Dr. Peg Gray-Vickrey [email protected] 1 Acute Care: Delirium & Dementia National Conference for Nurse Practitioners October 7, 2016 Session 208 Dr. Peg Gray-Vickrey Objectives • Identify common causes and clinical presentation of dementia and delirium in the older adult. • Outline effective techniques for diagnosing dementia and delirium. • Examine evidence-based interventions for the older adult with dementia and delirium. Delirium • The term delirium is based on the Latin roots • de- away from • lira- furrow in field • ium- Latin for singular • This literally means “a going off the plowed track” “a madness”

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

Dr. Peg Gray-Vickrey [email protected] 1
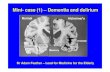
Acute Care: Delirium & Dementia
National Conference for Nurse Practitioners October 7, 2016 Session 208 Dr. Peg Gray-Vickrey
Objectives
• Identify common causes and clinical presentation of dementia and delirium in the older adult.
• Outline effective techniques for diagnosing dementia and delirium.
• Examine evidence-based interventions for the older adult with dementia and delirium.
Delirium
• The term delirium is based on the Latin roots
• de- away from
• lira- furrow in field
• ium- Latin for singular
• This literally means “a going off the plowed track” “a madness”

Dr. Peg Gray-Vickrey [email protected] 2
Delirium
• Delirium is a disturbance of the higher cortical centers that causes a reduced ability to focus, sustain, or shift attention. • Rapid and drastic decline of cognitive functioning
• Perceptual disturbances • Hallucinations
• Delusions
Prevalence
• Delirium is one of the most common syndromes that older adults develop • 30% of older adults • 1-2% in the community • 10-15% on general surgical unit
• 40-50% recovering from hip surgery • 50% CABG • 70-87% in the ICU (for older patients)
• 10-20% in general medical unit • Cardiac patients 11-46% • Orthopedic patients 12-51% • CVA 10-27%
• Up to 80% in near-death terminal cases
• 32-96% of elderly patients are discharged without complete resolution of symptoms • Common in Nursing Homes following hospital admission
Prevalence – Lack of Awareness
• Chart Reviews in most general hospitals will show that delirium is only mentioned 1-2% when published research suggests a prevalence of 30-50%
• Clinicians fail to recognize and address postoperative delirium in as many as 80% of the cases
Clark C. Preventing hospital acquired delirium. Health Leaders. 2015; April; 60-63.
Brooks P, Spillane J. Dick K, Stuart-Shor E. Developing a strategy to identify and treat older patients with postoperative delirium. AORN. 2014;99(2);256-275.

Dr. Peg Gray-Vickrey [email protected] 3
Pathophysiology
• Complex neuropsychiatric syndrome
• Often multifactorial in origin
• Likely affects multiple domains of the central nervous system
• Cause is unknown
• Current Theories:
• Deficiency in the cholinergic neurotransmitter system
• Melatonin abnormalities
• Neuronal damage secondary to oxidative stress or inflammation
• Inflammation induced perivascular edema leading to hypoxia and subsequent reduced synthesis of acetylcholine
• No known genetic markers for predisposition to delirium
Pathophysiology
• Neuroimaging of the brain reveals general disruption in higher cortical function with dysfunction in the following areas, particularly on the non-dominate side:
• Prefrontal cortex
• Subcortical structures
• Thalamus
• Basal ganglia
• Frontal and temporoparietal cortex
• Fusiform cortex
• Lingual gyri
• Functional neuroimaging (SPECT) has shown up to a 40% reduction in cerebral blood flow
Fong, TG, Bogardus, ST, Daftary, A, et.al. Cerebral perfusion changes in older delirious patients using 99mTc HMPAO SPECT. J Gerontol A Biol Sci Med Sci. 2006;61(12):1294-1299.
Outcome
• Symptoms typically resolve in 10-12 days
• May last up to 2-6 months
• Duration is dependent on underlying problem and management
• 44% of cases have 2 or more etiologies
• May progress to stupor, coma, seizures or death, especially if untreated
• Persistent delirium is associated with functional impairments of ADL’s and IADL’s
• Challenges of discharge planning

Dr. Peg Gray-Vickrey [email protected] 4
Outcome
• Elderly patients- 22-76% chance of dying during current hospitalization
• 6 month mortality- 23-33%
• 12 month mortality- 50%
• In the Long-Term Care Facility Post Discharge
• Average duration of delirium is 21 days
• 55% persisted for 1 month post discharge
• 25% persisted 3 months post discharge
Study on Prognosis
• London Health Sciences Center, Ontario
• 1235 patients over age 70
• 880 no delirium
• 355 delirium present (28.7%)
• Out of the 355 patients with delirium-69% had poor recovery
• 86 discharged to home
• 55 died
• 46 functional decline in ADL
• 215 discharged to LTC or rehab setting
• At 3 months-97 had poor recovery, 1 died, 136 permanently institutionalized
Dasgupta M & Brymer C. Prognosis of delirium in hospitalized elderly: Worse than we thought. Int J Geriatr
Psychiatry. 2014;29:497-505.
Clinical Features
• Prodrome
• Restlessness, irritability, sleeplessness
• Often missed
• Decreased Attention (hallmark) and Concentration
• Altered Arousal
• Reduced Clarity in the Environment
• Psychomotor Abnormalities
• Sleep-Wake Cycle Disturbances
• Disorientation to Time and Space
• Altered Perceptions Including Hallucinations, Delusions, and Misperceptions
• Grossly Distorted Judgement with Impaired Insight

Dr. Peg Gray-Vickrey [email protected] 5
Criteria for Identifying Delirium • The Diagnostic and Statistical Manual of Mental Disorders,
Fifth Edition, 2013 (DSM-5) diagnostic criteria for delirium is as follows:
• Disturbance in attention (ie, reduced ability to direct, focus, sustain, and shift attention) and awareness.
• Change in cognition (eg, memory deficit, disorientation, language disturbance, perceptual disturbance) that is not better accounted for by a preexisting, established, or evolving dementia.
• The disturbance develops over a short period (usually hours to days) and tends to fluctuate during the course of the day.
• There is evidence from the history, physical examination, or laboratory findings that the disturbance is caused by a direct physiologic consequence of a general medical condition, an intoxicating substance, medication use, or more than one cause.
Hypoactive vs. Hyperactive
• Hypoactive-24% of cases
• Common in older adults
• Lethargic
• Apathetic
• Withdrawn
• Somnolent
• Blunted affect
• Seem depressed or sedated
• Hyperactive-30% of cases
• Fearful
• Anxious
• Agitated
• Hyper-alert
• Hallucinations
• Unpredictable behavior
Hypoactive Delirium
• Associated with more complications
• Aspiration pneumonia
• Pressure ulcers
• Deep vein thrombosis

Dr. Peg Gray-Vickrey [email protected] 6
Mixed Delirium
• Most common type of delirium in adults under the age of 65
• Incidence of 46%
• Patients fluctuate between hypoactive and hyperactive states of delirium
Risk Factors
• Age
• Older Adults >75
• Young Children
• Vision or hearing impairment
• Decreased functional status
• Alcohol abuse
• Dementia-
• This is a leading risk factor, with 2/3rds of all cases of delirium occurring in individuals with dementia!
• Depression
• Abnormalities of serum sodium, potassium or glucose
Precipitating Risk Factors
• Hospital-related factors that contribute to delirium
• Physical restraints
• Postoperative pain
• Prolonged bed rest
• Sleep deprivation
• Surgery
• Medications
• Polypharmacy (3 or more medications)
• Complex cancer treatments
• High risk medications

Dr. Peg Gray-Vickrey [email protected] 7
High Risk Medications
• Anticholinergics
• Anticonvulsants
• Antiemetics
• Antihistamines
• Anti-Parkinson agents
• Antipsychotics
• Benzodiazepines
• Chemotherapy
• Digitalis
• Diuretics
• Histamine-2 Blockers--
cimetidine (Tagamet)
• Opioid analgesics
(especially with
impaired renal function)
• Steroids
Risk Factors continued
• Underlying Medical Conditions
• Infections
• Liver or renal failure
• CNS pathology
• Dementia
• Hip fracture
• Sudden withdrawal of alcohol or opioid analgesics
• Hypoxia
• Trauma
• Malnutrition
• Sleep deprivation
• Poorly managed pain
Risk Factors continued
• Environmental Factors • ICU Admission (and any new environment)
• Postoperative Status
• Sleep deprivation
• Sensory overload or deprivation

Dr. Peg Gray-Vickrey [email protected] 8
Delirium goes undetected in 72% of cases when routine monitoring is not in place!
Andrews L. Silva S, Kaplan S & Zimbro K. Delirium monitoring and patient outcomes in a general intensive care unit. AJCC.
2015;24(1): 48-56.
Assessment of Delirium
• Confusion Assessment Method (CAM) • Standardized and Validated-used in more than 4,000 studies
• https://www.healthcare.uiowa.edu/igec/tools/cognitive/CAM.pdf
• https://consultgeri.org/try-this/general-assessment/issue-13
• Must meet criteria 1&2 and either 3 or 4
1. Sudden onset with fluctuating course
2. Inattention
3. Disorganized thinking
4. Altered level of consciousness
CAM-Short Form
http://www.hospitalelderlifeprogram.org/delirium-instruments/confusion-assessment-method-long-cam/cam/

Dr. Peg Gray-Vickrey [email protected] 9
CAM Long Form
CAM-S Severity Score
• CAM-S Severity Score-quantify intensity of delirium
• http://www.hospitalelderlifeprogram.org/uploads/disclaimers/CAMS_instrument.pdf
Assessment of Delirium
• CAM-ICU-Updated in 2014 • http://www.icudelirium.org/docs/CAM_ICU_trai
ning.pdf • 1st step is Richmond Agitation-Sedation Scale
(RASS) for LOC • 2nd step is CAM-ICU
Using the CAM-ICU clip:
http://www.icudelirium.org/delirium/monitoring.html
Memories from the ICU clip:
http://www.icudelirium.org/testimonials.html

Dr. Peg Gray-Vickrey [email protected] 10
Workup
• History
• Physical, cognitive and neurological exam
• Electrolytes, CBC and differential, Renal and Liver function tests, fasting blood sugar
• Thyroid function studies
• EKG
• Oxygen saturation
• Urinalysis with sediment/culture
• Urine and blood drug screens
• Thiamine and vitamin B-12 levels
• Neuroimaging
Need for Family Education
“In many ways, delirium is an accepted but often undisclosed complication of inpatient care, because patients are unaware of the risks. Clinicians don’t think they can prevent it, so they don’t talk about it like they might regarding a risk of an infection or fall.”
Clark C. Preventing hospital acquired delirium. Health Leaders. (2015); April; 60-63.
Patient and Family Education
• Educate patient and family
• Not Crazy!
• Delirium educational brochure-Vanderbilt
• http://www.icudelirium.org/docs/delirium_education_brochure.pdf

Dr. Peg Gray-Vickrey [email protected] 11
Management of Delirium
• Identify and treat underlying etiology-single most effective treatment!
• Increase observation and monitoring
• Discontinue or minimize dosing of nonessential medications
• Monitor and assure safety of patient
Nonpharmacological Management • Environmental modifications
• Remove tubes as soon as possible
• Remove telemetry wires as soon as possible
• Limit use of restraints
• Reduce Noise
• Change lights based on the time of day
• Have visible 24 hour clocks
• Maintain good sleep hygiene
• Provide patients with personal belongings
• Maintain continuity of staff
• Use volunteer sitters
• Ensure glasses are clean and hearing aid is in working order
Nonpharmalogical Management • Pain
• Frequent pain assessment
• Try changes in position, massage and heat
• Sleep deprivation
• Back rubs
• Music therapy
• Lavender essential oils
• Limit noise at night
• Immobility and inactivity
• Begin early mobilization
• Daily ambulation
• Referral to physical therapy

Dr. Peg Gray-Vickrey [email protected] 12
Nonpharmalogical Management • Nutrition consult
• Fall risk assessment protocol
• Reorientation
• Music therapy
• Challenges in evidence-based practice
• 28 unique nonpharmalogical interventions have been used in studies
• A single intervention was tested in 5 studies
• Multiple interventions were tested in 12 studies
• The interventions associated with clinical benefit included
• Mobilization, Reorientation, Education of Nurses, Music Therapy
Pharmacological Management
• Medications to prevent delirium are not efficacious
• Treatment is indicated for acute agitation or when the safety of the patient or others is at risk
Pharmacological Management
• Conventional Antipsychotics • Block central dopamine receptors
• Reduces both the duration and severity of delirium by decreasing hallucinations, delusions, and disorganized thinking
• Haloperidol • A Cochrane review found that for short-term
use, a conventional antipsychotic is equally efficacious and safer than an atypical agent
• In the ICU, there is lack of evidence supporting pharmacological treatment for delirium

Dr. Peg Gray-Vickrey [email protected] 13
Pharmacological Management
• Haloperidol
• Low dose for patients over 65
• 2 mg by mouth twice a day or 0.25-0.5 mg every 4 hours until symptoms are under control . Do not exceed 10mg/24 hours
• 1 mg intravenous twice a day. Do not exceed 5 mg in 24 hours
Pharmacological Management
• Atypical Antipsychotics
• Blocks cortical serotonergic receptors
• Risperidone 0.5 mg by mouth twice a day
• Olanzapine 2.5 mg by mouth daily
• Quetiapine fumarate 25 mg by mouth at HS
• Ziprasidone
• Aripiprazole • Minimally sedating
• Negligible effect of QT interval prolongation
Second-Generation Antipsychotics • May reduce duration of delirium
• Lack of data on the effectiveness of the different subtypes of delirium
• Majority of data demonstrate no effect on significant outcomes such as length of stay and mortality
• Second-generation antipsychotics have fewer reported adverse effects when compared to haloperidol

Dr. Peg Gray-Vickrey [email protected] 14
Orthopedic Clients
• Findings suggest that antipsychotic reduce the incidence of postoperative delirium, at least in certain surgical populations with a baseline delirium risk of 18%.
Folk M, et. al. Do antipsychotics prevent postoperative delirium? A systematic review and meta analysis. Intl
J Geriatr Psychiatry. 2015; 30:333-344.
Oncology
• Haloperidol is considered the medication of choice to treat fear and hallucinations experienced by patients with delirium.
• Electrocardiograms should be monitored for lengthening of QT interval with ongoing haloperidol administration.
• If agitation or delirium cannot be controlled with routine pharmacologic and nonpharmacologic interventions, or if the patient is actively dying, palliative sedating drugs may be ordered
Clinical Practice Guidelines for Delirium in the ICU • American Association of Critical Care Medicine revised their
Clinical Practice Guidelines (originally published in 2002) in 2013
• Quality of evidence
• High (A)
• Moderate (B)
• Low/Very Low ©
• Strength of recommendation
• Strong (1)
• Weak (2)
Barr, J, Fraser, G, Puntillo, K. et. al. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the Intensive Care Unit. Critical Care Medicine, 2013;41(1): 263-306.

Dr. Peg Gray-Vickrey [email protected] 15
Clinical Practice Guidelines for Delirium in the ICU • Recommendations
• Recommend routine monitoring of delirium (B-1)
• CAM-ICU is a valid and reliable tool (A)
• Recommend early mobilization whenever feasible (B-1)
• No recommendation for using delirium prevention protocol-no compelling evidence (C)
• No recommendation on using a combined nonpharmacologic and pharmacologic prevention protocol in the ICU (C)
• Do not suggest that either haloperidol or atypical antipsychotics be administered to prevent delirium in the ICU (C-2)
• There is no published evidence that the treatment with haloperidol reduces the duration of delirium in the ICU (C)
• Atypical antipsychotics may reduce the duration of delirium (C)
Manage Common Complications of Delirium • Urinary Incontinence
• Pressure Ulcers
• Falls/Injury
• Sleep problems
• Malnutrition
• Aspiration
Dementia
• Progressive decline of mental faculties resulting in both memory impairment and a second area of cognitive deficiency
• Aphasia (communication)
• Apraxia (purposeful actions)
• Agnosia (recognize common objectives)
• Disturbance in executive functioning (reasoning, planning, problem solving)

Dr. Peg Gray-Vickrey [email protected] 16
Types of Dementia
• Alzheimer’s Disease
• Vascular dementia
• Dementia with Lewy bodies (DLB)
• Mixed dementia
• Parkinson's disease
• Frontotemporal dementia
• Creutzfeldt-Jakob disease
• Normal pressure hydrocephalus
• Huntington's disease
• Wernicke-Korsakoff Syndrome
Frontotemporal Dementia
Formerly known as Pick’s Disease
Frontotemporal Dementia
• Rare form of dementia
• 10-20% of all dementia cases
• Most common dementia in younger people
• Frontotemporal degenerations are inherited in about a third of all cases.
• Genetic counseling and testing is available
• Disease process that results in progressive damage to the anterior temporal and frontal loves of the brain
• Onset: Mid 50s to 60s
• Prognosis: 2 to 20 years (average 8)

Dr. Peg Gray-Vickrey [email protected] 17
Types of Frontotemporal Dementia
• Behavior variant frontotemporal dementia (bvFTD).
• prominent changes in personality, interpersonal relationships and conduct
• the nerve cell loss is most prominent in areas that control conduct, judgment, empathy and foresight, among other abilities.
• Primary progressive aphasia (PPA).
• affects language skills, speaking, writing and comprehension.
• In semantic variant of PPA, individuals lose the ability to understand or formulate words in a spoken sentence.
• In nonfluent/agrammatic variant of PPA, a person’s speaking is very hesitant, labored or ungrammatical.
Clinical Presentation
• Disease of behavior and language dysfunction
• Wide variation of symptoms
• Increasing inappropriate social behavior
• Withdrawn
• Disinhibited
• Decreased self awareness
• Repetitive behaviors
• Distractibility
• Poor financial judgment
• Emotional blunting
• Lack of motivation
• Abrupt and frequent mood changes
Clinical Presentation
• Language changes
• Expression of language
• Hesitant speech
• Talks less
• Retains the meaning of words
• Word Meaning
• Produces fluent speech but doesn’t understand words or recognize objectives

Dr. Peg Gray-Vickrey [email protected] 18
Clinical Presentation
• Movement
• Decreased movement on one side of the body
• Muscle rigidity
• Problems with gait and balance
Frontotemporal Dementia
• Frontotemporal atrophy
• Pick Cells(ballooned neurons)
Treatment
• There in no FDA approve medication or treatment for frontotemporal dementia.
• Treatment is often based on medications that reduce agitation, irritability and/or depression.
• FTD inevitably gets worse over time and the speed of decline differs from person to person.
• Individuals with FTD often have muscle weakness and coordination problems, leading to immobility and causing problems with swallowing, chewing, and controlling bladder and/or bowels.

Dr. Peg Gray-Vickrey [email protected] 19
Vascular Dementia
Vascular Dementia
• Causes by brain damage from impaired blood flow to brain
• Second most common form of dementia
• 10-30% of all cases of dementia
• Japan-50% of all cases of dementia
• Vascular brain changes often coexist with other types of dementia
• Begins between ages of 40-70
• 5 year survival rate-39%
• 1 year post stroke- 25% dementia rate
• 5 years post stroke-39% dementia rate
Risk Factors
• Advancing age (80s to 90s)
• History of MI or Stroke
• Atherosclerosis
• High Cholesterol
• High Blood Pressure
• Diabetes
• Smoking
• Atrial Fibrillation

Dr. Peg Gray-Vickrey [email protected] 20
Presentation of Vascular Dementia • Symptoms vary depending on severity of the blood vessel
damage and the portion of brain that has impaired blood flow
• Memory loss may or may not be a significant symptom depending on the specific brain areas where blood flow is reduced.
• Post-stroke dementia (sudden onset)
• Widespread small vessel disease
• Common early signs include impaired planning and judgment; uncontrolled laughing and crying; declining ability to pay attention; impaired function in social situations; and difficulty finding the right words.
Presentation of Vascular Dementia • Trouble concentrating
• Inability to organize thoughts
• Difficulty deciding what to do
• Restlessness
• Aphasia
• Incontinence
• Depression
Treatment
• The FDA has not approved any drugs specifically to treat symptoms of vascular dementia
• Controlling risk factors that may increase the likelihood of further damage to the brain's blood vessels is the most important treatment strategy.

Dr. Peg Gray-Vickrey [email protected] 21
Alzheimer’s disease
Epidemiology of Alzheimer’s Disease • 360,000 new cases annually
• Up to 50% of cases are not picked up by primary care clinicians
• Dementia patients have a shortened life span—average survival 4-8 years from diagnosis. But can live as long as 20 yrs.
• Prevalence increases with age • Up to 50% >85 years-old
• 5.4 million Americans currently have AD
Amyloid Plaques and Neurofibrillary Tangles

Dr. Peg Gray-Vickrey [email protected] 22
Preclinical AD
• Alzheimer’s disease begins in the entorhinal cortex-(connected to the hippocampus-essential to the formation of short and long term memories)
• Affected regions begin to atrophy 10-20 years before any identifiable signs and symptoms occur.
• Memory loss is the first visible sign
• Memory loss primary symptom of Mild Cognitive Impairment (MCI)
Mild AD (early stage)
• Increased number of plaques and tangles first damage areas of brain that control memory, language and reasoning
• Disease begins to affect cerebral cortex
• Clinical diagnosis of AD is usually made during this stage
• Memory loss
• Confusion (place)
• Taking longer to accomplish tasks
• Trouble handling money
• Poor judgment
• Loss of spontaneity and initiative
• Mood and personality changes
• Increased anxiety

Dr. Peg Gray-Vickrey [email protected] 23
Moderate AD (middle-stage)
• AD damage has spread to areas of cerebral cortex that control language, reasoning, sensory processing, and conscious thought
• Affected regions continue to atrophy
• Behavior problems occur (restlessness, agitation, anxiety, tearfulness, wandering)
• Increased memory loss
• Short attention span
• Problems recognizing family and friends
• Difficulty with language (reading writing and working with numbers
• Inability to learn new things
• Difficulty organizing thoughts and thinking logically
Severe AD (late stage)
• Tangles and plaques are widespread throughout the brain
• Further atrophy of cerebral cortex
• Most individuals with AD dies from other illnesses, especially aspiration pneumonia
• Most patients are completely dependent on others for care
• Loss of communication-groaning, moaning or grunting
• Loss of recognition
• Loss of sense of self
• Weight loss
• Seizures, infection
• Lack of bowel and bladder control

Dr. Peg Gray-Vickrey [email protected] 24
Severe AD
Changes in PET Scans with Age
20 year-old 80 year-old
Changes in PET Scans with AD
Normal PET Scan PET Scan in AD

Dr. Peg Gray-Vickrey [email protected] 25
Early Diagnosis
• It is possible to delay the onset and progression of AD and related disorders by six or more years. • Preventative strategies • Early diagnosis • Early treatment
• Preventative therapy delays the onset of AD by 3.5 years!
• Early detection and treatment of AD delays progression by at least 2.8 years!
Diagnostic Evaluation
• Definitive diagnosis of Alzheimer’s Disease is only possible during a brain biopsy or during an autopsy (when plaques and tangles can be seen)
• A comprehensive workup is accurate in diagnosis 90% of the time
Diagnostic Evaluation
• Detailed patient history
• Family insights on how behavior and personality have changed
• Physical examination and thorough neurological examination
• Laboratory tests
• Computerized tomography or magnetic resonance imaging test
• Comprehensive neuropsychological testing

Dr. Peg Gray-Vickrey [email protected] 26
Diagnostic Evaluation
• Folstein Mini-Mental State Examination (MMSE)
• Alzheimer’s Disease Assessment Scale-
• Cognitive subscale (ADAS-cog)
• Functional Assessment Questionnaire
• Dementia Rating Scale
• Cohen-Mansfield Agitation Inventory
• Clock Drawing Test
Criteria for “Probable” Alzheimer’s Disease • Dementia confirmed by clinical and
neuropsychological examination
• Problems in at least two areas of cognitive functioning
• Progressive worsening of memory and other mental functioning
• No disturbances of consciousness
• Symptoms beginning between ages of 40-90
• No other disorders that might account for the dementia
Update to the 1984 Criteria
• 2011-Workgroup from National Institute on Aging and Alzheimer’s Association
• Tasked to revise the 1984 criteria for AD dementia
• Develop criteria that would be flexible and useful for practitioners and researchers
• Currently being used for research only

Dr. Peg Gray-Vickrey [email protected] 27
Classification Criteria for AD
• Probable AD Dementia
• Meets criteria for dementia
• Insidious onset over months to years
• Clear-cut history of worsening cognition
• Amnestic presentation (learning and memory)
• Nonamnestic presentation (word-finding, inability to recognize objects, impaired reasoning and judgment)
Classification Criteria for AD
• Probable AD Dementia with Increased Level of Certainty
• Documented decline by neuropsychological evaluation or standardized mental status examinations
• Carrier of a causative genetic mutation
• APP, PSEN1, PSEN2
Classification Criteria for AD
• Probable AD Dementia with Evidence of AD Pathophysiological Process
• Biomarkers of brain amyloid-beta in CSF are low
• Biomarkers of neuronal degeneration or injury
• Elevated CSF tau
• Decreased fluorodeoxyglucose uptake on PET
• Atrophy of brain on MRI

Dr. Peg Gray-Vickrey [email protected] 28
What treatments are available? • One of the biggest stumbling blocks in developing effective
drug therapy for Alzheimer's disease has been the lack of a comprehensive hypothesis that explains the mechanism behind all of the histopathological changes seen in patients suffering from Alzheimer's disease.
FDA Approved Medications
• Cholinesterase Inhibitors
• donepezil (Aricept)
• Used for all stages of Alzheimer’s Disease
• rivastigmine (Exelon)
• Approved for mild to moderate stages of Alzheimer’s Disease
• galantamine (Razadyne)
• Approved for mild to moderate stages of Alzheimer’s Disease
Clinical Expectations from Cholinesterase Inhibitor Therapy • Primary Benefits • Maintain current level of daily functioning
• “No change” means therapy is helping
• Maintain current level of cognition
• Decrease emergence of behavioral and psychological disturbances
• Secondary Benefits • Decrease caregiver burden and distress
• Decrease overall health-care cost
• Delay institutionalization

Dr. Peg Gray-Vickrey [email protected] 29
FDA Approved Medications
• N-methyl-D-aspartate (NMDA) Receptor Antagonists
• memantine (Namenda)
• Memantine is prescribed to improve memory, attention, reason, language and the ability to perform simple tasks.
• Works best in moderate to advanced AD
• Combination effect with donepezil (Namzaric)
Management of Dementia
• Patient Education
• Reducing excess disability
• Address safety concerns
• Address ability to live independently
• Address decision making capacity (medical and financial decisions)
• Family support
• Screen for abuse and neglect
Management of Dementia
• Symptomatic treatment with a cholinesterase inhibitor for AD only. • May make Frontotemporal Dementia symptoms
worse.
• Treat medical comorbidity with intensity appropriate to stage of disease and patient wishes
• Treat psychiatric comorbidity with non-pharmacological interventions, and if necessary, pharmacological interventions
• Counseling regarding participation in trials • Address End-of-Life issues

Dr. Peg Gray-Vickrey [email protected] 30
Maintaining Cognitive Health
Preventative Care
• Research focus is now turning to prevention trials • A number of studies are underway to test the effectiveness of
various therapies in people without symptoms or with MCI
• Prevention trials are the most costly of all research projects
• Most research is preliminary
• Focus on developing a vaccine
Preserving Healthy Brain Aging
• Omega-3 fatty acids
• Fatty, cold-water fish (tuna, salmon, mackerel)
• Decrease inflammation and help with immunity
• 1-2 capsules, 1-3 times daily
• Curcumin (tumeric/turmeric)
• Green tea—antioxidant, anti-inflammatory and immune effects

Dr. Peg Gray-Vickrey [email protected] 31
Preserving Healthy Brain Aging • Cardiovascular risk factors for dementia include
• Diabetes
• Heart Disease
• High Cholesterol
Preserving Healthy Brain Aging
• Decreasing levels of stress
• Maintain close social ties with family, friends and the community
• Music Therapy– calming music may reduce wandering and restlessness, boost brain chemicals, and improve behavior
Preserving Healthy Brain Aging
• Regular exercise and physical activity
• Aerobic exercise
• Dancing
• Walking
• Swimming

Dr. Peg Gray-Vickrey [email protected] 32
Preserving Healthy Brain Aging
• Maintain high level of intellectually stimulating activities • Reading
• Board games
• Playing a musical instrument
• Playing puzzle games
• Going to museums
References • Acee, A. Type 2 diabetes and vascular dementia: Assessment and clinical strategies of care.
MedSurg Nursing. 2012; 21(6): 349-353.
• The American Psychiatric Association Practice Guideline on the Use of Antipsychotics to Treat Agitation or Psychosis in Patients with Dementia. (2016). American Psychiatric Association Arlington, VA
• Andrews L, Silva S, Kaplan S, Zimbro K. Delirium monitoring and patient outcomes in a general intensive care unit. AJCC. 2015;24(1):48-56.
• Barr, J, Fraser, G, Puntillo, K. et. al. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the Intensive Care Unit. Critical Care Medicine, 2013;41(1): 263-306.
• Bathula M, Gonzales J. The pharmacologic treatment of intensive care unit delirium: A systematic review. Annals of Pharmacotherapy. 2013;47(9):1168-1174.
• Bond SM. Delirium at home: Strategies for home health clinicians. Home Healthcare Nurse. 2009;27(1):24-34.
• Brooks P, Spillane J. Dick K, Stuart-Shor E. Developing a strategy to identify and treat older patients with postoperative delirium. AORN. 2014;99(2);256-275.
• Burock J. Delirium in the Elderly. Medicine and Health. 2012;95(7):214-215.
• Clark C. Preventing hospital acquired delirium. Health Leaders. 2015; April; 60-63.
• Dasgupta M, Brymer C. Prognosis of delirium in hospitalized elderly: Worse than we thought. Int J Geriatr Psychiatry. 2014;29:497-505.
• Derby S. Assessment and management of delirium in the older adult with cancer. Clinical Journal of Oncology Nursing. 2011;15(3):247-250.
References • DeSimone EM, Viereck L. Alzheimer’s disease: Increasing numbers, but no cure. U.S. Pharmacist.
2011;36(1):26-42.
• Faught D. Delirium: The nurse’s role in prevention, diagnosis, and treatment. MedSurg Nursing. 2014;23(5):301-305.
• Fong, TG, Bogardus, ST, Daftary, A, et.al. Cerebral perfusion changes in older delirious patients using 99mTc HMPAO SPECT. J Gerontol A Biol Sci Med Sci. 2006;61(12):1294-1299.
• Folk M, et. al. Do antipsychotics prevent postoperative delirium? A systematic review and meta analysis. Intl J Geriatr Psychiatry. 2015; 30:333-344.
• Gagliardi JP. Differentiating among depression, delirium, and dementia in elderly patients. Virtual Mentor. 2008;10(6):383-388.
• Gion T, Leclaire-Thoma A. Delirium in the brain-injured patient. Rehabilitation Nursing. 2014;39:232-239.
• Harrison-Dening, K. Dementia: diagnosis and early interventions. British Journal of Neuroscience Nursing. 2013; 9(3): 131-137.
• Hollingworth P. Harold D, Jones L, Owen MJ, Williams J. Alzheimer’s disease genetics: Current knowledge and future challenges. International Journal of Geriatric Psychiatry. 2011;26:793-802.
• Holroyd-Leduc JM, Khandwala F, Sink KM. How can delirium best be prevented and managed in older patients in hospital? CMAJ. 2010; 182(5); 465-470.
• Holzer, S, Warner, JP, Iliffe, S. Diagnosis and management of the patient with suspected dementia in primary care. Drugs Aging. 2013; 30: 667-676.
• Inouye S, Kosar CM, Tommet D. et al. The CAM-S: Development and validation of a new scoring system for delirium severity in 2 cohorts. Annals of Internal Medicine. 2014;160(8):526-533.

Dr. Peg Gray-Vickrey [email protected] 33
References • Marcantonio ER, Bergmann MA, Kiely DK, Orav EJ, Jones RN. Randomized trial of a delirium
abatement program for postacute skilled nursing facilities. JAGS. 2010;58(6):1019-1026.
• Mergenhagen, KA, Arif S. Delirium in the elderly: Medications, causes, and treatment. U.S. Pharmacist. 2008.
• Miller MO. Evaluation and management of delirium in hospitalized older patients. American Family Physician. 2008;78(11):1265-1270.
• Mittal V, Williamson D, Thomas J, Tampi RR. Delirium in the elderly: A comprehensive review. American Journal of Alzheimer’s Disease and other Dementias. 2011;26(2):97-109.
• Tiedeman M, Kim C, Flurie R, Korch-Black K, Brandt NJ. Alzheimer’s disease: Current treatment options and future developments. Formulary. 2011;46:268-284.
• Rivosecchi R. Smithburger P. Svec A. Campbell S. Kane-Gill S. Nonpharmacological interventions to prevent delirium: An evidence-based systematic review. Critical Care Nurse. 2015;35(1):39-51.
• Reus, VI, Fochtmann, LJ, Eyler, AE et. al. The American Psychiatric Association practice guideline on the use of antipsychotics to treat agitation or psychosis in patients with dementia. Am J Psychiatry 2016; 173:5:543-546.
• Qaseem A, Snow V, Cross JT, Forciea MA, Hopkins R, Shekelle P, et al. Current Pharmacologic Treatment of Dementia: A Clinical Practice Guideline from the American College of Physicians and the American Academy of Family Physicians. Ann Intern Med. 2008;148:370-378. (reaffirmed in 2013)
• Wierenga CA, Bondi MW. Dementia and Alzheimer’s disease: What we know now. Generations. 2011;35(2):37-45.
• Weisenfeld L. Delirium: the ADVISE approach and tips from the frontlines. Geriatrics. 2008;63(5):28-31.
Related Documents