Hemorrhagic Stroke Justin S. Cetas MD, Ph.D. Assistant Professor of Neurological Surgery Chief of Neurosurgery PVAMC

Hemorrhagic Stroke
Feb 24, 2016
Hemorrhagic Stroke . Justin S. Cetas MD, Ph.D. Assistant Professor of Neurological Surgery Chief of Neurosurgery PVAMC. Hemorrhagic Stroke . Loosely defined as sudden loss of brain function due to bleeding - PowerPoint PPT Presentation
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Hemorrhagic Stroke Justin S. Cetas MD, Ph.D.Assistant Professor of Neurological SurgeryChief of Neurosurgery PVAMC

Hemorrhagic Stroke
• Loosely defined as sudden loss of brain function due to bleeding
• Presentation, prognosis, cause and hence treatment vary depending on the location of bleeding
• Major Types: epidural, subdural, subarachnoid, intraparenchymal, intraventricular

Intracerebral hemorrhage
• Sudden onset focal neurologic abnormality• More often associated with HA, nausea,
loss of consciousness, acute severe HTN• CT best and fastest method to distinguish
from ischemic stroke


Intracerebral hemorrhage
• 10-15% of all strokes• Potential causes include:
– Hypertension (majority)– amyloid angiopathy,– AVM or dAVF– aneurysm– use of sympathomimetic drugs (cocaine,
methamphetamine)– Vasculitis– Moyamoya disease

OHSU Neurological Surgery
Hemorrhagic stroke Hypertension
• Most important and prevalent modifiable risk factor
• 60-70% of spontaneous ICH • Untreated>treated• Stopping medication>continuing• Brainstem and deep hemispheric locations
most common

OHSU Neurological Surgery

OHSU Neurological Surgery

OHSU Neurological Surgery
Hemorrhagic Stroke Amyloid
• Major cause of lobar hemorrhage • Amyloid protein in media and adventia of
arteries, arterioles, and capillaries • Increases with age• 5-8% 60-69 yrs• 57-58% 90yrs or older• Associated with Apolipoprotein E

OHSU Neurological Surgery
Hemmorhagic stroke Anticoagulant therapy
• OAT for atrial fibrillation common and growing
• Increases risk of ICH (0.3-3.7%)• Increases severity and mortality of ICH• Mortality may be as high as 67%

OHSU Neurological Surgery
Hemorrhagic stroke other risk factor
• Heavy alcohol use • Current tobacco use• Diabetes• Prior cerebral infarct 5-22 fold increase• Hypocholesterolemia
– Reduced platelet function– Fragile vessels– Comorbidities
• Family history

OHSU Neurological Surgery

OHSU Neurological Surgery

OHSU Neurological Surgery
Hemorhagic stroke AVM
• 0.5/100,000 • Abnormal vessels draining directly into veins
without capillary bed • Mean age at diagnosis 40• Risk factors:
– Prior hemorrhage – Deep location– Deep venous drainage– Venous restrictive disease – Associated aneurysm

OHSU Neurological Surgery
Hemorrhagic stroke DAVF
• Abnormal shunting of normal arteries into brain– Type I Meningeal arteries – meningeal veins– Type II similar to I with venous reflux– Type III Direct shunting to cortical veins– Type IV venous ectasias
• Follow trauma (may be remote)• Can arise spontaneously in the elderly

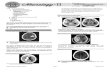
Case Illustration
• 50 year old man experienced sudden headache
• He becomes confused and nauseated • On arrival to ED he become unresponsive• Urgent CT demonstrates IPH, SDH with
mass effect






dAVF post op

OHSU Neurological Surgery
Hemorrhagic stroke Moyamoya
• Progressive stenosis or occlusion of the circle of Willis arteries
• Numerous neovessels arise “puff of smoke”• Dilated neovessles form microaneurysms

OHSU Neurological Surgery
Hemorrhagic stroke - Moyamoya

OHSU Neurological Surgery
Moyamoya
• 0.06/100,000 whites• 0.54/100,000 in Japan• Women 2x higher than men• Multiple hemorrhages • Associated with Down’s syndrome

Intracerebral Hemorrhage
• Location of hemorrhage • Presence of IVH• Volume of hemorrhage
– Best predictor of outcome

ICH Grading scale
• Glasgow Coma Scale:– 3-4 2– 5-12 1– 13-15 0
• ICH Volume– >30 cc 1– <30 0
• Infratentorial– Yes 1– No 0
• Age – >80 1– <80 0
Mortality Score26% 272% 397% 4

Cerebral Aneurysms and SAH
• SAH accounts for 3-4% of all strokes (10/100,000)
• Fatality approx 50%– 10-15% with sudden death at initial bleed– 40% die within 1 month of admission
• 30% of survivors with morbidity• 6% of the population may harbor an
aneurysm(s) • ½ of SAH in patients younger than 55

Epidemiology
• Modifiable risk factors for SAH: • Hypertension, smoking, excessive alcohol
(undefined)• Modifiable risk factors double risk of SAH,
contribute to 2/3 cases • Genetic risk factors important in 10% of
cases

Cerebral Aneurysms
Van Gijn et al. 2007

SAH
• Typical presentation• Sudden onset WORST HEADACHE of
Life• Rapidly followed by nausea vomiting
confusion or coma• High risk of re-rupture• Hydrocephalus



Grading Schemes
Hunt Hess Clinical Grade • 1. Asymptomatic, mild headache, slight nuchal
rigidity • 2. Moderate to severe headache, nuchal rigidity,
no neurologic deficit other than cranial nerve palsy• 3. Drowsiness / confusion, mild focal neurologic
deficit • 4. Stupor, moderate-severe hemiparesis • 5. Coma, decerebrate posturing

Grading Schemes
Fisher Grade: Appearance of hemorrhage on CT
• 1 None evident • 2 Less than 1 mm thick • 3 More than 1 mm thick • 4 Any thickness with intraventricular
hemorrhage or parenchymal extension

Case Illustration
• 49 year old woman experienced sudden onset headache and left arm weakness
• Sleepy but oriented and conversant• Transferred to OHSU



OHSU Neurological Surgery




Hemorrhagic stroke
• Goals of early intervention– Establish an airway– Blood pressure control – Reverse coagulopathy– Establish the etiology of the hemorrhage– Surgical intervention if indicated

OHSU Neurological Surgery
Acute Hypertensive Response
• Dramatic rise with ICH • Remains elevated for 24 hours• Current recommendation SBP>160• SBP>140 may be safe• Too low may exacerbate ischemic injury of
adjacent brain

Hemorrhagic Stroke
• ICU care is supportive• Aimed at preventing secondary injury• Aggressive ICU care in first 48 hours
improves survival and outcomes• Dedicated stroke unit improves survival
and recovery

OHSU Neurological Surgery
• Evacuation of clot
– Early evacuation associated with slight increase in rehemorrhage rate
– may shorten hospital stay but has no proven impact on long term outcomes except
– Mass effect causing further injury• Surgery aimed at preventing secondary
injury

OHSU Neurological Surgery
Intraparenchymal Hemorrhages
• Recovery can take months• Long-term outcomes are difficult to predict
early on in disease course• Multi-disciplinary rehabilitation important

Delayed Ischemic Neurological Deficits
• Develops 5-15 days after SAH• Risk factors:
– Fisher Grade– Age <68 years (elderly may become
symptomatic with little spasm)– Smoking, Cocaine use, Hypertension
• Genetics: variations in eNOS system

Delayed Ischemic Neurological Deficits
• Symptoms may be vague: sleepiness, lethargy or stupor, unexplained fever, diuresis
• May be localizing: Hemiparesis, language disturbance, abulia, gaze impairment etc.
• Confounders: poor grade, sedation, etc.

Neuro ICU
• SAH associated with derrangements of multiple brain systems
• Careful monitoring and early intervention critical to preventing infarcts
• Improved patient outcomes with dedicated Neuro-ICU

Conclusion
• Primary goal of treatment is to prevent secondary injury
• Prolonged ICU stay expected • Many patients can make meaningful recoveries• Individual recovery can be hard to predict • SAH sets up complex pathological processes
that are poorly understood• Future studies needed
Related Documents