APPROPRIATE USE CRITERIA ACC/AATS/AHA/ASE/ASNC/SCAI/ SCCT/STS 2016 Appropriate Use Criteria for Coronary Revascularization in Patients With Acute Coronary Syndromes A Report of the American College of Cardiology Appropriate Use Criteria Task Force, American Association for Thoracic Surgery, American Heart Association, American Society of Echocardiography, American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and the Society of Thoracic Surgeons Coronary Revascularization Writing Group Manesh R. Patel, MD, FACC, FAHA, FSCAI, Chair John H. Calhoon, MD Gregory J. Dehmer, MD, MACC, MSCAI, FACP, FAHA* James Aaron Grantham, MD, FACC Thomas M. Maddox, MD, MSC, FACC, FAHA David J. Maron, MD, FACC, FAHA Peter K. Smith, MD, FACCy *Society for Cardiovascular Angiography and Interventions Representative. ySociety of Thoracic Surgeons Representative. Rating Panel Michael J. Wolk, MD, MACC, Moderator Manesh R. Patel, MD, FACC, FAHA, FSCAI, Writing Group Liaison Gregory J. Dehmer, MD, MACC, MSCAI, FACP, FAHA, Writing Group Liaison* Peter K. Smith, MD, FACC, Writing Group Liaison James C. Blankenship, MD, MACCz Alfred A. Bove, MD, PHD, MACCz Steven M. Bradley, MDx Larry S. Dean, MD, FACC, FSCAI* Peter L. Duffy, MD, FACC, FSCAI* T. Bruce Ferguson, JR, MD, FACCz Frederick L. Grover, MD, FACCz Robert A. Guyton, MD, FACCk Mark A. Hlatky, MD, FACCz Harold L. Lazar, MD, FACC{ Vera H. Rigolin, MD, FACCz Geoffrey A. Rose, MD, FACC, FASE# Richard J. Shemin, MD, FACCk Jacqueline E. Tamis-Holland, MD, FACCz Carl L. Tommaso, MD, FACC, FSCAI* L. Samuel Wann, MD, MACC** John B. Wong, MDz zAmerican College of Cardiology Representative. xAmerican Heart Association Representative. kSociety of Thoracic Surgeons Representative. {American Association for Thoracic Surgery Representative. #American Society of Echocardiography Representative. **American Society of Nuclear Cardiology Representative. This document was approved by the American College of Cardiology Board of Trustees in October 2016. The American College of Cardiology requests that this document be cited as follows: Patel MR, Calhoon JH, Dehmer GJ, Grantham JA, Maddox TM, Maron DJ, Smith PK. ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2016 appropriate use criteria for coronary revascularization in patients with acute coronary syndromes: a report of the American College of Cardiology Appropriate Use Criteria Task Force, American Association for Thoracic Surgery, American Heart Association, American Society of Echocardiography, American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and the Society of Thoracic Surgeons. J Am Coll Cardiol 2016;XX:xxx–xx. This document has been reprinted in Catheterization and Cardiovascular Interventions and the Journal of Nuclear Cardiology. Copies: This document is available on the World Wide Web site of the American College of Cardiology (www.acc.org). For copies of this document, please contact Elsevier Reprint Department, fax (212) 633-3820 or e-mail [email protected]. Permissions: Multiple copies, modification, alteration, enhancement, and/or distribution of this document are not permitted without the express permission of the American College of Cardiology. Please contact [email protected]. JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. -, NO. -, 2016 ª 2016 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION PUBLISHED BY ELSEVIER ISSN 0735-1097/$36.00 http://dx.doi.org/10.1016/j.jacc.2016.10.034

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript
-
J O U R N A L O F T H E A M E R I C A N C O L L E G E O F C A R D I O L O G Y V O L . - , N O . - , 2 0 1 6
ª 2 0 1 6 B Y T H E AM E R I C A N C O L L E G E O F C A R D I O L O G Y F O U N D A T I O N
P U B L I S H E D B Y E L S E V I E R
I S S N 0 7 3 5 - 1 0 9 7 / $ 3 6 . 0 0
h t t p : / / d x . d o i . o r g / 1 0 . 1 0 1 6 / j . j a c c . 2 0 1 6 . 1 0 . 0 3 4
APPROPRIATE USE CRITERIA
ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2016 Appropriate Use
Criteria for Coronary Revascularization inPatients With Acute Coronary Syndromes
A Report of the American College of Cardiology Appropriate Use Criteria Task Force, AmericanAssociation for Thoracic Surgery, American Heart Association, American Society of Echocardiography,American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions,Society of Cardiovascular Computed Tomography, and the Society of Thoracic Surgeons
CoronaryRevascularizationWriting Group
Manesh R. Patel, MD, FACC, FAHA, FSCAI, Cha
John H. Calhoon, MD
ir
Gregory J. Dehmer, MD, MACC, MSCAI, FACP, FAHA*James Aaron Grantham, MD, FACCThomas M. Maddox, MD, MSC, FACC, FAHA
This document was approved by the American College of Cardiology Boa
The American College of Cardiology requests that this document be cited
Maron DJ, Smith PK. ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2016 appr
coronary syndromes: a report of the American College of Cardiology Appro
American Heart Association, American Society of Echocardiography, Americ
and Interventions, Society of Cardiovascular Computed Tomography, and th
This document has been reprinted in Catheterization and Cardiovascular
Copies: This document is available on the World Wide Web site of the Am
please contact Elsevier Reprint Department, fax (212) 633-3820 or e-mail rep
Permissions: Multiple copies, modification, alteration, enhancement, and
permission of the American College of Cardiology. Please contact healthper
David J. Maron, MD, FACC, FAHAPeter K. Smith, MD, FACCy
*Society for Cardiovascular Angiography and Interventions
Representative. ySociety of Thoracic Surgeons Representative.
Rating Panel
Michael J. Wolk, MD, MACC, Moderator
Manesh R. Patel, MD, FACC, FAHA, FSCAI,Writing Group LiaisonGregory J. Dehmer, MD, MACC, MSCAI, FACP, FAHA,Writing Group Liaison*Peter K. Smith, MD, FACC, Writing Group Liaison
James C. Blankenship, MD, MACCz
Alfred A. Bove, MD, PHD, MACCzSteven M. Bradley, MDxLarry S. Dean, MD, FACC, FSCAI*Peter L. Duffy, MD, FACC, FSCAI*T. Bruce Ferguson, JR, MD, FACCzFrederick L. Grover, MD, FACCzRobert A. Guyton, MD, FACCk
Mark A. Hlatky, MD, FACCzHarold L. Lazar, MD, FACC{Vera H. Rigolin, MD, FACCzGeoffrey A. Rose, MD, FACC, FASE#Richard J. Shemin, MD, FACCkJacqueline E. Tamis-Holland, MD, FACCzCarl L. Tommaso, MD, FACC, FSCAI*L. Samuel Wann, MD, MACC**John B. Wong, MDz
zAmerican College of Cardiology Representative. xAmerican HeartAssociation Representative. kSociety of Thoracic Surgeons Representative.{American Association for Thoracic Surgery Representative. #AmericanSociety of Echocardiography Representative. **American Society of
Nuclear Cardiology Representative.
rd of Trustees in October 2016.
as follows: Patel MR, Calhoon JH, Dehmer GJ, Grantham JA, Maddox TM,
opriate use criteria for coronary revascularization in patients with acute
priate Use Criteria Task Force, American Association for Thoracic Surgery,
an Society of Nuclear Cardiology, Society for Cardiovascular Angiography
e Society of Thoracic Surgeons. J Am Coll Cardiol 2016;XX:xxx–xx.
Interventions and the Journal of Nuclear Cardiology.
erican College of Cardiology (www.acc.org). For copies of this document,
/or distribution of this document are not permitted without the express
http://www.acc.orgmailto:[email protected]:[email protected]://dx.doi.org/10.1016/j.jacc.2016.10.034
-
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-2
Appropriate UseCriteria TaskForce
Gregory J. Dehmer, MD, MACC, Co-Chair
John U. Doherty, MD, FACC, Co-Chair
Steven R. Bailey, MD, FACC, FSCAI, FAHANicole M. Bhave, MD, FACCAlan S. Brown, MD, FACCyyStacie L. Daugherty, MD, FACCMilind Y. Desai, MBBS, FACCClaire S. Duvernoy, MD, FACCLinda D. Gillam, MD, FACCRobert C. Hendel, MD, FACC, FAHAyyChristopher M. Kramer, MD, FACC, FAHAzzBruce D. Lindsay, MD, FACCyy
Warren J. Manning, MD, FACCManesh R. Patel, MD, FACC, FAHAxxRitu Sachdeva, MBBS, FACCL. Samuel Wann, MD, MACCyyDavid E. Winchester, MD, FACCMichael J. Wolk, MD, MACCyyJoseph M. Allen, MA
yyFormer Task Force member, current member during the writingeffort. zzFormer Task Force Co-Chair, current Co-Chair during thewriting effort. xxFormer Task Force Chair, current Chair during thewriting effort.
TABLE OF CONTENTS
ABSTRACT . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
PREFACE . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
1. INTRODUCTION . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
2. METHODS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Indication Development . . . . . . . . . . . . . . . . . . . . . . . . . -
Scope of Indications . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
3. ASSUMPTIONS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
General Assumptions . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
4. DEFINITIONS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Indication . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Cardiac Risk Factor Modification and AntianginalMedical Therapy . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Culprit Stenosis . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Symptoms of Myocardial Ischemia . . . . . . . . . . . . . . . . . -
Unstable Angina . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Stress Testing and Risk of Findings on NoninvasiveTesting . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
The Role of Patient Preference in the AUC . . . . . . . . . . -
Specific Acute Coronary Syndromes . . . . . . . . . . . . . . . . -
5. ABBREVIATIONS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
6. CORONARY REVASCULARIZATION IN PATIENTS
WITH ACS: AUC (BY INDICATION) . . . . . . . . . . . . . . . -
Table 1.1 STEMI – Immediate Revascularization byPCI . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Table 1.2 STEMI – Initial Treatment by FibrinolyticTherapy . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
Table 1.3 STEMI – Revascularization of NonculpritArtery During the Initial Hospitalization . . . . . . . . . . . . -
Table 1.4 NSTEMI/Unstable Angina . . . . . . . . . . . . . . . . -
7. DISCUSSION . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
REFERENCES . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . -
APPENDIX A
Appropriate Use Criteria for CoronaryRevascularization in Patients With Acute CoronarySyndromes: Participants . . . . . . . . . . . . . . . . . . . . . . . . . -
APPENDIX B
Relationships With Industry and Other Entities . . . . . . -
ABSTRACT
The American College of Cardiology, Society for Cardiovas-cular Angiography and Interventions, Society of ThoracicSurgeons, and American Association for Thoracic Surgery,along with key specialty and subspecialty societies, havecompleted a 2-part revision of the appropriate use criteria(AUC) for coronary revascularization. In prior coronaryrevascularization AUC documents, indications for revascu-larization in acute coronary syndromes (ACS) and stableischemic heart disease were combined into 1 document. Toaddress the expanding clinical indications for coronaryrevascularization, and in an effort to align the subjectmatterwith the most current American College of Cardiology/American Heart Association guidelines, the new AUC forcoronary artery revascularization were separated into 2documents addressing ACS and stable ischemic heart dis-ease individually. This document presents the AUC for ACS.
Clinical scenarios were developed to mimic patientpresentations encountered in everyday practice and
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
3
included information on symptom status, presence ofclinical instability or ongoing ischemic symptoms, priorreperfusion therapy, risk level as assessed by noninvasivetesting, fractional flow reserve testing, and coronaryanatomy. This update provides a reassessment of clinicalscenarios that the writing group felt to be affected bysignificant changes in the medical literature or gaps fromprior criteria. The methodology used in this update issimilar to the initial document but employs the recentmodifications in the methods for developing AUC, mostnotably, alterations in the nomenclature for appropriateuse categorization.
A separate, independent rating panel scored theclinical scenarios on a scale of 1 to 9. Scores of 7 to 9indicate that revascularization is considered appropriatefor the clinical scenario presented. Scores of 1 to 3indicate that revascularization is considered rarelyappropriate for the clinical scenario, whereas scores inthe mid-range (4 to 6) indicate that coronary revascu-larization may be appropriate for the clinical scenario.Seventeen clinical scenarios were developed by awriting committee and scored by the rating panel: 10were identified as appropriate, 6 as may be appropriate,and 1 as rarely appropriate.
As seen with the prior coronary revascularization AUC,revascularization in clinical scenarios with ST-segmentelevation myocardial infarction and non–ST-segmentelevation myocardial infarction were considered appro-priate. Likewise, clinical scenarios with unstable anginaand intermediate- or high-risk features were deemedappropriate. Additionally, the management of nonculpritartery disease and the timing of revascularization arenow also rated. The primary objective of the AUC is toprovide a framework for the assessment of practice pat-terns that will hopefully improve physician decisionmaking.
PREFACE
The American College of Cardiology (ACC), in collabo-ration with the Society for Cardiovascular Angiographyand Interventions, Society for Thoracic Surgeons,American Association for Thoracic Surgery, and othersocieties, developed and published the first version ofthe appropriate use criteria (AUC) for coronary revas-cularization in 2009, with the last update in 2012. TheAUC are an effort to assist clinicians in the rational useof coronary revascularization in common clinical sce-narios found in everyday practice. The new AUC forcoronary revascularization was developed as separatedocuments for acute coronary syndromes (ACS) andstable ischemic heart disease (SIHD). This was done toaddress the expanding clinical indications for coronaryrevascularization, include new literature published since
the last update, and align the subject matter with theACC/American Heart Association guidelines An addi-tional goal was to address several of the shortcomingsof the initial document that became evident as experi-ence with the use of the AUC accumulated in clinicalpractice.
The publication of AUC reflects 1 of several ongoingefforts by the ACC and its partners to assist clinicians whoare caring for patients with cardiovascular diseases and insupport of high-quality cardiovascular care. The ACC/American Heart Association clinical practice guidelinesprovide a foundation for summarizing evidence-basedcardiovascular care and, when evidence is lacking, pro-vide expert consensus opinion that is approved in reviewby the ACC and American Heart Association. However, inmany areas, variability remains in the use of cardiovas-cular procedures, raising questions of over- or under-use.The AUC provide a practical standard upon which toassess and better understand variability.
We are grateful to the writing committee for thedevelopment of the overall structure of the document andclinical scenarios and to the rating panel, a professionalgroup with a wide range of skills and insights, for theirthoughtful deliberation of the merits of coronary revas-cularization for various clinical scenarios. We would alsolike to thank the parent AUC Task Force and the ACC staff,Joseph Allen, Leah White, and specifically Maria Velas-quez, for their skilled support in the generation of thisdocument.
Manesh R. Patel, MD, FACCChair, Coronary Revascularization Writing Group
Chair, Appropriate Use Criteria Task Force
Michael J. Wolk, MD, MACCModerator, Appropriate Use Criteria Task Force
1. INTRODUCTION
In a continuing effort to provide information to patients,physicians, and policy makers, the Appropriate Use TaskForce approved this revision of the 2012 coronary revas-cularization AUC (1). Since publication of the 2012 AUCdocument, new guidelines for ST-segment elevationmyocardial infarction (STEMI) (2) and non–ST-segmentelevation myocardial infarction (NSTEMI)/unstableangina (3) have been published with additional focusedupdates of the SIHD guideline and a combined focusedupdate of the percutaneous coronary intervention (PCI)and STEMI guideline (4,5). New clinical trials have beenpublished extending the knowledge and evidence aroundcoronary revascularization, including trials that challengeearlier recommendations about the timing of nonculpritvessel PCI in the setting of STEMI (6–8). Additionalstudies related to coronary artery bypass graft surgery,medical therapy, and diagnostic technologies such as
-
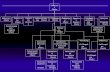
FIGURE 1 AUC Development Process
Indi
catio
n D
evel
opm
ent
App
ropr
iate
ness
D
eter
min
atio
nV
alid
atio
n D
aD
eter
min
atio
nDevelop lissumption
Prow
AA
ist of indicns, and def
ospective with Clinic
% Use AppropriaAppropria
Appro
cations, finitions
R
I
Compariscal Record
that is te, May B
ate, Rarelyopriate
Review Paprovi
WritingIn
Rating PIndication
1st roun
Appro(7–9) Ap(4–6) M(1–3) Ra
son ds
e y
anel >30 mide feedba
g Group Rndications
Panel Ratens in Two R
d – No Int
opriate Usppropriateay Be Apparely Appr
members ack
Revises
es the Rounds
teraction
se Score epropriate ropriate
LiteraturGuidelin
ProD
Increa
re Review ne Mappin
spective CDecision A
se Approp
and ng
Clinical Aids
priate Use
AUC ¼ appropriate use criteria.
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-4
fractional flow reserve (FFR) have emerged as well asanalyses from The National Cardiovascular Data Registry(NCDR) on the existing AUC that provide insights intopractice patterns, clinical scenarios, and patient featuresnot previously addressed (9–11).
In an effort to make the AUC usable, meaningful, and asup-to-date as possible, the writing group was asked todevelop AUC specifically for coronary revascularization inACS including STEMI to coincide with the recently pub-lished focused update of the STEMI guidelines (5). A newseparate AUC document specific to SIHD is under prepa-ration and will be forthcoming. The goal of the writinggroup was to develop clinical indications (scenarios) thatreflect typical situations encountered in everyday prac-tice, which are then classified by a separate rating panel
using methodology previously described in detail (12)(Figure 1). In addition, step-by-step flow charts are pro-vided to help use the criteria.
2. METHODS
Indication Development
A multidisciplinary writing group consisting of cardio-vascular health outcomes researchers, interventionalcardiologists, cardiothoracic surgeons, and general car-diologists was convened to review and revise the coro-nary revascularization AUC.
The revascularization AUC are on the basis of our cur-rent understanding of procedure outcomes plus the po-tential patient benefits and risks of the revascularization
-
Sco
Sco
Sco
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
5
strategies examined. The AUC are developed to identifymany of the common clinical scenarios encountered inpractice, but cannot possibly include every conceivablepatient presentation. (In this document, the phrase“clinical scenario” is frequently used interchangeablywith the term “indication.”) Some patients seen in clinicalpractice are not represented in these AUC or have addi-tional extenuating features that would alter the appro-priateness of treatment compared with the exact clinicalscenarios presented.
AUC documents often contain more detailed clinicalscenarios than the more generalized situations covered inclinical practice guidelines, and thus, subtle differencesbetween these documents may exist. Furthermore,because recommendations for revascularization or themedical management of coronary artery disease (CAD) arefound throughout several clinical practice guidelines, theAUC ratings herein are meant to unify related clinicalpractice guidelines and other data sources and provide auseful tool for clinicians. The AUC were developed withthe intent to assist patients and clinicians, but are notintended to diminish the acknowledged complexity oruncertainty of clinical decision-making and should not bea substitute for sound clinical judgment. There areacknowledged evidence gaps in many areas where clinicaljudgement and experience must be blended with patientpreferences, and the existing knowledge base must bedefined in clinical practice guidelines.
It is important to emphasize that a rating of appro-priate care does not mandate that a procedure orrevascularization strategy be performed, may be appro-priate care represents reasonable care and can beconsidered by the patient and provider, and finally, arating of rarely appropriate care should not prevent atherapy from being performed. It is anticipated thatthere will be some clinical scenarios rated as rarelyappropriate where an alternative therapy or performingrevascularization may still be in the best interest of aparticular patient. Situations where the clinician believesa therapy contrary to the AUC rating is best for the pa-tient may require careful documentation as to the spe-cific patient features not captured in the clinical scenarioor the rationale for the chosen therapy. Depending onthe urgency of care, obtaining a second opinion may behelpful in some of these settings.
The AUC can be used in several ways. As a clinical tool,the AUC assist clinicians in evaluating possible therapiesunder consideration and can help better inform patientsabout their therapeutic options. As an administrative andresearch tool, the AUC provide a means to compare utili-zation patterns across a large subset of providers todeliver an assessment of an individual clinician’s man-agement strategies with those of similar physicians. It isimportant to again emphasize that the AUC should be
used to measure overall patterns of clinical care ratherthan to adjudicate the appropriateness of individualcases. The ACC and its collaborators believe that anongoing review of one’s practice using these criteria willhelp guide more effective, efficient, and equitable allo-cation of healthcare resources, and ultimately lead tobetter patient outcomes. Under no circumstances shouldthe AUC be used as the sole means to adjudicate ordetermine payment for individual patients—rather, theintent of the AUC is to provide a framework to evaluateoverall clinical practice and to improve the quality of care.
In developing these AUC for coronary revasculariza-tion, the rating panel was asked to rate each indicationusing the following definition of appropriate use:
A coronary revascularization or antianginal thera-peutic strategy is appropriate care when the potential
benefits, in terms of survival or health outcomes(symptoms, functional status, and/or quality of life)exceed the potential negative consequences of the
treatment strategy.
Although antianginal therapy is mentioned in thisdefinition, the writing committee acknowledges that thefocus of this document is revascularization, as it is thedominant therapy for patients with ACS. Medical therapymay have a role in the management of ongoing ischemicsymptoms, but not to the extent that it does for SIHD.
The rating panel scored each indication on a scale from1 to 9 as follows:
re 7 to 9: Appropriate care
re 4 to 6: May be appropriate care
re 1 to 3: Rarely appropriate care
Appropriate Use Definition and Ratings
In rating these criteria, the rating panel was asked toassess whether the use of revascularization for eachindication is “appropriate care,” “may be appropriatecare,” or “rarely appropriate care” using the followingdefinitions and their associated numeric ranges.
Median Score 7 to 9: Appropriate Care
An appropriate option for management of patients in thispopulation due to benefits generally outweighing risks;an effective option for individual care plans, although notalways necessary depending on physician judgment andpatient-specific preferences (i.e., procedure is generallyacceptable and is generally reasonable for the indication).
Median Score 4 to 6: May Be Appropriate Care
At times, an appropriate option for management of pa-tients in this population due to variable evidence oragreement regarding the risk-benefit ratio, potential
-
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-6
benefit on the basis of practice experience in theabsence of evidence, and/or variability in the popula-tion; effectiveness for individual care must be deter-mined by a patient’s physician in consultation with thepatient on the basis of additional clinical variables andjudgment along with patient preferences (i.e., proceduremay be acceptable and may be reasonable for theindication).
Median Score 1 to 3: Rarely Appropriate Care
Rarely an appropriate option for management of patientsin this population due to the lack of a clear benefit/riskadvantage; rarely, an effective option for individual careplans; exceptions should have documentation of theclinical reasons for proceeding with this care option (i.e.,procedure is not generally acceptable and is not generallyreasonable for the indication).
Scope of Indications
The indications for coronary revascularization in ACS weredeveloped considering the following common variables:
1. The clinical presentation (STEMI, NSTEMI, or other ACS);2. Time from onset of symptoms;3. Presence of other complicating factors (severe heart
failure or cardiogenic shock; hemodynamic or elec-trical instability, presence of left ventricular dysfunc-tion, persistent or recurring ischemic symptoms);
4. Prior treatment by fibrinolysis;5. Predicted risk as estimated by the Thrombolysis In
Myocardial Infarction score;6. Relevant comorbidities; and7. Extent of anatomic disease in the culprit and non-
culprit arteries.
The writing group characterized ACS and their man-agement into the 2 common clinical presentations: STEMIand NSTEMI/unstable angina. The anatomic construct forCAD is on the basis of the presence or absence of impor-tant obstructions in the coronary arteries categorized bythe number of vessels involved 1-, 2-, and 3-vessel CAD)and the ability to identify the culprit artery responsiblefor the ACS Although the culprit stenosis is frequentlyobvious from the coronary angiogram, there are situationswhere the location of the culprit stenosis is uncertain orwhere multiple culprit stenoses may exist.
After initial treatment of the patient with an ACS, itmay be helpful to categorize the amount of myocardiumat risk or affected by ischemia; thus, a minority of sce-narios include noninvasive testing. The writing groupcharacterized noninvasive test findings as low-risk versusintermediate- or high-risk, as these terms are routinelyused in clinical practice. The use of FFR measurement isincreasing in the setting of stable ischemic heart disease,but there are limited data on its utility in the setting of
ACS to evaluate nonculprit vessels (6). Nevertheless, thewriting group provided some indications with invasivephysiology testing (represented by FFR) in nonculpritvessels in patients with ACS.
3. ASSUMPTIONS
General Assumptions
Specific instructions and assumptions used by the ratingpanel to assist in the rating of clinical scenarios are listedin the following text:
1. Each clinical scenario is intended to provide the keyinformation typically available when a patient pre-sents with an ACS, recognizing that especially in thesetting of an STEMI, the need for rapid treatment mayprevent a complete evaluation.
2. Although the clinical scenarios should be rated on thebasis of the published literature, the writing commit-tee acknowledges that in daily practice, decisionsabout therapy are required in certain patient pop-ulations that are poorly represented in the literature.Therefore, rating panel members were instructed touse their best clinical judgment and experience inassigning ratings to clinical scenarios that have lowlevels of evidence.
3. In ACS, the percent luminal diameter narrowing of astenosis may be difficult to assess. Determining thesignificance of a stenosis includes not only thepercent luminal diameter narrowing, but also theangiographic appearance of the stenosis and distalflow pattern. For these clinical scenarios, a coronarystenosis in an artery is defined as:
n Severe:a. A $70% luminal diameter narrowing of an
epicardial stenosis made by visual assessmentin the “worst view” angiographic projection; or
b. A $50% luminal diameter narrowing of the leftmain artery made by visual assessment, in the“worst view” angiographic projection.
n Intermediate:c. A $50% and
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
7
6. Revascularization by either percutaneous or surgicalmethods is performed in a manner consistent withestablished standards of care at centers with quality/volume standards (18–20).
7. No unusual extenuating circumstances exist in theclinical scenarios such as but not limited to do-not-resuscitate status, advanced malignancy, unwilling-ness to consider revascularization, technical reasonsrendering revascularization infeasible, or comorbid-ities likely to markedly increase procedural risk.
8. Assume that the appropriateness rating applies onlyto the specific treatment strategy outlined in thescenario and not additional revascularization pro-cedures that may be performed later in the patient’scourse. Specifically, additional elective revasculari-zation procedures (so called delayed staged proced-ures) performed after the hospitalization for ACS areevaluated and rated in the forthcoming AUC docu-ment on SIHD. For data collection purposes, this willrequire documenting that the procedure is staged(either PCI or hybrid revascularization with surgery).
9. As with all previously published clinical policies, de-viations by the rating panel from prior publisheddocuments were driven by new evidence and/orimplementation of knowledge that justifies suchevolution. However, the reader is advised to paycareful attention to the wording of an indication in thepresent document and should avoid making compar-isons to prior documents.
10. Indication ratings contained herein supersede theratings of similar indications contained in previousAUC coronary revascularization documents.
4. DEFINITIONS
Definitions of terms used throughout the indication setare listed here. These definitions were provided to anddiscussed with the rating panel before the rating of in-dications. The writing group assumed that noninvasiveassessments of coronary anatomy (i.e., cardiac computedtomography, cardiac magnetic resonance angiography)provide anatomic information that is potentially similarto X-ray angiography. However, these modalities do notcurrently provide information on ischemic burden and arenot assumed to be present in the clinical scenarios.
Indication
A set of patient-specific conditions defines an “indica-tion,” which is used interchangeably with the phrase“clinical scenario.”
Cardiac Risk Factor Modification andAntianginal Medical Therapy
The indications assume that patients are receivingguideline-directed medical therapies for their ACS
including antiplatelet and anticoagulant medications,beta-blockers, statins, and other medications as indicatedby their clinical condition.
Culprit Stenosis
The phrase “culprit stenosis” is often used interchange-ably with “infarct-related artery” to identify the coronaryartery stenosis and/or artery responsible for the ACS. Inthis document, the phrase “culprit stenosis or culprit ar-tery” is preferred, because in the setting of unstable anginathere may be a culprit stenosis or culprit artery, but bydefinition, there is no evidence of a myocardial infarction.
Symptoms of Myocardial Ischemia
For the purposes of the clinical scenarios in this docu-ment, the AUC are intended to apply to patients who havethe typical underlying pathology of an ACS, not simply anelevated troponin value in the absence of an appropriateclinical syndrome. The symptoms of an ACS may bedescribed as both typical and atypical angina or symp-toms felt to represent myocardial ischemia, such as ex-ertional dyspnea, and are captured under the broad term“ischemic symptoms.” Although previous AUC had usedthe Canadian Cardiovascular Society system for anginalclassification, the writing group recognized that the broadspectrum of ischemic symptoms may limit patients’functional status in a variety of ways, and capturing theCanadian Cardiovascular Society status in clinical practicemay also vary widely. Therefore, the presence or absenceof ischemic symptoms are presented without specificscale. Additionally, post–ACS symptoms may persist and/or be easily provoked with minimal activity.
Unstable Angina
The definition of unstable angina is largely on the basis ofthe clinical presentation. Unstable angina is defined astypical chest pain or other ischemic symptoms occurringat rest or with minimal exertion, and presumed to berelated to an acutely active coronary plaque. In contrastto stable angina, unstable angina is often described assevere and as a frank pain. Moreover, unstable anginamay be new in onset or occur in a crescendo pattern in apatient with a previous stable pattern of angina. Unstableangina may be associated with new electrocardiographicchanges such as transient ST-segment elevation, ST-segment depression, or T-wave inversion, but may bepresent in the absence of electrocardiographic changes.Several scoring systems exist for determining high-riskpatients with ACS (Tables A and B).
Stress Testing and Risk of Findings on Noninvasive Testing
Stress testing and coronary CTA are commonly used forboth diagnosis and risk stratification of patients with cor-onary artery disease or those with suspected ACS.
-
TABLE AHigh-Risk Features for Short-Term Risk ofDeath or Nonfatal MI in Patients WithNSTEMI/UA
At least 1 of the following:n History—accelerating tempo of anginal symptoms in preceding 48 hoursn Character of pain—prolonged ongoing (>20 minutes) rest painn Clinical findings
n Pulmonary edema, most likely due to ischemian New or worsening MR murmurn S3 or new/worsening ralesn Hypotension, bradycardia, tachycardian Age >75 years
n ECGn Transient ST-segment deviation >0.5 mmn Bundle-branch block, new or presumed newn Sustained ventricular tachycardia
n Cardiac markern Elevated cardiac TnT, TnI, or CK-MB (e.g., TnT or TnI >0.1 ng per ml)
High-risk features were defined as in the ACS guidelines (21).
CK-MB ¼ creatine kinase, MB isoenzyme; ECG ¼ electrocardiogram; MI ¼ myocardialinfarction; MR ¼ mitral regurgitation; NSTEMI ¼ non–ST segment elevation myocardialinfarction; TnI ¼ troponin I; TnT ¼ troponin T; UA ¼ unstable angina.
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-8
Although often contraindicated in ACS, stress testing maybe performed for further risk stratification later during theindex hospitalization. Risk stratification by noninvasivetesting is defined as (4):
Lo
Int
Hig
TABL
Variablen Agen $3 rn Known Aspin Seven ST-sn Elev
Risk of dn Lown Inten High
ACS ¼ alitus; FH
w-risk stress test findings: associated with a 3%per year cardiac mortality rate.
The Role of Patient Preference in the AUC
Patients often make decisions about medical treatmentswithout a complete understanding of their options. Pa-tient participation or shared decision-making describes acollaborative approach where patients are providedevidence-based information on treatment choices and areencouraged to use the information in an informed dia-logue with their provider to make decisions that not onlyuse the scientific evidence, but also align with theirvalues, preferences, and lifestyle (23–25). The alternative
E BThrombolysis In Myocardial Infarction RiskScore—For Patients With Suspected ACS (22)
s (1 point each)$65 yearsisk factors (HTN, DM, FH, lipids, smoking)n CAD (stenosis $50%)
rin use in past 7 daysre angina ($2 episodes within 24 hours)egment deviation $0.5 mmated cardiac markers
eath or ischemic event through 14 days: 0–2 (70% diameter stenosis in 1 angiographic plane or >50%in 2 planes and in an artery >2 mm suitable for stentimplantation. Treatment of the nonculprit stenosis
-
ACS ¼AUC ¼CAD ¼FFR ¼NSTEM
PCI ¼SIHD
STEM
TABLE C Treatment of Nonculprit Stenoses in the Patient With STEMI
PRAMI(n ¼ 465)
CvLPRIT(n ¼ 296)
DANAMI3-PRIMULTI(n ¼ 627)
Randomization After primary PCI “During” primary PCI After primary PCI
Lesion criteria >50% DS >70% DS or >50% DS in 2 views >50% DS and FFR 90% DS
Strategy for non–IRA lesions Immediate—at time of primary PCI Immediate or staged within index admission Staged within index admission (average day 2)
CvLPRIT ¼ Complete Versus Lesion-Only Primary PCI Trial; DANAMI3-PRIMULTI ¼ The Third Danish Study of Optimal Acute Treatment of Patients with STEMI: Primary PCI in Mul-tivessel Disease; DS ¼ diameter stenosis; FFR ¼ fractional flow reserve; IRA ¼ infarct-related artery; PCI ¼ percutaneous coronary intervention; PRAMI ¼ Preventive Angioplasty inAcute Myocardial Infarction Trial.
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
9
immediately following the primary PCI was encouraged,but could be deferred to later during the same hospitali-zation. In DANAMI3-PRIMULTI (The Third Danish Study ofOptimal Acute Treatment of Patients with STEMI: PrimaryPCI in Multivessel Disease), nonculprit stenoses weretreated if the diameter stenosis was >50% and theFFR 90%.Treatment of the nonculprit stenoses was planned for 2days after the primary PCI during the index hospitaliza-tion. These variations in the criteria for nonculprit stenosistreatment and timing of treatment from these 3 relativelysmall studies make it challenging to develop clinical sce-narios. This is an evolving shift in the treatment paradigmfor patients presenting with STEMI that, at present, isincompletely understood. Scenarios were developed toallow the rating panel to evaluate clinical situations thatmirror the evidence provided in these new trials.
This AUC only covers clinical scenarios where theculprit artery and additional nonculprit arteries aretreated at the time of primary PCI or later during theinitial hospitalization. The writing group recognizes theremay be circumstances where treatment of a nonculpritartery is deferred beyond the initial hospitalization. Thatspecific circumstance was not studied in the 3 recent trials
TABLE 1 .1 STEMI—Immediate Revascularization by PCI
Indication
Revascularization of the Presumed Culprit Artery by PCI (Primary PCI)
1. n Less than or equal to 12 hours from onset of symptoms
2. n Onset of symptoms within the prior 12–24 hours ANDn Severe HF, persistent ischemic symptoms, or hemodynamic or electri
3. n Onset of symptoms within the prior 12–24 hours ANDn Stable without severe HF, persistent ischemic symptoms, or hemodyn
Successful Treatment of the Culprit Artery by Primary PCI Followed by Immethe Same Procedure
4. n Cardiogenic shock persisting after PCI of the presumed culprit arteryn PCI or CABG of 1 or more additional vessels
5. n Stable patient immediately following PCI of the presumed culprit artn One or more additional severe stenoses
6. n Stable patient immediately following PCI of the presumed culprit artn One or more additional intermediate (50%–70%) stenoses
The number in parenthesis next to the rating reflects the median score for that indication.
A ¼ appropriate; CABG ¼ coronary artery bypass graft; HF ¼ heart failure; M ¼ may be apST-segment elevation myocardial infarction.
of nonculprit stenosis treatment. However, if the char-acteristics of the patient are such that treatment of non-culprit stenoses are deferred beyond the initialhospitalization, it is assumed the patient is clinicallystable. These clinical scenarios will be evaluated in theforthcoming SIHD document.
5. ABBREVIATIONS
cal insta
amic or
diate R
ery
ery
propriate
acute coronary syndrome
appropriate use criteria
coronary artery disease
fractional flow reserve
I ¼ non–ST-segment elevation myocardial infarctionpercutaneous coronary intervention
¼ stable ischemic heart diseaseI ¼ ST-segment elevation myocardial infarction
6. CORONARY REVASCULARIZATION IN
PATIENTS WITH ACS: AUC (BY INDICATION)
Scenarios 1 to 3 in Table 1.1 specifically address treatmentof the culprit stenosis at the time intervals and with the
Appropriate Use Score (1–9)
A (9)
bility presentA (8)
electrical instabilityM (6)
evascularization of 1 or More Nonculprit Arteries During
A (8)
M (6)
M (4)
; PCI ¼ percutaneous coronary intervention; R ¼ rarely appropriate; STEMI ¼
-
TABLE 1 .2 STEMI—Initial Treatment by Fibrinolytic Therapy
Indication Appropriate Use Score (1–9)
PCI of the Presumed Culprit Artery After Fibrinolysis
7. n Evidence of failed reperfusion after fibrinolysis (e.g., failure of ST-segment resolution, presence of acutesevere HF, ongoing myocardial ischemia, or unstable ventricular arrhythmias)
A (9)
8. n Stable after fibrinolysis ANDn Asymptomatic (no HF, myocardial ischemia, or unstable ventricular arrhythmias) ANDn PCI performed 3–24 hours after fibrinolytic therapy
A (7)
9. n Stable after fibrinolysis ANDn Asymptomatic (no HF, myocardial ischemia, or unstable ventricular arrhythmias) ANDn PCI >24 hours after onset of STEMI
M (5)
The number in parenthesis next to the rating reflects the median score for that indication.
A ¼ appropriate; CABG ¼ coronary artery bypass graft; HF ¼ heart failure; M ¼ may be appropriate; PCI ¼ percutaneous coronary intervention; R ¼ rarely appropriate; STEMI ¼ST-segment elevation myocardial infarction.
TABLE 1 .3 STEMI—Revascularization of Nonculprit Artery During the Initial Hospitalization
Indication Appropriate Use Score (1–9)
Successful Treatment of the Culprit Artery by Primary PCI or Fibrinolysis Revascularization of 1 or More Nonculprit Arteries Duringthe Same Hospitalization
Revascularization by PCI or CABG
10. n Spontaneous or easily provoked symptoms of myocardial ischemian One or more additional severe stenoses
A (8)
11. n Asymptomaticn Findings of ischemia on noninvasive testingn One or more additional severe stenoses
A (7)
12. n Asymptomatic (no additional testing performed)n One or more additional severe stenoses
M (6)
13 n Asymptomatic (no additional testing performed)n One or more additional intermediate stenoses
R (3)
14. n Asymptomaticn One or more additional intermediate (50%–70%) stenosesn FFR performed and #0.80
A (7)
The number in parenthesis next to the rating reflects the median score for that indication.
A ¼ appropriate; CABG ¼ coronary artery bypass graft; FFR ¼ fractional flow reserve; M ¼ may be appropriate; PCI ¼ percutaneous coronary intervention; R ¼ rarely appropriate;STEMI ¼ ST-segment elevation myocardial infarction.
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-10
presence or absence of symptoms as noted. Scenarios 4 to6 in Table 1.1 specifically address treatment of 1 or morenonculprit stenoses during the same procedure as treat-ment of the culprit stenosis. Because these scenarios arespecific for nonculprit treatment immediately following
TABLE 1.4 NSTEMI/Unstable Angina
Indication
Revascularization by PCI or CABG
15. n Evidence of cardiogenic shockn Immediate revascularization of 1 or more coronary arteries
16. n Patient stabilizedn Intermediate- OR high-risk features for clinical events (e.g., TIMI scorn Revascularization of 1 or more coronary arteries
17. n Patient stabilized after presentationn Low-risk features for clinical events (e.g., TIMI score #2)n Revascularization of 1 or more coronary arteries
The number in parenthesis next to the rating reflects the median score for that indication.
A ¼ appropriate; CABG ¼ coronary artery bypass graft; M ¼ may be appropriate; NSTEintervention; R ¼ rarely appropriate; TIMI ¼ Thrombolysis In Myocardial Infarction.
primary PCI, the criteria for treatment used in DANAMI3-PRIMULTI cannot be applied in this table.
As noted in Table 1.1, treatment of the nonculprit arterycan occur at several different times after treatment of theculprit stenosis. Because Table 1.1 covers those scenarios
Appropriate Use Score (1–9)
A (9)
e 3–4)A (7)
M (5)
MI ¼ non–ST-segment elevation myocardial infarction; PCI ¼ percutaneous coronary
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
11
where nonculprit treatment occurs immediately after theprimary PCI, this table is specific for treatment of non-culprit stenoses after the initial procedure, but during theinitial hospitalization.
Unstable angina/NSTEMI category—in patients withThrombolysis In Myocardial Infarction 3 flow and multi-ple coronary artery stenoses, consideration should begiven for heart team evaluation in patients with a highburden of CAD, such as 2-vessel disease with proximal leftanterior descending coronary artery stenosis or more se-vere disease.
7. DISCUSSION
The new AUC ratings for ACS are consistent with existingguidelines for STEMI and NSTEMI-ACS (Figure 2). Forpatients with ACS, revascularization by either PCI or
FIGURE 2 Flow Diagram for the Determination of Appropriate Use in Patie
Asx ¼ asymptomatic; CABG ¼ coronary artery bypass graft; FFR ¼ fractional flomyocardial infarction; PCI ¼ percutaneous coronary intervention; STEMI ¼ ST-s
CABG is the most commonly used therapy, and this isreflected in the ratings of “appropriate care” or “may beappropriate care” for all but 1 of the 17 scenarios pre-sented. Although these AUC ratings do not compare themerits of PCI versus CABG for revascularization in ACS, inclinical practice, patients presenting with STEMI typicallyare treated by PCI of the culprit stenosis. However, theoption of surgical revascularization should be consideredfor patients with ACS but less acute presentation, espe-cially in those with complex multivessel CAD.
The current AUC rate revascularization as “appropriatecare” for patients presenting within 12 hours of the onsetof STEMI or up to 24 hours if there is clinical instability.For STEMI patients presenting more than 12 and up to 24hours from symptom onset but with no signs of clinicalinstability, revascularization was rated as “may beappropriate,” indicating that many on the technical panel
nts With Acute Coronary Syndromes
w reserve; HF ¼ heart failure; NSTEMI ¼ non–ST-segment elevationegment elevation myocardial infarction; UA ¼ unstable angina.
-
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-12
consider it reasonable to revascularize such patients.Furthermore, nonculprit artery revascularization at thetime of primary PCI was rated as “may be appropriate,”but because this is an emerging concept on the basis ofrelatively small studies, clinical judgment by the operatoris encouraged.
For STEMI patients initially treated with fibrinolysis,revascularization was rated as “appropriate therapy” inthe setting of suspected failed fibrinolytic therapy or instable and asymptomatic patients from 3 to 24 hours afterfibrinolysis. In the setting of suspected failed fibrinolysis,the need for revascularization is usually immediate,whereas in stable patients with apparent successfulfibrinolysis, revascularization can be delayed for up to 24hours. For stable patients >24 hours after fibrinolysis,revascularization was rated as “may be appropriate.”Revascularization soon after apparent successful fibrino-lysis is supported by data and guideline recommenda-tions about the management of patients transferred fromcenters where PCI is not available.
Nonculprit artery revascularization during the indexhospitalization after primary PCI or fibrinolysis was alsorated as appropriate and reasonable for patients with 1 ormore severe stenoses and spontaneous or easily provokedischemia or for asymptomatic patients with ischemicfindings on noninvasive testing. In the presence of anintermediate-severity nonculprit artery stenosis, revas-cularization was rated as “appropriate therapy” providedthat the FFR was #0.80. For patients who are stable andasymptomatic after primary PCI, revascularization wasrated as “may be appropriate” for 1 or more severe ste-noses even in the absence of further testing. The only“rarely appropriate” rating in patients with ACS occurredfor asymptomatic patients with intermediate-severitynonculprit artery stenoses in the absence of any addi-tional testing to demonstrate the functional significanceof the stenosis.
For patients with NSTEMI/unstable angina, andconsistent with existing guidelines and the available
evidence, revascularization was rated as “appropriatecare” in the setting of cardiogenic shock or in a patientwith intermediate- or high-risk features. For stable pa-tients with low-risk features, revascularization wasrated as “may be appropriate.” Decisions around thetiming of revascularization, management of multivesseldisease, and concomitant pharmacotherapy should allbe on the basis of evidence from the relevant practiceguidelines.
In conclusion, the AUC for ACS are consistent withthe large body of evidence and guideline recommenda-tions that support invasive strategies to define anatomyand revascularize patients with STEMI and NSTEMI-ACS. The evolving evidence around nonculprit stenosisrevascularization has led to ratings that revasculariza-tion may be appropriate after primary PCI in selectedasymptomatic patients with severe stenoses, definedherein as $70% diameter narrowing, or in patients withintermediate-severity stenosis if FFR testing isabnormal. As in prior versions of the AUC, theserevascularization ratings should be used to reinforceexisting management strategies and identify patientpopulations that need more information to identify themost effective treatments.
ACC PRESIDENT AND STAFF
Richard A. Chazal, MD, FACC, PresidentShalom Jacobovitz, Chief Executive OfficerWilliam J. Oetgen, MD, FACC, Executive Vice President,
Science, Education, and QualityJoseph M. Allen, MA, Team Leader, Clinical Policy and
PathwaysLeah White, MPH, CCRP, Team Leader, Appropriate Use
CriteriaMarίa Velásquez, Senior Research Specialist, Appropriate
Use CriteriaAmelia Scholtz, PhD, Publications Manager, Clinical
Policy and Pathways
R EF E RENCE S
1. Patel MR, Dehmer GJ, Hirshfeld JW, Smith PK,Spertus JA. ACCF/SCAI/STS/AATS/AHA/ASNC/HFSA/SCCT 2012 appropriate use criteria for coronaryrevascularization focused update: a report of theAmerican College of Cardiology Foundation Appro-priate Use Criteria Task Force, Society for Cardiovas-cular Angiography and Interventions, Society ofThoracic Surgeons, American Association for ThoracicSurgery, American Heart Association, American Societyof Nuclear Cardiology, and the Society of Cardiovas-cular Computed Tomography. J Am Coll Cardiol. 2012;59:857–81.
2. O’Gara PT, Kushner FG, Ascheim DD, et al. 2013ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the
American College of Cardiology Foundation/AmericanHeart Association Task Force on Practice Guidelines.J Am Coll Cardiol. 2013;61:e78–140.
3. Jneid H, Anderson JL, Wright RS, et al. 2012 ACCF/AHA focused update of the guideline for the manage-ment of patients with unstable angina/non–ST-eleva-tion myocardial infarction (updating the 2007 guidelineand replacing the 2011 focused update): a report of theAmerican College of Cardiology Foundation/AmericanHeart Association Task Force on Practice Guidelines.J Am Coll Cardiol. 2012;60:645–81.
4. Fihn SD, Blankenship JC, Alexander KP, et al. 2014ACC/AHA/AATS/PCNA/SCAI/STS focused update of theGuideline for the Diagnosis and Management of
Patients With Stable Ischemic Heart Disease: a reportof the American College of Cardiology/American HeartAssociation Task Force on Practice Guidelines, and theAmerican Association for Thoracic Surgery, PreventiveCardiovascular Nurses Association, Society for Cardio-vascular Angiography and Interventions, and Societyof Thoracic Surgeons. J Am Coll Cardiol. 2014;64:1929–49.
5. Levine GN, O’Gara PT, Bates ER, et al. 2015ACC/AHA/SCAI focused update on primary percu-taneous coronary intervention for patients withST-elevation myocardial infarction: an update ofthe 2011 ACCF/AHA/SCAI Guideline for Percuta-neous Coronary Intervention and the 2013ACCF/AHA Guideline for the Management of
http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref1http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref2http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref3http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref4http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
13
ST-Elevation Myocardial Infarction: a report of theAmerican College of Cardiology/American HeartAssociation Task Force on Clinical Practice Guide-lines and the Society for Cardiovascular Angiog-raphy and Interventions. J Am Coll Cardiol. 2016;67:1235–50.
6. Engstrom T, Kelbaek H, Helqvist S, et al. Completerevascularisation versus treatment of the culprit lesiononly in patients with ST-segment elevation myocardialinfarction and multivessel disease (DANAMI-3-PRI-MULTI): an open-label, randomised controlled trial.Lancet. 2015;386:665–71.
7. Gershlick AH, Khan JN, Kelly DJ, et al. Ran-domized trial of complete versus lesion-onlyrevascularization in patients undergoing primarypercutaneous coronary intervention for STEMI andmultivessel disease: the CvLPRIT trial. J Am CollCardiol. 2015;65:963–72.
8. Wald DS, Morris JK, Wald NJ, et al. Randomized trialof preventive angioplasty in myocardial infarction.N Engl J Med. 2013;369:1115–23.
9. Bradley SM, Spertus JA, Kennedy KF, et al. Patientselection for diagnostic coronary angiography andhospital-level percutaneous coronary interventionappropriateness: insights from the National Cardio-vascular Data Registry. JAMA Intern Med. 2014;174:1630–9.
10. Chan PS, Patel MR, Klein LW, et al. Appropriatenessof percutaneous coronary intervention. JAMA. 2011;306:53–61.
11. Desai NR, Bradley SM, Parzynski CS, et al. Appro-priate use criteria for coronary revascularization andtrends in utilization, patient selection, and appropri-ateness of percutaneous coronary intervention. JAMA.2015;314:2045–53.
12. Hendel RC, Patel MR, Allen JM, et al. Appropriateuse of cardiovascular technology: 2013 ACCF appro-priate use criteria methodology update. J Am CollCardiol. 2013;61:1305–17.
13. Smith SC Jr, Allen J, Blair SN, et al. AHA/ACCguidelines for secondary prevention for patients withcoronary and other atherosclerotic vascular disease:2006 update endorsed by the National Heart, Lung,and Blood Institute. J Am Coll Cardiol. 2006;47:2130–9.
14. Pearson TA, Blair SN, Daniels SR, et al. AHAguidelines for primary prevention of cardiovasculardisease and stroke: 2002 update: Consensus PanelGuide to Comprehensive Risk Reduction for Adult Pa-tients Without Coronary or Other AtheroscleroticVascular Diseases. American Heart Association ScienceAdvisory and Coordinating Committee. Circulation.2002;106:388–91.
15. Buse JB, Ginsberg HN, Bakris GL, et al. Primaryprevention of cardiovascular diseases in people withdiabetes mellitus: a scientific statement from theAmerican Heart Association and the American DiabetesAssociation. Circulation. 2007;115:114–26.
16. Adult Treatment Panel III. Third report of theNational Cholesterol Education Program (NCEP)Expert Panel on Detection, Evaluation, and Treat-ment of High Blood Cholesterol in Adults (AdultTreatment Panel III) final report. Circulation. 2002;106:3143–421.
17. Chobanian AV, Bakris GL, Black HR, et al. Seventhreport of the Joint National Committee on Prevention,Detection, Evaluation, and Treatment of High BloodPressure. Hypertension. 2003;42:1206–52.
18. Harold JG, Bass TA, Bashore TM, et al. ACCF/AHA/SCAI 2013 update of the clinical competencestatement on coronary artery interventional proced-ures: a report of the American College of CardiologyFoundation/American Heart Association/AmericanCollege of Physicians Task Force on Clinical Compe-tence and Training (Writing Committee to Revise the2007 Clinical Competence Statement on CardiacInterventional Procedures). J Am Coll Cardiol. 2013;62:357–96.
19. Hillis LD, Smith P, Anderson J, et al. 2011 ACCF/AHA guidelines for coronary artery bypass graft sur-gery: a report of the American College of CardiologyFoundation/American Heart Association Task Force onPractice Guidelines. J Am Coll Cardiol. 2011;58:e123–210.
20. Levine GN, Bates ER, Blankenship JC, et al. 2011ACCF/AHA/SCAI guideline for percutaneous coronaryintervention: a report of the American College of Car-diology Foundation/American Heart Association TaskForce on Practice Guidelines and the Society for Car-diovascular Angiography and Interventions. J Am CollCardiol. 2011;58:e44–122.
21. Amsterdam EA, Wenger NK, Brindis RG, et al.2014 AHA/ACC guideline for the management ofpatients with non–ST-elevation acute coronary syn-dromes: a report of the American College of Cardi-ology/American Heart Association Task Force onPractice Guidelines. J Am Coll Cardiol. 2014;64:e139–228.
22. TIMI Study Group. Available at: http://www.timi.org. Accessed March 15, 2011.
23. Chewning B, Bylund CL, Shah B, Arora NK,Gueguen JA, Makoul G. Patient preferences for shareddecisions: a systematic review. Patient Educ Couns.2012;86:9–18.
24. Lin GA, Fagerlin A. Shared decision making: state ofthe science. Circ Cardiovasc Qual Outcomes. 2014;7:328–34.
25. Ting HH, Brito JP, Montori VM. Shared decisionmaking: science and action. Circ Cardiovasc Qual Out-comes. 2014;7:323–7.
26. Buchanan A. Medical paternalism. Philos Public Aff.1978;7:370–90.
KEY WORDS ACC Appropriate Use Criteria,coronary revascularization, imaging, medicaltherapy, multimodality
http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref5http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref6http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref7http://refhub.elsevier.com/S0735-1097(16)36782-1/sref8http://refhub.elsevier.com/S0735-1097(16)36782-1/sref8http://refhub.elsevier.com/S0735-1097(16)36782-1/sref8http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref9http://refhub.elsevier.com/S0735-1097(16)36782-1/sref10http://refhub.elsevier.com/S0735-1097(16)36782-1/sref10http://refhub.elsevier.com/S0735-1097(16)36782-1/sref10http://refhub.elsevier.com/S0735-1097(16)36782-1/sref11http://refhub.elsevier.com/S0735-1097(16)36782-1/sref11http://refhub.elsevier.com/S0735-1097(16)36782-1/sref11http://refhub.elsevier.com/S0735-1097(16)36782-1/sref11http://refhub.elsevier.com/S0735-1097(16)36782-1/sref11http://refhub.elsevier.com/S0735-1097(16)36782-1/sref12http://refhub.elsevier.com/S0735-1097(16)36782-1/sref12http://refhub.elsevier.com/S0735-1097(16)36782-1/sref12http://refhub.elsevier.com/S0735-1097(16)36782-1/sref12http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref13http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref14http://refhub.elsevier.com/S0735-1097(16)36782-1/sref15http://refhub.elsevier.com/S0735-1097(16)36782-1/sref15http://refhub.elsevier.com/S0735-1097(16)36782-1/sref15http://refhub.elsevier.com/S0735-1097(16)36782-1/sref15http://refhub.elsevier.com/S0735-1097(16)36782-1/sref15http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref16http://refhub.elsevier.com/S0735-1097(16)36782-1/sref17http://refhub.elsevier.com/S0735-1097(16)36782-1/sref17http://refhub.elsevier.com/S0735-1097(16)36782-1/sref17http://refhub.elsevier.com/S0735-1097(16)36782-1/sref17http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref18http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref19http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref20http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://refhub.elsevier.com/S0735-1097(16)36782-1/sref21http://www.timi.orghttp://www.timi.orghttp://refhub.elsevier.com/S0735-1097(16)36782-1/sref23http://refhub.elsevier.com/S0735-1097(16)36782-1/sref23http://refhub.elsevier.com/S0735-1097(16)36782-1/sref23http://refhub.elsevier.com/S0735-1097(16)36782-1/sref23http://refhub.elsevier.com/S0735-1097(16)36782-1/sref24http://refhub.elsevier.com/S0735-1097(16)36782-1/sref24http://refhub.elsevier.com/S0735-1097(16)36782-1/sref24http://refhub.elsevier.com/S0735-1097(16)36782-1/sref25http://refhub.elsevier.com/S0735-1097(16)36782-1/sref25http://refhub.elsevier.com/S0735-1097(16)36782-1/sref25http://refhub.elsevier.com/S0735-1097(16)36782-1/sref26http://refhub.elsevier.com/S0735-1097(16)36782-1/sref26
-
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-14
APPENDIX A. APPROPRIATE USE CRITERIA FOR CORONARY REVASCULARIZATION IN PATIENTS WITH
ACUTE CORONARY SYNDROMES: PARTICIPANTS
Writing Group
Manesh R. Patel, MD, FACC, FAHA, FSCAI—AssociateProfessor of Medicine, Director Interventional Cardiologyand Catheterization Labs, Duke University Health System,Duke Clinical Research Institute, Durham, NC
John H. Calhoon, MD—Professor and Chair, PresidentsCouncil Chair for Excellence in Surgery, Department ofCardiothoracic Surgery, Director, University of TexasHealth Science Center at San Antonio, Heart and VascularInstitute, San Antonio, TX
Gregory J. Dehmer, MD, MACC, MSCAI, FACP, FAHA—Clinical Professor of Medicine, Texas A&M Health ScienceCenter College of Medicine, Medical Director, Cardiovas-cular Services, Central Texas Division, Director, Cardiol-ogy Division, Baylor Scott & White–Temple Memorial,Temple, TX
James Aaron Grantham, MD, FACC—Associate ClinicalProfessor, University of Missouri–Kansas City School ofMedicine, Director, Cardiovascular Disease FellowshipProgram, University of Missouri–Kansas City School ofMedicine, Director, Cardiovascular Medical Education,Saint Luke’s Hospital, Kansas City, MO
Thomas M. Maddox, MD, MSc, FACC, FAHA—NationalDirector, VA CART Program Cardiology, VA Eastern Col-orado Health Care System, Associate Professor, Depart-ment of Medicine, Cardiology, University of Colorado,Colorado Cardiovascular Outcomes Research Consortium,Denver, CO
David J. Maron, MD, FACC, FAHA—Clinical Professor ofMedicine, Cardiovascular, Director, Preventive Cardiol-ogy, ISCHEMIA Trial Co-Chair, Principal Investigator,Stanford University School of Medicine, Stanford, CA
Peter K. Smith, MD, FACC—Professor of Surgery, Divi-sion Chief, Cardiovascular and Thoracic Surgery, DukeUniversity, Durham, NC
Rating Panel
Michael J. Wolk, MD, MACC, Moderator—Past President,American College of Cardiology, Clinical Professor ofMedicine, Weill Medical College of Cornell University,New York Cardiology Associates, New York, NY
Manesh R. Patel, MD, FACC, FAHA, FSCAI, WritingCommittee Liaison—Associate Professor of Medicine, Di-rector Interventional Cardiology and CatheterizationLabs, Duke University Health System, Duke ClinicalResearch Institute, Durham, NC
Gregory J. Dehmer, MD, MACC, MSCAI, FAHA, WritingCommittee Liaison—Clinical Professor of Medicine, Texas
A&M Health Science Center College of Medicine, MedicalDirector, Cardiovascular Services, Central Texas Division,Director, Cardiology Division, Baylor Scott and White,Temple Memorial, Temple, TX
Peter K. Smith, MD, FACC, Writing Committee Liaison—Professor of Surgery, Division Chief, Cardiovascular andThoracic Surgery, Duke University, Durham, NC
James C. Blankenship, MD, MACC—Staff Physician, Di-rector, Cardiac Catheterization Laboratory, Division ofCardiology, Geisinger Medical Center, Danville, PA
Alfred A. Bove, MD, PhD, MACC—Past President,American College of Cardiology, Professor Emeritus,Lewis Katz School of Medicine, Heart and Vascular,Temple University, Philadelphia, PA
Steven M. Bradley, MD—Staff Cardiologist, VA EasternColorado Health Care System, Assistant Professor ofMedicine, Division of Cardiology at the University ofColorado, Denver, CO
Larry S. Dean, MD, FACC, FSCAI—Professor of Medicineand Surgery, University of Washington School of Medi-cine, Director, University of Washington, MedicineRegional Heart Center, Seattle, WA
Peter L. Duffy, MD, FACC, FSCAI—Director of Qualityfor the Cardiovascular Service Line, First Health of theCarolinas, Reid Heart Institute/Moore Regional Hospital,Pinehurst, NC
T. Bruce Ferguson, Jr., MD, FACC—Professor ofThoracic Surgery, Department of Cardiovascular Sciences,Cardiothoracic Surgery, East Carolina Heart Institute, EastCarolina University, Greenville, NC
Frederick L. Grover, MD, FACC—Professor of Cardio-thoracic Surgery, Department of Cardiothoracic Surgery,University of Colorado, Denver, CO
Robert A. Guyton, MD, FACC—Chief of CardiothoracicSurgery, Professor of Surgery, Division of CardiothoracicSurgery, Department of Surgery, Director, Thoracic Sur-gery Residency Program, Emory University School ofMedicine, Atlanta, GA
Mark A. Hlatky, MD, FACC—Professor of HeathResearch and Policy, Health Services Research, Professorof Medicine, Cardiovascular Medicine, Stanford Univer-sity School of Medicine, Stanford, CA
Harold L. Lazar, MD, FACC—Director, CardiothoracicResearch Program, Professor of Cardiothoracic Surgery,Boston University School of Medicine, Boston, MA
Vera H. Rigolin, MD, FACC—Professor, Cardiology,Northwestern University Feinberg School of Medicine,Chicago, IL
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
15
Geoffrey A. Rose, MD, FACC, FASE—Chief, Division ofCardiology, Sanger Heart and Vascular Institute, Char-lotte, NC
Richard J. Shemin, MD, FACC—Robert and Kelly DayProfessor, Chief of Cardiothoracic Surgery, Executive ViceChair of Surgery, Co-Director of the Cardiovascular Cen-ter, Director of Cardiac Quality at the Ronald ReaganUCLA Medical Center, Los Angeles, CA
Jacqueline E. Tamis-Holland, MD, FACC—Director,Interventional Cardiology Fellowship, Mount Sinai, SaintLuke’s Hospital Director, Women’s Heart NY AssistantProfessor of Medicine, Icahn School of Medicine at MountSinai Hospital, New York, NY
Carl L. Tommaso, MD, FACC, FSCAI—Director of theCardiac Catheterization Laboratory at Skokie IllinoisHospital, part of the Northshore University Health Sys-tem, Associate Professor of Medicine at Rush MedicalCollege in Chicago, Chicago, IL
L. Samuel Wann, MD, MACC—Past President, AmericanCollege of Cardiology, Clinical Cardiologist, Columbia St.Mary’s Healthcare, Medical Director, Heart Failure Pro-gram, Milwaukee, WI
John B. Wong, MD—Chief, Division of Clinical DecisionMaking, Primary Care Physician, Principal Investigator,Institute for Clinical Research and Health Policy Studies,Professor, Tufts University School ofMedicine, Boston, MA
Reviewers
Jeffrey L. Anderson, MD, FACC—Associate Chief of Car-diology, Intermountain Medical Center, Murray, UT
James C. Blankenship, MD, MACC—Staff Physician, Di-rector, Cardiac Catheterization Laboratory, GeisingerMedical Center, Division of Cardiology, Danville, PA
Jeffrey A. Brinker, MD, FACC—Professor of Medicine,Johns Hopkins Hospital, Baltimore, MD
Alexandru I. Costea, MD—Associate Professor, Univer-sity of Cincinnati Medical Center, Cincinnati, OH
Ali E. Denktas, MD, FACC—Assistant Professor, BaylorCollege of Medicine, Houston, TX
Lloyd W. Klein, MD, FACC—Professor of Medicine,Melrose Park, IL
Frederick G. Kushner, MD, FACC—Clinical Professor,Tulane University Medical Center, Medical Director, HeartClinic of Louisiana, Marrero, LA
Glenn N. Levine, MD, FACC—Professor, Baylor Collegeof Medicine, Cardiology, Pearland, TX
David Joel Maron, MD, FACC—Professor of Medicineand Emergency Medicine, Stanford University School ofMedicine, Stanford, CA
James B. McClurken, MD, FACC—Director of ThoracicSurgery, Professor of Surgery Emeritus, Temple Univer-sity, School of Medicine, Richard A Reif Heart Institute,Doylestown Hospital, Doylestown, PA
Robert N. Piana, MD, FACC—Professor of Medicine,Cardiology, Vanderbilt University Medical Center, Nash-ville, TN
John A. Spertus, M.D, MPH, FACC—Adjunct Professor ofMedicine, Washington University School of Medicine, St.Louis, MO
Raymond F. Stainback, MD, FACC—Medical Director,Non-Invasive Cardiology Texas Heart Institute at BaylorSt. Luke’s Medical Center, Houston, TX
Robert C. Stoler, MD, FACC—Director of Cardiac Cath-eterization Laboratory, Cardiology Consultants of Texas,Dallas, TX
Todd C. Villines, MD, FACC—Co-Director of Cardiovas-cular Computed Tomography and Assistant Chief, Cardi-ology Service at Walter Reed Army Medical Center,Rockville, MD
David H. Wiener, MD, FACC—Professor of Medicine,Jefferson Medical College, Jefferson Heart Institute,Philadelphia, PA
ACC Appropriate Use Criteria Task Force
John U. Doherty, MD, FACC, FAHA—Co-Chair, AUC TaskForce, Professor of Medicine, Jefferson Medical College ofThomas Jefferson University, Philadelphia, PA
Gregory J. Dehmer, MD, MACC—Co-Chair, AUC TaskForce, Medical Director, Cardiovascular Services, CentralTexas Division, Baylor Scott & White Health, Temple, TX
Steven R. Bailey, MD, FACC, FSCAI, FAHA—Chair, Di-vision of Cardiology, Professor of Medicine and Radi-ology, Janey Briscoe Distinguished Chair, University ofTexas Health Sciences Center, San Antonio, TX
Nicole M. Bhave, MD, FACC—Clinical Assistant Profes-sor, Department of Internal Medicine, Division of Car-diovascular Medicine, University of MichiganCardiovascular Center, Ann Arbor, MI
Alan S. Brown, MD, FACC—Medical Director, MidwestHeart Disease Prevention Center, Advocate LutheranGeneral Hospital, Director, Division of Cardiology, ParkRidge, IL
Stacie L. Daugherty, MD, FACC—Associate Professor,Division of Cardiology, Department of Medicine, Univer-sity of Colorado School of Medicine, Denver, CO
Milind Y. Desai, MBBS, FACC—Associate Director,Clinical Investigations Heart and Vascular Institute,Cleveland Clinic, Cleveland, OH
Claire S. Duvernoy, MD, FACC—Cardiology SectionChief, Division of Cardiology, University of MichiganHealth System, Ann Arbor, MI
Linda D. Gillam, MD, FACC—Chair, Department of Car-diovascular Medicine, Morristown Medical Center, Mor-ristown, NJ
Robert C. Hendel, MD, FACC, FAHA—Director of Car-diac Imaging and Outpatient Services, Division of Cardi-ology, Miami University School of Medicine, Miami, FL
-
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-16
Christopher M. Kramer, MD, FACC, FAHA—FormerCo-Chair, AUC Task Force, Ruth C. Heede Professor ofCardiology & Radiology, and Director, CardiovascularImaging Center, University of Virginia Health System,Charlottesville, VA
Bruce D. Lindsay, MD, FACC—Professor of Cardiology,Cleveland Clinic Foundation of Cardiovascular Medicine,Cleveland, OH
Warren J. Manning, MD, FACC—Professor of Medicineand Radiology, Beth Israel Deaconess Medical Center,Division of Cardiology, Boston, MA
Manesh R. Patel, MD, FACC, FAHA—Former Chair,AUC Task Force, Assistant Professor of Medicine, Division
of Cardiology, Duke University Medical Center, Durham,NC
Ritu Sachdeva, MBBS, FACC—Associate Professor, Divi-sion of Pediatric Cardiology, Department of Pediatrics,Emory University School of Medicine, Children’s HealthCare of Atlanta, SibleyHeart Center Cardiology, Atlanta, GA
L. Samuel Wann, MD, MACC—Staff Cardiologist,Columbia St. Mary’s Healthcare, Milwaukee, WI
David E. Winchester, MD, FACC—Assistant Professor ofMedicine, University of Florida, Division of Cardiology,Gainesville, FL
Joseph M. Allen, MA—Team Leader, Clinical Policy andPathways,AmericanCollegeofCardiology,Washington,DC
-
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
17
APPENDIX B. RELATIONSHIPS WITH INDUSTRY (RWI) AND OTHER ENTITIES
The College and its partnering organizations rigorouslyavoid any actual, perceived, or potential conflicts of in-terest that might arise as a result of an outside relation-ship or personal interest of a member of the rating panel.Specifically, all panelists are asked to provide disclosurestatements of all relationships that might be perceived asreal or potential conflicts of interest. These statementswere reviewed by the Appropriate Use Criteria Task Force,
Participant Employment ConsultantSpeakBure
Writing G
Manesh R. Patel(Chair)
Duke University HealthSystem, Duke ClinicalResearch Institute—
Associate Professor ofMedicine, Director
Interventional Cardiologyand Catheterization Labs
None Non
John H. Calhoon University of Texas HealthScience Center at SanAntonio Department ofCardiothoracic Surgery,Heart and VascularInstitute Director—Professor and Chair,
Presidents Council Chairfor Excellence in Surgery
None Non
Gregory J.Dehmer
Baylor Scott & White-Temple Memorial, TexasA&M Health ScienceCenter College of
Medicine, Central TexasDivision—Clinical Professor
of Medicine, MedicalDirector, Cardiovascular
Services, Director,Cardiology Division
None Non
James AaronGrantham
Saint Luke’s Hospital—Associate Clinical
Professor, University ofMissouri–Kansas CitySchool of Medicine—
Director, CardiovascularDisease FellowshipProgram, Director,
Cardiovascular MedicalEducation
n AbbottVascular†
n Asahi-Intecc†n Boston
Scientific†n Bridgepoint
MedicalSystems†
n Medtronic†
Non
Thomas M.Maddox
VA Eastern ColoradoHealth Care System—National Director,
Associate Professor,Department of Medicine,Cardiology, University of
Colorado, ColoradoCardiovascular OutcomesResearch Consortium
None Non
APPROPRIATE USE CRITERIA FOR CORONARY REVAS
CORONARY SYNDROMES: MEMBERS OF THE WRITING
AND AUC TASK FORCE—RELATIONSHIPS WITH INDUS
discussed with all members of the rating panel at the face-to-face meeting, and updated and reviewed as necessary.The following is a table of relevant disclosures by therating panel and oversight working group members. Inaddition, to ensure complete transparency, a full list ofdisclosure information—including relationships notpertinent to this document—is available in the OnlineAppendix.
ersau
Ownership/Partnership/Principal
PersonalResearch
Institutional,Organizational,
or OtherFinancialBenefit
ExpertWitness
roup
e None None None None
e None None None None
e None None None None
e None n Abbott Vascular†n Asahi-Intecc†n Boston
Scientific†n Bridgepoint
MedicalSystems†
n Medtronic†
None None
e None None None None
Continued on the next page
CULARIZATION IN PATIENTS WITH ACUTE
GROUP, RATING PANEL, INDICATION REVIEWERS,
TRY AND OTHER ENTITIES (RELEVANT)
http://jaccjacc.acc.org/Clinical_Document/AUC_for_Coronary_Revasc_in%20Patients_with%20ACS_-_Comprehensive_RWI.docxhttp://jaccjacc.acc.org/Clinical_Document/AUC_for_Coronary_Revasc_in%20Patients_with%20ACS_-_Comprehensive_RWI.docx
-
Participant Employment ConsultantSpeakersBureau
Ownership/Partnership/Principal
PersonalResearch
Institutional,Organizational,
or OtherFinancialBenefit
ExpertWitness
David J. Maron Stanford University Schoolof Medicine—ClinicalProfessor of Medicine,Cardiovascular, Director,Preventive Cardiology
None None None None None None
Peter K. Smith Cardiovascular andThoracic Surgery, DukeUniversity—Professor ofSurgery, Division Chief
None None None None None None
Rating Panel
James C.Blankenship
Geisinger Medical Center,Division of Cardiology—Staff Physician, Director,Cardiac Catheterization
Laboratory
None None None n Abbott Vascular*n AstraZeneca*n Boston
Scientific*n GlaxoSmithKline*n Hamilton Health
Services*n Medinol LTD*n Orexigen Thera-
peutics/Takeda*n Stentys, Inc.*n Takeda
Pharmaceuticals
None None
Alfred A. Bove Temple University, LewisKatz School of Medicine,Heart and Vascular—Professor Emeritus
None None None n Merck Schering-Plough†
None None
Steven M.Bradley
VA Eastern ColoradoHealth Care System,
Division of Cardiology atthe University ofColorado—Staff
Cardiologist, AssistantProfessor of Medicine
None None None None None None
Larry S. Dean Medicine Regional HeartCenter University ofWashington School ofMedicine—Professor ofMedicine and Surgery,
Director
n Philips Medical† None None n EdwardsLifesciences†
None None
Peter L. Duffy First Health of theCarolinas, Reid Heart
Institute/Moore RegionalHospital—Director of
Quality for theCardiovascular Service Line
None n Vol-canoCorp†
None None None None
T. BruceFerguson, Jr.
East Carolina HeartInstitute, East Carolina
University, Department ofCardiovascular Sciences,Cardiothoracic Surgery—Professor of Thoracic
Surgery
None None n RFPi* n NovadaqTechnologies†
None None
Frederick L.Grover
University of Colorado,Department of
Cardiothoracic Surgery—Professor of
Cardiothoracic Surgery
n Somalution None None None None None
Robert A.Guyton
Emory University Schoolof Medicine, Division ofCardiothoracic Surgery,Department of Surgery,
Thoracic SurgeryResidency Program—Chiefof Cardiothoracic Surgery,
Professor of Surgery,Director
n Medtronic† None None None None None
Continued on the next page
APPENDIX B. CONTINUED
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-18
-
Participant Employment ConsultantSpeakersBureau
Ownership/Partnership/Principal
PersonalResearch
Institutional,Organizational,
or OtherFinancialBenefit
ExpertWitness
Mark A. Hlatky Stanford University Schoolof Medicine,
Cardiovascular Medicine,Health Services Research—
Professor of HeathResearch and Policy,Professor of Medicine
None None None n Sanofi-Aventis
None
Harold L. Lazar Boston University Schoolof Medicine,
Cardiothoracic ResearchProgram—Director
Professor ofCardiothoracic Surgery
None None None None None None
Vera H. Rigolin Northwestern UniversityFeinberg School of
Medicine, Cardiology—Professor
None None None None n Pfizer† None
Geoffrey A.Rose
Division of Cardiology,Sanger Heart and Vascular
Institute—Chief
None None None None n Medtronic None
Richard J.Shemin
Ronald Reagan UCLAMedical Center,
Cardiovascular Center—Director of Cardiac
Quality, Robert and KellyDay Professor, Chief ofCardiothoracic Surgery,Executive Vice Chair of
Surgery
n EdwardsLifesciences
n Sorin Group
None None None None None
Jacqueline E.Tamis-Holland
Saint Luke’s Hospital,Icahn School of Medicineat Mount Sinai HospitalMount Sinai—Director,Women’s Heart NY,
Assistant Professor ofMedicine, Director,
Interventional CardiologyFellowship
None None None None None None
Carl L. Tommaso Rush Medical College inChicago, Skokie IllinoisHospital, part of theNorthshore University
Health System—Directorof the CardiacCatheterization
Laboratory, AssociateProfessor of Medicine
None None None None None None
L. Samuel Wann Columbia St. Mary’sHealthcare—ClinicalCardiologist, MedicalDirector, Heart Failure
Program
n UnitedHealthcare
None None None None None
John B. Wong Tufts University School ofMedicine—Chief, Division
of Clinical DecisionMaking, Primary CarePhysician, Principal
Investigator, Institute forClinical Research andHealth Policy Studies,
Professor
None None None None None None
Continued on the next page
APPENDIX B. CONTINUED
J A C C V O L . - , N O . - , 2 0 1 6 Patel et al.- , 2 0 1 6 :- –- AUC for Coronary Revascularization in Patients With ACS
19
-
Participant Employment ConsultantSpeakersBureau
Ownership/Partnership/Principal
PersonalResearch
Institutional,Organizational,
or OtherFinancialBenefit
ExpertWitness
Reviewers
Jeffrey L.Anderson
Intermountain MedicalCenter—Associate Chief of
Cardiology
n Sanofi-Aventisn The Medicines
Company
None None None None None
Jeffrey A.Brinker
Johns Hopkins Hospital—Professor of Medicine
None None None None None None
Alexandru I.Costea
University of CincinnatiMedical Center—Associate
Professor
None None None None n BostonScientific*
None
Ali E. Denktas Baylor College ofMedicine—Assistant
Professor
None None None n AstraZenecan Edwards
Lifesciences
None None
Lloyd W. Klein Melrose Park—Professor ofMedicine
None None None None None None
Frederick G.Kushner
Tulane University MedicalCenter, Heart Clinic ofLouisiana—ClinicalProfessor, Medical
Director
None None None None None None
Glenn N. Levine Baylor College ofMedicine, Cardiology—
Professor
None None None None None None
David J. Maron Stanford University Schoolof Medicine—Professor ofMedicine and Emergency
Medicine
None None None None None None
James B.McClurken
Temple University, Schoolof Medicine, Richard A Reif
Heart Institute,Doylestown Hospital—Director of ThoracicSurgery, Professor ofSurgery Emeritus
None None None None None None
Robert N. Piana Vanderbilt UniversityMedical Center—Professorof Medicine, Cardiology
n Axio Researchn Harvard Clinical
ResearchInstitute
n W.L. Gore &Associates, Inc.
None None None None None
John A. Spertus Washington UniversitySchool of Medicine—Adjunct Professor of
Medicine
n Amgenn Bayer Health-
carePharmaceuticals
n Janssenn Novartisn Regeneron
None n HealthOutcomesSciences
None None None
Raymond F.Stainback
Texas Heart Institute atBaylor St. Luke’s MedicalCenter, Non-InvasiveCardiology—Medical
Director
None None None None None None
Robert C. Stoler Cardiology Consultants ofTexas—Director of Cardiac
CatheterizationLaboratory
n Boston Scientificn Medtronic
None None None None None
Continued on the next page
APPENDIX B. CONTINUED
Patel et al. J A C C V O L . - , N O . - , 2 0 1 6
AUC for Coronary Revascularization in Patients With ACS - , 2 0 1 6 :- –-20
-
Participant Employment ConsultantSpeakersBureau
Ownership/Partnership/Principal
PersonalResearch
Institutional,Organizational,
or OtherFinancialBenefit
ExpertWitness
Todd C. Villines Cardiology Service atWalter Reed Army MedicalCenter—Co-Director of
Cardiovascular ComputedTomography and Assistant
Chief
n BoehringerIngelheim†
None None None None None
David H. Wiener Jefferson Medical College,Jefferson Heart Institute—
Professor of Medicine
None None None None None None
Appropriate Use Criteria Task For
Related Documents