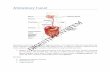
Digestive system
Oct 31, 2014
Complete Notes of Digestive system,
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript


Digestive system
• Organs of digestive system: Mouth, tongue, oesaphageo-pharynx, oesaphagus, stomach, duodenum, Jejunum, Ileum, Ascending colon, Transverse colon, Descending colon, Rectum, Anus.
• Accessory organs of digestive system: Salivary glands, Tongue, Liver, Gall bladder, Gastric glands, Intestinal glands, Goblet cells.
• Sphincters of GIT: Cardiac sphincter, Pyloric sphincter, Ileocecal sphincter, Sphincter of Odii, Anal sphincter.

Functions of Digestive system
• Ingestion, Movement of food, Digestion (Mechanical digestion eg, maceration with the help of teeth, mixing of food in the stomach, and chemical digestion-with the help of enzymes)Absorption (Assimilation),Defecation.

Histology of GIT: From within outside• 1. Mucosa: Epithelial cells absorption, secretion,; Goblet cells-
mucus, enteroendocrine cells- hormones. (Lamina propria-blood, lymphatic vessels, scattered lymph nodules)
• 2. sub-mucosa: Areolar connective tissue that binds to muscularis, blood vessels, Meissner plexus-ANS, for regulating secretions from glands)
• 3. Muscularis (inner circular and outer longitudinal smooth muscles), : Mouth, pharynx, upper esophagus- made of skeletal muscles use full for swallowing, and external anal sphincter that helps in controlling defecation.
• Rest of GIT muscularis is made of inner circular and outer longitudinal muscle cells that helps in the GIT movements namely peristaltic and pendular / segmental movements to cause movement of food and mixing food in GI canal. This regulated by Myenteric or Auerbach plexus present between circular and longitudinal muscles.
• 4. Serosa: Made up of epithelial cells and connective tissue cells.

Eating, Masticating, Drinking, Sucking, Tasting, Breathing, Vomiting, Digesting, deglutition,Speaking, Expression ( Smiling - Laughing - Crying - Kissing – Whistling, Smiling - Laughing - Crying - Kissing – Whistling)
The upper jaw, that is part of the skull . The lower jaw, connected with the upper jaw and with ability to move up-down and from side to side.

Mouth: Non-keratinized stratified squamous epithelium (esophagus and anal canal)
• The mouth or oral cavity is surrounded by the cheeks and lips. • The cheeks (buccal) contain buccinator muscle • The parotid duct opens adjacent to the 2nd molar tooth. • The lips (labia) contain numerous muscles that control the
mouth. • Vestibule is part of the cavity between the teeth and the cheeks
or lips.• Hard palate-anterior part of roof of the mouth (formed by part
of maxilla and palatine bone)• Soft palate: posterior part of roof of the mouth, it is arch shaped
muscular partition of between oropharynx and nasopharynx and lined by mucus membrane

EATING AND SWALLOWING
• the front teeth cut the food • - the side teeth tear and shred it • - the back teeth crush and grind it • - the saliva moistens the food• - the action of the tongue and the cheeks mix
it all up so that it is easy to swallow • - tiny pimples on the surface of the tongue,
the 'taste buds' tell you what you are tasting.


Tongue• The tongue is a muscular organ in the mouth. The tongue is covered with moist, pink
tissue called mucosa. Tiny bumps called papillae give the tongue its rough texture. Thousands of taste buds cover the surfaces of the papillae. Taste buds are collections of nerve-like cells that connect to nerves running into the brain.
• In the back of the mouth, the tongue is anchored into the hyoid bone. The tongue is vital for chewing and swallowing food, as well as for speech.
• The four common tastes are sweet, sour, bitter, and salty.• The tongue has many nerves that help detect and transmit taste signals to the brain. • The extrinsic muscles of tongue, hypoglosssus, styloglossus help to move the
tongue side to side and in and out. These movements maneuver food for chewing, shape the food into a round mass, force the food to the back of the mouth for swallowing (deglutition).
• The intrinsic muscles originate and insert within the tongue and alter the size and shape of the tongue for speech and swallowing.
• The frenulum , a fold of the mucus membrane in the mid line of under surface of the tongue attached to the floor of the mouth helps in limiting the movements of the tongue posteriorly.
• Taste buds sends impulses to cortex for expression of specific taste and to salivatory nuclei in the brain stem and then to salivary glands.




Taste buds• The majority of taste buds on the tongue sit on raised protrusions of the tongue surface
called papillae. There are four types of papillae present in the human tongue:
• Fungiform papillae - as the name suggests, these are slightly mushroom-shaped if looked at in longitudinal section. These are present mostly at the apex (tip) of the tongue, as well as at the sides. Innervated by facial nerve. They appear as red spots on the tongue - red because they are richly supplied with blood vessels. The total number of fungiform papillae per human tongue is around 200. Papillae at the front of the tongue have more taste buds (1-18) compared to the mid-region (1-9). It has been calculated that there are 1120 fungiform taste buds per tongue.
• Filiform papillae - these are thin, long papillae "V"-shaped cones that don't contain taste buds but are the most numerous. These papillae are mechanical and not involved in gustation. They are characterized by increased keratinization.
• Foliate papillae - these are ridges and grooves towards the posterior part of the roof of the mouth found on lateral margins. Innervated by facial nerve (anterior papillae) and glossopharyngeal nerve (posterior papillae).
• Circumvallate papillae - there are only about 10 to 14 of these papillae on most people, and they are present at the back of the oral part of the tongue. They are arranged in a circular-shaped row just in front of the sulcus terminalis of the tongue. They are associated with ducts of Von Ebner's glands, and are innervated by the glossopharyngeal nerve.

• Foliate papillae - these are ridges and grooves towards the posterior part of the roof of the mouth found on lateral margins. Innervated by facial nerve (anterior papillae) and glossopharyngeal nerve (posterior papillae). On average 5.4 foliate papillae per side of the tongue, 117 taste buds per foliate papillae, total = 1280 foliate taste buds per tongue.
• Circumvallate papillae - there are only about 10 to 14 of these papillae on most people, and they are present at the back of the oral part of the tongue. They are arranged in a circular-shaped row just in front of the sulcus terminalis of the tongue. They are associated with ducts of Von Ebner's glands, and are innervated by the glossopharyngeal nerve. 3-13 circumvallate papillae per tongue with 252 taste buds per papillae, total = 2200 circumvallate taste buds per tongue

Tongue• Taste buds contain the receptors for taste. They are located around the
small structures on the upper surface of the tongue, soft palate, upper esophagus and epiglottis, which are called papillae. These structures are involved in detecting the five (known) elements of taste perception: salty, sour, bitter, sweet, and umami.
• Taste buds contain the receptors for taste. They are located around the small structures on the upper surface of the tongue, soft palate, upper esophagus and epiglottis, which are called papillae. These structures are involved in detecting the five (known) elements of taste perception: salty, sour, bitter, sweet, and savory (or umami). Via small openings in the tongue epithelium, called taste pores, parts of the food dissolved in saliva come into contact with taste receptors.
• The gustatory (taste) cells, a chemoreceptor, occupy the central portion of the bud; they are spindle-shaped, and each possesses a large spherical nucleus near the middle of the cell. Those tiny hairs send messages to the brain, which interprets the signals and identifies the taste for you.


Salt taste
• Salt is sodium chloride (Na+ Cl-). Na+ ions enter the receptor cells via Na-channels. These are amiloride-sensitive Na+ channel (as distinguished from TTX-sensitive Na+ channels of nerve and muscle). The entry of Na+ causes a depolarization, Ca2+ enters through voltage-sensitive Ca2+ channels, transmitter release occurs and results in increased firing in the primary afferent nerve.

Sour taste
• Sour taste is acid and acid is protons (H+). There is exciting new evidence that there is an acid-sensing channel - the PKD2L1 channel1.This channel is a member of the transient receptor potential channel (TRP) family and is a non-selective cation channel. The activity of PKD2L1 is gated by pH (H+ ion concentration). This new discovery displaces the previous ideas that H+ ions block K+ channels causing a depolarization, or that H+ ions enter the cell through ENaC channels. These mechanisms may exist but do not lead directly to sour perception.

Sweet taste
• There are receptors T1R2 + T1R3) in the apical membrane that bind glucose (sucrose - a combination of glucose and fructose - and other carbohydrates). Binding to the receptor activates a G-protein which in turn activates phospholipase C (PLC-ß2). PLC generates IP3 and diacyl glycerol (DAG). These intracellular messengers, directly or indirectly, activate the TRPM5 channel and depolarization occurs. Ca2+ enters the cell through depolarization-activated Ca2+ channels, transmitter is released increasing firing in the primary afferent nerve.

Bitter taste
• Bitter substances bind to the T2R receptors activating the G-protein and causing activation of PLC. The second messengers DAG and IP3 are produced (by hydrolysis of phosphatidylinositol-4,5-bisphosphate) activating TRPM5 and mediating release of Ca2+ from internal stores. The elevated Ca2+ causes transmitter release and this increases the firing of the primary afferent nerve.

Umami taste• Umami is the taste of certain amino acids (e.g. glutamate, aspartate and related
compounds). It was first identified by Kikunae Ikeda at the Imperial University of Tokyo in 1909. It was originally shown that the metabotropic glutamate receptor (mGluR4) mediated umami taste. Binding to the receptor activates a G-protein and this elevates intracellular Ca2+. More recently it has been found that the T1R1 + T1R3 receptors mediate umami taste. Binding to the receptors activates the non-selective cation channel TRPM5 as for sweet and bitter receptors (i.e. via G-protein, PLC, IP3 and DAG - see above). Guanosine 5'-monophosphate (GMP) and inosine 5'-monophosphate (IMP) potentiate the effect of umami tastes by binding to another site of the T1R1 receptor.
• Monosodium glutamate, added to many foods to enhance their taste (and the main ingredient of Soy sauce), stimulates the umami receptors. But, in addition, there are ionotropic glutamate receptors (linked to ion channels), i.e. the NMDA-receptor, on the tongue. When activated by these umami compounds or soy sauce, non-selective cation channels open, thereby depolarizing the cell. Calcium enters, causing transmitter release and increased firing in the primary afferent nerve

Strange taste facts• Taste is mainly smell. Hold your nose, close your eyes, and try to tell
the difference between coffee or tea, red or white wine, brandy or whisky. In fact, with blocked nose (clothes peg or similar) you can't tell the difference between grated apple and grated onion - try it! Of course, this is because what we often call taste is in fact flavor. Flavour is a combination of taste, smell, texture (touch sensation) and other physical features (eg. temperature).
• The durian fruit smells horrible. Some people cannot bear to eat it because it smells so foul. But it is called the "King of Fruits" and tastes delicious. It is very large (can be the size of a football) and comes from South East Asia.

Salivary Gland• Type of Secretory Cells• Parotid: Serous: Inferior and anterior and anterior to the ears
between the skin and masseter muscle (Stensen’s duct- opens at the upper second Maxillary Molar tooth).[ANS: parasympathetic through glossopharyngeal nerve (CN IX) via the otic ganglion]
• Submandibular: Mixed: Beneath the base of the tongue in the posterior part of the floor of the mouth (Wharton’s ducts run superficially under the mucosa on either side of midline of the floor of mouth, opening on either side of the frenulum.[facial nerve (CN VII) via the submandibular ganglion]
• Sublingual: Mucus: Superior to the submandibular glands , Lesser sublingual (Rivinus’ ) ducts open to the floor of the mouth cavity.[facial nerve (CN VII) via the submandibular ganglion]
• Saliva: 99.5% water, 0.5% solids (Na& K -- Cl,HCO3, PO4,urea, uric acid, serum albumin and globulin,, mucin, lysozyme, & salivary amylase. Direct Sympathetic innervation of the salivary glands takes place via preganglionic nerves in the thoracic segments T1-T3 which synapse in the superior cervical ganglion with postganglionic neurons that release norepinephrine, cause increase in secretion.

Salivary glands•Minor salivary glands:
They are 1-2mm in diameter and unlike the other glands, they are not encapsulated by connective tissue only surrounded by it. The gland is usually a number of acini connected in a tiny lobule. A minor salivary gland may have a common excretory duct with another gland, or may have its own excretory duct. Their secretion is mainly mucous in nature (except for Von Ebner's glands) and have many functions such as coating the oral cavity with saliva. Von Ebner's glands are glands found in circumvallate papillae of the tongue. They secrete a serous fluid that begin lipid hydrolysis. They facilitate the perception of taste.
Starch is converted into maltotriose and maltose from amylose, or maltose, glucose and "limit dextrin" from amylopectin. Because it can act anywhere on the substrate, α-amylase tends to be faster-acting than β-amylase( in animals). During the ripening of fruit, β-amylase breaks starch into maltose, resulting in the sweet flavor of ripe fruit.

•
TOOTH ENAMEL (1), is the hardest of the parts of the tooth and also the hardest of all the tissues of human body. Tooth enamel is a protective tooth structure that covers the exposed part of a tooth, the crown. DENTIN (2) or IVORY, is the tissue below the tooth enamel that forms the main mass of a tooth. It supports the tooth enamel and absorbs the pressure of eating. The dentine consists of a number of micro-fibers imbedded in a dense homogeneous matrix of collagenous proteins. DENTAL PULP (3) , a soft connective tissue containing nerves and blood vessels, that nourish the tooth. It is the most internal structure of a tooth, surrounded by the dentine. Dental pulp is found in the soft center of the tooth, inside the pulp chamber and the root canal. CEMENTUM (4) , is the part of tooth anatomy that covers the dentine outside of the root (under the gum line) and it is attached to the bone of the jaw with little elastic fibers. Cementum is hard as bone but not as hard as the tooth enamel. GUMS (5) , the tough pink-colored tissue that covers the bone of the jaw and supports the tooth structure inside the alveolar bone. PERIODONTAL LIGAMENT (6) , the tissue between the cementum and the alveolar bone. It consists of tough little elastic fibers that keep the tooth attached to the jaw. ALVEOLAR BONE (7) , the bone of the jaw that keeps the tooth in its place, it feeds and protects it.


Incisors– one rootCanine– one rootFirst and Second molars have four cuspsUpper molars have three rootsLower molars have two roots

Teeth• Incisors. Incisors are the eight teeth in the front and center of your
mouth (four on top and four on bottom). These are the teeth that you use to take bites of your food. Incisors are usually the first teeth to erupt, at around 6 months of age for your first set of teeth, and between 6 and 8 years of age for your adult set.

Canines.
• Your four canines are the next type of teeth to develop. These are your sharpest teeth and are used for ripping and tearing food apart. Primary canines generally appear between 16 and 20 months of age with the upper canines coming in just ahead of the lower canines. In permanent teeth, the order is reversed. Lower canines erupt around age 9 with the uppers arriving between 11 and 12 years of age.

Premolars.
• Premolars, or bicuspids, are used for chewing and grinding food. You have four premolars on each side of your mouth, two on the upper and two on the lower jaw. The first premolars appear around age 10 and the second premolars arrive about a year later.

Molars.
• Primary molars are also used for chewing and grinding food. These appear between 12 and 15 months of age. These molars are replaced by the first and second permanent molars (four upper and four lower). The first molars erupt around 6 years of age while the second molars come in between 11 and 13 years of age.

Third molars.
• Third molars are commonly known as wisdom teeth. These are the last teeth to develop and do not typically erupt until age 18 to 20, and some people never develop third molars at all. For those who do, these molars may cause crowding and need to be removed.

Deglutition• Machanism of moving food into stomach• Facilitated by : saliva, mucus, mouth, pharynx, and
esophagus• 1.Voluntary stage: Food moves to oropharynx• 2.Pharyngeal stage: Involuntary passage of the
bolus from oropharynx to esophagus.• 3. Esophageal stage: Transit of food from esophagus
to stomach

Deglutination• Oral phasePrior to the following stages of the oral phase, the mandible depresses and the lips abduct to allow food or liquid to enter the oral cavity. Upon entering the oral cavity, the mandible elevates and the lips adduct to assist in oral containment of the food and liquid. The following stages describe the normal and necessary actions to form the bolus, which is defined as the state of the food in which it is ready to be swallowed.1) Moistening:Food is moistened by saliva from the salivary glands (parasympathetic).2) Mastication:Food is mechanically broken down by the action of the teeth controlled by the muscles of mastication. Buccinator (VII) helps to contain the food against the occlusal surfaces of the teeth. The bolus is ready for swallowing when it is held together by (largely mucus) saliva (VII—chorda tympani and IX—lesser ppetrosal), sensed by the lingual nerve of the tongue . Any food that is too dry to form a bolus will not be swallowed.

Deglutination• 3)Trough formation: A trough is then formed at the back of the
tongue by the intrinsic muscles (XII). he trough obliterates against the hard palate from front to back, forcing the bolus to the back of the tongue. The intrinsic muscles of the tongue (XII) contract to make a trough (a longitudinal concave fold) at the back of the tongue. The tongue is then elevated to the roof of the mouth (by the mylohyoid (mylohyoid nerve—Vc), genioglossus, styloglossus and hyoglossus (the rest XII)) such that the tongue slopes downwards posteriorly. The contraction of the genioglossus and styloglossus (both XII) also contributes to the formation of the central trough.
• 4) Movement of the bolus posteriorly: propelled posteriorly into the pharynx. In order for anterior to posterior transit of the bolus to occur, orbicularis oris contracts and adducts the lips to form a tight seal of the oral cavity. Next, the superior longitudinal muscle elevates the apex of the tongue to make contact with the hard palate and the bolus is propelled to the posterior portion of the oral cavity.

Deglutination• Once the bolus reaches the palatoglossal arch of the oropharynx, the
pharyngeal phase, which is reflex and involuntary, then begins. Receptors initiating this reflex are proprioceptive (afferent limb of reflex is IX and efferent limb is the pharyngeal plexus- IX and X). They are scattered over the base of the tongue, the palatoglossal and palatopharyngeal arches, the tonsillar fossa, uvula and posterior pharyngeal wall. Stimuli from the receptors of this phase then provoke the pharyngeal phase. In fact, it has been shown that the swallowing reflex can be initiated entirely by peripheral stimulation of the internal branch of the superior laryngeal nerve. This phase is voluntary and involves important cranial nerves: V (trigeminal), VII (facial) and XII (hypoglossal).

Deglutination• Pharyngeal phase: For the pharyngeal phase to work properly
all other egress from the pharynx must be occluded—this includes the nasopharynx and the larynx. When the pharyngeal phase begins, other activities such as chewing, breathing, coughing and vomiting are
concomitantly inhibited.• 5) Closure of the nasopharynx:
• The soft palate is tensed by tensor palati (Vc), and then elevated by levator palati (pharyngeal plexus—IX, X) to close the nasopharynx. There is also the simultaneous approximation of the walls of the pharynx to the posterior free border of the soft palate, which is carried out by the palatopharyngeus (pharyngeal plexus—IX, X) and the upper part of the superior constrictor (pharyngeal plexus—IX, X).

Deglutination• 6) The pharynx prepares to receive the bolus:The pharynx is pulled upwards and forwards by the suprahyoid and longitudinal pharyngeal muscles – stylopharyngeus (IX), salpingopharyngeus (pharyngeal plexus—IX, X) and palatopharyngeus (pharyngeal plexus—IX, X) to receive the bolus. The palatopharyngeal folds on each side of the pharynx are brought close together through the superior constrictor muscles, so that only a small bolus can pass.
7) Opening of the auditory tube
The actions of the levator palati (pharyngeal plexus—IX, X), tensor palati (Vc) and salpingopharyngeus (pharyngeal plexus—IX, X) in the closure of the nasopharynx and elevation of the pharynx opens the auditory tube, which equalises the pressure between the nasopharynx and the middle ear. This does not contribute to swallowing, but happens as a consequence of it.

Deglutination• 8) Closure of the oropharynx: The oropharynx is kept closed by
palatoglossus (pharyngeal plexus—IX, X), the intrinsic muscles of tongue (XII) and styloglossus (XII).
9) Laryngeal closure: A finite period of apnea must necessarily take place with each swallow. The aryepiglotticus (recurrent laryngeal nerve of vagus) contracts, causing the arytenoids to appose each other (closes the laryngeal aditus by bringing the aryepiglottic folds together), and draws the epiglottis down to bring its lower half into contact with arytenoids, thus closing the aditus. Additionally, the larynx is pulled up with the pharynx under the tongue by stylopharyngeus (IX), salpingopharyngeus (pharyngeal plexus—IX, X), palatopharyngeus (pharyngeal plexus—IX, X) and inferior constrictor (pharyngeal plexus—IX, X).This phase is passively controlled reflexively and involves cranial nerves V, X (vagus), XI (accessory) and XII (hypoglossal). The respiratory center of the medulla is directly inhibited by the swallowing center for the very brief time that it takes to swallow. This means that it is briefly impossible to breathe during this phase of swallowing and the moment where breathing is prevented is known as deglutition apnea.

Deglutination• 10) Hyoid elevation: The hyoid is elevated by digastric (V & VII) and
stylohyoid (VII), lifting the pharynx and larynx up even further.• 1) Bolus transits pharynx• The bolus moves down towards the esophagus by pharyngeal
peristalsis which takes place by sequential contraction of the superior, middle and inferior pharyngeal constrictor muscles (pharyngeal plexus—IX, X). The lower part of the inferior constrictor (cricopharyngeus) is normally closed and only opens for the advancing bolus. Gravity plays only a small part in the upright position—in fact, it is possible to swallow solid food even when standing on one’s head. The velocity through the pharynx depends on a number of factors such as viscosity and volume of the bolus. In one study, bolus velocity in healthy adults was measured to be approximately 30–40 cm/s.

Deglutination• Esophageal phase12) Esophageal peristalsisLike the pharyngeal phase of swallowing, the esophageal phase of swallowing is under involuntary neuromuscular control. However, propagation of the food bolus is significantly slower than in the pharynx. The bolus enters the esophagus and is propelled downwards first by striated muscle (recurrent laryngeal, X) then by the smooth muscle (X) at a rate of 3 – 5 cm/sec. The upper esophageal sphincter relaxes to let food pass, after which various striated constrictor muscles of the pharynx as well as peristalsis and relaxation of the lower esophageal sphincter sequentially push the bolus of food through the esophagus into the stomach.13) Relaxation phaseFinally the larynx and pharynx move down with the hyoid mostly by elastic recoil. Then the larynx and pharynx move down from the hyoid to their relaxed positions by elastic recoil. Swallowing therefore depends on coordinated interplay between many various muscles, and although the initial part of swallowing is under voluntary control, once the deglutition process is started, it is quite hard to stop it.

Esophagus
Consists of a muscular tube through which food
passes from the pharynx to the stomach. During
swallowing, food passes from the mouth through
the pharynx into the esophagus and travels via
peristalsis to the stomach. is continuous with the
laryngeal part of the pharynx at the level of the
C6 vertebra. The esophagus passes through posterior
mediastinum in thorax and enters abdomen through a
hole in the diaphragm at the level of the tenth thoracic
vertebrae (T10). It is usually about 10–50 cm long
depending on individual height (20-25 cm) . It is divided into cervical, thoracic and abdominal parts. Due to the inferior pharyngeal constrictor muscle, the entry to the esophagus opens only when swallowing or vomiting.

In human anatomy, the greater sac, also known as the general cavity (of the abdomen) or peritoneum of the peritoneal cavity proper, is the cavity in the abdomen that is inside the peritoneum but outside of the lesser sac.It is connected with the lesser sac via the omental foramen, also known as the Foramen of Winslow or Epiploic Foramen.

The peritoneum• The peritoneum, like the pericardium and pleura, is a serous membrane
that invests viscera. It is comprised of parietal and visceral peritoneum. There are many specializations of the peritoneum. All of the special structures that will be covered here are composed of two layers of peritoneum (much like the pulmonary ligament). They differ in location and what they connect. (Greek, peritonaion = stretch around)
• Mesenteries: result from the invagination of "intraperitoneal" organs into the sac. The mesenteries connect viscera to the posterior abdominal wall and are VERY important in that they conduct blood vessels and nerves. (There are no vessels within the peritoneal cavity, of course.) The mesentery of the colon is usually called the "mesocolon". For example, we speak of the "transverse mesocolon" and the "sigmoid mesocolon". (The other parts of the colon are not completely invested by peritoneum, and are therefore "retroperitoneal".) Also, often "the mesentery" refers specifically to the mesentery of the small intestine.

Mesenteries & Omenta• Mesenteries: result from the invagination of "intraperitoneal" organs
into the sac. The mesenteries connect viscera to the posterior abdominal wall and are VERY important in that they conduct blood vessels and nerves. (There are no vessels within the peritoneal cavity, of course.) The mesentery of the colon is usually called the "mesocolon". For example, we speak of the "transverse mesocolon" and the "sigmoid mesocolon". (The other parts of the colon are not completely invested by peritoneum, and are therefore "retroperitoneal".) Also, often "the mesentery" refers specifically to the mesentery of the small intestine. (Greek, mes = in the midst of, enteron = intestine)
• Omenta: generally refers to a free fold of peritoneum. This is exemplified by the greater omentum, which attaches to the stomach, droops far down into the abdominal cavity, and comes back up to attach to the transverse colon. The lesser omentum, on the other hand, is not really "free". It connects the stomach to the liver, and its membranous portion is called the hepatogastric ligament.

Retroperitoneal structures• Primarily retroperitoneal: • Urinary: adrenal glands, kidneys, ureter, bladder• Circulatory: aorta, inferior vena cava• Digestive: esophagus (part), rectum (part, lower third is
extraperitoneal).• Secondarily retroperitoneal: the head, neck, and body of the pancreas
(but not the tail, which is located in the splenorenal ligament), the duodenum, except for the proximal first segment, which is intraperitoneal, ascending and descending portions of the colon (but not the transverse colon or the cecum).

Stomach
1. Body of stomach* 2. Fundus* 3. Anterior wall* 4. Greater curvature* 5. Lesser curvature* 6. Cardia* 9. Pyloric sphincter* 10. Pyloric antrum* 11. Pyloric canal* 12. Angular notch* 13. Gastric canal* 14. Rugal folds
Rugae folds of mucus membrane


Fundus
PylorusCardiac

Stomach- Anatomy
• The stomach is a J shaped muscular, hollow, dilated part of the digestion system which functions as an important organ of the digestive tract. It lies in the epigastric, umbilical, and left hypochondriac regions of the abdomen. It is involved in the second phase of digestion, following mastication (chewing). The stomach lies between the esophagus and the duodenum. It is on the left upper part of the abdominal cavity. The top of the stomach lies against the diaphragm. Lying behind the stomach is the pancreas. The greater omentum hangs down from the greater curvature. It has cardiac orifice, and pyloric orifice. It has greater and lesser curvatures.

Stomach• The stomach is surrounded by parasympathetic (stimulant) and
orthosympathetic (inhibitor) plexuses (networks of blood vessels and nerves in the anterior gastric, posterior, superior and inferior, celiac and myenteric), which regulate both the secretions activity and the motor (motion) activity of its muscles.
• In adult humans, the stomach has a relaxed, near empty volume of about 45 ml and mucus membranes are folded to form rugae. Because it is a distensible organ, it normally expands to hold about one litre of food, but can hold as much as two to three litres. The stomach of a newborn human baby will only be able to retain about 30 ml.
• The lesser curvature of the stomach is supplied by the right gastric artery inferiorly, and the left gastric artery superiorly, which also supplies the cardiac region. The greater curvature is supplied by the right gastroepiploic artery inferiorly and the left gastroepiploic artery superiorly. The fundus of the stomach, and also the upper portion of the greater curvature, is supplied by the short gastric artery which arises from splenic artery.

At the bottom of gastric pits are openings of the gastric glands.Gastric glands:Chief (Zymogenic) glands: Pepsinogen, gastric lipaseParietal (oxyntic) cells:Hydrochloric acid, Intrensic factorMucus cells: MucusAbove three – gastric juice: 2-3 L/dayG cells: [Pyloric antrum] ---Gastrin
Limited to body of the stomach
What is endoscopy ?What is gastroscopy ?
Achylesia


Stomach-Secretion of gastric juice• Gastric acid facilitates digestion of proteins and the absorption of
calcium, iron, and vitamin B12. It also suppresses growth of bacteria, which can help prevent enteric infections and small intestinal bacterial overgrowth.
• Cephalic, Gastric, and Intestinal phases: • The cephalic phase is activated by the thought, taste, smell and site
of food, and swallowing. It is mediated mostly by cholinergic/vagal
mechanisms.• The gastric phase is due to the chemical effects of food and
distension of the stomach. Gastrin appears to be the major mediator since the response to food is largely inhibited by immunoneutralizing or blocking gastrin.
• The intestinal phase accounts for only a small proportion of the acid secretory response to a meal; its mediators remain controversial.

Physiology of stomach• Gastric juice: • The pH of gastric acid is 1.35 to 3.5. Causes denaturation of proteins This exposes the protein's peptide bonds.• Acidity being maintained by the proton pump H+/K+ ATPase. • The parietal cell releases bicarbonate into the blood stream in the process,
which causes a temporary rise of pH in the blood, known as alkaline tide.• HCl activates pepsinogen into the enzyme pepsin [ proteolysis]• Gastric acid production is regulated by both the autonomic nervous
system and several hormones.• The parasympathetic nervous system, via the vagus nerve, and the
hormone gastrin stimulate the parietal cell to produce gastric acid, both directly acting on parietal cells and indirectly, through the stimulation of the secretion of the hormone histamine from enterochromaffine-like cells (ECL).
• Vasoactive intestinal peptide, cholecystokinin, and secretin all inhibit production

Stimulation of Gastric Acid Secretion
• Endocrine : Gastrin is the digestive hormone that is secreted by the gastrin (G) cells which are located in the pyloric glands towards the distal end of the stomach. This hormone is released into the stomach cavity when the presence of protein is detected in the stomach contents. Due to the vigorous churning in the stomach, the gastrin is able to make contact and act upon the ECL [Entero chromaphin] cells, stimulating it to secrete histamine.
• Nervous : Acetylcholine released by the vagus nerve and enteric system acts on the ECL cells to secrete histamine, which in turn stimulates HCl production and secretion. The antral D-cells produce somatostatin. It is inhibitory of gastric and
• The antral D-cells produce somatostatin. It is inhibitory of gastric and pancreatic secretions.

HCl production• Parietal cells contain an extensive secretory network (called
canaliculi) from which the HCl is secreted by active transport into the stomach. The enzyme hydrogen potassium ATPase (H+/K+ ATPase) is unique to the parietal cells and transports the H+ against a concentration gradient of about 3 million to 1, which is the steepest ion gradient formed in the human body.
• Hydrogen ions are formed from the dissociation of water molecules. The enzyme carbonic anhydrase converts one molecule of carbon dioxide and one molecule of water indirectly into a bicarbonate ion (HCO3-) and a hydrogen ion (H+).
• The bicarbonate ion (HCO3-) is exchanged for a chloride ion (Cl-) on the basal side of the cell and the bicarbonate diffuses into the venous blood, leading to an alkaline tide.
• Potassium (K+) and chloride (Cl-) ions diffuse into the canaliculi.• Hydrogen ions are pumped out of the cell into the canaliculi in
exchange for potassium ions, via the H+/K+ ATPase.


Gastric juice• The production of gastric acid in the stomach is tightly regulated by
positive regulators and negative feedback mechanisms. Four types of cells are involved in this process: parietal cells, G cells, D cells and enterochromaffine-like cells. Besides this, the endings of the vagus nerve (CN X) and the intramural nervous plexus in the digestive tract influence the secretion significantly.
• Nerve endings in the stomach secrete two stimulatory neurotransmitters: acetylcholine and gastrin-releasing peptide. Their action is both direct on parietal cells and mediated through the secretion of gastrin from G cells and histamine from enterochromaffine-like cells. Gastrin acts on parietal cells directly and indirectly too, by stimulating the release of histamine.
• The release of histamine is the most important positive regulation mechanism of the secretion of gastric acid in the stomach. Its release is stimulated by gastrin and acetylcholine and inhibited by somatostatin.

Absorption from stomach

Neutralization• In the duodenum, gastric acid is neutralized by sodium bicarbonate. This also
blocks gastric enzymes that have their optima in the acid range of pH. The secretion of sodium bicarbonate from the pancreas is stimulated by secretin. This polypeptide hormone gets activated and secreted from so-called S cells in the mucosa of the duodenum and jejunum when the pH in duodenum falls below 4.5 to 5.0. The neutralization is described by the equation:
• HCl + NaHCO3 → NaCl + H2CO3• The carbonic acid rapidly equilibrates with carbon dioxide and water through
catalysis by carbonic anhydrase enzymes bound to the gut epithelial lining[4], leading to a net release of carbon dioxide gas within the lumen associated with neutralisation. In the absorptive upper intestine, such as the duodenum, both the dissolved carbon dioxide and carbonic acid will tend to equilibrate with the blood, leading to most of the gas produced on neutralisation being exhaled through the lungs.

Control of secretion and motility of stomach• Gastrin: The hormone gastrin causes an increase in the secretion of HCl
from the parietal cells, and pepsinogen from chief cells in the stomach. It also causes increased motility in the stomach. Gastrin is released by G-cells in the stomach in response to distenstion of the antrum, and digestive products(especially large quantities of incompletely digested proteins). It is inhibited by a pH normally less than 4 (high acid), as well as the hormone somatostatin.
• Cholecystokinin: Cholecystokinin (CCK) has most effect on the gall bladder, causing gall bladder contractions, but it also decreases gastric emptying and increases release of pancreatic juice which is alkaline and neutralizes the chyme.
• Secretin: n a different and rare manner, secretin, produced in the small intestine, has most effects on the pancreas, but will also diminish acid secretion in the stomach.
• Gastric Inhibitory peptide: Gastric inhibitory peptide (GIP) decreases both gastric acid release and motility.
• Enteroglucon: enteroglucagon decreases both gastric acid and motility

Digestions in stomach• :• Pepsinogen is the main gastric enzyme. It is produced by the
stomach cells called "chief cells" in its inactive form pepsinogen, which is a zymogen. Pepsinogen is then activated by the stomach acid into its active form, pepsin. Pepsin breaks down the protein in the food into smaller particles, such as peptide fragments and amino acids. Protein digestion, therefore, first starts in the stomach, unlike carbohydrate and lipids, which start their digestion in the mouth.
• Hydrochloric acid (HCl): This is in essence positively charged hydrogen atoms (H), or in lay-terms stomach acid, and is produced by the cells of the stomach called parietal cells. HCl mainly functions to denature the proteins ingested, to destroy any bacteria or virus that remains in the food, and also to activate pepsinogen into pepsin.

Digestions in stomach• .• Intrinsic factor (IF): Intrinsic factor is produced by the
parietal cells of the stomach. Vitamin B12 (Vit. B12) is an important vitamin that requires assistance for absorption in terminal ileum. Initially in the saliva, haptocorrin secreted by salivary glands binds Vit. B, creating a Vit B12-Haptocorrin complex. The purpose of this complex is to protect Vitamin B12 from hydrochloric acid produced in the stomach. Once the stomach content exits the stomach into the duodenum, haptocorrin is cleaved with pancreatic enzymes, releasing the intact vitamin B12. Intrinsic factor (IF) produced by the parietal cells then binds Vitamin B12, creating a Vit. B12-IF complex. This complex is then absorbed at the terminal portion of the ileum.

Digestions in stomach
• Mucin: The stomach has a priority to destroy the bacteria and viruses using its highly acidic environment but also has a duty to protect its own lining from its acid. The way that the stomach achieves this is by secreting mucin and bicarbonate via its mucous cells, and also by having a rapid cell turn-over.
• Gastrin: This is an important hormone produced by the "G cells" of the stomach. G cells produce gastrin in response to stomach stretching occurring after food enters it, and also after stomach exposure to protein. Gastrin is an endocrine hormone and therefore enters the bloodstream and eventually returns to the stomach where it stimulates parietal cells to produce hydrochloric acid (HCl) and Intrinsic factor (IF).

Pancreas

1. Bile ducts: 2. Intrahepatic bile ducts, 3. Left and right hepatic ducts, 4. Common hepatic duct, 5. Cystic duct,6.Common bile duct, 7. Ampulla of Vater, 8. Major duodenal papilla 9. Gallbladder, 10-11. Right and left lobes of liver. 12. Spleen. 13. Esophagus. 14. Stomach. Small intestine: 15. Duodenum, 16. Jejunum 17. Pancreas: 18: Accessory pancreatic duct, 19: Pancreatic duct. 20-21: Right and left kidneys (silhouette).

Pancreas

Pancreas

• Pancreas

Pancreas anatomy• The pancreas lies in the epigastrium and left hypochondrium areas of
the abdomen at 2nd lumbar vertebral level. Pancreas is a 12-15 – cm long J-shaped (like a hockey stick), soft, lobulated, retroperitoneal organ. I00-160 gram in weight. It lies transversely, although a bit obliquely, on the posterior abdominal wall behind the stomach, across the lumbar (L1-2) spine. The head fits into the loop of duodenum. The neck is the constricted part between the head and the body. The body lies behind the stomach. The tail is the left end of the pancreas. It lies in contact with the spleen.
Main duct (Wirsung) runs the entire length of pancreas. Joins Common Bile duct at the ampulla of Vater. It is 2 – 4 mm in diameter, has 20 secondary branches.
Lesser duct (Santorini) drains superior portion of head and empties separately into 2nd portion of duodenum.

Pancreas anatomy• Blood supply: Variety of major arterial sources (celiac, Superior
mesenteric , and splenic arteries)• Celiac Common Hepatic Artery Gastroduodenal Artery
Superior pancreaticoduodenal artery which divides into anterior and posterior branches
• SMA(Superior mesenteric artery) Inferior pancreaticoduodenal artery which divides into anterior and posterior branches
• Splenic artery run on the superior border of pancreas going to spleen and supplies upper portions of pancreas.
• Venous drainage: Follows arterial supply;
Anterior and posterior arcades drain head and the body. Splenic vein drains the body and tail. Major drainage areas are Suprapancreatic Portal Vein, Retropancreatic Portal Vein, Splenic vein, Infrapancreatic superior mesenteric vein and ultimately, into portal vein.


Arterial supply to pancreas

Venous drainage from pancreas

Anatomy of pancreas• . The body and neck of the pancreas drain into splenic vein; the head
drains into the superior mesenteric and portal veins. Lymph is drained via the splenic, celiac and superior mesenteric lymph node. Innervation of Pancreas: Sympathetic fibers from the splanchnic nerves. Parasympathetic fibers from the vagus. Both give rise to intrapancreatic periacinar plexuses. Parasympathetic fibers stimulate both exocrine and endocrine secretion. Sympathetic fibers have a predominantly inhibitory effect.• Exocrine pancreas 85% of the volume of the gland• Extracellular matrix – 10%• Blood vessels and ducts - 4%• Endocrine pancreas – 1%

Pancreas– Acinus →small intercalated ducts → interlobular duct →
pancreatic duct→duodenum. – Acinar cells which secrete primarily digestive enzymes– Centroacinar or ductal cells which secrete fluids and electrolytes
• Hormones produced by 5 classes of islet cells include:– α-cells → Glucagon- a 29 amino acid molecule which targets the
liver to breakdown glycogen and release glucose.– β cells → Insulin- a 51 amino acid molecule which targets the liver
and most body cells except the brain to take up glucose.– Delta cells → Somatostatin ↓ release of insulin & glucagon.– “F” cells → Pancreatic polypeptide ↓ gall bladder contraction.– “G” cells → Gastrin ↑ acid secretion, gastric motility and stomach emptying.

Insulin
• Insulin is synthesized by the beta cells of the pancreas
• Insulin and C peptide are packaged into secretory granules and released together into the cytoplasm
• 95% belong to reserve pool and 5% stored in readily releasable pool
• Thus small amount of insulin is released under maximally stimulatory conditions

Physiology – Exocrine Pancreas• Secretion of water and electrolytes originates in the centroacinar and
intercalated duct cells. Pancreatic enzymes originate in the acinar cells. Final product is a colorless, odorless, and isosmotic alkaline fluid that contains digestive enzymes (amylase, lipase, and trypsinogen).
• 500 to 800 ml pancreatic fluid secreted per day. Alkaline pH results from secreted bicarbonate which serves to neutralize gastric acid and regulate the pH of the intestine. High pH neutralizes acidic gastric chyme and provides optimum pH for the enzymatic digestion
• Enzymes digest carbohydrates, proteins, and fats.• Fluid (pH from 7.6 to 9.0) acts as a vehicle to carry inactive proteolytic
enzymes to the duodenal lumen. Bicarbonate is formed from carbonic acid by the enzyme carbonic anhydrase.
• Major stimulants: are Secretin, Cholecystokinin, Gastrin, Acetylcholine.• Major inhibitors: Atropine, Somatostatin, Pancreatic polypeptide and
Glucagon

Exocrine--Enzyme secretion• Four classes of enzymes are secreted• Proteolytic--Peptidases• Lipolytic--lipases• Carohydrate-hydrolyzing--amylases• Nucleolytic--nucleases• Proteolytic enzymes activated when they enter duodenum• Trypsin secreted as trypsinogen(Trypsin inhibitor in pancreas)• Chymotrypsin secreted as chymotrypsinogen• Both zymogens require enterokinases secreted by mucosa of
proximal intestine for activation• Nucleolytic enzymes hydrolyze phosphodiseter bonds that
unite nucleotides in nucleic acid• Ductal cells produce high quantity of bicarbonate into the
pancreatic juice.

Exocrine--Enzyme secretion• Enterokinase secreted by the small intestine activates trypsinogen
into trypsin(active), small amount of trypsin formed in intestine can itself activates trypsinogen into trypsin.
• Trypsin activates conversion of Chymotrypsinogen into chymotrypsin and conversion of procarboxypeptidase into carboxy peptidase• Sodium bicarbonhate in pancreatic juice neutralizes the acid pH of
chyme coming from stomach and entering duodenum because alkaline pH is necessary for pancreatic enzymes digest food in the small intestine.
• Pancreatic alpha amylase hydrolyses starch, glycogen and most other complex carbohydrates into disaccharides
• Pancreatic lipases consists of lipase, cholesterol lipase, and phospholipase hydrolyzes water soluble esters and lipid soluble esters are hydrolyzed with the help of bile salts present in bile juice.

Pancreatic exocrine function• Trypsin acts on native proteins and partly digested proteins in the
stomach, like metaproteins, proteases, peptones and polypeptides and converts them into lower peptides containing tripeptides or dipeptides.
• Chymotrypsin also converts proteins into tri and dipeptides.• Carboxy peptidases splits amino acids having free carboxyl groups
from proteins.• Nucleotidases digest nucleoproteins• Phases of pancreatic secretion:1. Cephalic phase: Sight, smell or thought of food induce secretion Enzyme secretion enhanced due to stimulation of enteric neurones which release acetylchoiline and Vagal stimulation causes secretion of enzymes and bicarbonate. Bicarbonate secretion is stimulated through enteric neurones through noradenaline release.*** In this phase very little pancreatic secretion enters duodenum.

Pancreatic exocrine function• Gastric phase: When stomach distends due to food content
pancreatic juice secretion increases. Vago-vagal reflex-acetylcholine is the transmitter. Protein breakdown products in the stomach stimulates G cells in the stomach release gastrin hormone into the blood which causes low volume, high enzymes juice secretion from the pancreas.
• Intestinal phase: It occurs after the Chyme entering the small intestine. Stimulated by Secretin(by ‘S’ cells produce prosecretin which is converted into active secretin by acidic chyme, this hormone enters blood and acts on pancreas to cause pancreatic juice) and ‘I’ cells produce cholycystokinin hormones (due to presence of proteases and long chain fatty acids in the upper small intestine, goes into blood then to pancreas to increase pancreatic exocrine secretion)secreted by duodenum and jejunum mucosal cells.

Regulation of Pancreatic Secretion
• Two patterns of secretion– Basal secretion • Bursts of increased bicarb and enzyme secretion that
last 10 to 15 minutes
– Post prandial stage• Divided into cephalic phase, gastric phase, intestinal
phase

Post Prandial stage
• Cephalic phase– Occurs in response to the sight or taste of food– Mediated by the vagus– Results in the production of enzymes and
bicarbonate

Post Prandial stage
• Gastric phase– Occurs partially in response to distension of
stomach which stimulates gastrin release by vagal reflex
– Gastrin and neural reflex stimulate acid secretion by gastric parietal cells and pancreatic enzyme secretion

Post Prandial stage
• Intestinal phase– Initiated in response to acid entering the duodenum – Most important phase– When pH falls <4.5 secretin is released from the intestine– Secretin inturn stimulates the pancreatic ducts to secrete
bicarbonate– Presence of fatty acid, oligopeptides and amino acids
results in release of CCK which increase secretion of pancreatic enzymes

Exocrine secretion of pancreas• Proteases: essential for protein digestion, secreted as
proenzymes and require activation for proteolytic activity.• Duodenal enzyme, enterokinase, converts trypsinogen to
trypsin• Trypsin, in turn, activates chymotrypsin, elastase,
carboxypeptidase, and phospholipase.

• Ultimate result of all these actions is food digestion and absorption
• Inhibitory hormones– Pancreatic polypeptide– Peptide YY
• Vagal nerve stimulation induces bicarbonate secretion – activity mediated through VIP hormones which is present in vagal nerve endings and throughout the entire GIT

Exocrine secretion of pancreas• Secretin - released from the duodenal mucosa in response to a
duodenal luminal pH < 3.• Enzyme Secretion: amylases, lipases, and proteases• Major stimulants: Cholecystokinin, Acetylcholine, Secretin, VIPSynthesized in the endoplasmic reticulum of the acinar cells and are packaged in the zymogen granules. Released from the acinar cells into the lumen of the acinus and then transported into the duodenal lumen, where the enzymes are activated.• Amylase: only digestive enzyme secreted by the pancreas in an active
form. Functions optimally at a pH of 7, hydrolyzes starch and glycogen to glucose, maltose, maltotriose, and dextrins
• Lipase: function optimally at a pH of 7 to 9, emulsify and hydrolyze fat in the presence of bile salts.
Related Documents