Practice CMAJ CMAJ • OCTOBER 27, 2009 • 181(9) © 2009 Canadian Medical Association or its licensors 615 A 46-year-old man presented with a pruritic diffuse erup- tion on his thighs, lower legs and buttocks that had grad- ually worsened over a 1-year period. His medical his- tory included a heart transplant, insulin-dependent diabetes mellitus, chronic renal failure for which he was receiving peri- toneal dialysis, hypertension, gout and hyperlipidemia. An exam- ination showed follicular keratotic papules that were distributed diffusely over his legs and buttocks (Figure 1). The results of a skin biopsy showed a hair follicle with perforation that extended into the dermal tissue and contained a tract of necrotic tissue debris with degenerate elastin fibres (Figure 1). These findings were consistent with acquired perforating dermatosis. Perforating dermatoses are a group of conditions character- ized by transepidermal elimination of dermal material (colla- gen, elastic tissue or necrotic connective tissue). Major perfor- ating disorders include reactive perforating collagenosis (inherited disorder of collagen perforation), elastosis perforans serpiginosa (elastic tissue perforation associated with Down syndrome and Ehler–Danlos syndrome), perforating folliculitis (perforation of necrotic material secondary to local trauma) and acquired perforating dermatosis. The differential diagnosis includes prurigo nodularis, folliculitis, arthropod bites, multi- ple keratoacanthomas, psoriasis and lichen planus. 1 Acquired perforating dermatosis classically presents with severely pruritic follicular hyperkeratotic papules, sometimes umbilicated, on the hair-bearing limbs of adults, as in our patient. Generalized papules may also be seen. Acquired per- forating dermatosis is a chronic disease, usually associated with diabetes mellitus or renal failure or both. In patients receiving dialysis, acquired perforating dermatosis occurs in about 10% of patients. 2 It is also rarely associated with liver disease, malignant disease, hypothyroidism and HIV. 3 Investigations include skin biopsy and a search for associ- ated systemic diseases. Treatment may be directed at relieving pruritus, because perforating disorders can be exacerbated by koebnerization (lesions appearing at sites of minor trauma, as in psoriasis). Most treatment strategies are supported by anec- dotal evidence and include oral or topical retinoids and topical or intralesional corticosteroids. 1 Phototherapy (narrow-band or broad-band UVB, or psoralen plus UVA) may be helpful for pruritus. Other approaches include the use of antibiotics (e.g., doxycycline) and destructive methods such as cryotherapy, sur- gical debridement and laser therapy. 1 Our patient was given retinoids, both oral (acitretin 25 mg daily) and topical (tazarotene gel 0.1%). After 4 months of retinoid therapy, the patient’s pruritus was substantially reduced and the rash had improved by more than 80%. However, he died suddenly from severe cardiac disease. REFERENCES 1. Bolognia JL. Jorizzo JL, Rapini RP, editors. Dermatology. 2nd ed. Spain: Mosby; 2008. 2. Morton CA, Henderson IS, Jones MC, et al. Acquired perforating dermatosis in a British dialysis population. Br J Dermatol 1996;135:671-7. 3. Saray Y, Seckin D. Bilezikci B. Acquired perforating dermatosis: clinicopathologi- cal features in twenty-two cases. J Eur Acad Dermatol Venereol 2006;20:679-88. Clinical images Acquired perforating dermatosis: association with diabetes and renal failure Carrie B. Lynde BSc, Melanie D. Pratt MD From the Faculty of Medicine (Lynde), University of Toronto, Toronto, Ont., and the Division of Dermatology (Pratt), Department of Medicine, Univer- sity of Ottawa, Ottawa, Ont. Cite as CMAJ 2009. DOI:10.1503/cmaj.082013 DOI:10.1503/cmaj.082013 Figure 1: A 46-year-old man with diabetes and renal failure. Follicular keratotic papules consistent with acquired perforating dermatosis were distributed diffusely over his legs (A) and buttocks (B). Skin biopsy (C) showing a hair follicle with perforation extending into the dermal tissue which contains a tract of necrotic tissue debris with degenerate elastin fibres (hematoxylin–eosin stain, original magnification × 40). A B C Previously published at www.cmaj.ca

APD
Sep 08, 2015
ACQUIRED PERFORATING DISEASE
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
-
PracticeCMAJ
CMAJ OCTOBER 27, 2009 181(9) 2009 Canadian Medical Association or its licensors
615
A46-year-old man presented with a pruritic diffuse erup-tion on his thighs, lower legs and buttocks that had grad-ually worsened over a 1-year period. His medical his-tory included a heart transplant, insulin-dependent diabetesmellitus, chronic renal failure for which he was receiving peri-toneal dialysis, hypertension, gout and hyperlipidemia. An exam-ination showed follicular keratotic papules that were distributeddiffusely over his legs and buttocks (Figure 1). The results of askin biopsy showed a hair follicle with perforation that extendedinto the dermal tissue and contained a tract of necrotic tissuedebris with degenerate elastin fibres (Figure 1). These findingswere consistent with acquired perforating dermatosis.Perforating dermatoses are a group of conditions character-
ized by transepidermal elimination of dermal material (colla-gen, elastic tissue or necrotic connective tissue). Major perfor -ating disorders include reactive perforating collagenosis(inherited disorder of collagen perforation), elastosis perforansserpiginosa (elastic tissue perforation associated with Downsyndrome and EhlerDanlos syndrome), perforating folliculitis(perforation of necrotic material secondary to local trauma)and acquired perforating dermatosis. The differential diagnosisincludes prurigo nodularis, folliculitis, arthropod bites, multi-ple keratoacanthomas, psoriasis and lichen planus.1Acquired perforating dermatosis classically presents with
severely pruritic follicular hyperkeratotic papules, sometimes
umbilicated, on the hair-bearing limbs of adults, as in ourpatient. Generalized papules may also be seen. Acquired per-forating dermatosis is a chronic disease, usually associatedwith diabetes mellitus or renal failure or both. In patientsreceiving dialysis, acquired perforating dermatosis occurs inabout 10% of patients.2 It is also rarely associated with liverdisease, malignant disease, hypothyroidism and HIV.3Investigations include skin biopsy and a search for associ-
ated systemic diseases. Treatment may be directed at relievingpruritus, because perforating disorders can be exacerbated bykoebnerization (lesions appearing at sites of minor trauma, asin psoriasis). Most treatment strategies are supported by anec-dotal evidence and include oral or topical retinoids and topicalor intralesional corticosteroids.1 Phototherapy (narrow-band orbroad-band UVB, or psoralen plus UVA) may be helpful forpruritus. Other approaches include the use of antibiotics (e.g.,doxycycline) and destructive methods such as cryotherapy, sur-gical debridement and laser therapy.1 Our patient was givenretinoids, both oral (acitretin 25 mg daily) and topical(tazarotene gel 0.1%). After 4 months of retinoid therapy, thepatients pruritus was substantially reduced and the rash hadimproved by more than 80%. However, he died suddenly fromsevere cardiac disease.
REFERENCES1. Bolognia JL. Jorizzo JL, Rapini RP, editors. Dermatology. 2nd ed. Spain: Mosby;
2008.2. Morton CA, Henderson IS, Jones MC, et al. Acquired perforating dermatosis in a
British dialysis population. Br J Dermatol 1996;135:671-7.3. Saray Y, Seckin D. Bilezikci B. Acquired perforating dermatosis: clinicopathologi-
cal features in twenty-two cases. J Eur Acad Dermatol Venereol 2006;20:679-88.
Clinical images
Acquired perforating dermatosis: association with diabetesand renal failure
Carrie B. Lynde BSc, Melanie D. Pratt MD
From the Faculty of Medicine (Lynde), University of Toronto, Toronto, Ont.,and the Division of Dermatology (Pratt), Department of Medicine, Univer-sity of Ottawa, Ottawa, Ont.
Cite as CMAJ 2009. DOI:10.1503/cmaj.082013DOI:10.1503/cmaj.082013
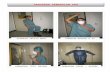
Figure 1: A 46-year-old man with diabetes and renal failure. Follicular keratotic papules consistent with acquired perforating dermatosis weredistributed diffusely over his legs (A) and buttocks (B). Skin biopsy (C) showing a hair follicle with perforation extending into the dermal tissuewhich contains a tract of necrotic tissue debris with degenerate elastin fibres (hematoxylineosin stain, original magnification 40).
A B C
Previously published at www.cmaj.ca
image-lynde-la:Layout 1 07/10/09 10:02 AM Page 615
Related Documents