Hernia
May 15, 2015
Direct, Indirect and Femoral Hernia for Undergraduates
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript


What is a hernia? External abdominal hernias –
Protusion of the abdominal viscus through a weak spot in the abdominal wall.

Anatomy of the inguinal region

Boundaries of the inguinal canal

Weak spot on the anterior abdominal wall through which the Direct inguinal hernia protrudes.
Bounded by-Medially – Outer border of Rectus AbdominalisLaterally – By the inf Epigastric vesselsBelow – Medial part of the inguinal ligament

Contents of the inguinal canal
Ilioinguinal nerve - Medial part of the canal. it pierces through the internal oblique distributing filaments to it, enters the inguinal canal midway and the accompanies the spermatic cord till the Sup inguinal ring.
Males – Spermatic cord and its coverings and the remnants of the processus vaginalis
Females – Round ligament and the remnants of the processus vaginalis

Contents•DD –ductus deferens•GFN – Genitofemoral Nerve•Testicular plexus of sym nerves•LV –Lymph vessels•PPV –Pampiniform plexus•TA – Testicular artery•Artery to the vas•Artery to the Cremaster

Indirect hernia More common Major cause is a patent Processus Vaginalis Groups –
Bubonocele – Limited in the canal and the processus is closed at the sup inguinal ring. Presents as an inguinal swelling
Funicular – Processus is closed at its lower end just above the epidydimis. Therefore hernia is felt separated from the testis and above it.
Complete – Complete patent processus. Therefore the hernial sac is continuous with the tunica vaginalis of testis. Hernia is in front of at sides of the testis and it cannot be palpated easily. Congenital but detected only in adolescent life.

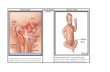
Peritoneum Extraperitoneal fat Int Spermatic fascia Cremasteric fascia Ext spermatic fascia Superficial fascia Skin
Coverings of an Indirect Inguinal Hernia

Direct Inguinal Hernia
Most important point is that neck is medial to the inferior epigastric vessels while indirect hernia’s neck is lateral to the vessels.
Always acquired with one rare exception
Rarely attains a large size and never descends into the scrotum and rarely gets strangulated because it has a wide neck.

Feature Indirect Hernia
Direct Hernia
Definition Enter at the deep inguinal canal
and traverse the length of the
canal
Protrudes through the posterior wall
of the canal through
Hesselbach’s triangle
Age and Sex Children and young adults;
M>>F
Elderly individuals; females not
affected
Laterality 2/3rds cases are U/L, right side is more common
>1/2 of the cases are B/L
Shape and Completion
Complete » Pyriform
Incomplete » Oval
Always incomplete and is spherical in shape

Feature Indirect hernia
Direct hernia
Reducibilty Doesn’t reduce by itself, has to be reduced by
patient or doctor
Automatically reduces when patient is lying
down
Impulse on coughing
On the index finger
On the middle finger
Invagination test
Impulse on the tip of the
finger
Impulse on the pulp of the
fingerRing
occlusion test
Doesn’t bulge out
Bulges out medial to the
finger

Clinical Features Pain – Dragging or aching type Sensation of heaviness and weight Painful and tender » Strangulated Swelling Others
Intestinal obstruction – if hernia is obstructing the lumen of the intestine. i.e colicky pain, vomiting, abdominal distension
Vomiting is an ominous sign and can indicate infection or impending rupture.

Femoral Hernia
Abdominal contents pass through the femoral ring and come out through the saphenous opening.
3rd most common hernia after inguinal and incisional and is more common in females.
Most liable to get strangulated.

Anatomy Femoral sheath is a continuation of transversalis
fascia into the thigh anteriorly and fascia iliaca posteriorly which fuse near the inguinal ligament.
It is divided into three compartments. The medial most compartment is called the femoral canal and contains efferent lymphatics, sometimes a small lymph node (lymph node of Cloquet) and areolar tissue.
The opening of the femoral canal is called the femoral ring through which femoral hernia occurs. The ring is generally closed by the femoral septum which is extraperitoneal tissue.


To the femoral triangle

The saphenous opening or the fossa ovalis is an opening in the fascia lata 4cm below and Lateral to the pubic tubercle.
Sharp upper and outer margins called falciform process. This process is important because it turns the femoral hernia upwards after it comes out of the opening.
Covered by loose areolar tissue called the cribriform fascia.
Traversed by the long saphenous vein and lymphatics.

Course of a Femoral hernia
Comes out through the femoral ring
Passes through the femoral canal
Comes out through the saphenous opening
Pushed up by the folds and moves up through the subcutaneous tissue of the thigh and can even reach above the inguinal ligament.

Coverings of Femoral hernia
Peritoneum Femoral septum Fatty content of the femoral canal Anterior layer of the femoral sheath Cribriform fascia Superficial fascia Skin

Clinical features and signs Age and Sex – Rare in young people. Majority
between 60 and 80 years. F>>M( but the most common hernia in females is inguinal hernia)
R>L ; B/L is seen in 20% cases. Pain is lesser than that of inguinal hernia and
can go unnoticed until strangulation Swelling- Small globular swelling lateral to and
below the pubic tubercle. More obvios on standing and straining.
Other symptoms – Abdominal colic, vomiting, distension and constipation.

Test Inguinal Hernia
Femoral Hernia
Position Neck of sac is below the inguinal
ligament and lat. to pubic
tubercle
Above the inguinal
ligament and medial to the pubic tubercle
Cough impulse
Indirect » Index Direct » Middle
Impulse is felt on Ring finger
Invagination test
Positive Negative (empty canl)
Ring occlusion
test
Direct » BulgeIndirect » No
bulge
Doesn’t come out

Related Documents