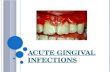
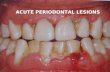
Acute enteric infections: etiology, clinical features, principles of treatment Lecture for the V year foreign students Assistant professor T. Sirotchenko Chair of pediatrics and children’s infection disease

Acute enteric infections
Oct 14, 2014
Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Acute enteric infections: etiology, clinical features, principles of treatment
Lecture for the V year foreign students
Assistant professor T. Sirotchenko
Chair of pediatrics and children’s infection disease

• Acute enteric infections are infections poly-etiological diseases (virus, bacterial, fungal, parasitical) with fecal – oral mechanism of the transmissions and with morbid affection on the different parts of the intestines.

• According the international classification all diarrheal diseases may be dividing on two groups: infection and non-infection. The infection diarrhea may be dividing on invasive group (inflammatory, bleeding) and secretory (non-inflammatory, watery).

• Rotavirus, Adenovirus, Coronavirus, Reovirus, Vibrio Cholerae, Escherichia coli (some types), pathogenic fungi, protozoa cause the secretory diarrheas.
• Shigella, Salmonella, Escherichia coli (some types), Yersenia enterocolitica, Campylobacter, Clostridium, Staphylococcus, lamblias, entmoebas cause the invasive diarrheas.
• Pathogenesis of diarrhea of AEI have such mechanisms as: osmotic, secretory, inflammatory

Osmotic mechanism of diarrhea (under virus AEI).
Virus damages
epithelium of the intestines
increases the level
of the disaccharidases (lactase, maltase, sucrase).
Disaccharides accumulate
in the cavity of intestines, decrease the osmotic pressure, hinder absorption of the water

Secretory mechanism (AEI with the enterotoxin
Enterotoxin activates
ferment (adenylatcyclase)
increases the synthesis of the cyclic nucleotides
stimulates the penetration of the cell’s membranes and increases
he secretion of the water and electrolytes

Inflammatory mechanism (invasive diarrheas).
Invasion the pathogen in the wall
of the intestine inflammation
synthesis of the inflammation’s
mediator (prostaglandins,
histamine, serotonin
and cytokines)
cell’s membranes are damaged, the microcirculation is broken,
intestinal motility is intensified.
exudates (with the blood, protein, mucus) are in the cavity of intestines, dimension enteric contents
are increased, quantity of the fluid is increased too.

EcherichiosisEcherichia coli,
gram - negative colibaccilius, non spore - forming bacteria,
Enteropathogenic (O111, O55, O25, O44, O127)
Enteroinvasive(O28, O124, O151, O143);
Enterohaemorrhagic(O159, O121, O126, O145)
Enterotoxigenic (O1, O2, O6, O9);

Echerichiosis
• The sources of infection are ill person and bacteriocarries.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary, watery, contact and domestic.
• Incubation period - 3 - 6 days.

Clinical algorithm: Echerichiosis
• intoxication
• vomiting, regurgitation
• faeces – watering, canary with the glassy mucous admixtures
• pain in stomach, haemorrhagic colitis

Echerichiosis ( clinic course)
• Beginning of disease is increase of temperature (37,5-380C), intoxication, disorders of the function of the intestines (remiss faeces, vomiting, regurgitation, increasing of the appetite) during first 5 days.
• Next faze ( 2-5 days) watering, canary faeces with the glassy mucous or blood’s admixtures; vomiting 1-2 times during day, prolonged and persistent bloating of stomach and palpatory tenderness, dehydration, decreasing of body’s mass.
• Next faze- decreasing of the temperature and intoxication, normal faeces, recovery

Laboratory tests:• epidemiological anamnesis
• blood ad urinal tests
• coprocytogramm ( microscopy of faeces) – presence of the mucus, leucocytes, epithelial cells
• haemoagglutination reaction (HGA) – on the 2-3- days and on the 10-12 days of disease
• express – test ( method of the luminescence) – detection of the Escherichia

Shigellosis
Pathogen – Shigellae, gram - negative colibaccilius,
aerobe
A (Sh. Dysenteriae)
B (Sh. Flexnery) D (Sh. Sonnei)
C (Sh. Boydi)

Shigellosis• The sources of infection are ill person and
bacteriocarries.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary (Sh.Sonnei), watery (Sh. Flexnery), contact and domestic, “alimentary line” take place – from beginning to end
• Incubation period – 0 (some hours) - 6 days.

Shigellosis: Children of the preschool and school age• acute beginning of disease ( increasing the
temperature – 38-40C, regurgitation, vomiting, decreasing of the appetite, head ache, toxic encephalopathy)
• periodical pain in the stomach
• spasm and pain in the sigmoid colon
• faeces – green, frequent, remiss, nonplentiful, with mucous, blood and purulent admixtures, “dysenteric or rectal spit” -
• relaxation of the external sphincter muscle of anus or incompletely closed anus

Shigellosis: Children of the early age• acute beginning of disease, severe
toxicosis, affections of the nervous and cardiovascular system
• toxic encephalopathy - disorders of the consciousness, convulsions, disorders of microcirculation
• enterocolitis
• prolonged clinical course

Rectoromanoscopic picture of shigellosis.

Clinic classification of the dysenteryType Severity Clinical
course
Typical form
Atypical forms:
low-grade
dyspeptic
subclinic
hypertoxic
slight
moderate
severe:
with the toxic symptoms
with the local process
mixed - forms
Acute ( under 1 month)
Prolonged ( under 3 month)
Bacterio-carrier

Laboratory tests:• epidemiological anamnesis
• blood ad urinal tests
• coprocytogramm ( microscopy of faeces) – presence of the mucus, leucocytes, epithelial cells
• bacteriologic tests – until beginning the treatment – inoculation of the some mediums (agar and so on)
• haemoagglutination reaction (HGA) – on the 2-3- days and on the 8-10 days of disease (uninformative)
• express – test ( method of the luminescence) – detection of the Shigella
•

Salmonellosis
Pathogen – Salmonellae ,
gram - negative facultative colibaccilius,
D (Salm. London
E (Salm. anatum)
F ( Salm. enteritidis)
C (Salm. infantis
A (Salm. typhimurium)
B (Salm. virchov)

Salmonellosis
• The sources of infection are ill person and bacteriocarries, animals.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary, watery, contact and domestic. Factors of transmissions are pork, meat of poultry, beef, eggs and egg’s dishes.

Salmonellosis
TypClinic classification of the typhoid fevere
Severity Clinic course
Typical forms:
a. localized (gastritis entheritis gastroenteritis and so on)
b. generalized
( such a typhus, septic)
Atypical forms:
low-grade
subclinic
hypertoxic
slight
moderate
severe
Acute ( under 1 month)
Prolonged ( under 3 month)
Chronic ( more than 3 month)
With the
complications

Salmonellosis: Children of the preschool and school age
• prolonged fever, vomiting
• coated tongue abdominal swelling morbidity and borborygmus in the right iliac part
• faeces have green mucus, blood and stinking odor
• heratosplenomegaly

Faeces of patient with salmonellosis.

Salmonellosis: Children of the early age:
• - gradual clinical course
• - severe toxicosis and exycosis
• - heamocolitis, heratosplenomegaly
• - septic form of disease
• - mixed – infections, complications
• - incidence of the forming of the bacteriocarrier

Laboratory tests:
• epidemiological anamnesis
• blood ad urinal tests
• coprocytogramm ( microscopy of faeces) – presence of the mucus, leucocytes, epithelial cells
• bacteriologic tests of faeces, blood and vomit masses, foodstuff– in first days, inoculation of the some mediums (bile salt agar and so on)

Typhoid fever
• Pathogen is Salmonella typhi, gram - negative facultative colibaccilius from D group.
• The sources of infection are ill person and bacteriocarries.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary, watery, contact and domestic. Factors of transmissions are use of the water or swimming in the indoor reservoir

Typhoid fever
Type Severity Clinic course
Typical forms
Atypical forms:
septic
with the separated affections
rudimentary
slight
moderate
severe:
toxic, heamorrhagic, with the nervus syndrome
with the etnteric syndrome
with cardiovascular syndrom
Without the complications
With the complications:
early, late, allergic,
purulent
With the acute condition
With the relapse

Typhoid fever: Children of the preschool and school age
• acute beginning with the high temperature
• head ache with the disturbances of the sleep, dizziness, status typhosus
• pale skin, nonplentiful pink maculopapular rush, which disappears after thumb pressure
• coated dry reinforced tongue with the imprint of the teeth
• hepatosplenomegaly
• bradicardia, dry and bubbling rales in the lungs
• constipation

Typhoid fever: Children of the early age:
• - acute clinical course with high fever
• - bad appetite, dyssomnia, nervoness
• - vomiting, spasms, mental confusion
• - severe toxicosis and exycosis, diarrhea – 10-15 time during day, green mucus
• - hepatosplenomegaly, enteroparesis
• - maculopapular rush is very pale or is absent
• - taxicardia, bacterial complications – otitis, pneumonia, stomatitis

. Roseoles ("rose spots") in patient with typhoid fever

Laboratory tests:• epidemiological anamnesis ( village stay-
пребывание в деревне, swimming in the reservoir, use the milk or milk’s product)
• blood ad urinal tests
• bacteriologic tests of blood ( three times during first days on the height of the fever), faeces ( during second week of the disease), and urine (during third week of the disease)
• serological tests – reaction of the indirect haemagglutination (RIG) with the erythrocytic antigen– after 6-7-days of disease, Vidal ‘s reaction – after 2 weeks of disease, RIG with the Vi- antigen – after 3 weeks of disease – for the diagnostic of bacteriocarries.

Paratyphoid A,B and C• Pathogen is Salmonella paratyphii, gram –
negative, anaerobe colibaccilius from A,B and C group.
• The sources of infection are ill person and bacteriocarries.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary (paratyphoid B), watery (paratyphoid A), contact and domestic.
• Factors of transmissions are foods (milk, salads, ice-cream, berries and vegetables), water, household goods

Main clinical sings of the paratyphoid A
• children of the preschool and school age
• incubation period – 5-20 days
• - acute beginning, fever, head ache, pain in the stomach
• - diarrhea - abdominal swelling, morbidity along the full length and borborygmus
• - catarrhal inflammation on the fauces, herpes, conjunctivitis
• - enteric bleeding, necrosis of intestine, enteric perforation

Main clinical sings of the paratyphoid B• children of the early age
• incubation period – 1-14 days
• specific intoxication with the gastroenterocolitis or enterocolitis
• acute beginning, fever, head ache, vomiting, diarrhea
• pale skin, maculopapular rush after 3-5-days of disease
• hepatosplenomegaly

Laboratory tests:
• epidemiological anamnesis use the milk or milk’s product or some another products)
• blood ad urinal tests
• bacteriologic tests of blood ( three times during first days on the height of the fever), faeces ( during second week of the disease), and urine (during third week of the disease)
• serological tests – reaction of the indirect haemagglutination (RIG) with the erythrocytic antigen– after 6-7-days of disease, Vidal ‘s reaction – after 2 weeks of disease, RIG with the Vi- antigen – after 3 weeks of disease – for the diagnostic of bacteriocarries.

Cholera• Pathogens are Vibrio choleare and Vibrio El
-Tor , gram – negative, aerobe vibrions.
• The sources of infection are ill person and bacteriocarries.
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary, watery, contact and domestic. Factors of transmissions are fruits, berries and vegetables, infection water, fish, shrimp, crabs, clams

Clinic classification of cholera
Type Severity Clinic course
Typical forms
Atypical forms:
low- grow
subclinic
fulminant
dry
slight
moderate
severe
Acute
Without complications
With the complications:
pneumonia, shock

Cholera : Children of the preschool and school age
• acute beginning with the severe diarrhea, vomiting, without pain in the stomach and spasms
• vomit masses are rice – water or lactoserum
• subnormal temperature
• acrocyanosis, laundress’s hands
• aphonia, husky voice, tachypnea, tachycardia, anuria

Cholera :Children of the early age• severe clinic course with the
complications
• beginning of disease with the high temperature and intoxication
• quickly developing of the hypotonic exicosis
• affects of the CNS
• hypocaliemia, hypoglycemia

Laboratory tests: Cholera• epidemiological anamnesis (use the fish, shrimp,
crabs, clams or some another products)
• blood ad urinal tests
• biochemical tests: level of the Na and K, creatinine, urea, general protein
• microscopy of the native smears of the feces ( may be find of the morphological virions)
• bacteriologic tests of blood, faeces under beginning the treatment
• express – diagnostic ( method of the luminescent antibodies) - after 3-5 hours
• – method of the immobilization and micro agglutination with the specific anticholera 01 – serum) - answer after some minutes

Yersinia’s infections • Pathogens are Yersenia enterocolitica and
Yersenia pseudotuberculosis, gram – negative, aerobe.
• The sources of infection are ill person and mouse, rat, dog, cat, pig, caw, sheep
• Mechanism of the transmissions is fecal – oral.
• The ways of the transmissions are alimentary, watery, contact and aerogenic.

Yersenia enterocolitica: main clinical sings• acute beginning with the pain in the stomach, pain
and borborygmus in the iliac parts, sickness
• general intoxication – head ache, pain in the joints, chill
• exanthema ( punctulated, in the axillary region and on the chest, around the joints, may be with hemorrhagic character
• icteritiousness of the skin, hepatomegaly, hepatitis
• hyperemia of the plants and palms
• fever
• diarrhea – with the green mucus, 10-15 time in day
• lymphadenopatia

Yersenia pseudotuberculosis: main clinical sings
• Incubation period – 3-18 days
• acute beginning with the general symptoms of intoxication ( head ache, fever, pain in the muscles and joints, pain in swallowing, scratch in the throat
• exanthema – little maculas on the skin of the throat, axillary and inguinal regions, white dermographism
• hyperemia of the conjunctivas, scleritis, catarrh of the respiratory tracts, cough, hyperemia and edema of the face ( symptoms of the “ hood” and “ glasses” hyperemia and edema of the plants and palms ( symptoms of the “ gloves” and “ socks”)
• pain and borborygmus in the iliac parts, pain in the stomach, sickness, vomiting
• diarrhea – 2-3- time in day
• hepatitis, arthritis, splenomegaly, lymphadenopatia

Pseudotuberculosis


Pseudotuberculosis

Laboratory tests:• epidemiological anamnesis (use the dirty
fruits and vegetables, milk’s and meat’s products without the thermal treatment)
• blood (leucocytosis, neuthrophylosis, lymphopenia, eosinophilia) ad urinal tests
• bacteriologic tests of blood, urine, mucus, pus and faeces ( three times during first days on the height of the fever)
• serological tests – RHA during dynamic of disease

Rotavirus infection• Rotavirus infection is acute infection disease it is
caused by viruses from family of REOVIRUS, it is characterized by disorders from digestive tract and respiratory tracts.
• The sources of infection are ill person or virus carrier.
• Mechanism of transmission is fecal - oral
• Ways of transmission is contact-domestic – by food, water.
• Entry of infection is peptic (digestive) tract.
• Epidemiology’s features – winter - spring seasonality, high contagiously, early age of the children, especially – babies

Clinic classification
TYPE Severity Clinic course
Typical:
Gastroenteritis
Gastritis
Enteritis
Slight
Middle weight
Severe
Acute
Prolonged
Without
complications
With
complications
Atypical:
Low – grow
Sub clinical

BASIC CLINICAL SINGS OF TYPICAL FORM:
• Acute beginning with the febrile temperature and vomiting during 1-2days.
• Urges to defecate arrear suddenly, is accompanied by grumbling in the intestine, meteorism. Faeces are liquid, watery and foamy with light color,without pathological admixtures or with the mucus, with heavy smell, from 5 до20 times per days.
• Signs of exicosis.
• Respiratory syndrome is beginning from the 2-З days of illness without tendencyto growth.

FEATURES OF CLINIC COURSE (children of the early age):
• Beginning from the severe symptoms of intoxication (languor, adinamia, mottled skin ), cyanosis, cramps, and cardiovascular disorders.
• On 2-3 days of illness child has maximum of the exicosis of 2-3 degrees.
• Rotaviral infection can be connected with the bacterial affects of intestine. In this case pathological admixtures appear in the faeces (mucus, blood, and pus).
• Duration of illness may be to10-14 days.

SPECIFIC METHODS OF LABORATORY DIAGNOSTIC
Rotatest – RHA with erythrocytes, accumulated with the rotaviral antibodies. Express method- result during 2- 4 hours.
• Serological method – diagnostically titers is more then 1: 16
• IFA( IgM)
Related Documents