dr. Indriati Dwi Rahayu Dept. Of Anatomy-Histology University of Brawijaya Malang BONE BONE DEVELOMENT DEVELOMENT

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

dr. Indriati Dwi Rahayu
Dept. Of Anatomy-Histology
University of Brawijaya Malang
BONE BONE DEVELOMENTDEVELOMENT

FUNCTION & COMPOSITION
BONE CLASSIFICATION
OSTEOGENESIS
REGULATION

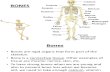
FUNCTION5 MAIN FUNCTIONS:
1. Support (give body shape and structure)
2. Protection (protect internal organs)
3. Movement (joints allow for motion)
4. Mineral storage (calcium, phosphorus)
5. Blood cell production (marrow)
FUNCTION & COMPOSITION

COMPOSITION
• water (25%)
• organic constituents (25%): incl.
osteoid (the carbon containing part of the matrix)
bone cells
• inorganic constituents, mainly calcium phosphate
(~ 50%).

A Chemical Analysis of Bone

COMPONENT Matrix Intercellular : acidophilic
* Fibers : type I collagen; in overlapping pattern
* Ground substance
ORGANIC : proteoglycan, glycoprotein, keratan sulfates
ANORGANIC : * Calcium * Phosphate
Ca-phosphate amorph (hydroxyapatite)
- bicarbonate, sitrat, Mg, K, Na
CELLS

FUNCTION & COMPOSITION
BONE CLASSIFICATION
OSTEOGENESIS
REGULATION

Based on textures:• Spongious bone (trabecular bone, cancellous bone, spongy)• Compact bone (dense bone, cortical bone)
Based on matrix arrangement :• Woven bone (primary bone tissue): • Lamellar bone (secondary bone tissue):
Based on maturities :• Immature bone (primary bone tissue): Immature bone is woven
bone. • Mature bone (secondary bone tissue). Mature bone
characteristically is lamellar bone.
Based on histogenesis • Intramembranous bone (mesenchymal bone)• Intracartilaginous bone (cartilage bone, endochondral bone)

Based on textures:Sponge bone (trabecular bone,
cancellous bone)
Can be primary on secondary
Compact bone (dense bone, cortical bone)
Must be secondary

Trabecular ; lamellar

COMPACT bone
• always as secondary bone
• Trabecula <<

DISTRIBUTION :
• Long Bones :
[epiphysis] spongious, covered by a
thin layer of compact bone
[diaphysis] almost totally composed
of compact bone, with a small
component of spongy bone on its
inner surface around the bone
marrow cavity.

• Flat bone :
two layers of compact bone
called plates (tables),
separated by a layer of spongy
bone called the diploe.
• irregular bone:
a core of spongy bone
completely surrounded by
compact bone

FUNCTION & COMPOSITION
BONE CLASSIFICATION
OSTEOGENESIS
REGULATION

HISTOGENESISHISTOGENESISHISTOGENESISHISTOGENESIS
Tulang PRIMER(Wovenbone)
Tulang PRIMER(Wovenbone)
Tulang SEKUNDER(Lamellar bone)
Tulang SEKUNDER(Lamellar bone)
PenulanganEndochondralPenulangan
EndochondralPenulangan
IntramembranousPenulangan
Intramembranous
INTRAMEMBRANOUS
Ossification
ENDOCHONDRAL
Ossification

INTRAMEMBRANOUS OSSIFICATION
They formed directly into bone ( de novo)
the Skull bones ( flat bones) were NEVER cartilage!
the source of most of the flat bones
also contributes to the growth of short bones and the
thickening of long bones.
The ossification centers of a bone grow radially and
finally fuse together, replacing the original connective tissue

Primary ossification center (starting point for ossification)
1. condensation of mesenchymal cells differentiate
osteoblast
2. osteoblast produce bone matrix and calcification
follows (Osteoid) encapsulation of some osteoblasts
osteocytes
3. islands of developing bone = TRABECULAE
4. Walls delineate elongated cavities containing capillaries,
bone marrow cells, and undifferentiated cells
5. Several such groups arise almost simultaneously at the
ossification center, so that the fusion of the walls gives the
bone a spongy structure.


Blue arrow - mesenchymal cells
Green arrow - osteocytes
Red arrow - Bone from Intramembraneous Oss. = trabeculae

ENDOCHONDRAL OSSIFICATION
takes place within a piece of hyaline cartilage whose shape resembles a model of the bone to be formed
Bone matrix deposition in the cartilage matrix
• Epiphysis remains cartilaginous and continues to grow Secondary ossification center (Forms spongy bone)
• Compact bone deposited in diaphysis by primary ossification center
• Spongy bone deposited in epiphysis by secondary ossification center
• responsible for the formation of short and long bones

1. Hyalin Cartilage Model
2. Periostal bone collar
- capillary invasion to the
perichondrium
- mesenchyme
osteoprogenitor
osteoblast secrete
matrix spiculae fusi
periostal bone collar
(Mx : intramembranous)

3. Chondrocyte near the collar PROLIFERATE isogenous groups parallel to the bone’s long axis.
Chondrocyte HIPERTROPHY (large, rounded) not separated by matrix superlacuna
CALCIFICATION of cartilage matrix between the superlacuna difusion failed hypertropic chondrocytes die
Formation of the primary marrow cavity (by chondroclast)

4. Periostal Bud penetrate the
primary marrow cavity, bring
the cells on the cartilage
matrix surface
5. OSSIFICATION : osteoid
deposition mineralization.
primary bone.
44
55
the calcified cartilage appears basophilic,
and the primary bone is eosinophilic

6. Secondary ossification center in epiphyses
Zona2 pd Epiphyseal cartilage + METAPHYSIS Epiphyseal plate
66



OSSIFICATION CENTERS
- In long bones :
* primer : mid
* sekunder : epi
enlarge seperated by epiphyseal plate
* tertiary ossification center : form the bony tubercles,
ridges for attachment of muscles, ligament

• SECONDARY BONE TISSUE (Mature = lamellar)
* by REMODELLING
* Feat : - collagen fibers positioned parallel
eachother
Osteon/Sistem Havers


REMODELLING• osteoclast erode the primary bone matrix cavities• Invasion the cavities by blood vessel, nerve, & lymphvessel• Deposit osteogenic cells (from perivascular) on the cavity wall• Differentiated to osteoblast + osteocyte• deposit secondary bone in concentric layers lamellae oldest: farthes from the vessels


Pertumbuhan Tulang
- till early adulthood, continously
with remodelling
- DIRECTION :
# growth in LENGTH:
By chondrocyte division in
epiphyseal zone
# Growth in girth
• by proliferation &
differentiation of
osteoprogenitor cells in the
inner layer of periosteum
• Bone deposition on the
outer surface of bone


BONE REPAIR
- Fractures tear vessel hemorrhage clot formation.
- macrophage remove the clot, fibroblast fill the space with fibrous connective tissue
- certain cells differentiate into chondrocyte
CALLUS (soft)
(islands of fibro cartilage & hyaline cartilage as model of ossification)
callus replaced by primar bone(bony callus) remodelled secondary bone



FUNCTION & COMPOSITION
BONE CLASSIFICATION
OSTEOGENESIS
REGULATION & Clinical Correlation

Hormonal Control involves the interplay among the actions of : PTH, increases blood calcium levels calcitonin, decreases blood calcium levels vitamin D, helps Calcium absorbtion in intestine &
decreases renal Calcium excretion Other hormones (ex: cortisol, growth hormone,
thyroid hormone, and the sex hormones. Growth hormone and thyroxine increase bone mass)


Osteoporosis
Cx : bone formation <<, bone resorbtion >>
decrease bone mass (ratio mineral : matrix normal)
Calcium Deficiency poor calcification of bone matrix
# chronic in children: Rickets (bone deformity)
# chronic in adult : Osteomalacia (decrease bone mass ,
ratio mineral : matrix : sub normal)
CLINICAL CORRELATION



Dwarfism
• Achondroplastic– long bones stop growing in
childhood• normal torso, short limbs
– spontaneous mutation during DNA replication
– failure of cartilage growth
• Pituitary – lack of growth hormone– normal proportions with
short stature

ENJOY YOUR TIME TO LEARN….
EXAM IS JUST ANOTHER DAY IN THE FUTURE…
DON’T WORRY…..BE HAPPY…
Related Documents