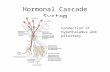
ED yr V Internal diseases, endocrinology Diseases of pituitary and hypothalamus Prof. Marek Bolanowski, M.D., Ph.D. Department of Endocrinology, Diabetes and Isotope Therapy Wrocław Medical University

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

ED yr V
Internal diseases, endocrinology
Diseases of pituitary and
hypothalamus
Prof. Marek Bolanowski, M.D., Ph.D. Department of Endocrinology,
Diabetes and Isotope Therapy
Wrocław Medical University


Pituitary tumors
Hypopituitarism
Diabetes insipidus

Pituitary tumors adenomas
Monoclonal, slowly growing, benign neoplasms
• clinical 0.02-0.025% but autopsy 10-20%
Hormonally active
• prolactin - prolactinoma - 50%
• GH - acromegaly - 20%
• ACTH - Cushing’s disease - 10%
• TSH, LH, FSH, α-subunit
Hormonally inactive - 20%

Other pituitary tumors
• Craniopharyngioma
• Glioma, chordoma
• Germinoma, dysgerminoma
• Metastatic

Metastatic tumors to the pituitary
• breast 50%
• lung 20%
• gastrointestinal tract 6-10%
• prostate 6-10%
• melanoma 2%
• other 8-16%

Pituitary tumors
• presence of endo- or exogenous stimulatory
factors/lack of inhibitory factors
• receptor defects, mutations, protooncogenes
activation, second messenger disturbances
• differentiation of stem cells
• clone expansion
• tumor formation
11q13 chromosome deletion in MEN-1, only

Pituitary tumors
Mass effects
• headache and visual disturbances: visual loss, visual field deficit, optic pallor, ocular dysmotility, pupillary abnormalities
Radiological
• sella enlargement, erosion of dorsum
• calcifications in the tumor
Hormonal
• hormonal excess/deficit
• diabetes insipidus


Pituitary adenomas Pituitary adenomas
• microadenomas < 10 mm
• macroadenomas ≥ 10 mm

Clinical presentation of
hyperprolactinemia in women
• amenorrhea and galactorrhea 81.0%
• amenorrhea 12.0%
• oligomenorrhea and galactorrhea 1.4%
• regular menses and galactorrhea 1.4%
• visual field defect 1.4%

Clinical presentation of
hyperprolactinemia in men
• loss of libido/potency 47%
• headache 13%
• visual failure 13%
• gynecomastia 6%
• galactorrhea 2%

Diagnosis of hyperprolactinemia
• Sustained hyperprolactinemia
> 20 ng/ml in women
> 10 ng/ml in men
< 200 ng/ml - microprolactinoma
> 200 ng/ml - macroprolactinoma
100-200 ng/ml – pseudoprolactinoma
• Macroprolactinemia

Macroadenoma of the pituitary
(acromegaly)


Symptoms and signs of acromegaly
• acral/facial changes 98%
• oligo/amenorrhea 72%
• excessive perspiration 64%
• headache 55%
• paresthesias/carpal tunnel syndrome 40%
• erectile dysfunction 36%
• hypertension 28%
• goiter 19%


Gigantism

Diagnostic criteria of acromegaly
• lack of GH suppression during OGTT < 1 µg/l (ng/ml)
• elevated IGF-1 level

Clinical features of Cushing’s
disease/Cushing’s syndrome
• central obesity 85%
• facial plethora 80%
• hirsutism 75%
• menstrual disorders 75%
• striae 50%
• weakness 50%


Localization tests in Cushing’s
syndrome
• ACTH
• high dose dexamethasone suppression test
• CRH stimulation test
• pituitary MRI
• adrenal CT/MRI
• inferior petrosal sinus sampling
• Cortisol profile
• Urinary free cortisol excretion

Clinical presentation of TSHoma
• goiter 94%
• visual field defects 42%
• ophthalmopathy 6%
• acromegaly 16%
• amenorrhea/galactorrhea 12%

Baseline laboratory changes in
TSHomas
• T4, T3 elevated
• TSH detectable
• α-subunit/TSH ratio > 1.0
• GH, Prl, LH, FSH elevated

Gonadotroph adenomas
• decreased visual acuity 43%
• hypopituitarism 22%
• asymptomatic 17%
• headache 8%
• combination of symptoms 10%
• testes enlargement rare
• ovarian hyperstimulation rare

Gonadotroph adenomas
• normal LH, FSH for age in women
• sometimes LH, FSH increased in men
• testosterone decreased in men
• exaggerated LH, FSH response in TRH test

Differential diagnostics
• pseudotumors / pituitary cells hyperplasia
• incidentaloma
• empty sella
• lymphocytic hypophysitis

Pituitary enlargement
• Pregnancy
• Hypothyroidism
• CRH or GHRH secretion in excess

Empty sella

Pituitary carcinoma
• rare, less than 1%
• about 100 cases in the literature
• carcinoma similar to invasive adenoma
• clinical course with frequent recurrences, treatment
resistance and manifestation of metastases

Surgical treatment
• selective, transsphenoidal adenomectomy
• repeated approaches
• transcranial surgery

The goals of neurosurgery
• complete cure
• vision preservation
• hormonal balance

Medical treatment of prolactinomas
Dopamine agonists:
• ergot derivatives
bromocriptine: Parlodel, Bromergon, Bromocorn, Ergolaktyna
1-3 times daily, 1.25-15 mg/day
pergolide, lisuride, once daily
Cabergoline: Dostinex 0.25-2 mg twice weekly
• non-ergot derivatives
quinagolide: Norprolac 37.5-150 mg/day

• The effect of
bromocriptine
treatment on
prolactinoma

Medical treatment of acromegaly -
GH secreting tumors
• somatostatin analogs
octreotide: Sandostatin, Sandostatin LAR
lanreotide: Somatuline Autogel
vapreotide
• dopamine agonists
bromocriptine: Parlodel, Bromergon
cabergoline: Dostinex
• GH receptor antagonist
pegvisomant blocks peripheral GH action


Radiotherapy of pituitary tumors
• conventional radiotherapy 40-50 Gy, fractioned in
doses 2.0-2.5 Gy at 4-5 sessions a week
• gamma unit stereotactic radiosurgery „gamma knife”

Incidentaloma
Problem of modern technology
• head trauma
• accidents
• CNS events
with a need for head CT/MRI scans

Pituitary incidentaloma
• on CT scans up to 20%
• on MR scans 10%
• autopsy 10% - 20% (micro)

Incidentaloma – management
algorithm
• hormonal function
• size, growth
• visual abnormalities presence
• other local disturbances
• generalized systemic disturbances

Pituitary incidentaloma
hormonal function assessment
functioning non-functioning
Prl GH, ACTH, macro micro
TSH, Gn visual field
function
MR
½, 1, 2, 5 years
DA
MR
surgery 1, 2, 5 years
SMSA

Hypopituitarism
• Idiopathic
• Due to pituitary tumor
• Iatrogenic
– Neurosurgery
– Radiotherapy

Hypopituitarism
• secondary hypocortisolism
• secondary hypothyroidism
• secondary hypogonadism
• GH deficiency

Secondary hypocortisolism
(ACTH deficiency)
• nausea, vomiting, abdominal pain, hypothermia
• hypovolemia, low blood pressure, postural hypotension
• asthenia, hypoglycemia
• hyponatremia, hyperkalemia
• no skin hyperpigmentation
• low ACTH, low cortisol

Secondary hypothyroidism
(TSH deficiency)
• cold intolerance, easy fatigability, weakness
• constipation, pale and dry skin, intellectual impairment
• bradycardia, slowed speech, hypothermia, oedema
• delayed relaxation of deep tendon reflexes
• low TSH and fT4

Secondary hypogonadism
(gonadotropin deficiency)
• eunuchoid proportions and sexual infantilism
(prior to puberty)
• absence of axillary and pubic hair, no breast
development
• secondary or primary amenorrhea
• impotence, loss of libido, infertility
• decrease in muscle and bone mass
• low LH/FSH, E2, T

GH deficiency
• growth retardation (prior to puberty)
• body composition changes:
adipose tissue increase,
muscles and bone mass decrease
• no GH increment following stimulation, low IGF-1

Sequence of the pituitary
hormonal deficiencies
• GH, IGF-1
• LH, FSH, E2, P, T
• TSH, fT4
• ACTH, cortisol
Necessity for hormonal replacement

Hormonal replacement
• Cortison, Hydrocortison 10-30 mg/d
• L-Thyroxine 50-150 mcg/d
• Estrogen/Progesterone
• Testosteron
• Growth hormone

Diabetes insipidus
• deficiency/lack of ADH
• kidneys insensitivity for ADH
• polyuria, polydipsia, thirst
• serum hyperosmolality > 295 mOsm/kg H20
• urine hypoosmolality
• urine specific gravity 1000-1008 g/l

Diabetes insipidus
• Desmopressin
Minirin tabl. 2 x 0.1 – 3 x 0.2 mg daily
Adiuretin nasal spay 1-2 x 10-40 µg
• Lysine-Vasopressin
Related Documents