5/5/2010 1 Hernias: Who, What, When, Where, Why? J. Scott Roth, MD Chief, Gastrointestinal Surgery Director, Minimally Invasive Surgery University of Kentucky June 16, 2009 Objectives Identify patients at risk for hernias Understand the etiology and pathophysiology of hernias Review the demographics of patients with hernias Discuss common hernia locations and associated signs and symptoms Understand why (or why not) a hernia should be repaired Provide an overview of techniques for hernia repair and associated controversies Common hernia types Inguinal Hernia Hernia: The protrusion of an organ or other bodily structure through the wall that normally contains it; a rupture. Inguinal: Of, relating to, or located in the groin. Myopectineal Orifice of Fruchaud MPO Superior- arched fibers of int. oblique Inferior – iliac bone Medial – rectus abdominis m. Lateral – iliopsoas & iliopectineal arch Hesselbach’s Triangle

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

5/5/2010
1
Hernias: Who, What, When, Where, Why?
J. Scott Roth, MD
Chief, Gastrointestinal Surgery
Director, Minimally Invasive Surgery
University of Kentucky
June 16, 2009
Objectives
Identify patients at risk for herniasUnderstand the etiology and pathophysiology of
herniasReview the demographics of patients with herniasDiscuss common hernia locations and associated
signs and symptomsUnderstand why (or why not) a hernia should be
repairedProvide an overview of techniques for hernia repair
and associated controversies
Common hernia types Inguinal Hernia
Hernia:The protrusion of an organ or other bodily
structure through the wall that normally contains it; a rupture.; p
Inguinal:Of, relating to, or located in the groin.
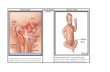
Myopectineal Orifice of Fruchaud
MPO
Superior- arched fibers of int. oblique
Inferior – iliac bone
Medial – rectus abdominis m. Lateral – iliopsoas & iliopectineal arch
Hesselbach’s Triangle

5/5/2010
2
Inguinal Hernia
U.S. Abdominal Hernia Repairs 2003
Inguinal hernia 770,000
Femoral hernia 30,000
Umbilical hernia 175,000
Epigastric, spigelian, etc. 80,000
Incisional hernia 105,000
Based on projected growth from 1996 National Survey of Ambulatory Surgery and National Center for Health Statistics
Hernia Repairs
Sex(%) Age(%)Procedure M F <15 15-44 45-64 >65
Inguinal Hernia 90 10 18 29 23 30Inguinal Hernia 90 10 18 29 23 30
Femoral Hernia 30 70 <1 19 29 48
Umbilical Hernia 57 33 13 33 36 17
Incisional Hernia 35 65 <1 25 35 39
Others –spig/epig 43 57 1 32 40 26
Hernia Management
Non-operative
Trus/Hernia belt
Operative
Medical Management

5/5/2010
3
External Support Watchful Waiting
Randomized Prospective Trial720 men over 5 years – repair vs. observation
Pain limiting activities 5.1% vs. 2.2% NS
23% WW patients cross over to repair23% WW patients cross over to repair17% cross over to WW from repair armComplications similar in initial repair/crossover rep.
2 patients with incarceration events – 1.8/1000 pt-yrsNo strangulation events
Fitzgibbons et al. JAMA 2006
Modern Hernia Repairs
Unchanged from 1890-1980
Primary tissue repair
Many repair types
Fundamentally similar
sutured repair, tension, prolonged recovery, disability, and high recurrence
“It will seem extremely bold to write about the radical repair of inguinal hernias, especially nowadays after all the publications in the past and the restless activity in the present. I thought of a surgical technique of physiological g q p y greconstruction of the inguinal canal, consisting of two openings, an abdominal and a subcutaneous, and of two walls, a posterior and an anterior, with the spermatic cord between them.”
Bassini 1889
Fathers of Inguinal Hernia Repair
Marcy
1871 – original paper on antiseptic hernia repair with closure of internal ring
JAMA 1887 The Cure of Hernia
Bassini
reported 1887, published 1889
Halsted
November 1889
Modified Bassini Repair

5/5/2010
4
Shouldice Hernia Repair
Repair established in 1952 at Shouldice hospital
Commonly referred to as the Bassini-Shouldice repair
Many similarities to Bassini except four layers ofMany similarities to Bassini except four layers of running suture to reconstruct posterior inguinal wall
Local Anesthesia – first to popularize inguinal herniorrhaphy under local anesthesia
Shouldice Repair
Shouldice Complications
Testicular atrophy – 0.36%Hematomas – 0.3%Infections – 1%Hydroceles – 0.7%yDysejaculation – 0.25%Mortality – 0.009%Recurrence rate - 0.5% primary; 1.5%recurrent
250,000 repairs over 20 years
CB McVayThe Pathologic Anatomy of the More Common
Hernias and their Anatomic Repair 1954
McVay Hernia RepairTension Free Hernia Repairs
The past twenty years
1980s – increase in numbers of tension free repairs
1990 b f t i f i1990s – number of tension free repairs surpasses sutured repairs

5/5/2010
5
Trends in Hernia Repair
200000
250000
300000
350000
Bassini
McVay
0
50000
100000
150000
200000
1970 1980 1990 1995 2000 2003
McVay
Shouldice
Lichtenstein
Laparoscopic
Groin Hernia Repairs
Procedure Type Number %
Lichtenstein 295,000 37%
Plug 270,000 34%
Laparoscopy 115,000 14%
Other Mesh 65,000 8%
Tissue rep 55,000 7%
Lichtenstein Hernia Repair
1984 – the tension-free hernioplasty project begun at the Lichtenstein Hernia Institute
Inguinal floor is reinforced by mesh prosthesisMesh placed between transversalis fascia and external oblique
aponeurosis8 x 16 cm polypropylene meshp yp pyRunning suture to inguinal ligamentTwo interrupted sutures superiorly(rectus sheath and internal oblique5cm of mesh lateral to internal ring
A multi-center experience with 6,764 Lichtenstein tension-free hernioplasties
Amid PK, Friis E, Horeyseck, Kux M. Hernia 1999;3(S12):47
6,764 Inguinal Hernia repairs
4 surgeons at 4 institutions
Recurrence rate 0.1 to 0.9 percent
Complications – infection, seroma, hematoma, neuralgia ~ 1%
Stoppa RepairGiant Prosthetic Reinforcement of the Visceral Sac
(GPRVS)
Polyester mesh to correct the structural weakness of the groin
Sutureless repair through self-stabilizationp g
Techniquemidline or pfannensteil incisionpreperitoneal approach
Stoppa et. al. Surg Clin N Am 1984
Stoppa Repair

5/5/2010
6
Stoppa RepairGiant Prosthetic Reinforcement of the Visceral Sac
(GPRVS)
Total patients 1992
Septic complications 2.1%
Follow up rate 79.2%
Follow up duration 2-12 years
Recurrence rate: overall 1.1%
primary hernia 0.56%
recurrent hernia 1.3%
Laparoscopic Inguinal Herniorrhaphy
First described in 1990
Techniques
Plug
Closure of internal ring
IPOM – intraperitoneal only of mesh
TAPP – transabdominal properitoneal
TEP – totally extraperitoneal

5/5/2010
7
Comparison of Conventional Anterior Surgery and Laparoscopic Surgery for Inguinal-Hernia Repair
Liem et al. NEJM 1997
Randomized Multicenter Trial – 87 surgeons
primary and initially recurrent unilateral inguinal herniasp y y g
487 Extraperitoneal laparoscopic repairs
507 Anterior repairs – Bassini(29%), Shouldice(22%),
Bassini-McVay(19%), McVay(9%),others
Comparison of Conventional Anterior Surgery and Laparoscopic Surgery for Inguinal-Hernia Repair
Liem et al. NEJM 1997
Comparison of Conventional Anterior Surgery and Laparoscopic Surgery for Inguinal-Hernia Repair
Liem et al. NEJM 1997
Comparison of Conventional Anterior Surgery and Laparoscopic Surgery for Inguinal-Hernia Repair
Liem et al. NEJM 1997
Recurrence rate
Open 31 (6%)Open 31 (6%)
Laparoscopic 17 (3%)
p=.05
Cost-Effectiveness of Extraperitoneal Laparoscopic Inguinal Hernia Repair: A Randomized Comparison with
Conventional HerniorrhaphyLiem et. al. Ann Surg 1997

5/5/2010
8
Meta-analysis of randomized clinical trials comparing open and laparoscopic inguinal hernia repair
Memon et al. Br J Surg 2003
Meta-analysis of randomized clinical trials comparing open and laparoscopic inguinal hernia repair
Memon et al. Br J Surg 2003
ConclusionsLaparoscopic Hernia repair
decreased hospital stayquicker return to normal activity/workq yfewer postoperative complicationsLonger operating timestrend toward higher short term recurrences in
laparoscopic (NS)
Study Design
14 Veterans Affairs medical centers
2164 patients randomly assigned
Lichtenstein technique
Laparoscopic repair (TAPP or TEP)
2 year follow up

5/5/2010
9
Open Mesh Versus Laparoscopic Mesh Repair of Inguinal HerniaNeumayer et al. NEJM 2004
Primary Hernia recurrences
Laparoscopic 79/781 (10.1%)
Lichtenstein 30/756 (4.0%)
Recurrent Hernia Rerecurrences
Laparoscopic 8/81 (10.0%)
Lichtenstein 11/78 (14.1%)
Open Mesh Versus Laparoscopic Mesh Repair of Inguinal HerniaNeumayer et al. NEJM 2004
Highly experienced Surgeons (>250 cases)Primary Hernia Recurrences Recurrent Hernia recurrence
Lap 13/253 (5.1%) Lap 1/28 (3.6%)Open 26/635 (4.1%) Open 11/64 (17.2%)
Inexperienced SurgeonsPrimary Hernia Recurrences Recurrent Hernia Recurrence
Lap 65/528 (12.3%) no statistical powerOpen 3/121 (2.5%)
97/989 (10%) Lap patients converted to open – various reasons

5/5/2010
10
…“a hernia repair is equivalent to repairing drywall”……
The Baltimore Sun
August 13, 2006
Incisional Hernias
Common clinical problem
More than 10% of laparotomy incisions
1.3 million laparotomies per year
150,000 hernias created annually
6-15% incidence of incarceration
2% incidence of strangulation
Biology of Hernias
Mechanisms of Recurrenceinfection, lateral detachment of mesh, inadequate mesh fixation, inadequate mesh, inadequate mesh overlap
Inlay with 2.5 fold increased recurrence compared to underlay, sandwich, overlay
Awad et al. JACS 201(1):132-140, 2005
Smokers with a 4 Fold increase in Incisional Hernia formation
Sorenseon et al. Arch Surg 140:119-123, 2005
Decreased Collagen I/III ratio associated with hernia formation
Junge et al. Langenbecks Arch Surg 389:17-22, 2004
Incisional Hernia Repairs in Non-Federal US Hospitals
Carlson et al. Hernia 2008
Flum et al. Ann Surg 137(1):129-135, 2003
Progression to Hernia RecurrenceWashington State Database 1987-1999
10,822 patients
12%5 years
23%13 years
Flum et al. Ann Surg 137(1):129-135, 2003
5 years

5/5/2010
11
Rates of Reoperation Primary vs. Mesh Repair
Luijendijk RW, Luijendijk RW, et al; NEJM, et al; NEJM, 20002000
Progression to Reoperation by use of mesh
Open Incisional Hernia Repair
• Overlay
• Inlay
• Underlay
• Sandwich
• Rives-Stoppa technique
Pascal’s Principle
Blaise Pascal (1623-1662)
liquid in a closed container at rest t it h ith t ltransmits a pressure change without loss to the walls
pressure in a gas or fluid is the same in all directions
Physiology of Hernias

5/5/2010
12
Law of LaPlace
Wall tension(T) is proportional to pressure(P) and radius(R)
Increased Radius Increased tension
T i l ti l t ll thi k (M)T inversely proportional to wall thickness(M)
T= P x R / 2M
T= tensionP= pressureR= radiusM= wall thickness
Physiology of Hernias
r
25
30
35
40
Complications and Recurrence are Decreased with Laparoscopic Approach
0
5
10
15
20
25
Complications Recurrence
LapOpen
Hiatal HerniasHiatal Hernias
22--5% of population 5% of population
Pathophysiology poorly understoodPathophysiology poorly understood
95% of HHs are Sliding Type I hernias95% of HHs are Sliding Type I hernias
69% asymptomatic69% asymptomatic
27% small HH with reflux27% small HH with reflux
35% large(>2cm) with reflux35% large(>2cm) with reflux
Paraesophageal hernias 2Paraesophageal hernias 2--5%(types 2,3,4)5%(types 2,3,4)
Hiatal Hernias: definedHiatal Hernias: defined
Type 1: GE Junction intermittently migrates Type 1: GE Junction intermittently migrates into mediastinuminto mediastinum
Type 2: GE Junction anchored at Type 2: GE Junction anchored at diaphragm with herniation of adjacent diaphragm with herniation of adjacent p g jp g jstomach into mediastinumstomach into mediastinum
Type 3: Combined Type 1 and 2Type 3: Combined Type 1 and 2Type 4: Viscera other than stomach in Type 4: Viscera other than stomach in
mediastinummediastinum

5/5/2010
13
Hiatal Hernia: Type 1Hiatal Hernia: Type 1
Type 1: GE Junction intermittently migrates into mediastinumType 1: GE Junction intermittently migrates into mediastinum
Hiatal Hernia: Type 2Hiatal Hernia: Type 2
Type 2: GE Junction anchored at diaphragm with herniation of adjacent Type 2: GE Junction anchored at diaphragm with herniation of adjacent stomach into mediastinumstomach into mediastinum
Type IIIType III
Type 3: Combined Type 1 and 2Type 3: Combined Type 1 and 2
Type IVType IV
Type 4: Viscera other than stomach in MediastinumType 4: Viscera other than stomach in Mediastinum
Paraesophageal Hernia Paraesophageal Hernia Types 2,3 & 4Types 2,3 & 4
30% present with severe complications if untreated30% present with severe complications if untreated
Hill, Tobias, Arch Surg 96:735Hill, Tobias, Arch Surg 96:735--744, 1968744, 1968
Tremendous controversyTremendous controversy
EvaluationEvaluationEvaluationEvaluation
When to operate When to operate –– if at allif at all
Which operationWhich operation

5/5/2010
14
PresentationPresentation
Often asymptomaticOften asymptomatic
Suspicion based on Suspicion based on imagingimaging
Volvulus
Asymptomatic Paraesophageal Hernia Asymptomatic Paraesophageal Hernia RepairRepair
Paraesophageal Hernias: Operation or ObservationParaesophageal Hernias: Operation or ObservationStylopoulos et al Annals of Surgery 236(4): 492Stylopoulos et al Annals of Surgery 236(4): 492--501, 2002501, 2002
Markov ModelMarkov ModelMinimally symptomatic type 2 and 3 HHs (reflux sx only)Minimally symptomatic type 2 and 3 HHs (reflux sx only)Pooled data for elective repair death rate (0Pooled data for elective repair death rate (0--5.2%)5.2%)1997 NIS database mortality for emergency repair (5.4%)1997 NIS database mortality for emergency repair (5.4%)
Literature suggests 17%Literature suggests 17%Literature suggests 17%Literature suggests 17%WW WW –– pooled risk of need for emergent repair 1.16% annuallypooled risk of need for emergent repair 1.16% annuallyAnnual risk of recurrence 1.9%Annual risk of recurrence 1.9%
Elective repair results in reduction of 0.13 Quality of Life Years Elective repair results in reduction of 0.13 Quality of Life Years
Watchful waiting preferred treatment in 83% of patientsWatchful waiting preferred treatment in 83% of patients
Paraesophageal Hernia Repair Mortality in Octogenarians
Poulose et al. J Gastrointest Surg 12:1888-1892, 2008
2005 National Inpatient Survey Database
Paraesophageal Hernias
excluded congenital or traumatic
1005 patients1005 patients
30 day outcomes
Recurrences/readmissions not evaluated
Includes Open and Laparoscopic Operations
Paraesophageal Hernia Repair Mortality in Octogenarians
Poulose et al. J Gastrointest Surg 12:1888-1892, 2008

5/5/2010
15
Conclusions
Hernias are common and frequently encountered
Most abdominal hernias should be repaired electively to avoid devastating complications
Watchful waiting is appropriate in high riskWatchful waiting is appropriate in high risk ASYMPTOMATIC patients
All symptomatic hernias should be repaired
Minimally Invasive Surgery offers improved outcomes and quicker return to activities for all hernia repairs
THANK YOU
J. Scott Roth, MD
Related Documents