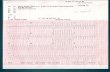
APPROACH TO A PATIENT WITH NARROW QRS COMPLEX TACHYCARDIA 24-08- 2011 .Nagula Praveen

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

APPROACH TO A PATIENT
WITH NARROW
QRS COMPLEX
TACHYCARDIA
24-08-2011Dr.Nagula Praveen

My first CASE experience …
1.A 35 yr old female came to medicine OP with complaints of pounding sensation in the heart,dizziness.lightheadedness..the episode lasted for few minutes relieved spontaneously without any efforts..ending up in the patient passing urine after the absence of palpitations…on examination her heart heart was normal…there are no neck abnormalities…no other features..her BP is normal ..her thyroid status is normal ..What is the diagnosis was asked ?

SUPRAVENTRICULARTACHYCARDIA

CASE scenario
A 28 yr old woman has rapid palpitations accompanied by chest pain and dizziness while playing her cello.she is brought to an ED.she has a faint regular pulse of 180 bpm.her blood pressure is 100/70 mm Hg.cardiovascular signs reveals no signs of heart failure.an ECG show a regular tachycardia with a narrow QRS complex and no apparent Pwaves ..how should her case be managed?

Clinically
Patient complains of recurrent palpitations,chest fullness,light headedness,presyncope,syncope.
Ppt factors may be present – exercise,caffeine,cigarette smoking,alcohol.
h/o heart disease,pulmonary disease,post AFablation. CAUTION :H/O DIGOXIN USE On examination– neck pounding –cannon waves “frog’s sign “
– practically pathognomic of AVNRT. HR is a non specific feature in differentiating SVTs.

STEP wise
Look for QRS duration. QRS complex regular/irregular. Then look for presence of p waves. P waves morphology P waves and QRS relationship 1:1 AV block present. QRS alternation Termination initiation of tachycardia. Effect of BBB on tachycardia cycle length.

Decision tree schema by BAR and colleagues STEP 1 –FOR ANY FAILURE OF AV CONDUCTION –AV block present ectopic atrial tachycardia.
STEP 2 – QRS alternation –each QRS is different from subsequent one by 5 mm –AVRT ,other tachycardia also
STEP 4 – p wave morphology in frontal plane –negative in lead I LEFT SIDE BYPASS TRACT.
STEP 5 –P WAVE in horizontal plane .left side,right side ..
Ref–ncbl.org.in



In brief from the diagram clues
Response to carotid sinus massage or adenosine –with termination of arrhythmia with Pwave –AVNRT with atrial premature beat .
Tachycardia persists with AV block –AT,AFL,SANRT Pseudo r ‘ wave in V1 –AVNRT SHORT RP interval – AVNRT,AVRT Long RP interval – AT,SANRT,AVNRT atypical

NARROW COMPLEX QRS TACHYCARDIA
SHORT RP INTERVAL
TYPICAL AVNRT
AVRT
LONG RP INTERVAL
ATYPICA
L AVNRT
AVRT
slow retrograde
conduction
Permanent Form
junctional
tachycardia
ATRIAL TACHYCARDIA
SANRTINAPPROPRIATE ST

ECG findings

Main Mechanisms and Typical Electrocardiographic Recordings of Supraventricular Tachycardia.

Pwaves
no
Irregular R-R
intervalATRIAL
FIBRILLATIO
N
Regular
R-R interv
al
AVNRT
yes
NORMAL MORPHOLOGY
SINUS TACHYCARDIASINUS NODE REENTRY
INAPPROPRIATE SINUS TACHYCARDIA



Differentiation of AVNRT from AVRT

P wave present but not of same morphology as sinus rhythm
Pseudo r’ wave in
V1
AVNRT
Pseudo S wave on lead II
AVNRT
Pwave ST-T
changes
Positive in
lead I
AVRT
Right
posterosepta
lAccessor
y pathway
Negative
in lead
I
AVRT
Left side
d accessory pathwa
y

AVNRT
Presence of a narrow complex tachycardia with regular R-R intervals and no visible p waves.
P waves are retrograde and are inverted in leads II,III,AVF.
P waves are buried in the QRS complexes –simultaneous activation of atria and ventricles – most common presentation of AVNRT –66%.
If not synchronous –pseudo s wave in inferior leads ,pseudo r’ wave in lead V1---30% cases .
P wave may be farther away from QRS complex distorting the ST segment ---AVNRT ,mostly AVRT.

AV NODAL REENTRANT TACHYCARDIA



AFTER ADENOSINE



AV-nodal-re-entry-tachycardia-(AVNRT)-on-an-ECG-heart-monitor[www.savevid.com].flv

AVRT
Typical – RP interval < PR interval RP interval > 80 milli sec Atypical –RP interval > PR interval Concealed bypass tract – only retrograde conduction Manifest bypass tract– both anterograde and
retrograde. Electrical alternans –the amplitude of QRS complexes
varies by 5 mm alternatively. Rate related BBB occuring and the rate of tachycardia
is decreasing –then the bypass tract is on the same side of the block.

AV REENTRANT TACHYCARDIA

PRinterv
al RP
interval
PR interval



WPW syndrome
Two types Orthodromic Antidromic Antidromic is wide complex tachycardia In NSR detected by delta wave. Can ppt into AF and VF on use of AV nodal blockers MEMBRANE ACTIVE ANTIARRHTYHMIC DRUGS are safe. CONCEALED WPW syndrome – no delta wave .less risk of
AF




Orthodromic AVRT

LOWN GANONG LEVINE syndrome Short PR interval Normal QRS complex PSVT

Sinus Tachycardia

Focal Atrial Tachycardia
P wave morphology changes. PR interval > 0.12 sec . Second,third degree AV block can occur. Tachycardia terminates with a qrs complex .. Right atrial origin– p wave inverted in V1. If biphasic in V1—initially positive then negative. Upright in lead AVL Opposite if of left atrial origin Superior origin –upright p waves in inferior leads Inferior origin –p waves are inverted in inferior leads.


Focal atrial tachycardia (LA focus)

Multifocal Atrial Tachycardia
At least three consequtive p waves with different morphologies with a rate > 100 bpm to be present.
Isoelectric baseline between p waves. Also called as choatic atrial tachycardia Mostly seen in COPD ,electrolyte abn,theophylline Rate usually does not exceed 130-140 bpm.

Multifocal Atrial Tachycardia

SANRT
Microreentrant tachycardia Usually precipitated and terminated by
premature atrial complexes. Atrial rate is usually 120-150 bpm. IART - Large or small reentrant circuit. AV block can occur.

Junctional tachycardias Non paroxysmal – accelerated junctional rhythm Rate < 100 bpm Usually junctional node 40-60 bpm Paroxysmal or focal junctional tachycardia is rare –automaticity. 110-250bpm. P waves may be before or after QRS complex Infrequent and nonsustained episodes –no treatment Acute termination of SVT and establish the mechanism of SVT
in case of acute setting. Long term goal is abolishing the arryhthmia substrate. Precipitating factors – electrolyte
imbalance,hypoxia,ischemia,hyperthyroidism to be sought out.

Acute Treatment
Of SVT

A 12 lead ECG during tachycardia and NSR.
No delay in therapy if the mechanism of SVT is not known.
Perform CAROTID SINUS MASSAGE,or give 6mg bolus adenosine.
In case of severe hemodynamic compromise a synchronised cardioversion to be given.

Carotid sinus massage
Check for carotid bruit before massage. At the level of cricoid cartilage,at the angle of
mandible the carotid sinus is situated. Gentle pressure is applied over the carotid sinus
for 5 -10 seconds. ECG recording to be present. In case of no response – try on the other side. Simultaneous pressure not to be applied both sides. Alternative manuevres are valsalva,gag reflex,ice
water pouring over the face.

If SVT is suspected to be AVnode dependent – drug of choice is adenosine and CCBs verapamil and diltiazem.
Useful for sustained cases of AV node independent tachycardias.
But digoxin,BBs,CCBs better control of ventricular response in atrial tachycardias
Class I agents to be combined with AV nodal blocking drugs – to eliminate 1:1 conduction of atrial to ventricles.

HEMODYNAMIC STATUS
STABLE BP >90/60 mmHg
Narrow QRSand regular
R-RVagal
maneuveresIV
adenosineIV
verapamil,diltiazemIV sotalolRefractor
y
Wide QRScomplex
Vagal
manuevresIV
adenosine
procainamid
e
Digoxin
Verapam
il Are contraindicated
UNSTABLEBP< 90/60 mmHg
Direct cardioversion

DRUG DOSE SIDE EFFECTS
AV NODAL BLOCKERS
ADENOSINE 6-12 mg bolus Flushing ,dyspneaChest pain
VERAPAMIL 0.15 mg/kg over 2 min
Hypotension bradycardia
DILTIAZEM 0.25-0.35 mg/kg -2 min
same
DIGOXIN 0.5-1.0 mg --- 2-10 min
Digoxin toxicity
PROPANOLOL 1-3mg over I min Hypotension bradycardia
CLASS I AAD
QUINIDINE 6-10MG/KG at 10 mg/min
hypotension
PROCAINAMIDE 10-15mg/kg at 50 mg/min
hypotension
DISOPYRAMIDE 1-2 mg/kg at 10 mg/min
hypotension
PROPAFENONE 1-2mg/min at 10 mg/min
Bradycardia,GI disturbance
FLECAINIDE 2 mg/kg at 10 mg/min
Bradycardia,dizziness
CLASS III SOTALOL 1-1.5mg/kg at 10 mg/min
Hypotension,proarrythmic
AMIODARONE 1.5 mg/kg during 15 min
Hypotension,bradycardia

Pharmacologic Agents for Short-Term Treatment of Supraventricular Tachycardia (SVT).
Delacrétaz E. N Engl J Med 2006;354:1039-1051.

AFTER ADENOSINE

Algorithm for Short term management
of SVT

Algorithm for long term
Management of SVT

Refractory cases
Narrow QRS complexes
IV adenosine
IV procainami
deIV
amiodarone
Atrial pacingDirect
cardioversion
Wide QRS Complexes
Atrial pacingDirect
cardioversion


Pill in the pocket approach In whom recurrences are infrequent. But sustained.well tolerated hemodynamically. Patients who have had only a single episode of SVT.. 100-200mg of flecainide at the onset of SVT is a reasonable
approach…until he reaches the hospital. 40-160 mg verapamil –without preexcitation, Betablockers Propafenone 150-450 mg. 80% cases interrupted with a combination of CCBand BB in 2
hrs…

Long term control of SVT Frequency and severity of episodes. LVF Cost benefits of radiofrequency ablation
over the pharmacotherapy . Pharmacotherapy is considered in patients
who defer catheter ablation,whom in which ablation failed,or carries a risk of AV block.
Multifocal atrial tachycardia Trial and error Accessory pathway – class Ia,Ic,III AV node blocking drugs Young patients – Ia drugs Class I agents LVD < 35% not used.
Long term treatment
Membrane active
AAD
Catheter
ablation
Curative surgery
Antitachycardia pacing

Adenosine
not to be used in bronchospastic pulmonary disease.
Adenosine precipitates asthma Given rapidly in 1-2 sec. If given by peripheral vein uplift the arm.. Max dose is 30 mg 6- 12-12 mg Terminates AVNRT .AFL with 2:1 block Potentiated by dipyradimole,carbamazepine –
decrease dose to 3 mg.

Other drugs
Calcium channel blockers,beta blockers ,digoxin are the next drugs to be used if not responded to adenosine
Usually 60 % cases respond to a dose of 6 mg and 95 % cases at 12 mg.
Type 1 a AAD, 1c,iii,AMIODARONE in refractory cases.
Beta blockers not to used IV in heart failure.
Long term treatment in case of recuurent episodes,hemodynamic instability.

Catheter guided Radiofrequency Ablation
Several multipolar catheters are introduced High right atrium ,bundle of
his ,RVapex,Coronary sinus. Radiofrequency is delivered at the site of earlier
activation Success is defined by elimination of the
tachycardia or loss of pre excitation. 90-98% success in AV node dependent 60-80% in case of AV node independent. Cryoablation more useful…

Catheter Ablation of Cardiac Arrhythmias.

Pacemakers
Temporary role in case of digoxin toxicity. Permanent in case of long term control To terminate the tachycardia Revert into sinus rhythm Prevent the occurrence. Overdrive suppression RF induced atrial pacing are used
No role of surgery presently in PSVT rx .

ACUTE LONG TERM
PHYSIOLOGICAL rest ,sedation valsalva
Valsalva maneuvre Carotid sinus massage
Carotid sinus massage
PHARAMACOLOGICAL
vagomimmetic Suppress triggering arrhythmias
Direct effect on AV node
Change properties of reentrant pathways
Slow VR Control VR
CATHETER ABLATION SURGERY
Ablation or sectioning of reentrant pathway
ELECTRONIC DEVICES
Temp .pacing cardioversion
Permanent pacemakerAntitachycardia pacing

Some important points
Rxof PSVT given for patient comfort except in IHD,MS
When the QRS complex is wide and VT is mistaken as SVT with ABERRANT conduction IV verapamil – not recommended decreases BP.
If DC cardioversion to be avoided because of possible adverse response to digitalis adm …pacing Rt atrium and ventricle via temp pacing.
In WPW syndrome avoid VERAPAMIL,LIDOCAINE . Avoid digoxin. In SANRT ,IART –class IA,IC ,BB SANRT –digoxin.

Cont…
Rx of ectopic atrial tachycardia – consider digitalis toxicity,chronic lung disease,metabolic abn,electrolyte abnormalities,acute MI ----temporary pacing.
Unsuccessful is EC Removal or reversal of inciting factor Surgical excision of focus. Rx of MAT –chronic lung disease,metabolic,rare
is digitlais toxicity ---CCBS,BBs ..no role of cardioversion,devices ,surgery.

In case of WPW syndrome symptomatic concealed or manifested ..and evidence of preexcitation on NSR …send the patient for catheter ablation…

Our case
1. carotid sinus pressure 2.IV adenosine. 3.long term treatment depends upon episodes. 4.any underlying abnormality to be checked for. 5.definitive etiology only knon by EP study. 6.95% cases respond to RF ablation. 7.much less complications with cryoablation. 8.in case if SVT recurrs after ablation –opt for
pacemaker..

Lets have a look at the ECGs

SUPRAVENTRICULAR TACHYCARDIAS“You only get so many heart beats – you should save some for later in life” Dr. Samuel Levine




DIAGNOSIS IS ATRIAL FLUTTER

Sinus tachycardia was thought..
but it was AFL


AVNRT in structural heart disease

Look for the correct lead placement

AVNRT can occur in the background of acute MI










Special problems 1.Coexisting Double Tachycardias May not be identified during noninvasive
testing ..needs EP study. Ex—typical AVNRT and AT. Concentric –eccentric –concentric. AVNRT –both APC,VPC AT only APC 2.Pseudo AF- infrequent presentation of PSVT. Occurs during onset and termination of tahcycardia. Multiple accessory AV pathways. In young who have AF without other risk factors. 5% of AVNRT. Group beating is seen

REFERENCES CARDIOLOGY third edition –Michael. H.Crawford HURST’S THE HEART – 12 th edition. BRAUNWALD’S HEART DISEASE –A TEXTBOOK OF CARDIOVASCULAR
MEDICINE – 7 th ED HARRISON’S PRINICPLES OF INTERNAL MEDICINE -17 th ED SUPRAVENTRICULAR TACHYCARDIA –NEJM 2006 CARDIOVASCULAR MEDICINE – SVT – JERONIMO FERRE’ BASIC AND BEDSIDE ELECTROCARDIOGRAPHY –ROMULO.F.BALTAZAR SCHAMROTH –ELECTROCARDIOGRAPHY www.medscape.com www.ecglibrary.com www.googleimages.com www.acc.org. www.clinicaltrials.gov www.nejm.org


Aim for any case of cardiology

Than
k youSagittari
an

Related Documents