1 19-1 Chapter 19 Cardiovascular System Blood: Functions 19-2 Plasma • Liquid part of blood. – Colloid: liquid containing suspended substances that don’t settle out of solution – 91% water. Remainder proteins, ions, nutrients, waste products, gases, regulatory substances • Proteins: – Albumins: viscosity, osmotic pressure, buffer, transports fatty acids, free bilirubin, thyroid hormones – Globulins: Transports lipids, carbohydrates, hormones, ions, antibodies, and complement – Fibrinogen: blood clotting

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

1
19-1
Chapter 19Cardiovascular System
Blood: Functions
19-2
Plasma• Liquid part of blood.
– Colloid: liquid containing suspended substances that don’t settle out of solution
– 91% water. Remainder proteins, ions, nutrients, waste products, gases, regulatory substances
• Proteins:– Albumins: viscosity, osmotic pressure, buffer,
transports fatty acids, free bilirubin, thyroid hormones
– Globulins: Transports lipids, carbohydrates, hormones, ions, antibodies, and complement
– Fibrinogen: blood clotting

2
19-3
Plasma, cont.• Ions: involved in osmosis, membrane potentials,
and acid-base balance• Nutrients: glucose, amino acids, triacylglycerol,
cholesterol, vitamins• Waste Products:
– Urea, uric acid, creatinine, ammonia salts. Breakdown products of protein metabolism
– Bilirubin. Breakdown product of RBCs– Lactic acid. End product of anaerobic
respiration• Gases: oxygen, carbon dioxide, and inert nitrogen• Regulatory substances: hormones, enzymes
19-4
Composition of Blood

3
19-5
Formed Elements• Red blood cells (erythrocytes). Biconcave discs,
anucleate, contain hemoglobin; transports oxygen and carbon dioxide.
• White blood cells (leukocytes)– Granulocytes: cytoplasm contains large
granules; have multi-lobed nuclei. Three distinctive types: neutrophils, eosinophils, basophils
– Agranulocytes: cytoplasm contains small granules and nuclei that are not lobed. Two distinctive types: lymphocytes and monocytes
• Platelets (thrombocytes). Cell fragment. Form platelet plugs, release chemicals necessary for blood clotting.
19-6

4
19-7
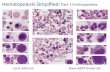
Hematopoiesis
19-8
Red Blood Cells
• Found in higher concentration in male than in female plasma
• Components– 1/3 Hemoglobin– 2/3 Lipids, ATP,
carbonic anhydrase

5
19-9
Hemoglobin• Types of hemoglobin
– Embryonic and fetal: have greater attraction for oxygen than adult. Fetal production stops after birth.
– Adult• Oxyhemoglobin:
transporting oxygen• Dexoyhemoglobin• Carbaminohemoglobin:
transporting carbon dioxide
19-10
Erythropoiesis
• RBCs last 120 days in circulation (enucleated)• Production of red blood cells
– (Stem cells → proerythroblasts → early erythroblasts →intermediate erythroblasts → late erythroblasts → reticulocytes)
• Erythropoietin: hormone stimulates RBC production; produced by kidneys in response to low blood O2 levels.

6
19-11
Hemoglobin Breakdown
19-12
• Neutrophils: after leaving bone marrow, stay in circulation 10-12 hours then move into other tissues. Become motile, phagocytize bacteria, antigen-antibody complexes and other foreign matter. Secrete lysozyme. Last 1-2 days.
• Eosinophils. Leave circulation and enter tissues during inflammatory response. Prevalent in allergicreactions. Destroy inflammatory chemicals like histamine. Release chemicals that help destroy Parasites (tapeworms, flukes, pinworms, and hookworms.)

7
19-13
•Basophils: least common. Leave circulation and migrate through tissues, play a role in both inflammatory responseand allergic reactions. Produce histamine and heparin.
•Lymphocytes: produced in red bone marrow but then migrate to lymphatic tissues and proliferate. Responsible for antibody production. Studied extensively with the immune system.
•Monocytes: remain in circulation for 3 days, leave circulation and become macrophages. Phagocytic cells. Can break down antigens and present them to lymphocytes for recognition.
19-14
Platelets• Cell fragments pinched off
from megakaryocytes in red bone marrow
• Surface glycoproteins and proteins allow adhesion to other molecules; i.e., collagen
• Important in preventing blood loss– Platelet plugs– Promoting formation and
contraction of clots

8
19-15
Hemostasis
• Arrest of bleeding• Events preventing excessive blood loss
– Vascular spasm: Vasoconstriction of damaged blood vessels. Can occlude small vessels. Caused by thromboxanes from platelets and endothelin from damaged endothelial cells.
– Platelet plug formation – Coagulation or blood clotting
19-16
Platelet Plug Formation1. Platelet adhesion. Occurs
when von Willebrand factor connects collagen and platelets.
2. Platelet release reaction. The release of ADP, thromboxanes, and other chemicals that activate other platelets. They in turn undergo the release reaction: cascade effect.
3. Platelet aggregation. Activated platelets express surface receptors that bind fibrinogen (protein found in plasma). Fibrinogen forms a bridge between platelets: platelet plug.
4. Expression of coagulation factor V and phospholipids. Important for coagulation

9
19-17
Coagulation• Stages
1.Activation of prothrombinase2.Conversion of prothrombin to
thrombin3.Conversion of fibrinogen to
fibrin (See Handout)• Coagulation factors.
– Proteins found in plasma. – Circulate in inactive state until
tissues are injured. – Damaged tissues and platelets
produce chemicals that begin activation of the factors.
• Pathways– Extrinsic– Intrinsic
• Result: blood clot. A network of threadlike fibrin fibers, trapped blood cells, platelets and fluid
19-18
Clot Formation

10
19-19
Control of Clot Formation• Anticoagulants: prevent coagulation factors from
initiating clot formation. • .• Anticoagulants
– Antithrombin: produced by liver, slowly inactivates thrombin
– Heparin: produced by basophils and endothelial cells. Increases effectiveness of antithrombin
– Prostacyclin: prostaglandin derivate from endothelial cells. Causes vasodilation and inhibits release of coagulating factors from platelets
19-20
Fibrinolysis• Clot retraction. Fibrin
threads of clot attached to blood vessel walls. Platelets produce processes that attach to fibrin threads. Actin and myosin molecules within platelets contract, pulling edges of wound together and squeezing out serum.
• Clot dissolved by activity of plasmin, an enzyme which hydrolyzes fibrin

11
19-21
Blood Grouping
• (Transfusion: transfer of blood or blood components from one individual to another)
• Determined by antigens (agglutinogens) on surface of RBCs
• Antibodies (agglutinins) can bind to RBC antigens, resulting in agglutination(clumping) or hemolysis (rupture) of RBCs
• Groups: ABO and Rh
19-22
ABO Blood Groups

12
19-23
Transfusion
• Type A blood has anti-B antibodies; Type B blood has anti-A antibodies
• (Suggested that these antibodies are present because of exposure to A and B antigens on bacteria and food)
• Donor: gives blood. Recipient: receives blood• Type O as “universal donor”. (Can actually cause
transfusion reactions because of antibodies in O blood plasma)
19-24
Rh Blood Group• First studied in rhesus monkeys• Types
– Rh positive: Have these antigens present on surface of RBCs– Rh negative: Do not have these antigens present
• Hemolytic disease of the newborn (HDN)– Rh positive fetus, Rh negative mother.– Late in pregnancy, Rh antigens of fetus cross placenta (through a
tear in placenta or during delivery); mother creates antiRh antibodies (primary response)
– Second Rh positive pregnancy might initiate secondary response and HDN (potentially fatal to fetus since antibodies to its RBCswould cross the placenta from the mother to the fetus, destroying fetal RBCs).
– Injection of RhoGAM. Contains antibodies against Rh antigens. Antibodies attach to any fetal RBCs and they are destroyed.

13
19-25
Erythroblastosis Fetalis
19-26
Diagnostic Blood Tests• Type and Crossmatch: determination of ABO
and Rh blood types. Red cells tested against antibodies
• Complete Blood Count– Red Blood Count: number of RBCs/ microliter of
blood– Hemoglobin Measurement: grams of hemoglobin/100
mL of blood. For a male, 14-18, female 12-16 g/100 mL
– Hematocrit Measurement: percent of blood that is RBCs
– White Blood Cell Count: 5,000-10,000 /microliter of blood

14
19-27
• Differential White Blood Count: determines percentage of each of the five types of WBC– Neutrophils: 60-70%– Lymphocytes: 20-30%– Monocytes: 2-8%– Eosinophils: 1-4%– Basophils: 0.5-1%
• Clotting– Platelet Count: 250,000- 400,000/microliter– Prothrombin Time Measurement: measures how long
it takes for blood to start clotting. 9-12 seconds. To test, thromboplastin is added to whole plasma
• Blood Chemistry: composition of materials dissolved or suspended in the plasma. Used to assess functioning of many body systems
Related Documents