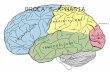
APHASIA --------------- OUTLINE What is aphasia? • Communication process Does the patient have aphasia ? • If so, where is the lesion? • What kind of aphasia is this? Is it important to diagnose aphasia? • Localization • Treatment • Prognosis • Functional state of the patient

Welcome message from author
This document is posted to help you gain knowledge. Please leave a comment to let me know what you think about it! Share it to your friends and learn new things together.
Transcript

APHASIA --------------- OUTLINE
What is aphasia?
• Communication process
Does the patient have aphasia ?
• If so, where is the lesion?• What kind of aphasia is this?• What is the etiology?
Is it important to diagnose aphasia?
• Localization• Treatment• Prognosis• Functional state of the patient

–Acquired disorder of language due to brain damage. In form of impaired ability to use or comprehend words.
Aphasia is an acquired communication disorder that impairs a person's ability to process language.
Aphasia impairs the ability to speak and understand others, and most people with aphasia experience difficulty reading and writing.
This class of language disorder ranges from having difficulty remembering words to being completely unable to speak, read, or write.
Encompassed under the term aphasia are selective, acquired disorders of reading (alexia) or writing (agraphia).
• Aphasia causes problems with any or all of the following communications abilities: speaking, listening, reading, and writing.
APHASIA

• Aphasia does not include:• Developmental disorders of
language, often called dysphasia in the united states.
• Purely motor speech disorders, limited to articulation of speech via the oral-motor apparatus, referred to as stuttering, dysarthria, and verbal apraxia.
• Disorders of language that are secondary to primary thought disorders, such as schizophrenia.
• Does not affect intelligence.

Communication
• Communication is a multidimensional dynamic process that allows human beings to interact with their environment.
• Through communication, people are able to express thoughts, needs, and emotions. Communication is a complex process that involves cerebration, cognition, hearing, speech production, and motor coordination.
• Evaluation of a communication disorder includes consideration of all aspects of the normal communication process

Language
• Language is the transformation of thoughts into meaningful symbols communicated by speech, writing, or gestures.

Anatomical basis of language
• Language is a higher cortical function lateralize to the dominant hemisphere ( left) supplied by MCA which is branch of anterior circulation (ICA).

Dominant hemisphere
• Language lateralize to the dominant hemisphere:
o80% of people are right handed.o 96-99% of right handed people in the left hemi sphere.o 60% of left handed people also lateralize to the left o 25% of left handed shows right dominancy. o the remaining are mixed dominancy.

Dominant hemisphere
• Many naturally left-handed children are trained to use the right hand for writing– in determining handedness, one must ask which hand is
preferred for throwing a ball– threading a needle, sewing– using a tennis racket or hammer– which eye is used for sighting a target with a rifle or other
instrument. • Pharmacological methods: injecting anesthetic in left
carotid artery and observe if aphasia occur

Middle Cerebral Artery
• It is the largest branch of internal carotid artery it gives off:• Lentriculostriate – perforating arteries: supply ant. Limb of I. capsule and
basal nuclei• Cortical branches
– Temporal branch– Majority of lateral aspect of:
» Frontal » Parietal
• MCA leasion: – Contralateral hemiparesis– Contralateral sensory deficits– Ipsilateral/homonymous hemianopsia– Gaze preference– Agnosia– R CVA Contralateral Neglect– Extremity weakness (upper>lower)

Analysis of language and definitions
• Language: complex system of communication symbols and rules for their use.
• Speech: the articulation and phonation of language sounds. • Motor speech disorders:
– Dysarthrias: disorder of articulation of single sounds, consistent. – Dysphonia: voice disorder – Stuttering – Apraxia of speech: misarticulation of phonemes,especially
consonant sounds. inconsistent distortions and substitutions of phonemes.

Analysis of language and definitions ,,,,,,Cont.....
• Paraphrasia: presence of errors in the patient’s speech output.– Semantic: substitution of an incorrect word from same group (e.g., “fork” for
“spoon”).
– Phonemic: involving substitution of an incorrect sound (e.g., “shoon” for “spoon”)
• Syntax: the grammatical construction of phrases and sentences.• Pragmatic : proper use of speech and language in a conversational
setting, including pausing while others are speaking, taking turns properly, and responding to questions.
• morphology is the use of appropriate word endings and connector words for tenses, possessives, and singular versus plural

Analysis of language and definitions ,,,,,Cont.....
• Neologisms: involve nonexistent word forms• Jargon speech: A pattern of paraphasic errors and
neologisms that so contaminate speech that the meaning cannot be discerned.
• word salad: normal speech morphology, normal sentence structure but incoherent content.
• Telegraphic: often producing the principal, meaning-containing nouns and verbs but omitting small grammatical words and morphemes.

Pathogenesis and etiology of aphasia
• Vascular lesions:– Ischemic strokes, the most common cause of aphasia.– The clinical features of the aphasia are of crucial importance to
the vascular diagnosis. – hemorrhagic strokes an important cause of aphasia, most
commonly the basal ganglionic hemorrhages associated with hypertension.
– AVM, drugs, may cause hemorrhages– amyloid angiopathy. – cerebral vasculitis.

Pathogenesis and etiology of aphasia
• Traumatic brain injury– Cerebral contusions– depressed skull fractures– hematomas of the intracerebral, subdural, and epidural spaces
– Gunshot wounds produce focal aphasic syndromes• Tumors of the left hemisphere
– The onset of the aphasia is gradual, and edema and mass effect may result in other cognitive deficits.
– Enlarging tumor may be difficult to distinguish from a diffuse encephalopathy or early dementia.

Pathogenesis and etiology of aphasia
• Infections of the nervous system– Brain abscesses can mimic tumors and present with aphasia– Chronic infections, such as tuberculosis or syphilis, can result in focal
abnormalities.– Herpes simplex encephalitis has a predilection for the temporal lobe
and orbital frontal cortex, and aphasia can be an early manifestation, along with headache, confusion, fever, and seizures.• Aphasia often is a permanent sequel in survivors of herpes encephalitis.
– AIDS: either the AIDS dementia complex or the opportunistic infections.

Pathogenesis and etiology of aphasia
• degenerative central nervous system diseases– Alzheimer’s disease may be more common in familial cases and may
predict poor prognosis.
– dialysis dementia syndrome: started with stuttering followed by true aphasia and dementia
• Seizures: – Epileptic aphasia is important to recognize because anticonvulsant drug
therapy can prevent the episodes

Broca Aphasia
• speech pattern:– Effortful, difficulty initiating speech– Non fluent – Hesitant – telegraphic speech. An example is “wife come hospital.”
• deficiency, particularly in the comprehension of complex syntax.• Third alexia: Reading often is impaired• Writing: right hand could be paralyzed, left hand apraxia • Associated neurological deficits
– right hemiparesis, hemisensory loss, – apraxia of the oral apparatus and the nonparalyzed left limbs
• frequent association with depression – Typically they are aware of and frustrated by their deficits.

Broca Aphasia
• Lesion:– Traditional Broca Area” Brodmann’s 44&45”– left frontoparietal lesions– territory of the upper division of the left middle cerebral artery

Wernicke’s Aphasia
• the opposite of Broca’s aphasia in that expressive speech is fluent but comprehension is impaired.
• speech pattern:– Effortless– excessively fluent (logorrhea).– Paragrammatism:
• speaker of a foreign language would notice nothing a miss, but a listener who shares the patient’s language detects speech empty of meaning, containing verbal paraphasias, neologisms, and jargon productions.
• Naming is deficient, often with bizarre, paraphasic substitutions for the correct name
• patients show greater deficit in one modality than in the other.

Wernicke’s Aphasia
• Writing samples are especially useful in the detection of mild Wernicke’s aphasia.
• Associated signs are limited in Wernicke’s aphasia– Most have no elementary motor or sensory deficits– right homonymous hemianopia may be present.
• Depression is less common; many Wernicke’s aphasics seem unaware of or unconcerned about their communicative deficits.
• The lesions – posterior portion of the superior temporal gyrus, sometimes extending into the
inferior parietal lobule.– Damage to Wernicke’s area (Brodmann’s area 22)– Wernicke’s area lies within the territory of the inferior division of the left middle
cerebral artery.

Global Aphasia
• summation of the deficits of Broca’s aphasia and Wernicke’s aphasia.
• Speech is nonfluent or mute, but comprehension also is poor, as are naming, repetition, reading, and writing.
• Most patients have dense right hemiparesis, hemisensory loss, and often hemianopia.

Conduction Aphasia
• striking deficit of repetition.• relatively normal spontaneous speech, although
some make literal paraphasic errors and hesitate frequently for self-correction.
• Naming may be impaired, but auditory comprehension is preserved.
• Associated deficits:– right-sided sensory loss may be present
• involvement of the arcuate fasciculus

Anomic Aphasia
• aphasic syndromes in which naming, or access to the internal lexicon, is the principal deficit.
• Spontaneous speech except for pauses produced by the inability to name.
• Comprehension, repetition, reading, and writing are intact, except for the same word-finding difficulty in written productions.
• less specific in localization• Anomic aphasia thus serves as an indicator of left
hemisphere or diffuse brain disease.

Transcortical
• repetition is normal• presumably because the causative lesions do not disrupt the perisylvian language
circuit from Wernicke’s area through the arcuate fasciculus to Broca’s area.
• Three types: 1.Isolation syndrome:
• global aphasia in which the patient repeats, often echolalically• occurring predominantly with large Watershed infarctions of the left hemisphere or both
hemispheres that spare the perisylvian cortex, or in advanced dementias.
2. Transcortical motor aphasia:• analog of Broca’s, speech is hesitant or telegraphic, comprehension is relatively spared, but
repetition is fluent.• deep frontal white matter, or in the medial frontal region, in territory of ANTERIOR CEREBRAL
ARTERY.
3. Transcortical sensory aphasia:• analog of Wernicke’s aphasia, repetition intact• occurring with strokes of the left temporo-occipital area and in dementias.

Disconnection syndromes:
loss of integration among deferent lobes due to lesion affecting the connecting pathways that leads to disorganized normal function.
• Intrahemespheric disconnection1. Conduction (also called "central") aphasia.2. Buccal Lingual and Sympathetic apraxia in Broca's aphasia. Destruction of the link
between left and right motor association cortices causes an apraxia of commanded movements of the left hand and weakness of right brachiofacial weakness, apraxia of tongue and lips.
3. Pure word deafness.
• Interhemespheric disconnection1.alexia without agraphia2.Left side apraxia3.Agenesis of corpus callosum: right and left visual fields can’t
match presented objects

Gerstmann’s syndrome
• Angular gyrus as the site of lesions
• Consist of :• Alexia• Agraphia• Right Left
Disorientation• Acalculia• Finger Agnosia

Clinical Evaluation of AphasiaHistory
– Onset, Frequency, Duration• Strokes are characterized by the abrupt onset of a neurological deficit in
a patient with vascular risk factors.• precise temporal profile is important
– Most embolic strokes are sudden and maximal at onset, whereas thrombotic strokes typically wax and wane or increase in steps.
– The sudden onset of Wernicke’s aphasia nearly always indicates an embolus to the inferior division of the left middle cerebral artery.
• Global aphasia may be caused by an embolus to the middle cerebral artery stem, thrombosis of the internal carotid artery, or even a hemorrhage into the deep basal ganglia. – deficits tend to worsen gradually over minutes to hours, in contrast with
the sudden or stepwise onset of ischemic strokes.• Cont,,,,,,

– Baseline: difficulty in articulation, vision, hearing, intelligence, education and literacy” reading and writing”, psychological diseases, memory deficit- dementia
– Progression- improved , slowly progressed – Associated symptoms– Etiological factors: DM, Hypertension, AF, AIDS, Fever,
vomiting, Trauma – Associated symptoms: other neurological symptoms
“ headache, loss of vision, weakness and motor deficit, sensory loss, epilepsy, cognitive defects”
Clinical Evaluation of Aphasia ,,,,,,, CONTHistory

Clinical Evaluation of Aphasia ,,,,,,,,, CONTExamination:
• Examination of Other Cortical Functionso Consciousness o Cognitive Function
o Mental Status and MemoryoOrientation o Alertness; Attention and Concentrationo Judgment and reasoning
o Thought Contents o Complete Neurological Exam
o aimed to localize the lesion “ Associated Deficit” o aimed to define the etiology.
– Psychiatric evaluation: acute encephalopathy or delirium• accompanying behavioral disturbances, such as agitation, hallucinations, drowsiness, or excitement, and
cognitive difficulties, such as disorientation, memory loss, or delusional thinking
– language assessment:oBedside Language Examination
o cont,,,

Clinical Evaluation of Aphasia ,,,,,,,,, CONTExamination:
– Content of speech– Paraphrasia– telegraphic speech– conjunctions and proposition use, syntax, and morphology of speech. – Neologism– Jargon of speech – Word salad – Assess pragmatism
– Other Useful Tests • For neurologists, the most helpful battery is the Boston Diagnostic Aphasia Examination • the Western Aphasia Battery.
– Both tests provide subtest information analogous to that obtained with the bedside examination, and therefore meaningful to neurologists, as well as aphasia syndrome classification.
– clinical systemic examination• clues to etiology
– AF– Hypertension and DM– Atherosclerosis – Signs increased intra cranial pressure –papilloedema, brain metastasis – AIDS – evidence of trauma– self injury and loss of sphenctric control –epilepsy
• Cont,,,,,

Clinical Evaluation of Aphasia ,,,,,,,, CONTDiagnostics:
– CBC and Chemistry Panel, PT, PTT, INR –May give clue to etiology and benefit in differentiating aphasia from
– ECG – IMAGING:
• CT W/WO CONTRAST • MRI• PET AND SPECT – Academic
– EEG– Carotid Doppler and MRA
• Referrals – Neurology – Speech-language pathologists
• Follow-up examinations also are helpful– the evolution of a neurological deficit over time is the most important clue to the
specific disease process.• Cont,,,,,,

Bedside Language Examination
D. Frank Benson and Norman, updated by Alexander and Benson (1997)

1. Spontaneous speech
• elicited by asking the patient to describe the weather or the reason for coming to the doctor.
• Counting or listing days of the week. • Signs:
– Fluency: Fluent speech flows rapidly and effortlessly; nonfluent speech is uttered in single words or short phrases, with frequent pauses and hesitations.
– initiation difficulty– word-finding difficulties – pauses

2. Naming
• asking the patient to name a few items in each of thee following category– objects– Object parts – Colors – Body parts – Pictures – Proper names of persons
• The examiner should ask questions to be sure that the patient recognizes the items or people that he or she cannot name.

3. Auditory comprehension
• follow a series of commands of one, two, and three steps. • one-step command is “Stick out your tongue”• two-step command is “Hold up your left thumb and close your eyes.”• The responses to nonsense questions (e.g., “Do you vomit every day?”) quickly
establish whether the patient comprehends. – Successful following of commands ensures adequate comprehension, at least at
this simple level.– failure to follow commands does not automatically establish a loss of
comprehension. The patient must hear the command, understand the language the examiner speaks, and possess the motor ability to execute it, including the absence of apraxia. • Because apraxia is difficult to exclude with confidence:
– it is advisable to test comprehension by tasks that do not require a motor act, such as yes/no questions, or by commands that require only a pointing response.

4. Repetition
• aphasic persons have special difficulty with grammatically complex sentences.
• grammatically complex sentences; “no ifs, ands, or buts” is especially challenging for aphasics.
– aphasics can repeat familiar or “high-probability” phrases much better than unfamiliar ones.
– whispering a phrase in the patient’s ear, as in a hearing test, may help cue the patient to attempt repetition.

5. Reading
• examiner must have some idea of the patient’s previous reading ability.– Reading should be tested both aloud and for comprehension.– The examiner should carry a few printed commands to facilitate
a rapid comparison of auditory and reading comprehension.

6. writing
• Spontaneous writing, such as a sentence describing why the patient has come for examination, is especially sensitive for the detection of language difficulty.
writing to dictation and copying should be tested.– A writing specimen may be the most sensitive indicator of mild
aphasia, and it provides a permanent record for future comparison.
• look for spelling errors, structural errors, and apraxia.

RECOVERY AND REHABILITATION OFTHE PATIENT WITH APHASIA
•The sudden onset of aphasia would be expected to cause great apprehension, but except for cases of pure or almost pure motor disorders of speech, most patients show remarkably little concern.

RECOVERY AND REHABILITATION OFTHE PATIENT WITH APHASIA
• After stroke – If symptoms last longer than two or three months, complete recovery is unlikely– People continue to improve over a period of time– Slow process for both patient and FAMILY– Need to learn compensatory strategies for communicating
• Global aphasia recovery occur after 6 months • The aphasia type often changes during recovery: Global aphasia
evolves into Broca’s aphasia, and Wernicke’s aphasia into conduction or anomic aphasia.
• Language recovery may be mediated by shifting of functions to the right hemisphere or to adjacent left hemisphere regions.

RECOVERY AND REHABILITATION OFTHE PATIENT WITH APHASIA
• Whether contemporary methods of speech therapy accomplish more than can be accounted for by spontaneous recovery is still uncertain.
• Most aphasic disorders are caused by vascular disease and trauma, and they are nearly always accompanied by some degree of spontaneous improvement in the days, weeks, and months that follow the stroke or accident.

Communication with aphasic Do’s and Don’ts
• Keep your voice at a normal level and emphasize key words• Augment speech with gesture and visual aids when
possible• Repeat statements when necessary• Do not attempt to finish the patients statement for them

Communication with aphasic Do’s and Don’ts
• Talk to the person as an adult NOT as a child• Minimize or eliminate background noise• Make sure you have the person’s attention before
communicating• Encourage and use all modes of communication– Speech/writing/drawing/yes-no responses

Communication with aphasic Do’s and Don’ts
• Give them time to talk and permit a reasonable amount of time to respond
• Accept all communication attempts• Keep your own communication simple but adult• Simplify sentence structure and reduce your rate of speech

References
– Neurology – Bradly – Neurology –Lindsay – Harison – Neuroanatomy –Snell– National Aphasia Association
Related Documents