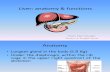
Anatomy Of The Liver And Effect Of Anaesthetic Drugs On Liver Presented by: Dr. Rajat Dadheech Moderator: Dr. Rama Chatterjee

Anatomy of the liver and effect of anaesthetic drugs on liver
Nov 11, 2014
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
- 1. Anatomy Of The Liver And Effect Of Anaesthetic Drugs On LiverPresented by:Dr. Rajat DadheechModerator:Dr. Rama Chatterjee
- 2. Anatomy of the liverThe liver is the largest gland of the body, weighing 1200 -1600 g, it is wedge- shaped, and covered by a network of connective tissue (Glissons capsule).
- 3. It is connected to the diaphragm and abdominal walls by five ligaments: the membranous falciform (also separates the right and left lobes), coronary, right and left triangular ligaments, and the fibrous round ligament (which is derived from the embryonic umbilical vein).
- 4. Lobes Of The LiverAnatomically the liver is divided into a Right and a Left lobe by the falciform ligamentThe Right lobe also has two minor lobes- The caudate lobe and The quadrate lobe
- 5. Blood Supply: The Liver receives around 1500 ml of blood/min The blood supply of the Liver is derived from The Portal Vein (80%) and The Hepatic Artery (20%) Terminal branches of the hepatic portal vein and hepatic artery empty together and mix as they enter sinusoids in the liver. Sinusoids are distensible vascular channels lined with highly fenestrated endothelial cells and bounded circumferentially by hepatocytes.
- 6. The bloodleaves thesinusoids via acentral vein ,which drains inthe hepatic vein.
- 7. Claude Couinad A french surgeon & anatomist who made significant contribution in the field of hepatobiliary surgery ,he was the first to describe segmental anatomy of the liver
- 8. Functional divisions of Liver Middle hepatic vein divides the liver into right and left lobes (or right and left hemiliver). This plane runs from the inferior vena cava to the gallbladder fossa (Cantlies line) Right hepatic vein divides the right lobe into anterior and posterior segments Left hepatic vein divides the left lobe into a medial and lateral part.
- 9. Histology Liver lobules hexagonal structuresconsisting ofhepatocytes At each of the sixcorners of a lobule is aportal triad
- 10. Portal Triads: Branches of two vessels: portal vein,hepatic artery, along with bile drainage ductules all runtogether to infiltrate all parts of liver. Zonal Flow of Blood
- 11. Zone 1- Rich in Oxygen, mitochondria Concerned with Oxidative metabolism and synthesis of glycogenZone 2- transitionZone 3- lowest in Oxygen, anaerobic metabolism,Biotransformation of drugs, chemicals, and toxinsMost sensitive to damage due to ischemia, hypoxia, congestion
- 12. Hepatic Micro Circulatory Cone
- 13. Biliary Tract:
- 14. Regulation of Hepatic Blood FlowIntrinsic Regulation Hepatic Arterial Buffer Response -HABR Pressure flow Autoregulation Metabolic controlExtrinsic Regulation Neural Control Humoral Control
- 15. Hepatic arterial buffer system With an intact HABR, changes in portal venous flow cause reciprocal changes in hepatic arterial flow. The HABR mechanism involves the synthesis and washout of adenosine from periportal regions. Various disorders (e.g., endotoxemia, splanchnic hypo perfusion) may decrease or even abolish the HABR and render the liver more vulnerable to hypoxic injury.
- 16. PRESSURE FLOW AUTO REGULATION- Hepatic pressure auto-regulation keeps constant blood flow despite wide fluctuation in systemic BP. The mechanism involves myogenic responses of vascular smooth muscle to stretch. The hepatic artery exhibits pressure-flow auto regulation in metabolically active liver (postprandial) but not in the fasting state. Thus, hepatic flow autoregulation is not likely to be an important mechanism during anesthesia. Pressure-flow autoregulation is nonexistent in the portal circulation.Thus, decrease in systemic blood pressureas often occurs during anesthesiatypically lead to proportional decrease in portal venous flow
- 17. Metabolic Control Decrease in oxygen tension or the pH , Pco2 of portal venous blood ,typically lead to increase in hepatic arterial flow. Postprandial hyperosmolarity increases hepatic arterial and portal venous flow but not in the fasting state. The underlying metabolic and respiratory status (e.g., hypercapnia, alkalosis, arterial hypoxemia) also modulates the distribution of blood flow within the liver.
- 18. NEURAL CONTROL Fibres of the vagus,phrenic and splanchnic nerves(postganglionic sympathetic fibres from T6 to T11)enter the liver at the hilum When sympathetic tone decreases,splanchnic reservoir increases whereas sympathetic stimulation,translocates blood volume from the splanchanic reservoir to the central circulation. Vagal stimulation alters the tone of the presinusoidal sphincters,the net effect is a redistribution of intrahepatic blood flow without changing total hepatic blood flow.
- 19. Humoral Control Gastrin, Glucagon, Secretin, Bile salts,Angiotensin II, Vasopressin, Catecholamines. Cytokines, Interleukins, and other inflammatory mediators have been implicated in the alteration of normal splanchnic and hepatic blood flow.
- 20. FACTORS AFFECTING HEPATICBLOOD FLOWINCREASE IN HEPATIC DECREASE IN HEPATICBLOOD FLOW BLOOD FLOW Hypercapnia IPPV Acute hepatitis Hypocapnia Supine posture Hyhpoxia Food intake Cirrhosis Drug: Beta Agonist alpha Stimulation Phenobaritone Beta blocker Enzyme inducers Halothane, volatile & anesthetics Vasopressin
- 21. Liver and Anaesthesia Anesthesia & anaesthetic drugs affects the hepatic function by following mechanisms : Alteration in the hepatic blood flow n HABR. Metabolic function. Drug metabolism. Billiary function.
- 22. Effect of volatile agents on hepaticblood flow Halothane: Causes hepatic arterial constincton, microvascular vasoconstriction Enflurane: Increase in hepatic vascular resistance Isoflurane: Increase in microvascular blood velocity Sevoflurane & Desflurane: Preservation of hepatic blood flow & function
- 23. EFFECT OF INTRAVENOUS AGENTSON HEPATIC BLOOD FLOW KETAMINE: Little effect on hepatic blood flow PROPOFOL: Significant splanchnic vasodilator increases both hepatic arterial & portal venous blood flow THIOPENTONE & ETOMIDATE: Hepatic arterial blood flow reduction, reducedf cardiac output
- 24. NEUROMUSCULAR BLOCKINGDRUGSVecuronium, rocuronium, mivacurium: Reduced elimination and Prolong duration of action specially with infusion & repeated dosesAtracurium & cisatracrium: Nondependant of hepatic metabolism and can be used without modification of doses in end stage liver disease
- 25. REGIONAL ANESHESIA & HEPATICBLOOD FLOW Reduction in hepatic blood flow in high spinal & epidural anesthesia Secondary to hypotension Reversed by vasopressors like dopamine, ephedrine
- 26. Halothane Hepatitis It is immunologically mediated,as it induces both neoantigens & auto antigens. The incidence of fulminant hepatic necrosis terminating in death associated with halothane was found to be 1 per 35,000. Demographic factors ; Its a idiosyncratic reaction, susceptible population include Mexican Americans ,Obese women, , Age >50 yrs, , Familial predisposition,Severe hepatic dysfunction while Children are resistant. Prior exposure to halothane is a important risk factor & multiple exposure increases the chance of hepatitis.
- 27. ISOFLURANE. Isoflurane metabolism yields highly reactiveintermediates (TF-acetyl chloride; acyl ester) that bindcovalently to hepatic proteins. For this isoflurane most likelycauses hepatitis.It undergoes minimal biodegradation, preservesmicrovascular blood flow & oxygen delivery more thanhalothane or enflurane .DESFLURANE-it is similarly biotransformed totrifluoroacyl metabolites, appears even less likely thanisoflurane to cause immune injury because only 0.02 to 0.2%of this agent is metabolized (1/1,000th that of halothane).Desflurane metabolites are usually undetectable in plasma,except after prolonged administration.
- 28. Desflurane hepatic blood flow ,it markedly reduce oxygendelivery to the liver and small intestine without producingcomparable reductions of hepatic oxygen uptake or hepatic andmesenteric metabolism. Therefore, desflurane anesthesia maydecrease the oxygen reserve capacity of both the liver and the smallintestine.SEVOFLURANE It is metabolized more extensively than isofluraneor desflurane,but slightly less than enflurane, and much less thanhalothane. The metabolism of sevoflurane is rapid (1.5 to 2 timesfaster than enflurane), and produces detectable plasmaconcentrations of fluoride and hexafluoroisopropanol (HFIP)within minutes of initiating the anesthesia. The liver conjugates most of the HFIP with glucuronic acid, whichis then excreted by the kidney.
- 29. NITROUS OXIDE- it produces a mildincrease in sympathetic nervous systemtone leads to mild vasoconstriction of thesplanchnic vasculature, leading to adecrease in portal blood flow, and mildvasoconstriction of the hepatic arterialsystem. N2O is a known inhibitor of theenzyme methionine synthase, whichcould potentially produce toxic hepaticeffects.
- 30. Intravenous Anesthetics- Etomidate and thiopental at larger doses (>750 mg) may cause hepatic dysfunction by hepatic blood flow, either from hepatic arterial vascular resistance or from reduced cardiac output and blood pressure. Ketamine has little impact on hepatic blood flow, even with large doses Propofol increases Blood Flow in both the hepatic arterial and portal venous circulation, suggesting a significant splanchnic vasodilator effect
- 31. OPIOIDS Opioids have little effect on hepatic function, provided they do not impair hepatic blood flow and oxygen supply. All opioids increase tone of the common bile duct and the sphincter of Oddi, as well as the frequency of phasic contractions, leading to increases in biliary tract pressure and biliary spasm. Morphine undergoes conjugation with glucoronic acid at hepatic & extra hepatic site (kidney). The significantly reduced metabolism of morphine in patients with advanced cirrhosis leads to a prolonged elimination half-life, markedly increased bioavailability of orally administered morphine, decreased plasma protein binding, and potentially exaggerated sedative and respiratory-depressant effects. The oral dose of the drug should be reduced because of increased bioavailability
- 32. Neuromuscular Blocking Drugs The volume of distribution of muscle relaxants, may increase due to albumin an increase in -globulin or the presence of edema.so the initial dose requirements of these medications are increased in cirrhotic patients and subsequent dose requirements may be , and drug effects prolonged, owing to in hepatic blood flow and impaired hepatic clearance, and possible concurrent renal dysfunction.
- 33. Neuromuscular Blocking DrugsVecuronium-it is a steroidal muscle relaxant It undergoes hepatic elimination by acetylation. Decreased clearance, a prolonged elimination half-life, and prolonged neuromuscular blockade in patients with cirrhosis . Rocuronium- another steroidal muscle relaxant with a faster onset of action than vecuronium, also undergoes hepatic metabolism and elimination. Hepatic dysfunction can increase the volume of distribution of rocuronium, thereby prolonging its elimination half-life and producing a longer clinical recovery profile and return of normal twitch tension.
- 34. Neuromuscular Blocking DrugsAtracurium & Cisatracurium Elimination half-lives and clinical durations of action are similar in cirrhotic.82%to Bound albumin they undergo clearance by organ-independent elimination i.e. spontaneous non-enzymatic degradation (Hoffmanns elimination). Laudanosine, a metabolite of both atracurium and cisatracurium, is eliminated primarily by the liver; and although its concentration may increase in patients undergoing liver transplantation, clinically relevant neurotoxicity has not been reported
- 35. EFFECTS OF HEPATIC DYSFUNCTIONOF ANESTHETIC DRUGS Altered protein binding Altered volume of distribution Altered drug metabolism due to hepatocyte dysfuction
- 36. EFFECTS OF HEPATIC DYSFUNCTIONON ANESTHETIC DRUGS Opioids: exaggerated sedative & respiratory depressant effect and Half life is almost doubled Benzodiazepines : Duration of action increased Thiopentone, Etomidate, Propofol, Ketamine: Repeated doses & prolong infusion causes accumulation of drugs Increases risk of hepatic encephalopathy
- 37. TAKE HOME MESSAGES Liver major organ of metabolism Live dysfuction affects pharmacokinetics of anesthetic drugs Anesthetic drugs affects liver function Neuroaxial blocks: reduction in hepatic blood flow due to hypotension Intropetative hypotension, hypoxia, hypocapnia, use of hepatotoxic drugs in perioperative period can cause postoperative hepatic dysfunction
Related Documents