HEALINGMESH PERFORMANCE & SUPPORT FOR THE LONG RUN Mediac AS Helle-Telemark Norway [email protected] [email protected] Global suppliers for biologic surgical materials. The native collagen tridimensional structure is fully maintained after processing Resetting the wound by restoring the physiological healing process Equine Pericardium ONE STEP PROCEDURE

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

HEALINGMESHPERFORMANCE & SUPPORT FOR THE LONG RUN
Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Global suppliers for biologic surgical materials.
The native collagen tridimensional structure is fully maintained after processing
Resetting the wound by restoring the physiological healing process
Equine PericardiumONE STEP PROCEDURE

Matches the elasticity and stiffness of dermis
Biomimetic surface for cell attachment that
Regenerative
Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Features of the Tissue Matrix
Provides coverage for underlying structures
Replicates dense connective tissue properties
Modulates the mechanotransduction properties of cells (i.e. produces appropriate ECM and growth factors)
Durable
Matrix that persists (does not dissolve) until cellular infiltration is adequate
Non-immunogenic
Degrades without producing inflamma-tory response
One application sufficient (compared with serial application of other dermal matrices)
Prevents hypertrophic scars or wound contractures
The native collagen tridimensional structure is fully maintained after processing.
Effective stabilization
Enzyme resistance
Terminal sterilization (beta radiation)
Effective destruction of all types of pathogens (SAL )-6

Treatment of Diabetic Foot Ulcer with Acellular Equine Pericardium
Age: 53, Male Diabetes Type 2Insulin treated
Pre-op
5 weeks-po 1 Year-po
Post-opUlcer location: anterior tibialCause: surgical deiscence after saphenectomy for by A-C bypassresulted in blister formation with an underlying grade 2 ulceration
HealingMesh was appliedOther treatment: non-adherent dressing applied and changed weeklyFollow-up: weekly follow-up until wound closure
Uneventful post-operative course with no swelling or major exudate.Wound closed after 4 weeks post.operative.The use of HealingMesh was successful in treating chronic diabetic leg ulcer.
Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
PATIENT
DIAGNOSIS
TREATMENT
OUTCOME
VASCULAR ULCERAlberto Cogo Valter Deanesi Rachele Reitano

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Treatment of Phlebo-lymphaedema Ulcer with Acellular Equine Pericardium
Age: 77, MalePhlebo-lymphaedema ulcer
Pre-op
Ulcer location: distal medial tibiaCause: phlebo-lymphedema
HealingMesh was appliedOther treatments: non-adherent dressing applied and changed weekly
Follow-up: weekly until wound closure
PATIENT
DIAGNOSIS
TREATMENT
Uneventful post-operative course with no swelling or major exudateWound closed after 45 days post operative.
The use of HealingMesh was successful in treating phlebo-lymphaedema ulcers.
OUTCOME
21 days-po
45 days-po
LYMPHAEDEMAAlberto CogoValter DeanesiRachele ReitanoChia Grigolo

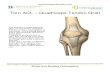
Treatment of Chronic Lesion of Achillis tendon
Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
ACHILLIS TENDON
PATIENT
Age 57, Male
DIAGNOSIS
TREATMENT
End-to-end Suture
Uneventful post-operative courseWound closed after 3 weeks post operative8 weeks with orthotic supportRange of motion exercises 10 to 14 days after the repairAt 6 weeks after the repair begun weight bearing exerciseMRI at 3 months post-op shows a complete healing of the achillis tendonFully recovery at 6 months post-op
OUTCOME
Achillis Tendon Rupture
HealingMesh was placed between the peritenon and tendon to augment the suture
Nicola GalanteGiampietro Bertasi

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
PRODUCT APPLICATION REFERENCE GUIDE
Step 1
HEALINGMESHAPPLICATION REFERENCE GUIDE
To prepare the wound bed, debride non-viable and hyperkeratotic tissue, if needed. Bleeding should be controlled with sterile compression.
Step 2
Prepare HealingMesh in accordance as outlined in the “Instructions for use”. 500 ml of sterile saline are required.
Step 3
Using sterile technique, measure and trim HealingMesh to the appropriate size in order to cover the wound. Make certain there is at least a 2-4 mm excess border for adequate fixation.

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Step 4
HealingMesh is secured to the wound bed utilizing the client’s preference of mechanical fixation (This is generally performed with 4-0 nylon suture or surgical staples).
It is important to place the sutures or staples in a pattern that maintains intimate contact between the dressing and the wound bed.It is very important to continue to push ‘HealingMesh’ down onto the wound bed as each stitch is placed to avoid tenting.Tenting occurs because the ‘HealingMesh’ is tensioned while being sutured and stretches taut off the bed.
Step 5
Keep HealingMesh hydrated. Hydrating ointments may be applied directly to Healing Mesh and covered with a secondary or appropriately sized sterile gauze, can be applied to maintain dressing-to-wound contact and help keep the HealingMesh secure.
Sutures or anchoring devices are removed once adequate healing has been achieved.
Step 6
1 YEARp.o

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
POSTOPERATIVE CARE
Step 8
NOTE
This is only a suggested protocol.Decision about appropriate care should be made based on the individual healthcare provider’s preference, experience and the extent and severity of the patient’s wounds.
An adequately padded outer warp, which may include a compression type bandage, may be applied to help control any lower extremity edema which could inhibit wound healing.
Step 7
To maintain a clean and moist wound environment, outer dressing changes should be performed at least every three/four days. Each dressing change is performed in a similar fashion utilizing antibiotic ointment and dressing materials.Careful observation of the wound should be completed to rule out presence of infection.

Hozibal, Kimberly B., and Dane K. Wukich. 2012, Diabetic foot infections: current concept review. Diabetic Foot Ankle; 3:1-8Dumville, Jo. C., Sohan Deshpande, Susan O'Meara, and Katharine Speak. 2011. Foam dressings for healing diabetic foot ulcers (Review). Cochrane Database System Rev; 9:1-46Gupta, Subhas, Barbara Bates-Jensen, Allen Gabriel, Allen Holloway, Jeffrey Niezgoda, and Dot Weir. 2007. Differentiating negativepressure wound therapy devices: an illustrative case series. Wounds,; 19(1):1-9Zamboni, W. A., H. P. Wong, L. L. Stephenson, and M. A. Pfeifer. 1997. Evaluation for hyperbaric oxygen for diabetic wounds: a prospective study. Undersea Hyperb Med; 24(3):175-179Wainwright, DJ, Bury, SB. 2011. Acellular Dermal Matrix in the Management of the Burn Patient. Aesthet Surg J; 31(7):13S-23SWong I, Burns J, Snyder S. 2010. Arthroscopic GraftJacket Repair of Rotator Cuff Tears. J Shoulder Elbow Surg; 19(2):104-109Wilkins, R. 2010. Acellular Dermal Graft Augmentation in Quadriceps Tendon Rupture Repair. Curr Orthop Pract, 21(3):315-319Lee, Daniel. 2007. Achilles Tendon Repair with Acellular Tissue Graft Augmentation in Neglected Ruptures. J Foot Ankle Surg; 46(6): 451-455Sbitany, H., Sandeen, S., Amalfi, A., Davenport, M., Langstein, H. 2009. Acellular Dermis-Assisted Prosthetic Breast Reconstruction versus Complete Submuscular Coverage: A Head-to-Head Comparison of Outcomes. Plast Reconstr Surg; 124:1735-174 10.Obermiller JF,Hodde JP,McAlexander CS,Kokini K,Badylak SF. A comparison of suture retention strengths for three biomaterials. Med Sci Monit 2004; 10: PI 1-PI 5. LinksHirooka A,Yoneda M,Wakaitani S,Isaka Y,Hayashida K,Fukushima S,Okamura K. Augmentation with a Gore-Tex patch for repair of large rotator cuff tears that cannot be sutured. J Orthop Sci 2002; 7: 451-456. LinksGood L,Odensten M,Pettersson L,Gillquist J. Failure of a bovine xenograft for reconstruction of the anterior cruciateligament. Acta Orthop Scand 1989; 60: 8-12. LinksJarman-Smith ML,Bodamyali T,Stevens C,Howell JA,Horrocks M,Chaudhuri JB. Porcine collagen crosslinking,degradation and its capability for fibroblast adhesion and proliferation. J Mater Sci Mater Med 2004; 15: 925-932.LinksLangdon SE,Chernecky R,Pereira CA,Abdulla D,Lee JM. Biaxial mechanical/structural effects of equibiaxial strainduring crosslinking of bovine pericardial xenograft materials. Biomaterials 1999; 20: 137-153.Sander T. VP Engineering,Pegasus Biologics, personal communication.Sward L,Hughes JS,Amis A,Wallace WA. The strength of surgical repairs of the rotator cuff. A biomechanical study on cadavers. J Bone Joint Surg Br 1992; 74: 585-588. LinksMura N,O'Driscoll SW,Zobitz ME,Heers G,An KN. Biomechanical effect of patch graft for large rotator cuff tears: Acadaver study. Clin Orthop Relat Res 2003; 415: 131-138. LinksDavis NR,Risen OM,Pringle GA. Stable, nonreducible cross-links of mature collagen. Biochemistry 1975; 14: 2031-2036.
Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Bibliography

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Order Information:
HM-040X050H Pericardium membrane in propylene - oxide alcoholic solution 40X50 mm
HM-060X080H Pericardium membrane in propylene - oxide alcoholic solution 60X80 mm
HM-070X080H Pericardium membrane in propylene - oxide alcoholic solution 70X80 mm
HM-060X120H Pericardium membrane in propylene - oxide alcoholic solution 60X120 mm
(OTHER SIZES ON DEMAND)

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Drives the regeneration of the connective tissueAdhesive to the connective tissueResistant to the traction pressure and retention of the sutureDouble layer it can be used as double layer, not rolled upSafe: 100,000+ devices implanted without complicationsShape memory it does not curl in the operating field Source BSE-free (horses are the only BSE-free mammalians)
Audio Technologies Biomembrane

Mediac ASHelle-TelemarkNorway
[email protected]@mediac-medical.eu
Copyright © 2017 MEDIAC & MEDIAC - MEDICAL is a Trade Mark | All rights reseved.
Mediac ASHelle-Telemark
Mediac BVOldenzaal
0373Sep 2017 - HMB/2.01
Related Documents