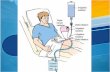
Benign Prostatic Hyperplasia Jay Lee, MD, FRCSC Clinical Associate Professor University of Calgary

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Benign Prostatic Hyperplasia
Jay Lee, MD, FRCSC
Clinical Associate Professor
University of Calgary

Copyright © 2017 by Sea Courses Inc.
All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or
by any means – graphic, electronic, or mechanical, including photocopying, recording, or information storage and retrieval systems without prior written permission of
Sea Courses Inc. except where permitted by law.
Sea Courses is not responsible for any speaker or participant’s statements, materials, acts or omissions.

• At the end of this program, participants will be able to:– Define terminology related to lower urinary tract
symptoms (LUTS)
– Recognize and diagnose LUTS secondary to benign prostatic hyperplasia (BPH)
– Predict progression in terms of symptoms, acute urinary retention and need for surgery
– Determine the appropriate care path for each patient

Definition of Terms
BPH – Benign Prostatic
Hyperplasia
BOO – Bladder Outlet Obstruction
LUTS – Lower Urinary Tract Symptoms
Hypertrophied detrusor muscle
Obstructed urinary flow

Natural History of BPH: Symptoms Worsen
Kirby RS et al. Benign prostatic hyperplasia. Health Press, 1995.
14
30%
55%
15%
Remain Stable ImproveWorsen

Richard F et al., Prog Urol 2001; 11(2):250-63.
0
10
20
30
40
50
60
7%9%
11%
27%
50-59 years
9%
15%17%
21%
60-69 years
30%
35%33%
48%
70-79 years
0 1-7 8-19 20-35 pointsIPSS
2,372 French menIIEF

Diabetes 20.2% 3.2%
Hypertension 32.0% 13.6%
Pelvic surgery 18.8% 2.4%
LUTS 72.2% 37.7%
Smoker 29.6% 34.6%
Regular alcohol 37.5% 42.4%
ED(n=853)
No ED(n=3581)
Braun M et al., Int J Impot Res 2000; 12:305-311

Risk Factors for BPH Progression
• Age 50 years or older
• Enlarged prostate (≥ 30 mL)
– PSA ≥ 1.4 ng/mL as a marker for prostate volume
• Moderate-to-severe urinary symptoms (AUA-SI score > 7)
McConnell JD et al. N Engl J Med. 2003;349:23872398. Roehrborn CG et al. Urology.1999;53:473480.

Clinical Outcomes in BPH vs. Other Diseases
Condition Clinical Outcome Incidence (%)*
Osteoporosis Vertebral fracture 1.5Hip fracture 18
Atherosclerosis Fatal/nonfatal MI 2.1
Superficial bladder cancer Recurrence 30–88
Kidney stones Recurrence 2–47
BPH AUR 7Surgical Intervention 10
*Annual incidence or rate per person-years
Adapted from Roehrborn CG et al. Urology 2000;56:9-18; McConnell JD et al. N Engl J Med 1998; 338:557-563.

BPH – Key Components of Diagnosis: History
General medical history– LUTS/severity/bother; hematuria, UTI, retention, incontinence– Review of nervous system (evidence of neurogenic bladder) – MS, spinal cord
injury…– DM– Family history of prostate cancer
Past surgical history– APR, spinal surgery– Urethral Surgery/instrumentation
Medications– Note use of diuretics, antihypertensives, psychotropics, anticholinergics, hormones,
some OTC cold medications– Current BPH treatment – Smoking, caffeine, EtOH intake

BPH / LUTS Symptoms Obstructive Symptoms
Hesitancy
Weak stream
Straining to pass urine
Prolonged micturition
Post-void dribbling
Sensation of incomplete bladder emptying
Acute or chronic urinary retention
Overflow incontinence
Irritative Symptoms
Frequency
Urgency
Nocturia
Urge incontinence
Dysuria
Hematuria
*Now: Storage and voiding

BPH – Key Components of Diagnosis: Focused Physical Exam
Digital rectal examination (DRE)
– Assess prostate size, consistency, symmetry, presence of nodules or indurations
– Size does not predict severity of symptoms or obstruction
Also
– Check for suprapubic fullness (i.e., retention)
– Neurologic Exam

BPH – Key Components of Diagnosis
– Urinalysis• Abnormalities could suggest other problems – hematuria, UTI,
proteinuria
– Discuss PSA measurement if:• Age > 50, life expectancy > 10 years (diagnosis of prostate cancer
would change management)
• Family history of prostate cancer (age 40)
• African American (age 40)
*** Serum creatinine • High creatinine necessitates imaging of upper tract

A Word On PSA
• DO NOT DO PSA IF:
– ACUTE RETENTION
– INFECTION
– LIFE EXPECTANCY < 10 YEARS

BPH - Complications
• If untreated, can progress to serious complications including:
– Acute Urinary Retention (AUR)– Bladder decompensation– Upper urinary tract compromise – obstructive
uropathy & renal failure– Recurrent UTI– Bleeding– Stones– Bladder diverticuli– Decreased quality of life
Anderson JB et al. Eur Urol 2001;39:390-399.

Treatment Options - Overview
• Watchful Waiting
• Lifestyle Modifications – ↓hs fluids, limit alcohol/caffeine, timing of diuretic use…
• Medical Therapy - -blockers, 5--reductase inhibitors….
• Surgery – TURP, minimally invasive strategies

- Blockers

Alpha Blockers: General• Established Mechanism of Action
– Blockade of sympathetic activity
– Relaxation of prostatic and bladder-neck smooth muscle
• Effects– Have rapid onset of action and are well tolerated– Improve urinary flow and reduce LUTS
• Flow rates ↑ by ~ 25%• Sx Scores ↓ by 20-40% (4-6 points)
– Do not affect prostate enlargement or PSA
*** Little effect on disease progression wrt rate of AUR/surgery
Adapted from Kirby RS. Eur Urol 1999;36(suppl 1):48-53.

Common -Blocker Side Effects
• Orthostatic hypotension
• Dizziness (central versus vascular phenomenon)
• Nasal Congestion
• Fatigue
• Head-ache
• GI Upset
• RETROGRADE EJACULATION

1A Blockers – Long-acting, Subtype Selective
• Tamsulosin (Flomax CR) - 0.4 mg – 0.8mg/day
• Alfuzosin (Xatral) – 10mg po qd
• Silodosin (Rapaflo) – 8 mg po qd
– Exhibits greater uro-selectivity
• Selective antagonist of 1A-receptor subtype
• Subtype makes up ~70% of all 1-receptors in the prostate
– Once daily dosing
– No antihypertensive properties therefore no dose adjustments are necessary

5--Reductase
Inhibitors

dutasteride
dutasteride
finasteride
Prostate Size Reduced
DHTTestosterone
5-α Reductase Inhibitors (5ARI’s)
Steers WD. Urology. 2001;58(suppl 6A):17–24.Bartsch G et al. Eur Urol. 2000;37:367380.
x x
x
5-AR = 5-alpha reductase; DHT = dihydrotestosterone
Type I 5AR
Type II 5AR

5--Reductase Inhibitors
Mechanism of action
– Regulates conversion of Tt to DHT
– ↓ Prostatic levels of DHT by 80-90%
– Slows rate of prostate enlargement
Effects (may take 6-9mo)
– Decreases prostate volume by ~ 20%
– Reduces the risk of AUR and the need for BPH-related surgery
– not appropriate for men with LUTS who do not have prostatic enlargement
*** Will lower PSA by 50% over 12 months

Indications for 5- Reductase Inhibitors
• Monotherapy or Combination therapy with
-blocker
• Large prostate - men with larger prostates
(> 40 g) respond more favorably(Response can be predicted by PSA - poor response if < 1.3 ng/ml)
• Hematuria 2° BPH

5ARI Efficacy: Summary• Data from robust randomized placebo-controlled studies has
confirmed that both dutasteride and finasteride have a significant
effect in men with enlarged prostates:
✓ Reducing symptoms (30% from baseline) and impact of BPH
✓ Reducing prostate size (20-30%)
✓ Improving urinary stream (1-2 ml/sec)
✓ Reducing risk of urinary retention and surgery (>50%)
• Improvements are generally seen after ~6 months or more and
continue to build beyond 2 years of therapy
McConnell JD et al. N Engl J Med 1998;338:557–63 Roehrborn CG et al. Urology 2002; 60: 434-441

PSA Testing in Patients on Medical Therapy for LUTS/BPH
• α-blocker therapy has no effect on PSA
• 5α-Reductase Inhibitors lower PSA by 40-50% in 6 months
– Critical to have baseline PSA
• Refer for biopsy if elevated
– Repeat PSA after 6 months treatment
• If does not fall, indicates non-compliance or cancer risk
– Double PSA value to determine cancer risk
– Progressively rising PSA on treatment is indication for referral and
biopsy

Combination TherapyModerate-Severe Symptoms and Enlarged Prostate
✓Rapid onset✓ Improvements in
symptoms and stream
✓Further improvement in symptoms and stream
✓Long-lasting symptom benefit
✓Prevent disease progression
✓Reduce risk of AUR and surgery
-blocker Combination 5-ARI

COMBINATION THERAPY

McConnell JD, et al. N Engl J Med 2003;349:2387-98.
Combination therapy is better than monotherapy at reducing risk of clinical progression
Cu
mu
lati
ve in
cid
ence
of
pro
gres
sio
n (
%)
Years

Roehrborn CG, et al. Eur Urol. 2010 Jan;57(1):123-31.
Combination therapy is better than monotherapy at improving symptoms
Month
Ad
just
ed m
ean
ch
ang
e in
IPS
S

What to do with the α-Blocker?
• With combination therapy, removal of the α-blocker after 6-9 months of therapy is reasonable1,4
• Majority of men will continue to enjoy good symptom control2,3,4
• More severe baseline symptoms may require that the α-blocker be continued longer-term2
1) Nickel CJ et al. Can J Urol; 2005;12(3);2677-2683 2) J Barkin et al. European Urology (2003): 44; 461-466. 3) Baldwin KC et al: Urology 58(2), 2001 3) Nickel et al. CUAJ 2008;2(1):16-21.

• Tadalafil 5mg currently indicated for men with BPH-related LUTS
• Recent clinical studies investigating PDE5-inhibitors in BPH

McVary KT, et al. J Urol. 2007 Apr;177(4):1401-7.
Mea
n c
han
ge
in
sym
pto
m s
core
WeeksEfficacy of Tadalafil
WeeksM
ean
ch
ang
e in
sym
pto
m s
core
Mea
n c
han
ge
in s
ymp
tom
sco
re
Tadalafil 20 mg
Efficacy of Vardenafil
Weeks
Efficacy of Sildenafil

-9
-8
-7
-6
-5
-4
-3
-2
-1
0
PLA Run InWeek - 4
BaselineWeek 0 Week 4 Week 8 Week 12
Me
an
Ch
an
ge
in
To
tal IP
SS
Sc
ore
fr
om
Bas
eli
ne
to
En
dp
oin
t
Placebo
Tad 2.5
Tad 5.0
Tad 10.0
Tad 20
Tadalafil Dosing For BPH
Compared to placebo (Ancova analysis)
* Tadalafil 2.5mg p<.05 at week 4, and Tadalafil 5, 10, and 20 mg p<.01 for Weeks 4, 8, and 12 compared to placebo
Clinical meaningfulimprovement

*
*P < .05 versus placebo-7
-6
-5
-4
-3
-2
-1
0
Baseline Week 4 Week 8 Week 12
Placebo
Tadalafil
Tamsulosin
* *
***
LS
Me
an
Ch
an
ge
fro
m B
ase
lin
e
Study LVID
Tadalafil vs Placebo and Tamusolsin vs Placebo

• Some plant extracts have shown some efficacy in small clinical trials
• Serenoa repens (saw palmetto berry extract)
• Pygeum africanum (African plum)

Bent S, et al. N Engl J Med 2006;354:557-66.
No statistically significant difference between treatment with saw palmetto and placebo
Mea
n c
han
ge
in
sym
pto
m s
core
Month

Absolute Indications for Surgery
• Refractory retention
• Renal failure – obstructive uropathy
• Recurrent infections
• Recurrent Bleeding
• Stones

BPH - When to Refer
• Referral warranted in patients with:
– IPSS > 20 (severe)
– Urinary retention
– Recurrent UTI
– Hematuria
– Bladder stones
– Renal insufficiency
– Failure of medical treatment
– Abnormal DRE or Elevated PSA

Key Messages
• BPH is very common in men
• BPH is progressive
• Multiple medications are available for treatment
• Some men will require intervention past medical therapy
Related Documents