1 Instrumented assessment of the effect of Botulinum Toxin-A in the medial 1 hamstrings in children with cerebral palsy 2 3 Bar-On L. PT MSc a,b , Aertbeliën E. Ir PhD c , Molenaers G. MD PhD a,d,e , Van 4 Campenhout A. MD a,d,e , Vandendoorent B. PT MSc b , Nieuwenhuys A. PT MSc a,b , 5 Jaspers E. PT PhD b,f , Hunaerts C. PT MSc a ; Desloovere K. PhD a, b 6 7 a Clinical Motion Analysis Laboratory, University Hospital Leuven, Pellenberg, 8 Belgium 9 b KU Leuven Department of Rehabilitation Sciences, Leuven, Belgium 10 c KU Leuven Department of Mechanical Engineering, Leuven, Belgium 11 d KU Leuven Department of Development and Regeneration, Leuven, Belgium 12 e Department of Orthopedics, University Hospital Leuven, Pellenberg, Belgium 13 f Neural Control of Movement Lab, ETH Zurich, Switzerland 14 15 Acknowledgements 16 This work was made possible by a grant from the Doctoral Scholarships Committee 17 for International Collaboration with non EER-countries (DBOF) of the Katholieke 18 Universiteit Leuven, Belgium. This work was further supported by a grant from 19 Applied Biomedical Research from the Flemish agency for Innovation by Science and 20 technology (IWT-TBM: grant number 060799); and by an unrestricted educational 21 grant from Allergan, Inc. (USA). 22 23 24 25 26 27 28

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

1
Instrumented assessment of the effect of Botulinum Toxin-A in the medial 1
hamstrings in children with cerebral palsy 2
3
Bar-On L. PT MSca,b, Aertbeliën E. Ir PhDc, Molenaers G. MD PhDa,d,e, Van 4
Campenhout A. MDa,d,e, Vandendoorent B. PT MScb, Nieuwenhuys A. PT MSca,b, 5
Jaspers E. PT PhDb,f, Hunaerts C. PT MSca; Desloovere K. PhDa, b 6
7
a Clinical Motion Analysis Laboratory, University Hospital Leuven, Pellenberg, 8
Belgium 9
b KU Leuven Department of Rehabilitation Sciences, Leuven, Belgium 10
c KU Leuven Department of Mechanical Engineering, Leuven, Belgium 11
d KU Leuven Department of Development and Regeneration, Leuven, Belgium 12
e Department of Orthopedics, University Hospital Leuven, Pellenberg, Belgium 13
f Neural Control of Movement Lab, ETH Zurich, Switzerland 14
15
Acknowledgements 16
This work was made possible by a grant from the Doctoral Scholarships Committee 17
for International Collaboration with non EER-countries (DBOF) of the Katholieke 18
Universiteit Leuven, Belgium. This work was further supported by a grant from 19
Applied Biomedical Research from the Flemish agency for Innovation by Science and 20
technology (IWT-TBM: grant number 060799); and by an unrestricted educational 21
grant from Allergan, Inc. (USA). 22
23
24
25
26
27
28

2
1. Introduction 29
30
Spasticity is characterized by a velocity-dependent increase in tonic stretch reflex [1] 31
with an accompanying increase in muscle resistance when a muscle is passively 32
stretched [2]. This definition, as well as the methods for spasticity assessment, has 33
been under much debate in the last decade. Nonetheless, neuromuscular tone 34
reduction remains an important treatment modality in children with cerebral palsy 35
(CP) [3]. For example, Botulinum Toxin type-A (BTX-A), injected intramuscularly, 36
causes a temporary reduction in reflex muscle activity by selectively blocking the 37
release of acetylcholine at the cholinergic nerve terminals. Whilst this has been found 38
effective to decrease spasticity in children with CP, there remains a large variability in 39
treatment response [4]. A comprehensive assessment of the effect of BTX-A on 40
spasticity could increase our knowledge of the pathology and improve our 41
understanding of this reported variability. 42
43
In children with CP, the effect of BTX-A is most commonly assessed with clinical 44
scales (Modified Ashworth-MAS [5], or Modified Tardieu Scale-MTS [6]). These 45
scales assess spasticity by subjectively interpreting the resistance felt during passive 46
stretch. Nonetheless, the perceived resistance may be a result of reflex muscle 47
activity as well as of changes in visco-elastic properties of the joint and muscle. The 48
available clinical scales fail to distinguish between both components and are thus not 49
deemed sensitive or valid to quantitatively assess the effect of BTX-A on the stretch 50
reflex. Moreover, they have also been criticized for their low reproducibility and poor 51
accuracy [7,8]. As such, clinical scales have a limited ability to differentiate between 52

3
patients or to explain the response variability after treatment. Instrumented methods 53
could provide a more comprehensive assessment. 54
55
Electromyography (EMG) has been used in adults to quantify the effect of BTX-A on 56
the pathological response during passive muscle stretch [9,10]. Simultaneously 57
assessing muscular resistance using torque sensors provides an integrated (EMG 58
and torque) instrumented measurement method [11]. However, in children with CP, 59
clinically-applicable integrated approaches to assess the effect of BTX-A have only 60
been applied to the upper limb [12], whereas lower limb muscles are most commonly 61
treated. We therefore used an instrumented method, that integrates EMG and torque, 62
as described by Bar-On et al. [13]. The repeatability and discriminate validity to 63
measure spasticity in the medial hamstrings (MEH) in children with CP has previously 64
been shown [13,14]. However, it is yet to be determined whether this instrumented 65
assessment is sensitive to detect treatment efficacy and if it can help understand 66
variability in treatment outcome. 67
68
Therefore, the aim of this study was to quantify and understand the effects of BTX-A 69
injection in treating MEH spasticity in children with CP, using an integrated 70
assessment based on EMG and torque. 71
72
73
2. Method 74
75
Children aged 3-18 years and scheduled for BTX-A in the MEH (Mm. 76
Semitendinosus and Semimembranosus) were recruited from the multidisciplinary 77

4
clinic for patients with CP (University Hospital ***). The exclusion criteria were: 78
presence of ataxia or dystonia; severe muscle weakness (<2+ on the Manual Muscle 79
Test [15]); poor selectivity [6]; bone deformities or contractures hindering neutral 80
alignment; cognitive problems that could impede the measurements; previous lower 81
limb orthopedic surgery (soft tissue or bony procedures); intrathecal Baclofen pump 82
or selective dorsal rhizotomy. Minimal strength production and good selectivity were 83
required because a voluntary contraction was used as an individual reference to 84
evaluate surface EMG (sEMG) signals in previous studies with the same subject 85
group [13,14]. In the current study however, voluntary contractions were expected to 86
be influenced by the BTX-A injections and the normalized sEMG was thus not 87
analyzed. The University Hospitals’ ethical committee approved the experimental 88
protocol and all children’s parents signed an informed consent. 89
90
As part of a regular multilevel BTX-A treatment, muscles to inject and dosages were 91
selected based on standard multidisciplinary evaluation. Injection with BTX-A 92
(Botox®, Allergan Ltd, UK) was done under a short anesthesia and ultrasound was 93
used to confirm needle position. All children underwent casting for a period of 10 94
days (lower-leg with optional removable upper-part used as a knee-extension 95
device), intensive physical rehabilitation as well as orthotic management (day and 96
night) following the BTX-A injections. 97
98
2.1 Data acquisition 99
100
The set-up of the instrumented assessment for the MEH is presented in Figure 1. In 101
children with unilateral CP, only the affected side was tested. In children with bilateral 102

5
involvement, the most involved side was tested. This was defined as the side with the 103
highest MEH MAS-score or, in case of symmetrical MAS-scores, the most severe 104
MTS-score. All assessments were performed prior to injection and 14-70 days after 105
injection, by the same trained assessor. For more details regarding the measurement 106
method, the reader is referred to [13]. 107
108
Four repetitions of passive MEH muscle stretches over the full range of motion 109
(ROM) were carried out at three velocities. Firstly, the knee joint was moved at low 110
velocity (LV) during 5s, followed by a movement at intermediate, medium velocity 111
(MV) during 1s, and finally at high velocity (HV), which was performed as fast as 112
possible. The interval between repetitions was 7s in order to avoid post-activation 113
depression of the electrophysiological response. 114
115
2.2 Data analysis 116
117
A 6th order zero-phase Butterworth bandpass filter ranging from 20-500Hz was 118
applied to filter the raw sEMG signal. The root mean square envelope of the sEMG 119
(RMS-EMG) signal was computed using a low-pass 30Hz 6th order zero-phase 120
Butterworth filter on the squared raw signal. EMG onset, ROM, maximum angular 121
velocity (VMAX), and the net internal joint torque were computed as previously 122
described [13]. 123
124
Repetitions were excluded when passive stretches were performed out of plane, at 125
inconsistent velocities, in case of poor quality sEMG signal (loss of signal, low signal-126
to-noise ratio or obvious artifacts), or when there was indication of antagonist 127

6
activation (rectus femoris sEMG activity). All data analyses were carried out with 128
MATLAB® Software 7.6.0 R2010a. 129
130
2.3 Outcome parameters 131
132
ROM was determined during LV; VMAX during all velocities. All other parameters were 133
calculated at each velocity and were extracted from the RMS-EMG and the computed 134
torque signals. Average RMS-EMG, expressed in mV, was computed as the square 135
root of the area underneath the RMS-EMG time curve, divided by the duration of the 136
time interval considered. The time interval started 200ms prior to the time 137
corresponding to VMAX and ended at the time corresponding to 90% of the full ROM. 138
From the computed torque signal, four instrumented spasticity parameters were 139
developed. Firstly, the amount of work required to stretch the muscle was calculated 140
as the integral of the net internal torque from the joint position at VMAX to 90% of the 141
ROM (referred to as ‘work’ and expressed in J). Torque was additionally analyzed at 142
70° knee flexion, an angle that corresponded to the overall mid-ROM of all children 143
(‘torque’, expressed in Nm). The angle of catch (AOC) was defined as the angle that 144
corresponded to the time of minimum power after maximum power and was 145
expressed as a percentage of the ROM [14]. Finally, the value of the power at the 146
AOC was used to quantify catch severity [14] (‘AOC power’, expressed in W). The 147
AOC and AOC power were calculated from the first HV stretch following the 148
procedure described in [14]. All other parameters were calculated by taking the 149
average of 2-4 repetitions per velocity. To provide a measure of the severity of 150
spasticity, the absolute change between MV and LV (MV-LV) and between HV and 151

7
LV (HV-LV) was also calculated for every parameter (except ROM, AOC, and AOC 152
power). 153
154
155
2.4 Statistical analysis 156
157
All parameters were checked for normal distribution using the Kolmogorov-Smirnov 158
test with p>0.1 indicating a normal distribution. To ensure that the velocity of passive 159
stretches was performed consistently between measurement sessions, VMAX at each 160
velocity was first compared between sessions using a paired samples t-test, or in 161
case of non-normal distributions, a Wilcoxon Matched Pairs Test (WMPT). Next, to 162
evaluate the sensitivity of the parameters to treatment with BTX-A, the average 163
change between pre- and post-treatment sessions was calculated. It was 164
hypothesized that ROM, AOC, and AOC power would increase and that RMS-EMG, 165
torque, and work parameters would decrease post-treatment. Average change 166
between pre- and post-treatment sessions was interpreted in view of the minimal 167
detectable change (MDC). MDC values were calculated from the standard error of 168
measurement (SEM) values reported by Bar-On et al. [13,14] (MDC=SEM*1.645*√2) 169
[16] (Supplementary Material 1). Those parameters whose average change 170
exceeded the MDC were compared between sessions using a paired samples t-test, 171
or a WMPT, as appropriate. 172
173
Finally, to explore the relationships between different outcome parameters, Pearson 174
product-moment correlation coefficients (or Spearman rank correlation coefficients, 175
as appropriate) were computed between all parameters. Correlations <0.20 were 176

8
considered poor; 0.21–0.40 fair; 0.41–0.60 moderate; 0.61–0.80 good; and 0.81–177
1.00, very good [17]. It was hypothesized that the pre-post change in torque 178
parameters would have the highest positive correlations to pre-post change in EMG 179
parameters at HV and at HV-LV. Significance was set at p<0.05. All statistical 180
analyses were performed using Statistica 10 (StatSoft). 181
182
183
3. Results 184
185
Nineteen children with CP participated in the study (Table 1). The mean dose for the 186
MEH was 3.02 U/kg (SD 0.75 U/kg; range: 1-4 U/kg). Assessments were performed 187
on average 9±15 days before and 43±16 days after BTX-A injection (see Figure 2 for 188
a representative example of EMG, torque, position, and power signals pre and post 189
BTX-A). All change pre-post parameters, except RMS-EMG at LV, had a normal 190
distribution. Mean values of all parameters at both sessions can be found in Table 2. 191
Comparison of VMAX between sessions indicated that at HV, muscles were stretched 192
significantly faster during the post-treatment session (increase of 31.5°/sec). ROM 193
increased around 10° post BTX-A, which was significant. At HV stretches, all 194
muscles had an EMG onset during both pre and post BTX-A assessments. RMS-195
EMG parameters significantly decreased post BTX-A at all stretch velocities. Torque 196
and work reduced significantly at HV-LV (decrease of 2.79Nm and 1.18J, 197
respectively), as well as torque at HV (decrease of 3.82Nm). AOC appeared 12.73% 198
further in the ROM and AOC power increased by 3.50W post BTX-A. Both 199
improvements were significant. 200
201

9
The individual and average change pre-post BTX-A for all outcome parameters and 202
their corresponding MDC values can be found in Figure 3.The average change 203
values of ROM at LV (10.90±16.16°), RMS-EMG at HV (0.012±0.011mv), RMS-EMG 204
at HV-LV (0.008±0.009mv), torque at HV-LV (2.79±3.27Nm), and AOC 205
(12.73±16.31%) were larger than their corresponding MDC values (Supplementary 206
Material 1). 207
208
At HV-LV, good correlations were found between RMS-EMG change and torque 209
change pre-post BTX-A (r=0.52), between AOC change and torque change pre-post 210
BTX-A (r=0.58), and a moderate correlation between ROM change and work change 211
pre-post BTX-A (r=0.45). At LV, a moderate correlation was found between ROM 212
change and work change pre-post BTX-A (r=0.45). 213
214
215
4. Discussion 216
217
This study provides a clinically-applicable, instrumented method to quantify the 218
response to BTX-A in spastic MEH in children with CP. Selected parameters, 219
extracted from EMG and torque, were shown to be sensitive to measure effect post 220
BTX-A. 221
222
Clinical spasticity assessments, such as the MAS and MTS, have been criticized for 223
their poor reliability [7,8] and questionable sensitivity in identifying the response to 224
treatment [18]. Moreover, the limited range of the ordinal scoring of the MAS results 225
in patients being clustered into broad severity groups [19]. Although the MTS has a 226

10
smaller gradation, Fosang et al. reported intra-assessor measurement errors up to 9° 227
in the MEH [20]. This results in an MDC value of 21°, which is higher than the 228
average reported change post BTX-A ranging from 2-12° [21,22]. In this study, on the 229
other hand, parameters from the instrumented assessment provided not only 230
sensitive continuous data, but also captured higher variable levels of response to 231
BTX-A treatment. Understanding this variability could enhance treatment delineation 232
and ensure more targeted and individualized anti-spasticity care. 233
234
Clinical tests in isolation cannot discern the relative contributions of neural and non-235
neural components of muscle tone. By integrating electrophysiological and 236
biomechanical parameters, a more comprehensive assessment was achieved. 237
Parameters investigating the change between velocities are able to capture velocity-238
dependent spasticity as defined by Lance [1]. These proved most sensitive to 239
treatment with BTX-A, with an average of 53% reduction in velocity-dependent RMS-240
EMG and a 47% reduction in torque. The moderate correlation between the change 241
in RMS-EMG% and in torque post BTX-A confirms that the decrease in torque is 242
partially influenced by velocity-dependent neurogenic factors. 243
244
All injected muscles showed an increased electrophysiological response to passive 245
HV stretches, indicating that spasticity was correctly diagnosed in all children. In 14 246
of the 19 muscles that were tested, we also found an EMG onset during LV stretches. 247
This may imply the presence of position- or muscle length-dependent spasticity, as 248
also reported in stroke [23] and spinal cord injured [24] patients. It has been 249
suggested that with increasing muscle length, group II afferent neurons activate 250
baseline muscle spindle activity, which in turn lowers the threshold, but not the 251

11
amplitude of the stretch reflex [25]. In the current study, the torque parameters at LV 252
did not change post BTX-A and the decrease in EMG at LV was clinically not relevant 253
(below the MDC). Furthermore, at LV, the change in torque was not correlated to the 254
change in EMG. This suggests that the low intensity muscle activity present during 255
LV stretches does not contribute towards the simultaneously measured torque and 256
that neither parameter is affected by BTX-A treatment. Torque parameters at LV are 257
thus believed to represent intrinsic stiffness (due to secondary changes of the spastic 258
muscle) rather than the neural components of tone [26]. On the other hand, the 259
change pre-post BTX-A in ROM at LV did significantly exceed the MDC. Since little 260
significant effect of BTX-A on intrinsic stiffness has been reported [27], and casting is 261
known to alter the extensibility of muscle and joint, this increased ROM is thought to 262
reflect the effect of post-injection casting. Alhusaini et al. [27] have also reported 263
increased ROM and unchanged intrinsic stiffness due to BTX-A during low-velocity 264
stretches of the gastrocnemius in children with CP. We conclude that it is important to 265
distinguish those patients with increased intrinsic stiffness from those with increased 266
reflex-related torque. This will already help determine the optimal treatment modality 267
for the individual child. 268
269
The AOC and its power value increased post BTX-A, suggesting an increase in the 270
velocity-threshold and a reduction in the catch severity after treatment. However, it 271
should be noted that Wu et al. have warned that the AOC position is positively 272
correlated to the velocity of stretch, with later catches occurring the higher the 273
velocity [28]. Since in the current study, the MEH muscles were stretched at a 274
significantly faster velocity post BTX-A, this could have affected the results. We 275
believe that considering the intensity with which the catch occurs, together with the 276

12
position, improves the interpretation of the spastic catch. However the repeatability of 277
this parameter should be enhanced. 278
279
In the current study, 12 children showed an improvement in RMS-EMG at HV-LV that 280
exceeded MDC, 6 were within the positive and negative MDC values, and 1 showed 281
increased RMS-EMG activity (i.e. worsening of spasticity) that was smaller than the 282
negative MDC value (Figure 3). In comparison, Pandyan et al. [18] measured RMS-283
EMG during fast passive stretches of the biceps muscle in stroke patients before and 284
after BTX-A injections. In accordance to our findings, they reported large response 285
variability, whereby 9 of their 14 subjects had decreased and 4 had increased RMS-286
EMG post BTX-A. They did not however quantify the MDC of the RMS-EMG 287
parameter, which may have led to an overestimation of responders and non-288
responders. In fact, to the best of our knowledge, no study has used information on 289
the measurement error of instrumented spasticity assessments to interpret the effect 290
of BTX-A, making comparisons difficult. 291
292
Despite the sensitivity of the instrumented measurement method, some 293
methodological limitations need to be considered. A first limitation is the significantly 294
higher stretch velocity during post-treatment sessions. However, despite faster 295
stretching post BTX-A, there was still an overall reduction in the spasticity 296
parameters. Furthermore, as has been reported by Chen et al. [12], BTX-A can 297
increase the velocity threshold of the spastic muscle, which could have accounted for 298
the increased VMAX post BTX-A. The VMAX post BTX-A was also closer to the velocity 299
at which the MEH of typically developing children is stretched [13]. A second possible 300
limitation is the lack of EMG normalization. This may have accounted for some of the 301

13
response variability seen among children. However, since BTX-A is known to affect 302
strength, normalization to e.g. maximum voluntary contraction is not suitable and will 303
only increase variability [29]. To ensure reliability of the calculated parameter and 304
minimize variability, a thoroughly standardized electrode application was applied. 305
This standardized procedure without normalization resulted in reliable RMS-EMG 306
parameters (Supplementary Material 1). Finally, while this study investigated the 307
effect of BTX-A on passive spasticity, it is also recommended to capture the effect of 308
BTX-A on functional activities (e.g. walking). More specifically, as only weak to 309
moderate correlations between clinical spasticity scores and gait parameters have 310
been reported [30], it would be useful to explore correlations between parameters 311
from instrumented tests and gait analysis. 312
313
In conclusion, the current study proposes an instrumented method to quantify the 314
effect of BTX-A on MEH spasticity in children with CP. Spasticity parameters that 315
were sensitive to treatment and larger than the MDC were identified. These could 316
potentially be used to categorize subjects according to the level of response and thus 317
assist in treatment planning. This consolidates the clinical validity of the proposed 318
method and opens up possibilities of exploring the effects in other muscles or of other 319
tone-reducing treatments such as selective dorsal rhizotomy and intrathecal baclofen. 320
Furthermore, combining multiple, integrated parameters was found superior over 321
interpreting a single parameter obtained from an isolated signal to assess treatment 322
efficacy. Increased torque at LV, representing intrinsic rather than reflex-related 323
stiffness, did not change post BTX-A. However, the large response variability among 324
children requires further studies using objective, instrumented measurements that 325
assess the effect of BTX-A. A better understanding of factors that determine 326

14
treatment outcome will allow individualized treatment planning and increase the 327
functional potential of children with CP. 328
329
330
Conflict of interest 331
There were no conflicts of interest. 332
333
334
Acknowledgements 335
This work was made possible by a grant from the Doctoral Scholarships Committee 336
for International Collaboration with non EER-countries (DBOF) of the Katholieke 337
Universiteit Leuven, Belgium. This work was further supported by a grant from 338
Applied Biomedical Research from the Flemish agency for Innovation by Science and 339
technology (IWT-TBM: grant number 060799); and by an unrestricted educational 340
grant from Allergan, Inc. (USA). 341
342
343
References 344
345
[1] Lance JW. The control of muscle tone, reflexes, and movement: Robert 346
Wartenbeg Lecture. Neurology 1980;30(12):1303. 347
[2] Sanger TD, Delgado MR, Gaebler-Spira D, Hallett M, Mink JW. Classification and 348
Definition of Disorders Causing Hypertonia in Childhood. Pediatrics 2003;111:89–97. 349

15
[3] Graham HK, Aoki KR, Autti-Rämö I, Boyd RN, Delgado MR, Gaebler-Spira DJ, et 350
al. Recommendations for the use of botulinum toxin type A in the management of 351
cerebral palsy. Gait and Posture 2000;11:67–79. 352
[4] Desloovere K, Schörkhuber V, Fagard K, Van Campenhout A, De Cat J, Pauwels 353
P, et al. Botulinum toxin type A treatment in children with cerebral palsy: evaluation of 354
treatment success or failure by means of goal attainment scaling. European Journal 355
of Paediatric Neurology 2012;16:229–36. 356
[5] Bohannon RW, Smith MB. Interrater reliability of a modified Ashworth scale of 357
muscle spasticity. Physical Therapy 1987;67:206–7. 358
[6] Boyd RN, Graham HK. Objective measurement of clinical findings in the use of 359
botulinum toxin type A for the management of children with cerebral palsy. European 360
Journal of Neurology 1999;6:23–35. 361
[7] Haugh a B, Pandyan a D, Johnson GR. A systematic review of the Tardieu Scale 362
for the measurement of spasticity. Disability and Rehabilitation 2006;28:899–907. 363
[8] Platz T, Eickhof C, Nuyens G, Vuadens P. Clinical scales for the assessment of 364
spasticity, associated phenomena, and function: a systematic review of the literature. 365
Disability and Rehabilitation 2005;27:7–18. 366
[9] Cousins E, Ward AB, Roffe C, Rimington LD, Pandyan AD. Quantitative 367
measurement of poststroke spasticity and response to treatment with botulinum toxin: 368
a 2-patient case report. Physical Therapy 2009;89:688–97. 369
[10] Marinelli L, Trompetto C, Mori L, Vigo G, Traverso E, Colombano F, et al. 370
Manual linear movements to assess spasticity in a clinical setting. PloS One 371
2013;8:53627. 372
[11] Lee H-M, Chen J-JJ, Wu Y-N, Wang Y-L, Huang S-C, Piotrkiewicz M. Time 373
course analysis of the effects of botulinum toxin type a on elbow spasticity based on 374

16
biomechanic and electromyographic parameters. Archives of Physical Medicine and 375
Rehabilitation 2008;89:692–9. 376
[12] Chen J-JJ, Wu Y-N, Huang S-C, Lee H-M, Wang Y-L. The use of a portable 377
muscle tone measurement device to measure the effects of botulinum toxin type a on 378
elbow flexor spasticity. Archives of Physical Medicine and Rehabilitation 379
2005;86:1655–60. 380
[13] Bar-On L, Aertbelien E, Wambacq H, Severijns D, Lambrecht K, Dan B, et al. 381
Clinical measurement to quantify spasticity in children with cerebral palsy by 382
integration of multidimensional signals. Gait and Posture 2013;38:141-7. 383
[14] Bar-On L, Aertbeliën E, Molenaers G, Bruyninckx H, Monari D, Jaspers E, et al. 384
Comprehensive quantification of the spastic catch in children with cerebral palsy. 385
Research in Developmental Disabilities 2012;34:386–96. 386
[15] Daniels L, Worthingham C. Muscle testing techniques of manual examination. In 387
Muscle testing techniques of manual examination. 4th ed. Philadelphia: WB 388
Saunders; 1986:4–26. 389
[16] De Vet HC, Terwee CB, Ostelo RW, Beckerman H, Knol DL, Bouter LM. Minimal 390
changes in health status questionnaires: distinction between minimally detectable 391
change and minimally important change. Health and Quality of Life Outcomes 392
2006;4:54. 393
[17] Katz JN, Larson MG, Phillips CB, Fossel AH, Liang MH. Comparative 394
Measurement Sensitivity of Short and Longer Health Status Instruments. Medical 395
Care 2013;30:917–25. 396
[18] Pandyan AD, Vuadens P, Van Wijck FM, Stark S, Johnson GR, Barnes MP. Are 397
we underestimating the clinical efficacy of botulinum toxin (type A)? Quantifying 398

17
changes in spasticity, strength and upper limb function after injections of Botox to the 399
elbow flexors in a unilateral stroke population. Clinical Rehabilitation 2002;16:654–400
60. 401
[19] Condliffe EG, Clark DJ, Patten C. Reliability of elbow stretch reflex assessment 402
in chronic post-stroke hemiparesis. Clinical neurophysiology 2005;116:1870–8. 403
[20] Fosang AL, Galea MP, McCoy AT, Reddihough DS, Story I. Measures of muscle 404
and joint performance in the lower limb of children with cerebral palsy. 405
Developmental Medicine and Child Neurology 2003;45:664–70. 406
[21] Kelly B, MacKay-Lyons MJ, Berryman S, Hyndman J, Wood E. Assessment 407
protocol for serial casting after botulinum toxin a injections to treat equinus gait. 408
Pediatric Physical Therapy 2008;20:233–41. 409
[22] Scholtes VA, Dallmeijer AJ, Knol DL,Speth LA, Maathuis CG, Jongerius PH, et 410
al. Effect of multilevel botulinum toxin a and comprehensive rehabilitation on gait in 411
cerebral palsy. Pediatric Neurology 2007;36:30–9. 412
[23] Malhotra S, Cousins E, Ward A,Day C, Jones P, Roffe C, et al. An investigation 413
into the agreement between clinical, biomechanical and neurophysiological 414
measures of spasticity. Clinical Rehabilitation 2008;22:1105–15. 415
[24] Van der Salm A, Veltink PH, Hermens HJ, Ijzerman MJ, Nene A V. Development 416
of a new method for objective assessment of spasticity using full range passive 417
movements. Archives of Physical Medicine and Rehabilitation 2005;86:1991–7. 418
[25] Burke D, Gillies JD, Lance JW. The quadriceps stretch reflex in human 419
spasticity. Journal of Neurology, Neurosurgery, and Psychiatry 1970;33:216–23. 420
[26] Foran JRH. Review Structural and mechanical alterations in spastic skeletal 421
muscle. Developmental Medicine and Child Neurology 2005:713–7. 422

18
[27] Alhusaini A a a, Crosbie J, Shepherd RB, Dean CM, Scheinberg A. No change in 423
calf muscle passive stiffness after botulinum toxin injection in children with cerebral 424
palsy. Developmental Medicine and Child Neurology 2011;53:553–8. 425
[28] Wu Y-N, Ren Y, Goldsmith A, Gaebler D, Liu SQ, Zhang LQ. Characterization of 426
spasticity in cerebral palsy: dependence of catch angle on velocity. Developmental 427
Medicine and Child Neurology 2010;52:563–9. 428
[29] Phadke CP, Ismail F, Boulias C. Assessing the neurophysiological effects of 429
botulinum toxin treatment for adults with focal limb spasticity: a systematic review. 430
Disability and Rehabilitation 2012;34:91–100. 431
[30] Desloovere K, Molenaers G, Feys H, Huenaerts C, Callewaert B, Van de Walle 432
P. Do dynamic and static clinical measurements correlate with gait analysis 433
parameters in children with cerebral palsy? Gait and Posture 2006;24:302–13. 434
435
TABLES 436
Table 1. Children’s characteristics 437
Children’s characteristics (n=19)
Mean age (SD) (years) 7.20 (3.09)
Male/female (n) male: 10, female: 9
Diagnosis (n)
- Unilateral involvement
- Bilateral involvement
3 right hemiplegia, 3 left hemiplegia
11 diplegia, 2 quadriplegia
GMFCS (I-IV) (n) I: 6, II: 9, III: 3, IV: 1
MAS MEH (0-4) (number of muscles) 0: 1, 1: 1, 1+: 4, 2: 11, 3: 2
Average MTS MEH (SD) -70.47˚ (26.84˚)

19
GMFCS: Gross Motor Function Classification Score; MAS MEH: Modified Ashworth 438
Score of the medial hamstrings from the pre-treatment session; MTS MEH: average 439
Modified Tardieu Score of the medial hamstrings from the pre-treatment session. 440
441
Table 2. Average and standard deviation values of spasticity parameters pre and 442
post BTX-A treatment. 443
Pre BTX-A Post BTX-A p
ROM (°) LV 73.77 (11.02) 84.67 (13.38) 0.009
VMAX (°/sec) LV 31.21 (10.05) 33.56 (11.26) 0.495
MV 82.83 (32.42) 76.73 (23.85) 0.486
HV 281.43 (39.98) 312.96 (43.88) 0.007
RMS-EMG (µv) LV a4.44 (7.31) a3.12 (7.60) a0.040
MV 14.30 (12.20) 8.67 (5.78) 0.025
HV 25.10 (12.01) 13.40 (8.62) <0.001
MV-LV 6.20 (5.75) 2.93 (3.68) 0.001
HV-LV 16.27 (9.94) 8.31 (7.16) <0.001
Torque (Nm) LV 3.19 (2.47) 2.57 (3.65) 0.535
MV 3.92 (3.44) 2.89 (3.00) 0.316
HV 10.49 (5.66) 6.67 (3.54) <0.001
MV-LV 0.73 (1.67) 0.26 (0.93) 0.244
HV-LV 7.10 (4.14) 4.31 (2.12) 0.002
Work (J) LV 2.85 (2.93) 2.44 (2.06) 0.574
MV 3.35 (2.41) 3.68 (3.37) 0.674
HV 6.57 (3.39) 6.20 (5.01) 0.692
MV-LV 1.11 (1.34) 0.65 (0.60) 0.078

20
HV-LV 4.32 (2.72) 3.14 (2.55) 0.020
AOC (%) HV 79.77 (12.62) 92.50 (9.30) 0.003
AOC power (W) HV -5.94 (6.51) -2.44 (4.34) 0.007
LV: low velocity stretch; MV: medium velocity stretch; HV: high velocity stretch; MV-444
LV: medium velocity stretch minus low velocity stretch; HV-LV: high velocity stretch 445
minus low velocity stretch; ROM: range of motion; VMAX: maximum angular velocity; 446
Torque: torque at 70˚ knee flexion; AOC: angle of catch defined as the angle 447
corresponding to the time of the first minimum power value after the time of the 448
maximum power, expressed as a percentage of the full range of motion; AOC power: 449
the power value at AOC. a Due to the skewed distribution of this parameter, median 450
and inter quartile ranges are provided and compared using the Wilcoxon Matched 451
Pairs Test. p<0.05 452

1
FIGURES 453
454
455
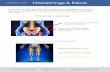
Figure 1. Instrumented spasticity assessment of the medial hamstrings muscle: test 456
starting position, direction of stretch (white arrow) and instrumentation. (1) a six DoF 457
force-sensor attached to a shank orthosis on the posterior aspect of the lower leg 458
(torque measurement); (2) two inertial measurement units (joint angle measurement); 459
and (3) surface electromyography (sEMG) of the medial hamstrings and rectus 460
femoris (muscle activity measurement). sEMG data from the rectus femoris were 461
utilized to ensure no active assistance of the patient during the passive stretches. 462
3
2
1

1
463
Figure 2. Pre (top row) and post (bottom row) BTX-A measurement of a child with spastic CP: RMS EMG-time (a, e), torque-464
position (b, f), position-time (c, g), and power-time graphs (d, h) during low (pink/ light gray), medium (green/gray), and high 465
(blue/black) velocity stretches. The position of the angle of catch (AOC) is indicated on the position- and power-time graphs. 466
467

1
468 469
470
471
472
473
474
475
476
477
478
479
480
481
482
483
484
485
486
487
-10
-5
0
5
10
15
20
25
30
RM
S-E
MG
HV
-LV
(µv
)
-30
-20
-10
0
10
20
30
40
50R
OM
LV
(de
g)
-30-20-10
01020304050
AO
C H
V (
%)
-15
-10
-5
0
5
10
15
20
Pow
er H
V (
W)
(j)
(c)
(i)
-6
-4
-2
0
2
4
6
Wor
k H
V (
J)
-6
-4
-2
0
2
4
6
8
Wor
k H
V-L
V (
J)
(h)
(a) -100-80-60-40-20
020406080
100
VM
AX
HV
(de
g/se
c)
(b)
(d)
-6-4-202468
1012
Tor
que
HV
(N
m)
-4
-2
0
2
4
6
8
10
12
Tor
que
HV
-LV
(N
m)
(f) (e)
(g)
-15-10-505
101520253035
RM
S-E
MG
(µv)

2
Figure 3. Change between pre and post BTX-A measurements in: a) range of motion 488
(ROM) at low velocity (LV); b) maximum angular velocity (VMAX) at high velocity (HV); 489
c) root mean square electromyography (RMS-EMG) at HV; d) change in RMS-EMG 490
between HV and LV (HV-LV); e) torque at 70˚ knee flexion at HV; f) torque at 70˚ 491
knee flexion at HV-LV; g) work at HV; h) work at HV-LV; i) relative position of the 492
angle of catch (AOC) at HV; and j) the power value at the AOC at HV. Each diamond 493
represents the individual value of a MEH (per child). The bar represents the mean 494
value for all muscles. The dashed horizontal lines represent the minimal detectable 495
change values. 496
Related Documents