormone, insulin

Type I diabetes
Insulin-dependent diabetes or early onset diabetes
Due to an autoimmune disorder, killing off the -cells
Treatment: Insulin injection
Appears during childhood, disability to produce insulin

Type II diabetes
Non insulin-dependent diabetes or late-onset diabetes
Most type II diabetics produce insulin, but the amount is inadequate or
The insulin receptors are unable to respond to insulin, a phenomenon called “insulin resistance”
Cause: excess body weight, high sugar diet, lack of exercise
Treatment: Drug therapy, careful diet.
Mostly occurs after age of 40 years

Symptoms of diabetes: Excessive thirst
Due to osmosis of water from cells to the blood, which has a low water potential
Copious urine Huge urine output due to excess water in blood
Poor vision Due to osmotic loss of water from the eye lens
Tiredness Due to loss of glucose in urine and poor uptakes of
glucose by liver and muscle cells Ketosis
Abnormal condition of excess ketone bodies (fatty acid metabolites) production, break down of lipids to supply energy
Muscle wasting Due to gluconeogenesis caused by increase glucagon

BLOOD CHOLESTEROL
CHEMICAL FACTORS

REGULATION OF CHOLESTEROLCHOLESTEROL IN THE BODY CHOLESTEROL IN THE
BLOOD
Made by liver cells Important as
component of membranes: bile salts (fat digestion), steroid hormones synthesis (estrogen and testosterone), acetylcholine synthesis
Insoluble in water Carried by
lipoproteins (LDL)

Why regulate cholesterol? Cholesterol needed by all cells need to
be circulated in reasonable concentrations in the blood
High cholesterol concentrations deposited in the linings of the artery walls Narrows the artery and resulted to heart
attack or stroke Patients with an inherited inability to
regulate blood cholesterol would not survive beyond childhood without treatment.

Liver cells are able to regulate cholesterol concentrations in their own cytoplasm
Cholesterol inhibits one of the enzymes involved in its own synthesis (negative feedback).

Cholesterol regulation by the liver
CHOLESTEROL AT NORMAL LEVEL IN BLOOD

BLOOD PH
CHEMICAL FACTORS

Regulation of Blood pH
maintaining the acid/base balance of your blood
Rely on buffers, the lungs and the kidneys.

Buffers pH is a measurement of the concentration of
hydrogen H+ ions Buffers are molecules which take in or release
ions in order to maintain the H+ ion concentration at a certain level.
Haemoglobin (Hb), certain proteins (Prot) and phosphates
Excessive H+ions in the blood , blood becomes acidic buffers remove the excess H + ions
Lack of H+ ions in the blood , blood becoming too basic, and so the buffers release H+ ions.
H-Hb↔Hb- + H+
Prot-H↔Prot- + H+
H2PO4-↔HPO4
2- + H+

Lungs control of blood pH HCO3
- + H+↔ H2CO3↔ CO2 + H2O
Breathing quickly will allow more CO2 to pass from the bloodstream into the air lower the level of CO2 in the blood.
If the CO2 is removed through breathing, it can't react and turn back into HCO3
- + H+. H+ is removed from the blood by reacting
with the buffer, but can't be remade because the CO2 required to do so has left the body.
raise your blood pH by hyperventilatinglower your blood pH by hypoventilatingfall below normal pH caused by hypoventilation is known as a respiratory acidosisrise in pH due to hyperventilation is known as a respiratory alkalosis

Kidney control of blood pH
Hydrogencarbonate mechanism
• In the cells lining the PCT and DCT, carbon dioxide reacts with water to form carbonic acid, which then dissociates into hydrogencarbonate ions and hydrogen ions.
CO2 + water Carbonic acid, H2CO3 HCO3+ + H+
• The hydrogencarbonate ions are reabsorbed into the blood whose pH is increased consequently. This is accompanied by the pumping of unwanted hydrogen ions into the lumen of the tubule.
In the lumen, the hydrogen ions combine with hydrogenphosphate ions to form dihydrogenphosphate ions, which is excreted in the urine.
At the same time, sodium ions are reabsorbed in exchange for the hydrogen ions. In the bloodstream, sodium ions maintain electrical neutrality with the hydrogencarbonate ions.
Ammonium mechanism The epithelial cells of DCT contain an enzyme,
which catalyses the formation of ammonia from the amino acid glutamine. (Amino acid glutamine ammonia)
In the lumen of the DCT, excess hydrogen ions combine with ammonia to form ammonium ions, which are excreted in the urine. (H+ + NH3+ NH4+)
The blood and tissue fluid normally have a pH of about 7.4.
The kidneys can decrease the hydrogen ion concentration either by hydrogencarbonate mechanism or by ammonium mechanism.

BLOOD SALT
CHEMICAL FACTORS


Rozaini Othman, GC Biologi

Regulation of Menstrual Cycle High oestrogen levels in the blood
around the time of ovulation have two effects: Inhibit the further release of GnRF and
hence of FSH by negative feedback. Cause anterior pituitary to release
increasing amounts of luteinising hormone (LH) positive feedback.

POSITIVE FEEDBACK: LH
LH stimulates ovulation, in which the ovarian follicle ruptures to release the secondary oocyte into the ovarian (fallopian) funnel.
It also stimulates the remains of the follicle in the ovary to develop into the corpus luteum (yellow body) secrete the hormone progesterone as well as oestrogen.
Oestrogen and progesterone maintain and develop the uterine wall further.

Negative Feedback: If fertilisation does not occur, the increasing
levels of these hormones eventually inhibit the further release of LH by negative feedback.
Without the maintaining effect of LH, the corpus luteum degenerates
Concentrations of oestrogen and progesterone fall and their maintaining action on the uterine wall is lost.
Uterine wall breaks down, resulting in the menstrual flow of cells and blood out through the vagina.


ALTERATIONS IN HOMEOSTASIS

Regulated changes
set points and normal ranges for homeostasis can change under various circumstances
associated with a particular stage in life, such as radical shift in hormone balance that occurs during puberty.
cyclic, such as the variation in hormone levels responsible for women’s menstrual cycle.

Acclimatization animal adjusts to changes in its
external environment acclimatization, a temporary change
during animal’s lifetime adaptation, a process of change in a
population brought about by natural selection acting over many generations.
For example, when a mammal moves from sea level to a much higher elevation, changes that occur several days facilitate activity at lowered oxygen concentrations such as:•Increased blood flow in the lungs•Increased production of red blood cells that carry oxygen

Thank you for your
attention.
The end….
IT’S REALLY CHILLY HERE….
WHERE AM I?
Related Documents